Abstract
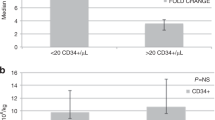
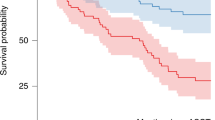
We describe 20 patients with myeloma and 1 with primary amyloidosis from 15 centres, all with advanced renal failure, most of whom had PBSC mobilised using plerixafor following previous failed mobilisation by conventional means (plerixafor used up-front for 4 patients). For 15 patients, the plerixafor dose was reduced to 0.16 mg/kg/day, with a subsequent dose increase in one case to 0.24 mg/kg/day. The remaining six patients received a standard plerixafor dosage at 0.24 mg/kg/day. Scheduling of plerixafor and apheresis around dialysis was generally straightforward. Following plerixafor administration, all patients underwent apheresis. A median CD34+ cell dose of 4.6 × 106 per kg was achieved after 1 (n=7), 2 (n=10), 3 (n=3) or 4 (n=1) aphereses. Only one patient failed to achieve a sufficient cell dose for transplant: she subsequently underwent delayed re-mobilisation using G-CSF with plerixafor 0.24 mg/kg/day, resulting in a CD34+ cell dose of 2.12 × 106/kg. Sixteen patients experienced no plerixafor toxicities; five had mild-to-moderate gastrointestinal symptoms that did not prevent apheresis. Fifteen patients have progressed to autologous transplant, of whom 12 remain alive without disease progression. Two patients recovered endogenous renal function post autograft, and a third underwent successful renal transplantation. Plerixafor is highly effective in mobilising PBSC in this difficult patient group.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Child JA, Morgan GJ, Davies FE, Owen RG, Bell SE, Hawkins K et al. Medical Research Council Adult Leukemia Working Party. High-dose chemotherapy with hematopoietic stem cell rescue for multiple myeloma. N Engl J Med 2003; 348: 1875–1883.
Lee C-K, Zangari M, Barlogie B, Fassas A, van Rhee F, Thertulien R et al. Dialysis-dependent renal failure in patients with myeloma can be reversed by high-dose myeloablative therapy and autotransplant. Bone Marrow Transplant 2004; 33: 823–828.
Knudsen LM, Nielsen B, Gimsing P, Geisler C . Autologous stem cell transplantation in multiple myeloma: outcome in patients with renal failure. Eur J Haematol 2005; 75: 27–33.
Yamamoto R, Kanda Y, Matsuyama T, Oshima K, Nannya Y, Suguro M et al. Myopericarditis caused by cyclophosphamide used to mobilize peripheral blood stem cells in a myeloma patient with renal failure. Bone Marrow Transplant 2000; 26: 685–688.
Narayanasami U, Kanteti R, Morelli J, Klekar A, Al-Olama A, Keating C et al. Randomized trial of filgrastim versus chemotherapy and filgrastim mobilization of hematopoietic progenitor cells for rescue in autologous transplantation. Blood 2001; 98: 2059–2064.
Calandra G, McCarty J, McGuirk J, Tricot G, Crocker S-A, Badel K et al. AMD3100 plus G-CSF can successfully mobilize CD34+ cells from non-Hodgkin's lymphoma, Hodgkin's disease and multiple myeloma patients previously failing mobilization with chemotherapy and/or cytokine treatment: compassionate use data. Bone Marrow Transplant 2008; 41: 331–338.
Duarte RF, Shaw BE, Marín P, Kottaridis P, Ortiz M, Morante C et al. Plerixafor plus G-CSF can mobilize hematopoietic stem cells from multiple myeloma and lymphoma patients failing previous mobilisation attempts: EU compassionate use data. Bone Marrow Transplant 2011; 46: 52–58.
Weaver CH, Tauer K, Zhen B, Schwartzberg LS, Hazelton B, Weaver Z et al. Second attempts at mobilization of peripheral blood stem cells in patients with initial low CD34+ cell yields. J Hematother 1998; 7: 241–249.
Goterris R, Hernandez-Boluda JC, Teruel A, Gomez C, Lis MJ, Terol MJ et al. Impact of different strategies of second-line stem cell harvest on the outcome of autologous transplantation in poor peripheral blood stem cell mobilizers. Bone Marrow Transplant 2005; 36: 847–853.
Boeve S, Strupeck J, Creech S, Stiff PJ . Analysis of remobilization success in patients undergoing autologous stem cell transplants who fail an initial mobilization: risk factors, cytokine use and cost. Bone Marrow Transplant 2004; 33: 997–1003.
MacFarland R, Hard ML, Scarborough R, Badel K, Calandra G . A pharmacokinetic study of plerixafor in subjects with varying degrees of renal impairment. Biol Blood Marrow Transplant 2010; 16: 95–101.
Hendrix CW, Flexner C, MacFarland RT, Giandomenico C, Fuchs EJ, Redpath E et al. Pharmacokinetics and safety of AMD1300, a novel antagonist of the CXCR4 chemokine receptor, in human volunteers. Antimicrob Agents Chemother 2000; 44: 1667–1673.
D’Addio A, Curti A, Worel N, Douglas K, Motta MR, Rizzi S et al. The addition of plerixafor is safe and allows adequate PBSC collection in multiple myeloma and lymphoma patients who are poor mobilizers after chemotherapy and G-CSF. Bone Marrow Transplant 2011; 46: 356–363.
Kumar S, Giralt S, Stadtmauer EA, Harousseau JL, Palumbo A, Bensinger W et al. Mobilization in myeloma revisited: IMWG consensus perspectives on stem cell collection following initial therapy with thalidomide-, lenalidomide-, or bortezomib-containing regimes. Blood 2009; 114: 1729–1735.
Dimopoulos MA, Christoulas D, Roussou M, Kastritis E, Migkou M, Gavriatopoulou M et al. Lenalidomide and dexamethasone for the treatment of refractory/relapsed multiple myeloma: dosing of lenalidomide according to renal function and effect on renal impairment. Eur J Haematol 2010; 85: 1–5.
Physicians’ Desk Reference. Red Book 2009: Pharmacy's Fundamental Reference, 113th Edition. Physicians' Desk Reference, New Jersey, 2009.
Delgado E, LeMaistre CF, Bachier C, Smith B, López-González G, Hougham M et al. Cost analysis of mobilization and autologous transplantation in patients who received AMD 3100 after failing standard mobilization. Blood (ASH Annual Meeting Abstracts) 2008; 112: 749a (Abstract 2151).
Acknowledgements
We thank the patients, nurses, data managers and stem cell laboratory staff at all participating centres. We would also like specifically to thank the following individuals for their assistance: Kristen Kemp, Program Coordinator & Quality Management Supervisor, Aurora St Luke's Medical Center, Milwaukee; Marie Ventimiglia, Bone Marrow Transplant Clinical Research Coordinator, Karmanos Cancer Institute, Detroit; Juli Murphy, Manager, BMT Clinical Research, Rocky Mountain Blood and Marrow Transplant Program, Denver; Dr Tharani Balasubramaniam, Leeds Teaching Hospitals, U.K.; Joy Sinclair, Apheresis Nurse Manager, Glasgow, U.K.; Dr Nicky Whitaker, Genzyme Europe; Purvi Mody, Genzyme Corporation USA; Pritesh Gandhi, Genzyme Corporation USA.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
Professor Roberto M Lemoli has received research support and compensation as a member of the scientific advisory board of Genzyme, Italy. Dr Kenny Douglas and Professor Gordon Cook have received consultancy and speaker bureau payments from Genzyme. Professor Nina Worel has received speaker bureau payments from Genzyme.
Rights and permissions
About this article
Cite this article
Douglas, K., Parker, A., Hayden, P. et al. Plerixafor for PBSC mobilisation in myeloma patients with advanced renal failure: safety and efficacy data in a series of 21 patients from Europe and the USA. Bone Marrow Transplant 47, 18–23 (2012). https://doi.org/10.1038/bmt.2011.9
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/bmt.2011.9
Keywords
This article is cited by
-
A plerixafor-based strategy allows adequate hematopoietic stem cell collection in poor mobilizers: results from the Canadian Special Access Program
Bone Marrow Transplantation (2014)
-
Plerixafor and G-CSF for autologous stem cell mobilization in AL amyloidosis
Bone Marrow Transplantation (2014)
-
Plerixafor in AL amyloidosis: improved graft composition and faster lymphocyte recovery after auto-SCT in patient with end-stage renal-disease
Bone Marrow Transplantation (2012)
-
Unsuccessful stem cell remobilization for autologous transplantation is predicted by renal impairment and a stem cell yield ⩽0.5 × 106 CD34+ cells/kg at first mobilization
Bone Marrow Transplantation (2012)
-
Novel agents and approaches for stem cell mobilization in normal donors and patients
Bone Marrow Transplantation (2012)