Abstract
Background:
Immune modulation in cancer refers to a range of treatments aimed at harnessing a patient’s immune system to achieve tumour control, stabilisation, and potential eradication of disease. A novel therapeutic drug class called immune checkpoint-blocking antibodies modulate T-cell pathways that regulate T cells and have the potential to reinvigorate an antitumour immune response. Ipilimumab was the first FDA-approved immune checkpoint antibody licensed for the treatment of metastatic melanoma (MM) and blocks a checkpoint molecule called cytotoxic T-lymphocyte antigen 4 (CTLA-4).
Methods:
Herein we review the preclinical and clinical development of ipilimumab. We outline the mode of action of these agents and other immune checkpoint inhibitors, the management of their toxicities, and how to adequately assess response to treatment.
Results:
As a result of these data, a number of other antibodies that block novel checkpoint molecules including programmed death-1 (PD-1), and corresponding ligands such as programmed death ligand-1 (PD-L1) are under preclinical and clinical development, and have demonstrated activity in multiple tumour types.
Conclusions:
This review will summarise the mechanism of action and clinical development of immune checkpoint antibodies, as well as lessons learned in the management and assessment of patients receiving these agents.
Similar content being viewed by others
Main
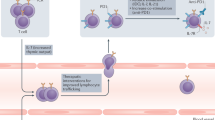
During immune surveillance, the host provides defense against foreign antigens, while ensuring it limits activation against self-antigens (Page et al, 2014). Immune checkpoints are cell surface molecules that serve as endogenous regulators of the immune response, limiting autoimmunity by mediating co-inhibitory signalling pathways (Nirschl and Drake, 2013). In cancer, these pathways are important in the tumour microenvironment and draining lymph nodes, leading to a state of T-cell exhaustion, thereby allowing tumour escape from immune surveillance, and unchecked tumour growth. Monoclonal antibodies (mAbs) that target immune checkpoints either antagonise co-inhibitory immunologic pathways or activate co-stimulatory pathways. These immune checkpoint antibodies are clinically active in a variety of malignancies, including those not traditionally classified as immunogenic, such as non-small-cell lung cancer (NSCLC).
The prototypical immune checkpoint mAb, and first to be approved by the FDA, is ipilimumab (Yervoy, Bristol-Myers Squibb, New York, NY, USA). Ipilimumab is a fully human antibody that targets cytotoxic T-lymphocyte antigen 4 (CTLA-4; Hodi et al, 2003) and was approved for metastatic melanoma (MM) based upon two phase III studies demonstrating an improvement in overall survival (OS; Hodi et al, 2010; Robert et al, 2011). After the initial clinical development of this agent, agents modulating other novel immune checkpoint molecules and their ligands have been identified, such as programmed death-1 (PD-1), programmed death ligand-1 (PD-L1), lymphocyte activation gene-3, T-cell immunoglobulin mucin protein-3, GITR, and CD-137 (Figure 1) among others (Page et al, 2014). This article will summarise the underlying mechanisms by which immune checkpoint mAbs elicit an antitumour effect, as well as outline the preclinical and clinical development of both single agent and combination immune modulation with checkpoint antibodies.
Targets of antibody immune modulators ( Page et al, 2014). Targets of antibody immune modulators. (A) Targetable members of the CD28/CTLA-4 immunoglobulin superfamily include cytotoxic T lymphocyte antigen 4 (CTLA-4), programmed cell death protein 1 (PD-1), B- and T-cell attenuator (BTLA), lymphocyte activation gene 3 (LAG3), and inducible T-cell costimulator (ICOS). (B) Targetable members of the tumour necrosis factor (TNF) superfamily include CD40, OX40, CD137/4-1BB, glucocorticoid-induced TNFR-related protein (GITR), and CD27. (C) Programmed cell death 1 ligand 1 (PD-L1). (D) Killer inhibitory receptor (KIR). (E) T-cell Ig and mucin-containing domain 3 (TIM3).
Anti-CTLA-4 antibodies
Preclinical studies with CTLA-4
CTLA-4 is a molecule expressed on the surface of CD-4 and CD-8 T cells as well as CD25+FOXP3+ T-regulatory cells, and is a member of the CD28/immunoglobulin superfamily (Avogadri et al, 2011). CTLA-4 competes with CD28 to bind to its ligands B7–1 (CD80) and B7–2 (CD86) on antigen-presenting cells (APCs). CTLA-4 generates an inhibitory signal that blocks a T-cell response. An anti-CTLA-4 antibody was first studied in transplantable tumour models of colon carcinoma (51BLim10), fibrosarcoma (Sa1N and CSA1M), ovarian cancer (OV-HM), and prostate cancer (TRAMPC1; Yang et al, 1997). In these models, primary shrinkage of tumours was observed in response to the mAb, and recurrence was not seen at the time of tumour rechallenge.
Anti-CTLA-4 agents: ipilimumab and tremelimumab
Ipilimumab was first tested in MM in a phase I trial of 17 patients and demonstrated two durable partial responses at a starting dose of 3 mg kg−1 (Tchekmedyian et al, 2002). A dose–response relationship was established in a double-blind phase II trial at three dose levels of 0.3, 3, or 10 mg kg−1, administered every 3 weeks for four doses, followed by 12-weekly maintenance therapy. A response rate (RR) of 11% and a median OS of 14 months were reported in the 10-mg kg−1 group, despite a greater incidence of grade 3/4 adverse events (AEs; Wolchok et al, 2010). On the basis of these findings, ipilimumab was investigated in the phase III setting in two randomised-controlled trials, that both demonstrated an improvement in OS (Hodi et al, 2010; Robert et al, 2011). The first trial compared ipilimumab at a dose of 3 mg kg−1 with or without gp100 peptide vaccine, vs the gp100 peptide vaccine alone (Hodi et al, 2010). The median OS in the ipilimumab and ipilimumab/gp100 groups was 10.1 vs 10.0 months, respectively, compared with 6.4 months with gp100 alone, with a hazard ratio (HR) of 0.68, P<0.001). In the first-line setting, ipilimumab/dacarbazine was compared with dacarbazine/placebo, at an ipilimumab dose of 10 mg kg−1, followed by maintenance ipilimumab or placebo every 12 weeks. This trial demonstrated an improvement in the median OS for the combination arm (11.2 months vs 9.1 months; Robert et al, 2011). In this study, the number of long-term survivors exceeded the number of patients with objective responses (ORs), with survival rates in the ipilimumab/dacarbazine group at 1 year of (47.3% vs 36.3%), 2 years (28.5% vs 17.9%), and 3 years (20.8% vs 12.2%; HR for death, 0.72; P<0.001). Responses were durable, with a median duration of response of 19.3 months with the combination and 8.1 months with dacarbazine alone. These observations suggest that immune-based therapies may generate a sustained antitumour effect in a subset of patients, long after completion of active therapy. Of patients re-induced on the original ipilimumab/gp100 trial, 19% (n=6/31) of patients exhibited an OR, with an additional 48% (n=15/31) achieving stable disease (SD; Hodi et al, 2010). Ipilimumab has also been evaluated in other cancers, with responses observed in both renal cell carcinoma (RCC) and NSCLC (Yang et al, 2007; Lynch et al, 2012). A three-arm phase II study in NSCLC evaluated concurrent, phased, and sequential ipilimumab combined with carboplatin and paclitaxel in patients with stage IV NSCLC (Lynch et al, 2012). This trial demonstrated a benefit in immune-related progression-free survival, defined later in this review. A subset analysis of this study benefit in patients with squamous cell carcinomas of the lung, leading to a large phase III study (NCT01285609).
A second antibody against CTLA-4, tremelimumab (MedImmune LLC, Gaithersburg, MD, USA), is a human immunoglobulin G2 (IgG2) monoclonal antibody (Ribas et al, 2007). Ribas et al (2013) reported a phase III trial of tremelimumab vs investigator’s choice of chemotherapy in MM, at a dose of 15 mg kg−1 every 3 months. A median duration of response of 36 months was seen with tremelimumab vs 14 months with combination chemotherapy (P=0.0011); however, no OS benefit was observed. This finding can potentially be explained by the exclusion of patients with an elevated lactate dehydrogenase level, crossover of patients to ipilimumab, as well as possible suboptimal dose and schedule.
Anti-PD-1/PD-L1 antibodies
Preclinical studies with the PD-1/PD-L1,2 pathway
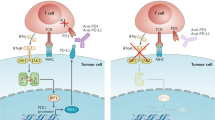
The PD-1/PD-L1,2 pathway is a second inhibitory immune checkpoint pathway, mediated by the transmembrane molecule PD-1 (CD279) found on the surface of T lymphocytes, B lymphocytes, and monocytes (Keir et al, 2008). PD-1 binds to PD-L1 and PD-L2, which are expressed on APCs and other cells, including tumour and normal tissues. Upon ligation to PD-L1/2, PD-1 suppresses downstream phosphoinositide 3-kinase (PI3K) and Akt signalling via an immunoreceptor tyrosine-based inhibitory motif. In contrast, CTLA-4 signalling inhibits Akt independent of PI3K(Parry et al, 2005). These two pathways therefore bring about similar effects but by different mechanisms.
Anti-PD-1 agents: nivolumab, MK3475 and pidilizumab
The first anti-PD-1 mAb to be clinically evaluated was nivolumab (BMS-936558), a human monoclonal immunoglobulin (Ig) G4 antibody. Results from a Phase Ib study of nivolumab reported activity in MM, RCC and NSCLC (Topalian et al, 2012). Objective response rates (ORRs) in these diseases were 28% (n=26/94), 24% (n=4/17), and 18% (n=14/76) respectively. The median duration of response was 74 weeks, with a median OS of 9.6 months in the patients with heavily-pretreated NSCLC. Nivolumab monotherapy at a dose of 3 mg kg−1 is currently being studied in phase III clinical trials in MM, RCC and NSCLC (Table 1). Successful re-induction with nivolumab has been described in a patient with melanoma who achieved a partial response (PR), followed by a period of SD for 16 months off treatment (Lipson et al, 2013).
A second humanised monoclonal IgG4 anti-PD-1 antibody, MK-3475 (Merck, Sharpe and Dohme, Whitehouse Station, NJ, USA), was deemed safe at 1 mg kg−1, 3 mg kg−1, and 10 mg kg−1 dose levels administered every 2 weeks in a phase I study, with no maximum tolerated dose (MTD) identified (Patnaik and Tolcher, 2012). This agent was subsequently studied in both first-line and ipilimumab-pretreated patients with MM, at dose levels 2 and 10 mg kg−1 administered every 2 or 3 weeks. Identical immune-related responses by immune-related response criteria (irRC), detailed later in this review, were 56% in both first-line and ipilImumab-pretreated patients at 10 mg kg−1 given every 2 weeks (Hamid et al, 2013). A phase II trial of this agent at two dose levels in comparison to chemotherapy, is currently in accrual (NCT01704287), as well as a phase III study in advanced MM compared to ipilimumab (NCT01866319).
In hematologic malignancies, the anti-PD-1 antibody pidilizumab (CT-011) demonstrated a ORR of 66% (n=19/32) when combined with rituximab in relapsed follicular lymphoma (Westin et al, 2014). An ORR of 51% was also seen in a phase II study of 35 patients with measurable disease after autologous stem-cell transplant for diffuse large B-cell lymphoma (n=18/35) (Armand et al, 2013). This agent is currently being studied in MM, malignant gliomas, RCC and combination with chemotherapy in advanced colorectal cancer (NCT01435369, NCT01952769, NCT01441765, NCT00890305).
Anti-PD-L1 agents: BMS-936559 and MPDL3280A
The first anti-PD-L1 mAb to be clinically evaluated was BMS-936559. Brahmer and colleagues reported a phase I study of this agent in multiple tumour types, including 75 patients with NSCLC and 52 with MM (Brahmer et al, 2012). The ORR 17% of patients with MM was 17% (n=9/52), 12% in RCC (n=2/17), 10% in patients with NSCLC (n=5/49). No MTD was found, and 9% of patients sustained grade 3/4 AEs. MPDL3280A is a second human mAb against PD-L1, and contains an engineered Fc portion that targets PD-L1. In a phase I trial of MPDL3280A administered to patients with MM, RCC and NSCLC, RR’s were 29%, 22% and 15% respectively (Hamid and Lawrence, 2012). Table 1 outlines current phase III trials with nivolumab and other agents targeting the PD-1/PD-L1,2 pathway, in a number of tumour types. Additional PD-L1-directed agents such as MEDI-4736 are being evaluated in the phase I setting.
Toxicities with immune checkpoint antibodies
The spectrum of AEs associated with immune checkpoint antibodies are termed immune-related AEs (irAE’s). The underlying pathophysiology relates to the immune-based mode of action of these agents, leading to T-cell inflammatory infiltration of solid organs, and increased serum inflammatory cytokines (Fecher et al, 2013). irAEs observed with ipilumumab appear to be dose-dependent, and range in severity from mild to fatal, and in onset from slow to sudden, but generally appear late, 8–10 weeks after initiation of therapy (Weber et al, 2012). Medical management is aimed at correctly identifying the irAE, grading based on the National Cancer Institute common toxicity criteria of AEs, and initiating early treatment with supportive care or immunosuppressive medications, typically corticosteroids. AEs with ipilumumab and tremelimab were common and ranged from mild to severe, with the incidence of grade 3/4 irAEs in phase III studies ranging from 17 to 56% (Ribas et al, 2007; Hodi et al, 2010; Robert et al, 2011). The most commonly observed irAEs with ipilumumab and tremelimumab are dermatitis (pruritus, rash), enterocolitis, endocrinopathies (hypophysitis, thyroiditis), liver enzyme abnormalities, and uveitis (Page et al, 2014). irAEs including mild fatigue, rash, diarrhea, and colitis have been described with anti-PD-1 agents, although AEs seem to be less common than those seen with anti-CTLA-4 antibodies (Gangadhar and Vonderheide, 2014). A rare but potentially fatal inflammatory pneumonitis was observed in 2–4% of cases, and led to three treatment-related deaths in the original phase I study of nivolumab (Topalian et al, 2012). In the phase I study of MK-3475 in MM, 13% of patients developed grade 3/4 irAEs, and 4% developed mild (grades 1–2) pneumonitis (Hamid et al, 2013). MPDL3280A had a 30–40% incidence of grade 3/4 AEs including hyperglycaemia, nephritis, and fatigue, but no cases of grade 3–5 pneumonitis were reported (Hamid and Lawrence, 2012). Toxicities may vary across tumour types, possibly explained by heterogeneity of antigen expression and resulting autoreactivity.
Management algorithms have emerged for irAE’s, such as inflammatory diarrhea/colitis and uniformly begin with elimination of potential infectious etiologies. Grade I diarrhea is managed with oral hydration, an American Dietary Association colitis diet, and loperamide (Weber et al, 2012). Diarrhea of grade 2 or greater can be managed with oral budesonide, oral corticosteroids, intravenous methylprednisolone, and occasionally infliximab (Fecher et al, 2013). Colitis-associated mortality is associated with management delays, failure to withhold ipilimumab, and an inadequate antidiarrheal regimen. The use of effective management algorithms have reduced life-threatening complications, with bowel perforations now occurring in <1% of patients.
Assessing response to immunotherapeutics
Antitumour responses with immunotherapies are heterogenous: responses may be mixed or delayed, lesions may enlarge before shrinking, lesions may remain stable or slowly regress over time. These responses can be potentially explained by T-cell activation and tumoral infiltration by immune cells, as well as intra-patient heterogeneity of tumour–host interactions. These observations led a group of colleagues to propose the ‘immune-related response criteria (irRC)’ for evaluating response to immunotherapeutic agents. These criteria are based on the rationale that immunotherapies generate an antitumour effect with response kinetics distinct from cytotoxic chemotherapy (Wolchok et al, 2009). The irRC thus recommends interval imaging at least 4 weeks apart to aid in the confirmation of asymptomatic progression. Owing to these response patterns, patients who experience clinically insignificant progression often continue therapy until progression is confirmed on subsequent imaging.
Intriguing clinical effects with immune checkpoint antibodies and radiation therapy have also been observed. The abscopal effect refers to tumour regression occurring outside an irradiated field, when a patient is receiving immunomodulatory therapy (Postow et al, 2012). The underlying mechanism is thought to be due to the stimulation of antigen release by local inflammation at the site of radiotherapy. The combination of radiation plus immunotherapy is being prospectively studied (NCT01703507, NCT01497808, NCT01565837, and NCT01689974).
Biomarkers to immune checkpoint molecules
As only a subset of patients treated with immune checkpoint antibodies experience durable and long-term disease control, predictive biomarker development has become a priority. The absolute lymphocyte count (ALC) is a potential pharmacodynamic biomarker for ipilimumab, with the ALC at 7 weeks (⩾1000 cells μl−1) and magnitude of ALC increases with therapy demonstrating promising results (Ku et al, 2010; Postow and Panageas, 2012). Baseline absolute eosinophil count and relative eosinophil count have also been associated with improved survival in these patients (Delyon et al, 2013; Schindler and Postow, 2013).
Potential predictive biomarkers for PD-1/PD-L1 targeting agents include PD-L1 expression by tumour cells by a variety of immunohistochemical (IHC) techniques and laboratory assays. Patients with tumours expressing PD-L1 in the original phase I trial of nivolumab had an ORR of 44% vs 17% among PD-L1-negative patients (Topalian et al, 2012). However, PD-L1 expression in a recent ipilimumab+nivolumab trial revealed similar response in both PD-L1-positive and -negative groups (RR n=8/17 in PD-L1 negative vs n=4/10 in PD-L1 positive; Grosso and Inzunza, 2013). Variations in IHC technique, cancer type, primary vs metastatic lesions, and treatment history are likely to contribute to PD-L1 expression. In addition, PD-L1 expression has been shown to be dynamic, and associated with tumour-intrinsic and tumour-extrinsic factors, such as loss of PTEN tumour suppressor expression, as well as interferon gamma production (Callahan and Curran, 2013). PD-L1 expression is being prospectively evaluated as a potential predictive biomarker in a phase III trial comparing nivolumab vs chemotherapy in melanoma (NCT01721746). It is important to recognise that no study to date has shown a 0% RR in patients with PD-L1-negative tumours, implying that this is not a binary indicator of potential durable benefit. Careful consideration should be exercised before any treatment decisions are made based on a heterogeneously and dynamically inducible biomarker. This is very much unlike static genetically encoded biomarkers, such as BRAF or EGFR mutations.
Combinatorial approaches
The combination of ipilimumab and nivolumab was recently evaluated in a phase I trial in MM, demonstrating a RR of 53% at the MTD, with all responding subjects in this cohort achieving a ⩾80% decline in tumour burden at 12 weeks (Wolchok et al, 2013). The combination was safe; however, there were more frequent (53%) grade 3/4 AEs than with either agent as monotherapy. Other mAb combinations are currently being investigated, and are detailed in Table 2. Another strategy is to combine checkpoint agents with other standard or investigational anticancer therapies including radiotherapy, cytotoxic chemotherapy, targeted therapies, or vaccine/cytokine therapy. However, the combination of ipilimumab+BRAF inhibitor vemurafenib produced significant hepatotoxicity, requiring termination of a phase I trial. (Ribas et al, 2013) A study of dabrafenib and trametinib with ipilimumab is ongoing and trials of targeted therapies with PD-1 pathway-blocking drugs are about to be initiated in MM.
Novel immune checkpoint molecules
New agents that attempt to target other immunomodulatory receptors on T cells and other immune cells are in development (Figure 1). Agonists of co-stimulatory molecules on B and T cells such as CD-137, OX40, and glucocorticoid-induced TNFR-related protein (GITR) are in clinical development (Mallett et al, 1990). A phase I study of an OX40 agonist in advanced solid tumours demonstrated tumour shrinkage of at least one metastatic lesion in 12 out of 30 subjects after one cycle of therapy (Curti et al, 2013). A humanised anti-GITR mAb (TRX518) also enhances co-stimulation in human lymphocytes in vitro, and is being studied in a dose-escalation trial (NCT1239134). CD-137/4-1BB is a third co-stimulatory mediator present on activated T cells, with corresponding ligands on activated B cells, and APCs (Lin et al, 2008). Agonist mAbs for CD137 enhance the co-stimulatory signal on T cells and such mAbs against CD137 have entered clinical trials in haematologic malignancies and others (urelumab: NCT01471210, NCT01775631; PF-05082566: NCT01307267).
Conclusion
Preliminary studies of CTLA-4, PD-1, and PD-L1-blocking antibodies show clear evidence of clinical activity, proving that immune checkpoint modulation is a viable emerging treatment modality across malignancy types, even in cancers not traditionally viewed as amenable to immunotherapy. However, because responses are confined to a subset of treated subjects, future development will focus upon rational combinatorial approaches and predictive biomarker discovery.
References
Armand P, Nagler A, Weller EA, Devine SM, Avigan DE, Chen YB, Kaminski MS, Holland HK, Winter JN, Mason JR, Fay JW, Rizzieri DA, Hosing CM, Ball ED, Uberti JP, Lazarus HM, Mapara MY, Gregory SA, Timmerman JM, Andorsky D, Or R, Waller EK, Rotem-Yehudar R, Gordon LI (2013) Disabling immune tolerance by programmed death-1 blockade with pidilizumab after autologous hematopoietic stem-cell transplantation for diffuse large B-cell lymphoma: results of an international phase II trial. J Clin Oncol 31 (33): 4199–4206.
Avogadri F, Yuan J, Yang A, Schaer D, Wolchok JD (2011) Modulation of CTLA-4 and GITR for cancer immunotherapy. Curr Top Microbiol Immunol 344: 211–244.
Brahmer JR, Tykodi SS, Chow LQ, Hwu WJ, Topalian SL, Hwu P, Drake CG, Camacho LH, Kauh J, Odunsi K, Pitot HC, Hamid O, Bhatia S, Martins R, Eaton K, Chen S, Salay TM, Alaparthy S, Grosso JF, Korman AJ, Parker SM, Agrawal S, Goldberg SM, Pardoll DM, Gupta A, Wigginton JM (2012) Safety and activity of anti-PD-L1 antibody in patients with advanced cancer. N Engl J Med 366 (26): 2455–2465.
Callahan MK HC, Curran MA (2013) Peripheral and tumor immune correlates in patients with advanced melanoma treated with combination nivolumab (anti-PD-1, BMS-936558, ONO-4358) and ipilimumab. The Annual Meeting of the American Society of Clinical Oncology, Chicago, USA. J Clin Oncol 31 (Suppl): abstr 3003.
Curti BD, Kovacsovics-Bankowski M, Morris N, Walker E, Chisholm L, Floyd K, Walker J, Gonzalez I, Meeuwsen T, Fox BA, Moudgil T, Miller W, Haley D, Coffey T, Fisher B, Delanty-Miller L, Rymarchyk N, Kelly T, Crocenzi T, Bernstein E, Sanborn R, Urba WJ, Weinberg AD (2013) OX40 is a potent immune-stimulating target in late-stage cancer patients. Cancer Res 73 (24): 7189–7198.
Delyon J, Mateus C, Lefeuvre D, Lanoy E, Zitvogel L, Chaput N, Roy S, Eggermont AM, Routier E, Robert C (2013) Experience in daily practice with ipilimumab for the treatment of patients with metastatic melanoma: an early increase in lymphocyte and eosinophil counts is associated with improved survival. Ann Oncol 24 (6): 1697–1703.
Fecher LA, Agarwala SS, Hodi FS, Weber JS (2013) Ipilimumab and its toxicities: a multidisciplinary approach. Oncologist 18 (6): 733–743.
Gangadhar TC, Vonderheide RH (2014) Mitigating the toxic effects of anticancer immunotherapy. Nat Rev Clin Oncol 11 (2): 91–99.
Grosso JFHC, Inzunza D (2013) Association of tumor PD-L1 expression and immune biomarkers with clinical activity in patients (pts) with advanced solid tumors treated with nivolumab (anti-PD-1; BMS-936558; ONO-4538). The Annual Meeting of the American Society of Clinical Oncology, Chicago, USA. J Clin Oncol 31 (Suppl): abstr 3016.
Hamid O, Robert C, Daud A, Hodi FS, Hwu WJ, Kefford R, Wolchok JD, Hersey P, Joseph RW, Weber JS, Dronca R, Gangadhar TC, Patnaik A, Zarour H, Joshua AM, Gergich K, Elassaiss-Schaap J, Algazi A, Mateus C, Boasberg P, Tumeh PC, Chmielowski B, Ebbinghaus SW, Li XN, Kang SP, Ribas A (2013) Safety and tumor responses with lambrolizumab (anti-PD-1) in melanoma. N Engl J Med 369 (2): 134–144.
Hamid OSJ, Lawrence DP (2012) Clinical activity, safety, and biomarkers with MPDL32801A, an engineered anti-PDL1 antibody in patients with locally advanced or metastatic malignant melanoma. J Clin Oncol 31 (Suppl): abstr 9010.
Hodi FS, Mihm MC, Soiffer RJ, Haluska FG, Butler M, Seiden MV, Davis T, Henry-Spires R, MacRae S, Willman A, Padera R, Jaklitsch MT, Shankar S, Chen TC, Korman A, Allison JP, Dranoff G (2003) Biologic activity of cytotoxic T lymphocyte-associated antigen 4 antibody blockade in previously vaccinated metastatic melanoma and ovarian carcinoma patients. Proc Natl Acad Sci USA 100: 4712–4717.
Hodi FS, O'Day SJ, McDermott DF, Weber RW, Sosman JA, Haanen JB, Gonzalez R, Robert C, Schadendorf D, Hassel JC, Akerley W, van den Eertwegh AJ, Lutzky J, Lorigan P, Vaubel JM, Linette GP, Hogg D, Ottensmeier CH, Lebbé C, Peschel C, Quirt I, Clark JI, Wolchok JD, Weber JS, Tian J, Yellin MJ, Nichol GM, Hoos A, Urba WJ (2010) Improved survival with ipilimumab in patients with metastatic melanoma. N Engl J Med 363 (8): 711–723.
Keir ME, Butte MJ, Freeman GJ, Sharpe AH (2008) PD-1 and its ligands in tolerance and immunity. Annu Rev Immunol 26: 677–704.
Ku GY, Yuan J, Page DB, Schroeder SE, Panageas KS, Carvajal RD, Chapman PB, Schwartz GK, Allison JP, Wolchok JD (2010) Single-institution experience with ipilimumab in advanced melanoma patients in the compassionate use setting: lymphocyte count after 2 doses correlates with survival. Cancer 116 (7): 1767–1775.
Lin W, Voskens CJ, Zhang X, Schindler DG, Wood A, Burch E, Wei Y, Chen L, Tian G, Tamada K, Wang LX, Schulze DH, Mann D, Strome SE (2008) Fc-dependent expression of CD137 on human NK cells: insights into "agonistic" effects of anti-CD137 monoclonal antibodies. Blood 112 (3): 699–707.
Lipson EJ, Sharfman WH, Drake CG, Wollner I, Taube JM, Anders RA, Xu H, Yao S, Pons A, Chen L, Pardoll DM, Brahmer JR, Topalian SL (2013) Durable cancer regression off-treatment and effective reinduction therapy with an anti-PD-1 antibody. Clin Cancer Res 19 (2): 462–468.
Lynch TJ, Bondarenko I, Luft A, Serwatowski P, Barlesi F, Chacko R, Sebastian M, Neal J, Lu H, Cuillerot JM, Reck M (2012) Ipilimumab in combination with paclitaxel and carboplatin as first-line treatment in stage IIIB/IV non-small-cell lung cancer: results from a randomized, double-blind, multicenter phase II study. J Clin Oncol 30 (17): 2046–2054.
Mallett S, Fossum S, Barclay AN (1990) Characterization of the MRC OX40 antigen of activated CD4 positive T lymphocytes–a molecule related to nerve growth factor receptor. EMBO J 9 (4): 1063–1068.
Nirschl CJ, Drake CG (2013) Molecular pathways: coexpression of immune checkpoint molecules: signaling pathways and implications for cancer immunotherapy. Clin Cancer Res 19 (18): 4917–4924.
Page DB, Postow MA, Callahan MK, Allison JP, Wolchok JD (2014) Immune modulation in cancer with antibodies. Annu Rev Immunol 65: 185–202.
Parry RV, Chemnitz JM, Frauwirth KA, Lanfranco AR, Braunstein I, Kobayashi SV, Linsley PS, Thompson CB, Riley JL (2005) CTLA-4 and PD-1 receptors inhibit T-cell activation by distinct mechanisms. Mol Cell Biol 25 (21): 9543–9553.
Patnaik AKS, Tolcher AW (2012) Phase I study of MK-3475 (anti-PD-1 monoclonal antibody) in patients with advanced solid tumors. J Clin Oncol 30: 2512.
Postow MA, Callahan MK, Barker CA, Yamada Y, Yuan J, Kitano S, Mu Z, Rasalan T, Adamow M, Ritter E, Sedrak C, Jungbluth AA, Chua R, Yang AS, Roman RA, Rosner S, Benson B, Allison JP, Lesokhin AM, Gnjatic S, Wolchok JD (2012) Immunologic correlates of the abscopal effect in a patient with melanoma. N Engl J Med 366 (10): 925–931.
Postow MAYJ, Panageas KS (2012) Evaluation of the absolute lymphocyte count as a biomarker for melanoma patients treated with the commercially available dose of ipilimumab (3 mg/kg). The American Society of Clinical Oncology Annual Meeting, Chicago, USA. J Clin Oncol 30 (Suppl): abstr 8595.
Ribas A, Hanson DC, Noe DA, Millham R, Guyot DJ, Bernstein SH, Canniff PC, Sharma A, Gomez-Navarro J (2007) Tremelimumab (CP-675,206), a cytotoxic T lymphocyte associated antigen 4 blocking monoclonal antibody in clinical development for patients with cancer. Oncologist 12 (7): 873–883.
Ribas A, Hodi FS, Callahan M, Konto C, Wolchok J (2013) Hepatotoxicity with combination of vemurafenib and ipilimumab. N Engl J Med 368 (14): 1365–1366.
Ribas A, Kefford R, Marshall MA, Punt CJ, Haanen JB, Marmol M, Garbe C, Gogas H, Schachter J, Linette G, Lorigan P, Kendra KL, Maio M, Trefzer U, Smylie M, McArthur GA, Dreno B, Nathan PD, Mackiewicz J, Kirkwood JM, Gomez-Navarro J, Huang B, Pavlov D, Hauschild A (2013) Phase III randomized clinical trial comparing tremelimumab with standard-of-care chemotherapy in patients with advanced melanoma. J Clin Oncol 31 (5): 616–622.
Robert C, Thomas L, Bondarenko I, O'Day S, M DJ, Garbe C, Lebbe C, Baurain JF, Testori A, Grob JJ, Davidson N, Richards J, Maio M, Hauschild A, Miller WH Jr, Gascon P, Lotem M, Harmankaya K, Ibrahim R, Francis S, Chen TT, Humphrey R, Hoos A, Wolchok JD (2011) Ipilimumab plus dacarbazine for previously untreated metastatic melanoma. N Engl J Med 364 (26): 2517–2526.
Schindler KHK, Postow MA (2013) Pretreatment levels of absolute and relative eosinophil count to improve oversall survival (OS) in patients with metastatic melanoma under treatment with ipilimumab, an anti-CTLA-4 antibody. The Annual Meeting of the American Society of Clinical Oncology. Chicagi, USA. J Clin Oncol 31 (Suppl): abstr 9024.
Tchekmedyian SGJ, Korman A, Keler T, Deo Y, Davis TA (eds) (2002) MDX-010 (human anti-CTLA4): a phase I trial in malignant melanoma. The American Society of Clinical Oncology Annual Meeting. The American Society of Clinical Oncology: Virginia, USA.
Topalian SL, Hodi FS, Brahmer JR, Gettinger SN, Smith DC, McDermott DF, Powderly JD, Carvajal RD, Sosman JA, Atkins MB, Leming PD, Spigel DR, Antonia SJ, Horn L, Drake CG, Pardoll DM, Chen L, Sharfman WH, Anders RA, Taube JM, McMiller TL, Xu H, Korman AJ, Jure-Kunkel M, Agrawal S, McDonald D, Kollia GD, Gupta A, Wigginton JM, Sznol M (2012) Safety, activity, and immune correlates of anti-PD-1 antibody in cancer. N Engl J Med 366 (26): 2443–2454.
Weber JS, Kahler KC, Hauschild A (2012) Management of immune-related adverse events and kinetics of response with ipilimumab. J Clin Oncol 30 (21): 2691–2697.
Westin JR, Chu F, Zhang M, Fayad LE, Kwak LW, Fowler N, Romaguera J, Hagemeister F, Fanale M, Samaniego F, Feng L, Baladandayuthapani V, Wang Z, Ma W, Gao Y, Wallace M, Vence LM, Radvanyi L, Muzzafar T, Rotem-Yehudar R, Davis RE, Neelapu SS (2014) Safety and activity of PD1 blockade by pidilizumab in combination with rituximab in patients with relapsed follicular lymphoma: a single group, open-label, phase 2 trial. Lancet Oncol 15 (1): 69–77.
Wolchok JD, Hoos A, O'Day S, Weber JS, Hamid O, Lebbe C, Maio M, Binder M, Bohnsack O, Nichol G, Humphrey R, Hodi FS (2009) Guidelines for the evaluation of immune therapy activity in solid tumors: immune-related response criteria. Clin Cancer Res 15 (23): 7412–7420.
Wolchok JD, Kluger H, Callahan MK, Postow MA, Rizvi NA, Lesokhin AM, Segal NH, Ariyan CE, Gordon RA, Reed K, Burke MM, Caldwell A, Kronenberg SA, Agunwamba BU, Zhang X, Lowy I, Inzunza HD, Feely W, Horak CE, Hong Q, Korman AJ, Wigginton JM, Gupta A, Sznol M (2013) Nivolumab plus ipilimumab in advanced melanoma. N Engl J Med 369 (2): 122–133.
Wolchok JD, Neyns B, Linette G, Negrier S, Lutzky J, Thomas L, Waterfield W, Schadendorf D, Smylie M, Guthrie T Jr, Grob JJ, Chesney J, Chin K, Chen K, Hoos A, O'Day SJ, Lebbé C (2010) Ipilimumab monotherapy in patients with pretreated advanced melanoma: a randomised, double-blind, multicentre, phase 2, dose-ranging study. Lancet Oncol 11 (2): 155–164.
Yang JC, Hughes M, Kammula U, Royal R, Sherry RM, Topalian SL, Suri KB, Levy C, Allen T, Mavroukakis S, Lowy I, White DE, Rosenberg SA (2007) Ipilimumab (anti-CTLA4 antibody) causes regression of metastatic renal cell cancer associated with enteritis and hypophysitis. J Immunother 30 (8): 825–830.
Yang YF, Zou JP, Mu J, Wijesuriya R, Ono S, Walunas T, Bluestone J, Fujiwara H, Hamaoka T (1997) Enhanced induction of antitumor T-cell responses by cytotoxic T lymphocyte-associated molecule-4 blockade: the effect is manifested only at the restricted tumor-bearing stages. Cancer Res 57 (18): 4036–4041.
Author information
Authors and Affiliations
Corresponding author
PowerPoint slides
Rights and permissions
This work is licensed under the Creative Commons Attribution-NonCommercial-Share Alike 3.0 Unported License. To view a copy of this license, visit http://creativecommons.org/licenses/by-nc-sa/3.0/
About this article
Cite this article
Naidoo, J., Page, D. & Wolchok, J. Immune modulation for cancer therapy. Br J Cancer 111, 2214–2219 (2014). https://doi.org/10.1038/bjc.2014.348
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/bjc.2014.348
Keywords
This article is cited by
-
Treatment-related pneumonitis after thoracic radiotherapy/chemoradiotherapy combined with anti-PD-1 monoclonal antibodies in advanced esophageal squamous cell carcinoma
Strahlentherapie und Onkologie (2024)
-
Differential Leukocyte MicroRNA Responses Following Pan T Cell, Allorecognition and Allosecretome-Based Therapeutic Activation
Archivum Immunologiae et Therapiae Experimentalis (2021)
-
Progress in the diagnosis and treatment of extensive-stage small cell lung cancer
Oncology and Translational Medicine (2019)
-
Transcriptional analysis of immune genes in Epstein–Barr virus-associated gastric cancer and association with clinical outcomes
Gastric Cancer (2018)
-
The Society for Immunotherapy of Cancer consensus statement on immunotherapy for the treatment of non-small cell lung cancer (NSCLC)
Journal for ImmunoTherapy of Cancer (2018)