Abstract
Background:
Outcomes for ampullary adenocarcinomas are heterogeneous, and numerous methods of categorisation exist. A histomolecular phenotype based on histology, caudal-type homeodomain transcription factor 2 (CDX2) staining and Mucin 1 (MUC1) staining has recently been tested and validated in two cohorts. We attempt to validate this classification in a large patient population.
Methods:
Tissue samples from 163 patients with resected ampullary adenocarcinoma were classified based on histology and immunohistochemical expression of CDX2 and MUC1. A pancreaticobiliary histomolecular classification (PB) was defined as a sample with pancreaticobiliary histology, positive MUC1 and negative CDX2 expression.
Results:
There were 82 deaths; median follow-up of 32.4 months; and median overall survival of 87.7 (95% CI 42.9–109.5) months. PB comprised 28.2% of the cases. Factors associated with overall survival were histological subtype (P=0.0340); T1/2 vs T3/4 (P=0.001); perineural (P<0.0001) and lymphovascular (P=0.0203) invasion; and histomolecular intestinal histomolecular phenotype (INT) vs PB phenotype (106.4 vs 21.2 months, P<0.0001). Neither MUC1 nor CDX2 was statistically significant, although MUC1 positivity defined as ⩾10% staining was significant (P=0.0023). In multivariate analysis, age (HR 1.03), PB phenotype (HR 2.26) and perineural invasion (PNI; HR 2.26) were associated with poor survival.
Conclusions:
The prognostic ability of histomolecular phenotype has been validated in an independent cohort of ampullary adenocarcinoma patients.
Similar content being viewed by others
Main
The ampulla of Vater represents a small anatomic region into which three different epithelia (pancreatic, duodenal and biliary) converge. Owing to this fact, the exact tissue of origin responsible for ampullary adenocarcinomas has been uncertain. The known heterogeneity of clinical behaviour has led to a number of investigators to explore various histological and molecular characteristics in an attempt to prognostically stratify ampullary adenocarcinomas. (Yeo et al, 1998; Bouvet et al, 2000; O’Connell et al, 2008; Smith et al, 2008; Albores-Saavedra et al, 2009; Berberat et al, 2009; Hatzaras et al, 2010; Ang et al, 2014).
Kimura et al. (1994) were the first investigators to subclassify ampullary adenocarcinoma based on histologic features (intestinal vs pancreaticobiliary) and noted a survival advantage for those with intestinal phenotype. Over the past two decades, multiple investigators have sought to improve upon the histologic classification (Kitamura et al, 1996; Seno et al, 2002; Zhou et al, 2004; Hansel et al, 2005; Chang et al, 2007; Roh et al, 2007; de Paiva Haddad et al, 2010; Moriya et al, 2011; Ang et al, 2014). Intestinal phenotype tends to stain for MUC2, CK20, CDX2 (caudal-type homeodomain transcription factor 2) and occasionally CEA and CD10. In contrast, pancreaticobiliary phenotype stains positively for Mucin 1 (MUC1), CK7 and MUC5A. In general, patients with cancers whose features are more aligned with intestinal phenotype fare better than those with elements of either biliary or pancreatic phenotype (Kimura et al, 1994; Kitamura et al, 1996; Zhou et al, 2004; Hansel et al, 2005; Chang et al, 2007; Roh et al, 2007; Sessa et al, 2007; Westgaard et al, 2008; de Paiva Haddad et al, 2010; Moriya et al, 2011). In particular, positive staining for MUC2 and CDX2 tended to correlate with better survival, whereas MUC1 positivity correlated with worse survival. However, most studies included relatively few patients with variable definitions for intestinal and pancreaticobiliary subsets and were not validated in independent cohorts.
Recently, Chang et al. (2013) used histology, CDX2 and MUC1 expression to classify patients with resected ampullary cancer. In their study, the pancreaticobiliary histomolecular phenotype (PB) was defined as having pancreaticobiliary histology, any MUC1 staining and negative CDX2 staining defined as a CDX2 H-index ⩽35. Cases not meeting this definition were considered intestinal histomolecular phenotype (INT). PB phenotype and lymph node positivity were both risk factors for poor overall survival (OS) in multivariate analysis, and these factors were verified across two separate validation cohorts. MUC1 is a transmembrane glycoprotein that is expressed in 66–98% of pancreatic adenocarcinomas and cholangiocarcinomas (Yonezawa et al, 2011), whereas CDX2 is a transcription factor that has a role in early intestinal differentiation (Silberg et al, 2000) and is commonly expressed in intestinal adenocarcinomas but infrequently seen in pancreatic (5%) or extrahepatic cholangiocarcinoma (5–22%; Hansel et al, 2005; Chang et al, 2007; Jun et al, 2014).
We sought to confirm the results obtained by Chang et al. (2013) in a large, independent cohort of patients with ampullary cancer. The ultimate aim of such an approach would be to establish a reliable, inexpensive method to provide better prognostication for resected ampullary adenocarcinomas.
Materials and Methods
Patients
Tissue samples from 163 patients with resected ampullary adenocarcinoma from MD Anderson Cancer Center (MDACC; N=111) and from the Johns Hopkins Hospital (JHH; N=52) from 1992 until 2007 were obtained and analysed as outlined below. The patient variables, including demographic information, comorbidities, treatment course and outcome were obtained from the electronic medical records. This study was approved by the respective institutional review boards.
Sample selection
Tissue microarrays (TMAs) of tumour and nearby normal tissue were created from formalin-fixed, paraffin-embedded tumour blocks of 163 patients who previously underwent pylorus preserving pancreaticoduodenectomy for an ampullary adenocarcinoma at JHH and MDACC as previously described (Van Heek et al, 2004; Overman et al, 2013). In all cases, the original H&E slides from each surgical resection were reviewed to confirm the diagnosis of ampullary adenocarcinoma. H&E slides were also analysed by two Gastrointestinal Pathologists (HW and MG), and tumours were categorised based on whether the tissue appeared intestinal-like (tall columnar cells with elongated nuclei), pancreaticobiliary-like (rounded cells with rounded nuclei with scant fibrous cores) or mixed (>10% of each). Mixed histology was further simplified and categorised based on the predominant tissue component.
Immunohistochemistry
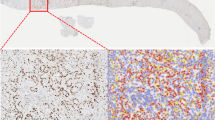
Immunohistochemical (IHC) stains were performed on 5-μm unstained sections from the TMA blocks. To retrieve the antigenicity, the tissue sections were treated at 100 °C in a steamer containing 10 mmol citrate buffer (pH 6.0) for 60 min. The sections were then immersed in methanol containing 0.3% hydrogen peroxidase for 20 min to block the endogenous peroxidase activity and were incubated in 2.5% blocking serum to reduce nonspecific binding. Sections were incubated for 90 min at 37 °C with primary antibodies: CDX2 (Biogenex, San Ramon, CA, USA; clone CDX-88) and MUC 1 (clone Ma695, Novocastra, Newcastle, UK). Standard avidin–biotin IHC analysis of the sections was performed according to the manufacturer’s recommendations (Vector Laboratories, Burlingame, CA, USA). MUC1 staining was graded as 0 (negative), 1 (very focally positive, 1–9%), 2 (focally positive, 10–50%) and 3 (positive >50%). A positive stain for MUC1 was defined as any positive staining (that is, 1, 2 or 3). Positive CDX2 samples were defined by an H-score>35%, where H-score=intensity of staining [0 to 3] × percentage of positive cells. Both definitions of MUC1 and CDX2 staining match those of Chang et al. (2013). IHC staining was interpreted independently by two gastrointestinal pathologists (HW and NN for CDX2 and VA and BS for MUC1) with any differences resolved by consensus review. A pancreaticobiliary histomolecular phenotype (PB) is defined as a tumour with pancreaticobiliary histology, CDX2 negativity and any MUC1 positivity.
Statistics
Association between categorical clinical variables was determined by the Fisher’s exact test. Survival curves were generated using the Kaplan–Meier method, and survival differences were determined with the log-rank test. The univariate Cox proportional hazards regression model for OS tested age, histological subtype, MUC1 staining, CDX2 staining, T stage, LN status, perineural invasion (PNI), lymphovascular invasion (LVI), neoadjuvant or adjuvant treatment and histomolecular phenotype. Cox proportional hazards models were fitted for multivariate analysis. After interactions between variables were examined, a backward stepwise procedure was used to derive the best-fitting model. The correlation coefficient (κ) was calculated according to the method of Cohen to estimate the interobserver agreement in MUC1 staining.
Results
Cohort characteristics
Characteristics of the combined MDACC and JHH ampullary cohort are summarised in Table 1. Males represented 58.8% of cases. Minorities were under-represented as 4.9% were African American. The mean age was 64.4 years (range 28–88 years old). There were 82 events (death) out of 163 (50.3%) patients analysed during the study period. The median follow-up for the entire cohort was 32.4 (0.3–189.5) months. The median OS was 87.7 (95% CI 42.9–109.5) months. The 3- and 5-year OS estimates were 62.8% (95% CI 54.4–70.1%) and 54.4% (95% CI 45.6–62.2%), respectively, for all patients.
Clinicopathological and molecular prognostic factors
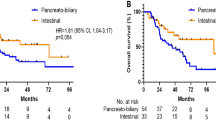
A PB histomolecular phenotype comprised 28.2% of the cases analysed. In univariate analysis, factors that were significantly associated with the median OS were intestinal vs pancreaticobiliary histology (109.5 vs 43.4 months, P=0.0340); T stage of 1 or 2 compared with 3 or 4 (114.1 vs 32.7 months, P=0.0001); absence of PNI compared with its presence (100.1 months vs 24.4, P<0.0001); absence of LVI compared with its presence (106.4 vs 25.3 months, P=0.0203); and INT vs PB histomolecular phenotype (106.4 vs 21.2 months, P<0.0001). Figure 1 shows the Kaplan–Meier curves comparing the ability of histological subtype vs histomolecular phenotype to classify ampullary adenocarcinomas. Lymph node status, CDX2 staining and MUC1 staining did not statistically correlate with OS. Lymph node positivity did correlate with histomolecular subtype as 49% of INT histomolecular phenotype were lymph node-positive, whereas 75% of PB histomolecular phenotype were lymph node-positive, P=0.004. A total of 28 cases with PB histology were reclassified as INT histomolecular phenotype due to either expression of CDX2 or lack of MUC1 expression. Survival for both groups was improved in comparison with the PB histomolecular phenotype cohort (Supplementary Figure 1).
A multivariate Cox proportional hazards model was used to assess the effect of multiple factors on OS. There were 154 patients available for the final analysis. Age (HR 1.03, 95% CI 1.01–1.06), PB histomolecular phenotype (HR 2.26, 95% CI 2.40–3.65) and PNI (HR 2.26, 95% CI 1.39–3.68) were the factors associated with OS in this analysis (Table 2). The T stage did not remain a significant factor in the multivariate model, although PNI and T stage were strongly correlated with 7.7% of T1 or T2 cases having PNI, whereas 52.1% of T3 and T4 having PNI (P<0.0001 by Fisher’s exact test).
CDX2 and MUC1 cutpoint analysis
To explore the lack of statistically significant correlation of MUC1 and CDX2 in univariate analysis conducted above, optimal cutpoints for these two markers were explored. Graphical analysis of H-index scores for CDX2 demonstrated that an H-score of >35 was acceptable (Supplementary Figure 2). For MUC 1, a positive MUC1 stain of ⩾10% was statistically significant with the median OS of 32.7 vs 109.5 months, P=0.0023 (Supplementary Table 1). In contrast to any positive staining, the MUC1-positive population reduced from 66 to 54% using the ⩾10% criterion. Incorporating this criterion within the histomolecular classification resulted in a PB histomolecular phenotype representing 25.7% of the study population with a median OS of 21.1 months compared with 108.3 m for the INT histomolecular phenotype, P<0.0001. In addition, utilising this MUC1 criterion resulted in an improved hazard ratio in multivariate modelling of 2.59 (95% CI 1.57–4.29) for the PB vs INT histomolecular phenotype (Supplementary Table 2). There was good intraobserver agreement (kappa=0.69) for MUC1 interpretation utilising a ⩾10% threshold.
Discussion
In this study we validate the histomolecular classification by Chang et al (2013) in a large data set. Our results lend support to the clinical use of this new classification for ampullary adenocarcinomas. Utilising this histomolecular classification allows the identification of a particularly aggressive cohort of patients (PB), which comprised 28.2% of our patient population. Given the inherent challenges of an IHC criteria of ‘any positive staining’ along with our data demonstrating improved prognostication with a MUC1 positivity defined as ⩾10% staining, we propose this definition for MUC1 positivity when applied to histomolecular subtyping of ampullary adenocarcinomas. Using this criterion, 25.2% of our population had a PB histomolecular phenotype with a median OS of 21.1 months in contrast to 108.3 months for the INT histomolecular phenotype, P<0.0001.
In the prior report by Chang et al. (2013) the MUC1 positivity rate varied from 42.7 to 67.4% across the three studied cohorts. In two cohorts, reviewed by the same pathologists, the rates were 67.4 and 59.7%, whereas in the third cohort, reviewed by a separate group of pathologists, the rate was 42.7%. In our opinion, this variation reflects both the challenges with applying an ‘any positive staining’ criteria to IHC review and the difficulty with MUC1 staining in general. As we found increasing MUC1 staining to correlate with worse outcomes, we propose that MUC1 positivity be defined at a ⩾10% tumour-staining criteria. This criterion is in alignment with prior work studying ampullary neoplasms in which a 10% threshold for MUC1 staining was utilised (Ohike et al, 2010).
Classifying ampullary tumours remains a challenge, and there is a reasonable level of disagreement by histology. In a recent study of 105 ampullary carcinoma cases concordance utilising histology alone was suboptimal with concordance among four gastrointestinal pathologists of κ=0.53 for intestinal subtype, κ=0.48 for pancreaticobiliary subtype, and κ=0.09 for mixed subtype (Ang et al, 2014). In this study the authors propose the use of an IHC panel including CDX2, MUC1, MUC2 and CK20 to aid in cases that are histologically ambiguous. However, 18% of cases could not be classified by IHC, and no outcome data were reported. Thus, despite the presence of multiple studies evaluating various IHC markers for prognostication of ampullary carcinomas, the validation of this study of the prognostic impact of the histomolecular criteria has demonstrated these criteria to be a reliable methodology to prognosticate ampullary carcinomas.
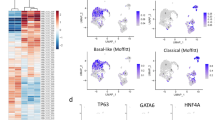
What this study does not address is whether there is a better method to classify these tumours based on an assay that can be considered closer to their underlying biology. Lessons from breast cancer may serve as a relevant example, in which subtypes differing based upon the cell of origin (luminal A, luminal B, ERBB2-overexpressing, basal, and so on) can be grouped based on gene expression-based classification (Perou et al, 2000), which corresponds fairly well with IHC detection of the key predictive markers such as the oestrogen receptor (ER) and HER2/neu. Although the biological understanding of ampullary adenocarcinomas is limited, a recent study that performed unsupervised gene expression clustering of ampullary adenocarcinomas identified two subgroups best classified as intestinal-like and biliary-like groups that were distinct from pancreatic adenocarcinoma (Overman et al, 2013). Such work supports the two-tiered classification of ampullary adenocarcinomas as defined in this study. Future efforts – perhaps using genomics or proteomics – to understand the molecular and biological basis of the histomolecular subgroups are needed.
Owing to the large sample size, TMAs were utilised for staining assessment, and despite the use of multiple cores per case, the possibility of variations in staining across the full tumour specimen cannot be determined. However, previous studies have shown that the results of TMA-based studies with two to three cores from each tumour are comparable to those using full sections. The suboptimal interobserver agreement for ampullary histological subtype determination that has been reported represents a limitation of the histological subtype-based prognostic classifier validated in this report. Our efforts to identify an optimal cutpoint for both CDX2 and MUC1 represent unvalidated findings and future efforts to further validate the optimal criteria for MUC1 positivity are needed.
How this study aids clinical decision-making regarding the choice of therapy – both in adjuvant and advanced settings – is an open question. The randomised phase III European Study Group for Pancreatic Cancer (ESPAC)-3 enroled resected periampullary adenocarcinomas, of which 297 were ampullary carcinomas, and randomized patients to observation vs chemotherapy (either bolus 5-FU or gemcitabine; Neoptolemos et al, 2012). After adjusting for prognostic factors, adjuvant chemotherapy improved OS, HR 0.75, P=0.03. However, differences by chemotherapy type were not seen and stratification by histological subtype was not reported as histological subtype determination was only carried out on 162 (55%) of the ampullary cases (Neoptolemos et al, 2012; Overman et al, 2012). Within this subgroup of ampullary cases an intestinal subtype demonstrated an improved DFS (P=0.01), but not OS (P=0.28). As in the ESPAC-3 study, other studies investigating ampullary subtypes had not investigated the predictive impact of such subtypes with regard to the type of chemotherapy. Despite this lack of data, the concept of ampullary subtype determined adjuvant chemotherapy (for example, FOLFOX for INT histomolecular phenotype and gemcitabine/cisplatin for PB histomolecular phenotype) has merit and should be explored in a clinical trial. In the metastatic setting the utilisation of histomolecular subtype determination with regard to the choice or sequence of systemic chemotherapy agents would represent a reasonable approach, given the limited studies and lack of consensus guidelines regarding systemic chemotherapy for metastatic ampullary carcinoma (Valle et al, 2010).
In conclusion, we validate the prognostic utility of a histomolecular classification of ampullary adenocarcinomas. This combination of histological and IHC classification of ampullary adenocarcinomas should be incorporated into clinical practice. Defining MUC1 positivity as ⩾10% staining should provide improved objectivity. Future efforts to understand the biological bases of ampullary subgroups are needed as is the incorporation of these subgroups into any future clinical trials.
Change history
30 June 2015
This paper was modified 12 months after initial publication to switch to Creative Commons licence terms, as noted at publication
References
Albores-Saavedra J, Schwartz AM, Batich K, Henson DE (2009) Cancers of the ampulla of vater: demographics, morphology, and survival based on 5,625 cases from the SEER program. J Surg Oncol 100: 598–605.
Ang DC, Shia J, Tang LH, Katabi N, Klimstra DS (2014) The utility of immunohistochemistry in subtyping adenocarcinoma of the ampulla of vater. Am J Surg Pathol 38: 1371–1379.
Berberat PO, Kunzli BM, Gulbinas A, Ramanauskas T, Kleeff J, Muller MW, Wagner M, Friess H, Büchler MW (2009) An audit of outcomes of a series of periampullary carcinomas. Eur J Surg Oncol 35: 187–191.
Bouvet M, Gamagami RA, Gilpin EA, Romeo O, Sasson A, Easter DW, Moossa AR (2000) Factors influencing survival after resection for periampullary neoplasms. Am J Surg 180: 13–17.
Chang DK, Jamieson NB, Johns AL, Scarlett CJ, Pajic M, Chou A, Pinese M, Humphris JL, Jones MD, Toon C, Nagrial AM, Chantrill LA, Chin VT, Pinho AV, Rooman I, Cowley MJ, Wu J, Mead RS, Colvin EK, Samra JS, Corbo V, Bassi C, Falconi M, Lawlor RT, Crippa S, Sperandio N, Bersani S, Dickson EJ, Mohamed MA, Oien KA, Foulis AK, Musgrove EA, Sutherland RL, Kench JG, Carter CR, Gill AJ, Scarpa A, McKay CJ, Biankin AV (2013) Histomolecular phenotypes and outcome in adenocarcinoma of the ampulla of vater. J Clin Oncol 31: 1348–1356.
Chang YT, Hsu C, Jeng YM, Chang MC, Wei SC, Wong JM (2007) Expression of the caudal-type homeodomain transcription factor CDX2 is related to clinical outcome in biliary tract carcinoma. J Gastroenterol Hepatol 22: 389–394.
de Paiva Haddad LB, Patzina RA, Penteado S, Montagnini AL, da Cunha JE, Machado MC, Jukemura J (2010) Lymph node involvement and not the histophatologic subtype is correlated with outcome after resection of adenocarcinoma of the ampulla of vater. J Gastrointest Surg 14: 719–728.
Hansel DE, Maitra A, Lin JW, Goggins M, Argani P, Yeo CJ, Piantadosi S, Leach SD, Biankin AV (2005) Expression of the caudal-type homeodomain transcription factors CDX 1/2 and outcome in carcinomas of the ampulla of Vater. J Clin Oncol 23: 1811–1818.
Hatzaras I, George N, Muscarella P, Melvin WS, Ellison EC, Bloomston M (2010) Predictors of survival in periampullary cancers following pancreaticoduodenectomy. Ann Surg Oncol 17: 991–997.
Jun SY, Eom DW, Park H, Bae YK, Jang KT, Yu E, Hong SM (2014) Prognostic significance of CDX2 and mucin expression in small intestinal adenocarcinoma. Mod Pathol 27: 1364–1374.
Kimura W, Futakawa N, Yamagata S, Wada Y, Kuroda A, Muto T, Esaki Y (1994) Different clinicopathologic findings in two histologic types of carcinoma of papilla of Vater. Jpn J Cancer Res 85: 161–166.
Kitamura H, Yonezawa S, Tanaka S, Kim YS, Sato E (1996) Expression of mucin carbohydrates and core proteins in carcinomas of the ampulla of Vater: their relationship to prognosis. Jpn J Cancer Res 87: 631–640.
Moriya T, Kimura W, Hirai I, Takasu N, Mizutani M (2011) Expression of MUC1 and MUC2 in ampullary cancer. Int J Surg Pathol 19: 441–447.
Neoptolemos JP, Moore MJ, Cox TF, Valle JW, Palmer DH, McDonald AC, Carter R, Tebbutt NC, Dervenis C, Smith D, Glimelius B, Charnley RM, Lacaine F, Scarfe AG, Middleton MR, Anthoney A, Ghaneh P, Halloran CM, Lerch MM, Oláh A, Rawcliffe CL, Verbeke CS, Campbell F, Büchler MW European Study Group for Pancreatic Cancer (2012) Effect of adjuvant chemotherapy with fluorouracil plus folinic acid or gemcitabine vs observation on survival in patients with resected periampullary adenocarcinoma: the ESPAC-3 periampullary cancer randomized trial. JAMA 308: 147–156.
O’Connell JB, Maggard MA, Manunga J Jr, Tomlinson JS, Reber HA, Ko CY, Hines OJ (2008) Survival after resection of ampullary carcinoma: a national population-based study. Ann Surg Oncol 15: 1820–1827.
Ohike N, Kim GE, Tajiri T, Krasinskas A, Basturk O, Coban I, Bandyopadhyay S, Morohoshi T, Goodman M, Kooby DA, Sarmiento JM, Adsay NV (2010) Intra-ampullary papillary-tubular neoplasm (IAPN): characterization of tumoral intraepithelial neoplasia occurring within the ampulla: a clinicopathologic analysis of 82 cases. Am J Surg Pathol 34: 1731–1748.
Overman M, Wang H, Varadhachary GR (2012) Adjuvant chemotherapy for resected periampullary adenocarcinoma. JAMA 308: 1855.
Overman MJ, Zhang J, Kopetz S, Davies M, Zhi-Qin J, Stemke-Hale K, Rümmele P, Pilarsky C, Grützmann R, Hamilton S, Hwang R, Abbruzzese JL, Varadhachary G, Broom B, Wang H (2013) Gene expression profiling of ampullary carcinomas classifies ampullary carcinomas into biliary-like and intestinal-like subtypes that are prognostic of outcome. PLoS One 8: e65144.
Perou CM, Sorlie T, Eisen MB, van de Rijn M, Jeffrey SS, Rees CA, Pollack JR, Ross DT, Johnsen H, Akslen LA, Fluge O, Pergamenschikov A, Williams C, Zhu SX, Lønning PE, Børresen-Dale AL, Brown PO, Botstein D (2000) Molecular portraits of human breast tumours. Nature 406: 747–752.
Roh YH, Kim YH, Lee HW, Kim SJ, Roh MS, Jeong JS, Jung GJ (2007) The clinicopathologic and immunohistochemical characteristics of ampulla of Vater carcinoma: the intestinal type is associated with a better prognosis. Hepatogastroenterology 54: 1641–1644.
Seno H, Oshima M, Taniguchi MA, Usami K, Ishikawa TO, Chiba T, Taketo MM (2002) CDX2 expression in the stomach with intestinal metaplasia and intestinal-type cancer: Prognostic implications. Int J Oncol 21: 769–774.
Sessa F, Furlan D, Zampatti C, Carnevali I, Franzi F, Capella C (2007) Prognostic factors for ampullary adenocarcinomas: tumor stage, tumor histology, tumor location, immunohistochemistry and microsatellite instability. Virchows Arch 451: 649–657.
Silberg DG, Swain GP, Suh ER, Traber PG (2000) Cdx1 and cdx2 expression during intestinal development. Gastroenterology 119: 961–971.
Smith RA, Ghaneh P, Sutton R, Raraty M, Campbell F, Neoptolemos JP (2008) Prognosis of resected ampullary adenocarcinoma by preoperative serum CA19-9 levels and platelet-lymphocyte ratio. J Gastrointest Surg 12: 1422–1428.
Valle J, Wasan H, Palmer DH, Cunningham D, Anthoney A, Maraveyas A, Madhusudan S, Iveson T, Hughes S, Pereira SP, Roughton M, Bridgewater J ABC-02 Trial Investigators (2010) Cisplatin plus gemcitabine versus gemcitabine for biliary tract cancer. New Engl J Med 362: 1273–1281.
Van Heek NT, Maitra A, Koopmann J, Fedarko N, Jain A, Rahman A, Iacobuzio-Donahue CA, Adsay V, Ashfaq R, Yeo CJ, Cameron JL, Offerhaus JA, Hruban RH, Berg KD, Goggins M (2004) Gene expression profiling identifies markers of ampullary adenocarcinoma. Cancer Biol Ther 3: 651–656.
Westgaard A, Tafjord S, Farstad IN, Cvancarova M, Eide TJ, Mathisen O, Clausen OP, Gladhaug IP (2008) Pancreatobiliary versus intestinal histologic type of differentiation is an independent prognostic factor in resected periampullary adenocarcinoma. BMC Cancer 8: 170.
Yeo CJ, Sohn TA, Cameron JL, Hruban RH, Lillemoe KD, Pitt HA (1998) Periampullary adenocarcinoma: analysis of 5-year survivors. Ann Surg 227: 821–831.
Yonezawa S, Higashi M, Yamada N, Yokoyama S, Kitamoto S, Kitajima S, Goto M (2011) Mucins in human neoplasms: clinical pathology, gene expression and diagnostic application. Pathol Int 61: 697–716.
Zhou H, Schaefer N, Wolff M, Fischer HP (2004) Carcinoma of the ampulla of Vater: comparative histologic/immunohistochemical classification and follow-up. Am J Surg Pathol 28: 875–882.
Acknowledgements
This work was supported by The Kavanagh Family Foundation.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
This work is published under the standard license to publish agreement. After 12 months the work will become freely available and the license terms will switch to a Creative Commons Attribution-NonCommercial-Share Alike 4.0 Unported License.
Supplementary Information accompanies this paper on British Journal of Cancer website
Rights and permissions
From twelve months after its original publication, this work is licensed under the Creative Commons Attribution-NonCommercial-Share Alike 4.0 Unported License. To view a copy of this license, visit http://creativecommons.org/licenses/by-nc-sa/4.0/
About this article
Cite this article
Schueneman, A., Goggins, M., Ensor, J. et al. Validation of histomolecular classification utilizing histological subtype, MUC1, and CDX2 for prognostication of resected ampullary adenocarcinoma. Br J Cancer 113, 64–68 (2015). https://doi.org/10.1038/bjc.2015.172
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/bjc.2015.172
Keywords
This article is cited by
-
Histologic subtype-based evaluation of recurrence and survival outcomes in patients with adenocarcinoma of the ampulla of Vater
Scientific Reports (2023)
-
The use of histopathological subtyping in patients with ampullary cancer: a nationwide analysis
World Journal of Surgical Oncology (2022)
-
Ampullary carcinoma of the duodenum: current clinical issues and genomic overview
Surgery Today (2022)
-
Adjuvant therapy for true ampullary cancer: a systematic review
Clinical and Translational Oncology (2020)
-
Distinct immunological properties of the two histological subtypes of adenocarcinoma of the ampulla of Vater
Cancer Immunology, Immunotherapy (2019)