Abstract
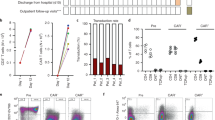
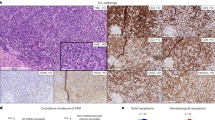
This single centre study assessed the incidence, kinetics and predictive factors of EBV reactivation and EBV-related lymphoproliferative diseases (LPD) in 33 consecutive patients who received a reduced intensity conditioning (RIC) before umbilical cord blood transplantation (UCBT). During the first 6 months after UCBT, weekly all patients were DNA-PCR screened in the peripheral blood for EBV reactivation and were clinically monitored for clinical features attributable to EBV. The cumulative incidences of EBV reactivation (defined as an EBV load >1000 EBV copies per 105 cells measured at least once during follow-up) at 6 months and 2 years after UCBT were 9 (95% confidence interval (CI), 2–22%) and 17% (95% CI, 6–33%), respectively. In 28 patients (85%), the EBV load remained negative at all times, and none of these patients experienced any sign of LPD. Five patients (15%) experienced at least one EBV reactivation episode. EBV reactivation was observed at a median of 132 days (range, 85–438) after UCBT. Two patients developed EBV-related LPD (cumulative incidence, 6% at 3 years). With a median follow-up of 468 days (range, 92–1277) post UCBT, the OS was 62% at 3 years. Five patients died of disease progression and seven patients died of transplant-related complications, including one case of EBV-related LPD. Univariate analysis did not identify any significant risk factor associated with EBV reactivation. We conclude that patients undergoing RIC UCBT are at risk for EBV reactivation, with the need for close EBV monitoring and the use of preemptive rituximab treatment as some cases may progress to life-threatening LPD.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Kelly SS, Parmar S, De Lima M, Robinson S, Shpall E . Overcoming the barriers to umbilical cord blood transplantation. Cytotherapy 2010; 12: 121–130.
Brunstein CG, Wagner JE . Umbilical cord blood transplantation and banking. Annu Rev Med 2006; 57: 403–417.
Barker JN, Krepski TP, DeFor TE, Davies SM, Wagner JE, Weisdorf DJ . Searching for unrelated donor hematopoietic stem cells: availability and speed of umbilical cord blood versus bone marrow. Biol Blood Marrow Transplant 2002; 8: 257–260.
Grewal SS, Barker JN, Davies SM, Wagner JE . Unrelated donor hematopoietic cell transplantation: marrow or umbilical cord blood? Blood 2003; 101: 4233–4244.
Mohty M, Rocha V, Chevallier P, Harousseau JL, Nagler A . Reduced-intensity conditioning for allogeneic stem cell transplantation: 10 years later. Curr Opin Oncol 2009; 21 (Suppl 1): S1.
Storb R, Yu C, Wagner JL, Deeg HJ, Nash RA, Kiem HP et al. Stable mixed hematopoietic chimerism in DLA-identical littermate dogs given sublethal total body irradiation before and pharmacological immunosuppression after marrow transplantation. Blood 1997; 89: 3048–3054.
Heslop HE . How I treat EBV lymphoproliferation. Blood 2009; 114: 4002–4008.
Barker JN, Martin PL, Coad JE, DeFor T, Trigg ME, Kurtzberg J et al. Low incidence of Epstein-Barr virus-associated posttransplantation lymphoproliferative disorders in 272 unrelated-donor umbilical cord blood transplant recipients. Biol Blood Marrow Transplant 2001; 7: 395–399.
Brunstein CG, Weisdorf DJ, DeFor T, Barker JN, Tolar J, van Burik JA et al. Marked increased risk of Epstein-Barr virus-related complications with the addition of antithymocyte globulin to a nonmyeloablative conditioning prior to unrelated umbilical cord blood transplantation. Blood 2006; 108: 2874–2880.
Mohty M, Bay JO, Faucher C, Choufi B, Bilger K, Tournilhac O et al. Graft-versus-host disease following allogeneic transplantation from HLA-identical sibling with antithymocyte globulin-based reduced-intensity preparative regimen. Blood 2003; 102: 470–476.
Malard F, Szydlo RM, Brissot E, Chevallier P, Guillaume T, Delaunay J et al. Impact of cyclosporine-A concentration on the incidence of severe acute graft-versus-host disease after allogeneic stem cell transplantation. Biol Blood Marrow Transplant 2010; 16: 28–34.
Mohty M, Jacot W, Faucher C, Bay JO, Zandotti C, Collet L et al. Infectious complications following allogeneic HLA-identical sibling transplantation with antithymocyte globulin-based reduced intensity preparative regimen. Leukemia 2003; 17: 2168–2177.
Chevallier P, Hebia-Fellah I, Planche L, Guillaume T, Bressolette-Bodin C, Coste-Burel M et al. Human herpes virus 6 infection is a hallmark of cord blood transplant in adults and may participate to delayed engraftment: a comparison with matched unrelated donors as stem cell source. Bone Marrow Transplant 2009; 45: 1204–1211.
Bressollette-Bodin C, Coste-Burel M, Besse B, Andre-Garnier E, Ferre V, Imbert-Marcille BM . Cellular normalization of viral DNA loads on whole blood improves the clinical management of cytomegalovirus or Epstein Barr virus infections in the setting of pre-emptive therapy. J Med Virol 2009; 81: 90–98.
Blaes AH, Cao Q, Wagner JE, Young JA, Weisdorf DJ, Brunstein CG . Monitoring and preemptive rituximab therapy for Epstein-Barr virus reactivation after antithymocyte globulin containing nonmyeloablative conditioning for umbilical cord blood transplantation. Biol Blood Marrow Transplant 2010; 16: 287–291.
Klein JP, Rizzo JD, Zhang MJ, Keiding N . Statistical methods for the analysis and presentation of the results of bone marrow transplants. Part I: unadjusted analysis. Bone Marrow Transplant 2001; 28: 909–915.
Klein JP, Rizzo JD, Zhang MJ, Keiding N . Statistical methods for the analysis and presentation of the results of bone marrow transplants. Part 2: regression modeling. Bone Marrow Transplant 2001; 28: 1001–1011.
Fine JP, Gray RJ . A proportional hazards model for subdistribution of a competing risk. JASA 1999; 94: 496–509.
Paya CV, Fung JJ, Nalesnik MA, Kieff E, Green M, Gores G et al. Epstein-Barr virus-induced posttransplant lymphoproliferative disorders. ASTS/ASTP EBV-PTLD Task Force and The Mayo Clinic Organized International Consensus Development Meeting. Transplantation 1999; 68: 1517–1525.
Heslop HE, Slobod KS, Pule MA, Hale GA, Rousseau A, Smith CA et al. Long-term outcome of EBV-specific T-cell infusions to prevent or treat EBV-related lymphoproliferative disease in transplant recipients. Blood 2010; 115: 925–935.
Thomson BG, Robertson KA, Gowan D, Heilman D, Broxmeyer HE, Emanuel D et al. Analysis of engraftment, graft-versus-host disease, and immune recovery following unrelated donor cord blood transplantation. Blood 2000; 96: 2703–2711.
Komanduri KV, St John LS, de Lima M, McMannis J, Rosinski S, McNiece I et al. Delayed immune reconstitution after cord blood transplantation is characterized by impaired thymopoiesis and late memory T-cell skewing. Blood 2007; 110: 4543–4551.
Mohty M, Mohty AM, Blaise D, Faucher C, Bilger K, Isnardon D et al. Cytomegalovirus-specific immune recovery following allogeneic HLA-identical sibling transplantation with reduced-intensity preparative regimen. Bone Marrow Transplant 2004; 33: 839–846.
Chakrabarti S, Milligan DW, Pillay D, Mackinnon S, Holder K, Kaur N et al. Reconstitution of the Epstein-Barr virus-specific cytotoxic T-lymphocyte response following T-cell-depleted myeloablative and nonmyeloablative allogeneic stem cell transplantation. Blood 2003; 102: 839–842.
Cohen J, Gandhi M, Naik P, Cubitt D, Rao K, Thaker U et al. Increased incidence of EBV-related disease following paediatric stem cell transplantation with reduced-intensity conditioning. Br J Haematol 2005; 129: 229–239.
Flamand L, Stefanescu I, Ablashi DV, Menezes J . Activation of the Epstein-Barr virus replicative cycle by human herpesvirus 6. J Virol 1993; 67: 6768–6777.
Faye A, Quartier P, Reguerre Y, Lutz P, Carret AS, Dehee A et al. Chimaeric anti-CD20 monoclonal antibody (rituximab) in post-transplant B-lymphoproliferative disorder following stem cell transplantation in children. Br J Haematol 2001; 115: 112–118.
Styczynski J, Reusser P, Einsele H, de la Camara R, Cordonnier C, Ward KN et al. Management of HSV, VZV and EBV infections in patients with hematological malignancies and after SCT: guidelines from the Second European Conference on Infections in Leukemia. Bone Marrow Transplant 2009; 43: 757–770.
van Esser JW, Niesters HG, Thijsen SF, Meijer E, Osterhaus AD, Wolthers KC et al. Molecular quantification of viral load in plasma allows for fast and accurate prediction of response to therapy of Epstein-Barr virus-associated lymphoproliferative disease after allogeneic stem cell transplantation. Br J Haematol 2001; 113: 814–821.
Wagner HJ, Cheng YC, Huls MH, Gee AP, Kuehnle I, Krance RA et al. Prompt versus preemptive intervention for EBV lymphoproliferative disease. Blood 2004; 103: 3979–3981.
Choquet S, Trappe R, Leblond V, Jager U, Davi F, Oertel S . CHOP-21 for the treatment of post-transplant lymphoproliferative disorders (PTLD) following solid organ transplantation. Haematologica 2007; 92: 273–274.
Acknowledgements
We thank the nursing staff for providing excellent care for our patients. We also thank the ‘Région Pays de Loire’, the ‘Association pour la Recherche sure Cancer (ARC)’, the ‘Fondation de France’, the ‘Fondation contre la Leucémie’, the ‘Agence de Biomédecine’, the ‘Association Cent pour Sang la Vie’, the ‘Association Laurette Fuguain’ and the association IRGHET for their generous and continuous support for our clinical and basic research work. Our group is supported by several grants from the French national cancer institute (PHRC, INCa). We would like to acknowledge the continuous support of the cell banking facility (‘tumurotheque’) of the CHU de Nantes.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Peric, Z., Cahu, X., Chevallier, P. et al. Features of EBV reactivation after reduced intensity conditioning unrelated umbilical cord blood transplantation. Bone Marrow Transplant 47, 251–257 (2012). https://doi.org/10.1038/bmt.2011.64
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/bmt.2011.64
Keywords
This article is cited by
-
Epstein-Barr virus-related post-transplant lymphoproliferative disease (EBV-PTLD) in the setting of allogeneic stem cell transplantation: a comprehensive review from pathogenesis to forthcoming treatment modalities
Bone Marrow Transplantation (2020)
-
Incidence and risk factors of EBV reactivation after unrelated cord blood transplantation: a Eurocord and Société Française de Greffe de Moelle-Therapie Cellulaire collaborative study
Bone Marrow Transplantation (2013)