Abstract
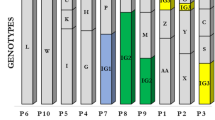
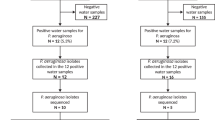
From May to October 2006, six severe Pseudomonas aeruginosa infections were diagnosed in patients undergoing SCT in the SCT unit of the Careggi hospital (Florence, Italy). Four of the infected patients were treated consecutively in the same room (room N). On the hypothesis of a possible environmental source of infection, samples were collected from different sites that had potential for cross-contamination throughout the SCT unit, including the electrolytic chloroxidant disinfectant used for hand washing (Irgasan) and the disinfectant used for facilities cleaning. Four of the environmental samples were positive for P. aeruginosa: three Irgansan soap samples and a tap swab sample from the staff cleaning and dressing room. The AFLP (amplified fragment length polymorphism) typing method employed to evaluate strain clonality showed that the isolates from the patients who had shared the same room and an isolate from Irgasan soap had a significant molecular similarity (dice index higher than 0.93). After adequate control measures, no subsequent environmental sample proved positive for P. aeruginosa. These data strongly support the hypothesis of the clonal origin of the infective strains and suggest an environmental source of infection. The AFLP method was fast enough to allow a ‘real-time’ monitoring of the outbreak, permitting additional preventive measures.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Fanci R, Paci C, Anichini P, Pecile P, Marra G, Casini C et al. Incidence and molecular epidemiology of Pseudomonas aeruginosa bacteremias in patients with acute leukemia: analysis by pulsed field gel electrophoresis. New Microbiol 2003; 26: 353–361.
Bukholm G, Tannaes T, Kjelsberg AB, Smith-Erichsen N . An outbreak of multidrug-resistant Pseudomonas aeruginosa associated with increased risk of patient death in an intensive care unit. Infect Control Hosp Epidemiol 2002; 23: 441–446.
Hakki M, Limaye AP, Kim KM, Kirby KA, Corey L, Boeckh M . Invasive Pseudomonas aeruginosa infections: high rate of recurrence and mortality after hematopoietic cell transplantation. Bone Marrow Transplant 2007; 39: 687–693.
Vianelli N, Giannini MB, Quarti C, Bucci Sabattini MA, Fiacchini M, de Vivo A et al. Resolution of Pseudomonas aeruginosa outbreak in a hematology unit with the use of disposable sterile water filters. Haematologica 2006; 91: 983–985.
Engelhart S, Krizek L, Glasmacher A, Fishnaller E, Marklein G, Exner M . Pseudomonas aeruginosa outbreak in a haematology–oncology unit associated with contaminated surface cleaning equipment. J Hosp Infection 2002; 52: 93–98.
Fanci R, Pecile P, Casalone E, Mengoni A, Tamburini E, Guidi S et al. Pseudomonas aeruginosa sepsis in stem cell transplantation patients. Infect Control Hosp Epidemiol 2006; 27: 767–770.
Renders N, Romling U, Verbrugh H, van Belkum A . Comparative typing of Pseudomonas aeruginosa by random amplification of polymorphic DNA of pulsed field gel electroph.oresis of DNA macrorestriction fragments. J Clin Microbiol 1996; 34: 3190–3195.
National Committee for Clinical and Laboratory Standard (NCCLS). Performance Standards for Antimicrobial Susceptibility Testing. 14th Informational Supplement M100-S14, Vol. 24, no. 1. NCCLS: Vilanova, PA, 2004.
Speijer H, Savelkoul PHM, Bonten MJ, Stobberingh EE, Tjhie JHT . Application of different genotyping methods for Pseudomonas aeruginosa in a setting of endemicity in an intensive care unit. J Clin Microbiol 1999; 37: 3654–3661.
Vos P, Hogers RM, Bleeker M, Reijans M, van de Lee T, Hornes M et al. AFLP: a new technique for DNA fingerprinting. Nucl Acids Res 1995; 23: 4407–4414.
McCann S, Byrne JL, Rovira M, Shaw P, Ribaud P, Sica S et al Outbreaks of infectious diseases in stem cell transplant units: a silent cause of death for patients and transplant programmes. Bone marrow transplant 2004; 33: 519–529.
Trautmann M, Lepper PM, Haller M . Ecology of Pseudomonas aeruginosa in the intensive care unit and the evolving role of water outlets as a reservoir of the organism. Am J Infect Control 2005; 33 (5 Suppl 1): S41–S49.
Aumeran C, Paillard C, Robin F, Kanold J, Baud O, Bonnet R et al. Pseudomonas aeruginosa and Pseudomonas putida outbreak associated with contaminated water outlets in an oncohaematology paediatric unit. J Hosp Infect 2007; 65: 47–53.
Barry MA, Crafen DE, Goularte TA, Lichtenberg DA . Serratia marcescens contamination of antiseptic soap containing triclosan: implications for nosocomial infection. Infect Control 1984; 5: 427–430.
Danchaivijitr S, Dhiraputra C, Rongrungruang Y, Srihapol N, Pumsuwan V . Microbial contamination of antiseptics and disinfectants. J Med Assoc Thai 2005; 88: S133–S139.
Boyce JM, Pittet D . Guideline for hand hygiene in health-care settings: recommendations of the healthcare infection control practices advisory committee and the Hicpac/Shea/Apic/Idsa hand hygiene task force. Infect Control Hosp Epidemiol 2002; 23: S3–41.
Siebor E, Lianes C, Lafon I, Ogier-Desserey A, Duez JM, Pechinot A et al. Presumed pseudobacteremia outbreak resulting from contamination of proportional disinfectant dispenser. Eur J Clin Microbiol Infect Dis 2007; 26: 195–198.
Acknowledgements
We are grateful to Mrs Cristina Indorato for technical assistance. This study was supported by a grant from Regione Toscana.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Fanci, R., Bartolozzi, B., Sergi, S. et al. Molecular epidemiological investigation of an outbreak of Pseudomonas aeruginosa infection in an SCT unit. Bone Marrow Transplant 43, 335–338 (2009). https://doi.org/10.1038/bmt.2008.319
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/bmt.2008.319