Abstract
Background:
Although T-cell immunity is thought to be involved in the prognosis of epithelial ovarian cancer (EOC) patients, immunosuppressive conditions hamper antitumour immune responses. Thus, their mechanisms and overcoming strategies need to be investigated.
Methods:
The role of NF-κB in human EOC cells and macrophages was evaluated by in vitro production of immunosuppressive IL-6 and IL-8 by EOC cells and in vivo analysis of immune responses in nude mice implanted with human EOC cells using an NF-κB inhibitor DHMEQ.
Results:
In EOC patients, increased plasma IL-6, IL-8, and arginase were observed. The NF-κB inhibitor DHMEQ inhibited the production of IL-6 and IL-8 by EOC cell lines. Immunosuppression of human DCs and macrophages by culture supernatant of EOC cells was reversed with the pretreatment of DHMEQ. Administration of DHMEQ to nude mice implanted with human EOC resulted in the restoration of T-cell stimulatory activity of murine DCs along with the reduction of tumour accumulation and arginase expression of MDSCs. Nuclear factor-κB inhibition in tumour-bearing mice also enhanced antitumour effects of transferred murine naive T cells.
Conclusions:
NF-κB is involved in the immunosuppression induced by human EOC, and its inhibitor may restore antitumour immune responses, indicating that NF-κB is an attractive target for EOC treatment.
Similar content being viewed by others
Main
Among gynaecological malignancies, epithelial ovarian cancer (EOC) is the leading cause of death due to dissemination or metastasis at diagnosis (Greenlee et al, 2001). The standard of care for EOC patients includes surgical cytoreduction followed by chemotherapy. However, recurrence frequently occurs, and recurrent tumours respond poorly to currently available treatments. Therefore, new therapeutic strategies are needed for EOC patients.
Recent research has suggested that CD8+ T-cell infiltration into tumours is not only an independent prognostic biomarker but also an important factor for responses to conventional chemotherapies and immunotherapies (Fridman et al, 2011). Epithelial ovarian cancer patients with high infiltration of CD4+ and CD8+ T cells into tumours have better prognoses, suggesting possible involvement of T-cell responses in controlling EOC (Hamanishi et al, 2011; Hwang et al, 2012). However, previous immunotherapies, including p53 peptide vaccination, have shown only limited clinical responses in patients with recurrent EOC (Leffers et al, 2009). One of the major reasons for the insufficient response to immunotherapy is thought to be immunosuppression in cancer patients (Yaguchi et al, 2011). In the tumour microenvironment, cancer cells produce various immunosuppressive cytokines, including interleukin (IL)-6, IL-10, VEGF, CCL2, and TGF-β, which subsequently impair dendritic cell (DC) ability to stimulate antitumour T cells, and induce various immunosuppressive cells such as myeloid-derived suppressor cells (MDSCs), tolerogenic DCs, and regulatory T cells (Tregs) (Kawakami et al, 2004; Sumimoto et al, 2006; Yaguchi et al, 2011). Therefore, it is important to elucidate molecular mechanism of the immunosuppression by EOC, and to develop strategies to restore immunocompetence in EOC patients.
Various mechanisms leading to immunosuppression in cancer patients have been reported; however, little information has been available regarding which pathways are important and whether or not the immunosuppressive state could be reversed by the signal inhibitors. We have previously reported that oncogene activation triggers various immunosuppressive cascades leading to the immunosuppressive tumour microenvironment. For examples, mutant BRAFV600E, activated STAT3, or activated β-catenin in human melanoma cells induces immunosuppression on DCs through the production of various immunosuppressive cytokines such as IL-10, IL-6, and VEGF, and their downregulation by RNA interference or specific inhibitors reduces immunosuppressive activity of human melanoma cells (Sumimoto et al, 2006; Iwata-Kajihara et al, 2011; Yaguchi et al, 2012). As activated oncogenic pathways vary among human cancers, further investigation on the immunosuppressive mechanism and the strategy for its reversal is important for the development of effective cancer treatment.
In this study, we have evaluated the role of NF-κB in the immunosuppression caused by human EOC. Nuclear factor-κB is a pleiotropic transcription factor and has important roles in cancer cell proliferation, survival, angiogenesis, drug resistance, and inflammation in cancer patients (Karin and Greten, 2005; Karin, 2006; Baud and Karin, 2009; Grivennikov and Karin, 2010; He and Karin, 2010). However, the roles of NF-κB in the EOC-induced immunosuppression has not been extensively studied (Cubillos-Ruiz et al, 2010). We have found that human EOC cells produce high levels of IL-6 and IL-8 through constitutively activated NF-κB signalling. These cytokines, IL-6 through the impairment of DC stimulation of antitumour T cells and expansion of immunosuppressive MDSCs, and IL-8 through a possible increase of immunosuppressive arginase (Raber et al, 2012), may induce immunosuppressive conditions in EOC patients. An NF-κB inhibitor, dehydroxymethylepoxyquinomicin (DHMEQ), had an activity that reversed the immunosuppression. These results demonstrate that altered NF-κB signalling is involved in the immunosuppression of EOC patients, together with the previously reported malignant features such as cancer cell proliferation and survival (Karin, 2006). Therefore, NF-κB is an attractive target for the development of new diagnostic and therapeutic modalities for EOC patients.
Materials and methods
Cell culture
Human EOC cell line JHOC-5 was kindly provided by Dr Kazunori Ochiai (Jikei University, Tokyo, Japan). Cell lines RMG-I, RMG-II, RMG-V, RMUG-L, and RMUG-S were established and maintained at our laboratory. JHOS-2 was purchased from RIKEN Bioresource Center Cell Bank (Tsukuba, Japan). OVCAR3 and OVK18 were purchased from the American Type Culture Collection (Rockville, MD, USA). Cell lines JHOC-5, RMG-I, RMG-II, and RMG-V were clear-cell subtypes, JHOS-2 and OVCAR3 were serous subtypes, RMUG-S and RMUG-L were mucinous subtypes and OVK18 was endometrioid subtype. Cells were grown in Dulbecco’s modified Eagle’s medium (DMEM)/F12 (JHOC-5, RMG-II, JHOS-2, RMUG-L, and RMUG-S), RPMI-1640 (OVCAR3 and OVK18), or F12 (RMG-I) supplemented with 10% heat-inactivated FBS, 100 μg ml−1 streptomycin (Life Technologies Inc., Grand Island, NY, USA), and 100 IU ml−1 penicillin (Life Technologies Inc.). The cell lines used in our study were authenticated by short tandem repeat profiling on January 2012.
Patients and clinical samples
All tissue samples of EOC were fixed in neutral-buffered formalin and embedded in paraffin. Plasmas were obtained from 37 EOC patients and 19 age-matched female healthy donors. The bloods taken from EOC 37 patients on the day of surgery were immediately centrifuged and plasmas were stored at −80 °C. The plasma of the healthy donors was similarly collected at the outpatient setting in the morning. Plasma human IL-6 and IL-8 was measured by ELISAs (BD Biosciences Pharmingen). Data were collected from clinical and pathological records with informed consent from patients following approval by the Institutional Review Board of Keio University School of Medicine (No. 20130118).
DHMEQ
Racemic DHMEQ was developed and kindly provided by Dr Kazuo Umezawa. It was dissolved in dimethylsulphoxide (DMSO; Wako Chemicals, Osaka, Japan) at a stock concentration of 10 mg ml−1, and then stored at –20 °C. The stock solution was subsequently diluted in culture medium to a final DMSO concentration of <1%.
Immunohistochemistry
Human ovarian cancer clinical samples embedded in paraffin blocks were cut into 4-μm-thick sections. Immunohistochemistry was performed as described previously (Goto et al, 2008) using anti-human p65 (Santa Cruz Biotechnology) and IL-6 (R&D Systems) antibodies. Negative controls were stained with nonspecific IgG. Immunohistochemical data were evaluated microscopically by a gynaecologic pathology specialist blinded to the patient outcomes. The results of p65 and IL-6 immunostaining were interpreted as positive if 25% or more of tumour cells exhibited cytoplasmic or nuclear staining.
Preparation of nuclear extracts and NF-κB transcription activation assay
For total cell extracts, adherent cancer cells were washed once with PBS, detached with trypsin, and collected in the culture medium. Nuclear extracts were prepared according to a previously reported method with some modification (Sumimoto et al, 2006). In brief, attached cells were harvested and washed with PBS, resuspended in 400 μl buffer A (10 mM HEPES, pH 7.9, 10 mM KCl, 1.5 mM MgCl2, 0.5 mM dithiothreitol, 0.5 mM phenylmethylsulphonyl fluoride, and 0.1% Nonidet P-40), and incubated on ice for 20 min. Nuclei were pelleted by centrifugation at 15 000 g for 15 min at 4 °C, resuspended in buffer C (20 mM HEPES, pH 7.9, 420 nM NaCl, 1.5 mM MgCl2, 1 mM dithiothreitol, 0.2 mM EDTA, 0.5 mM phenylmethylsulphonyl fluoride, and 20% glycerol), incubated on ice for 20 min, and then centrifuged at 150 000 g for 15 min at 4 °C. Nuclear extracts were stored at –80 °C. Nuclear factor-κB transcription activities in nuclear extracts of EOC cell lines were measured using an NF-κB Transcription Factor Microplate Assay (Marilgen Biosciences) according to the manufacturer’s instructions.
ELISAs and quantification of IL-6/IL-8 expression
To evaluate in vitro secretion of IL-6 and IL-8 by EOC cell lines, 5 × 105 cells were seeded into individual wells of a six-well plate. After 24 h of incubation, culture supernatants were collected and 2 ml of the culture medium with 10% FBS and various concentrations of DHMEQ (0, 5, and 10 μg ml−1) were added to each well. After 4 h of incubation, culture supernatants were aspirated and 2 ml of culture medium with 10% FBS and the same DHMEQ concentration was added to each well. After a further 4 h of incubation, cells and supernatants were collected and tested for the presence of human IL-6 and IL-8 by ELISAs (BD Biosciences Pharmingen), and nuclear extracts were prepared. Reverse transcription–polymerase chain reaction was performed using TaqMan probes (Applied Biosystems) for IL-6, IL-8, and GAPDH. A relative quantitative method was applied for the target mRNA that was normalised to the level of control GAPDH mRNA.
Monocyte-derived DC differentiation and monocyte-derived suppressive macrophage differentiation
Monocyte-derived DCs (Mo-DCs) were generated as described previously (Sumimoto et al, 2006) (Yaguchi et al, 2012). Briefly, human CD14+ monocytes were cultured with GM-CSF and IL-4, and with or without 20% (vol vol−1) culture supernatants from JHOC-5 cells pretreated with or without DHMEQ (5 μg ml−1). DHMEQ-pretreated JHOC-5 culture supernatants were dialysed to remove residual DHMEQ. Mouse anti-human IL-6 monoclonal antibody (R&D Systems) with the concentration of 1 μg ml−1 was added for the neutralisation of human IL-6 in the culture supernatant of JHOC-5 cells. On day 5, Mo-DCs were washed, reseeded, and stimulated with 1 μg ml−1 LPS. On day 6, culture supernatants were collected to measure IL-10, IL-12, and TNF-α by ELISAs (BD Biosciences Pharmingen), and Mo-DCs were analysed by flow cytometry. Antibodies against the following markers were used for staining: human CD1a, CD14, CD40, CD80, CD83, CD86, HLA-DR (Beckman Coulter, Brea, CA, USA), and PD-L1 (eBioscience).
Human monocyte-derived macrophages were generated as follows. Human CD14+ monocytes were cultured with 20% (vol vol−1) volumes of culture supernatants from JHOC-5 cells with various concentrations of DHMEQ (0, 1.25, 2.5, and 5 μg ml−1) to evaluate NF-κB-dependent suppressive effects. On day 2, cultured cells and remaining DHMEQ were washed, cells were detached, and, after adjusting cell numbers by counting, reseeded with allogeneic CD3+ T cells in the arginine-contained media. Arginase activity in macrophage lysates was measured using an Arginase Assay Kit (BioAssay Systems) following the manufacturer’s instructions.
Xenograft mouse model of ovarian cancer
All procedures involving animals and their care were approved by the animal care committee of Keio University in accordance with institutional and Japanese government guidelines for animal experiments. Mice were housed at a constant temperature and humidity under pathogen-free conditions, and received a standard diet and water. JHOC-5 cells (5 × 106) resuspended in DMEM/F12 were injected subcutaneously into the right flank of 6–8-week-old female BALB/c-nu/nu mice (CLEA, Tokyo, Japan). Six mice were included in each group. Mice received intraperitoneal injections of DHMEQ (5 mg kg−1) or DMSO (control group) diluted in RPMI-1640 medium every day from day 10 after tumour implantation until 2 days before being killed (day 31). Tumour volume measurements were performed with calipres by measuring the largest diameter and perpendicular length. Tumour volumes were calculated according to the following formula: 1/2 × (largest diameter) × (perpendicular diameter)2. At several occasions, mice sera were collected to measure human IL-6 by ELISA. Mice were killed on day 33, and tumours and spleens were harvested and mechanically dispersed into single-cell suspensions for assays.
Mixed leucocyte reaction and in vivo functional analysis of splenic DCs
Irradiated (32 Gy) 1.6 × 104 Mo-DCs and 1.6 × 105 allogeneic CD3+ T cells were cocultured in 96-well plates. On day 5, IFN-γ was measured by ELISA (BD Biosciences Pharmingen). On the same day, T-cell proliferation was measured by BrdU incorporation (Cell proliferation ELISA, BrdU kit; Roche). BrdU was added and incubated for 24 h after 5 days of culture. For T-cell IFN-γ release assays, irradiated DCs (1.6 × 104/200 μl per well) purified from nude mouse spleens using CD11c MACS beads (Miltenyi Biotec) were cocultured in 96-well plates with splenic T cells (1.6 × 105/200 μl per well) purified from BALB/c mice using CD90.2 MACS beads (Miltenyi Biotec), and stimulated with an anti-CD3 antibody (1 μg per ml) (BD Biosciences Pharmingen). After 5 days of incubation, IFN-γ and T-cell proliferation were measured as described above.
Flow cytometric analysis of MDSCs
Single-cell suspensions from spleens or tumours were stained with PE-conjugated rat anti-mouse Gr-1, fluorescein isothiocyanate (FITC)-conjugated rat anti-mouse CD11b, PE-conjugated rat anti-mouse F4/80, or FITC-conjugated rat anti-mouse CD11c antibodies (all purchased from BD Biosciences). Isotype-matched antibodies were used as controls. Samples were analysed using the Gallios and the Kaluza software (Beckman Coulter).
Cell isolation and arginase assay
Following tumour resection, tumours were washed in sterile RPMI-1640, and scissors were used to cut them into 1 mm3 fragments in a solution of type IV collagenase (1.4 mg ml−1) (Sigma, St. Louis, MO, USA) and DNase (0.3 KU ml−1) (Sigma). Tumour fragments were incubated in flasks with slow, continuous shaking at 37 °C for 60 min. Cell suspensions were then passed through Nytex filters. CD11b+ cells from tumour sites were purified using mouse CD11b MACS beads (Miltenyi Biotech).
Arginase activity was measured in CD11b+ cell lysates and ovarian patient plasma using an Arginase Assay Kit (BioAssay Systems) following the manufacturer’s instructions.
Adoptive cell transfer of murine T cells
At 6–8 weeks of age, nude mice were injected subcutaneously with 5 × 106 JHOC-5 cells. At 12 days after tumour inoculation, mice were treated with DHMEQ intraperitoneal injections daily. On day 17, mice received intravenous adoptive transfer of 2 × 106 splenic CD90.2+ naive T cells from syngeneic BALB/c mice. DHMEQ intraperitoneal injections were performed until day 28. Each treatment group included a minimum of seven mice. Serial tumour measurements were obtained and serum IL-6 levels were measured.
Statistical analysis
Statistical analysis was performed with the Student’s two-tailed t-test and Fisher’s exact test using SPSS ver. 21.0 (IBM Co., Armonk, NY, USA). Statistical significance was accepted at P<0.05.
Results
NF-κB-dependent production of IL-6 and IL-8 by human EOC cells
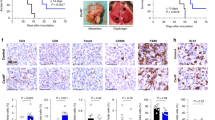
Production of IL-6 and IL-8, which have been previously shown to be produced by EOC cells (Ivarsson et al, 2000; Nilsson et al, 2005), was first evaluated in various human EOC cell lines. Among nine EOC cell lines tested, three clear cell lines, JHOC-5, RMG-I, and RMG-II, were found to produce high amounts of both IL-6 and IL-8 when measured by ELISA (Figure 1A). In addition, JHOC-5 and RMG-I cells exhibited a high NF-κB transcriptional activity (Figure 1B). Interleukin-6 and IL-8 were elevated in the plasma of EOC patients compared with that in healthy donors (Figure 1C). Immunohistochemical analysis of human EOC tissue samples showed that IL-6 and NF-κB (p65) expression in the cytoplasm and nuclei of EOC cells was positively correlated with each other (P=0.033) (Figure 1D and Table 1). These observations indicate that constitutively activated NF-κB signalling may be involved in the high production of IL-6 and IL-8 by human EOC cells, especially in clear-cell lines. Discrepancy between cytokine production and NF-κB activity measured by the Microplate Assay was observed in some cell lines, possibly because this assay detects various NF-κB-related molecules other than p65, which was correlated with IL-6 production (Figure 1D and Table 1).
NF- κ B-dependent production of IL-6 and IL-8 by human EOC cells. (A) Both IL-6 and IL-8 production was highly elevated in EOC cell lines JHOC-5, RMG-I, and RMG-II when culture supernatants were measured by ELISA. (B) DNA-binding activity of NF-κB p65 in nuclear lysates of EOC cell lines was measured. A correlation between IL-6 production and NF-κB activation was observed in JHOC-5 and RMG-I cell lines. (C) IL-6 (left) and IL-8 (right) in plasma obtained from EOC patients (n=24) and healthy donors (n=14) were measured by ELISA. Both IL-6 and IL-8 levels were higher in EOC patients than those in healthy donors. *P<0.05. All results are representative of three independent experiments. (D) Representative immunohistochemical results of NF-κB (p65) and IL6 staining of EOC tissue samples. A representative case with both NF-κB (p65) positive and IL-6 positive is shown (Pt.1). A representative case with NF-κB (p65) positive and IL-6 negative (Pt. 2). A representative case with both NF-κB (p65) negative and IL-6 negative (Pt.3). The results of p65 and IL-6 immunostaining were interpreted as positive if 25% or more of tumour cells exhibited cytoplasmic or nuclear staining. Sections were counterstained via Gill’s haematoxylin. Scale bar indicates 25 μm.
To confirm NF-κB-dependent production of IL-6 and IL-8, we tested the effects of an NF-κB inhibitor, DHMEQ. As shown in Figure 2A, DHMEQ significantly inhibited the production of both IL-6 and IL-8 by JHOC-5 and RMG-I cells, which was accompanied by a significant decrease of NF-κB transcriptional activity (Figure 2B) without affecting cell viability, proliferation or production of other cytokines such as VEGF and TGF-β1 (data not shown). Interleukin-6 and IL-8 production was transcriptionally inhibited by DHMEQ treatment as shown by the decrease of IL-6 and IL-8 mRNA in real-time PCR analyses (Figure 2C). Therefore, activated NF-κB signalling induces high production of IL-6 and IL-8 in human EOC cells.
IL-6 and IL-8 production by NF- κ B activation is reduced by DHMEQ treatment. (A) IL-6 and IL-8 production by JHOC-5 and RMG-I cell lines was reduced when DHMEQ was added in cell culture. (B) DNA-binding activity of NF-κB (p65) in nuclear lysates of JHOC-5 and RMG-I cells was also inhibited when DHMEQ was added in cell culture. (C) mRNA expression of IL-6 and IL-8 in JHOC-5 and RMG-I cells was inhibited by DHMEQ treatment. All results are representative of five independent experiments. Error bars indicate s.d. *P<0.05.
EOC cells produce suppressive factors for the generation of Mo-DCs in an NF-κB-dependent manner
We have previously reported that immunosuppressive cytokines, including IL-6, IL-10, and VEGF produced by human melanoma cell lines with activated mitogen-activated protein kinase signalling via BRAF mutation, cause impairment of human Mo-DCs (Sumimoto et al, 2006). In this study, we evaluated whether human EOC-derived factors produced in an NF-κB-dependent manner also impaired DC functions. The addition of culture supernatants from JHOC-5 cells to 5-day cultures of Mo-DC generation (20% final volume) from CD14+ peripheral blood monocytes in the presence of IL-4 and GM-CSF resulted in the generation of MO-DCs with a lower T-cell stimulatory activity than that of DCs without the addition of EOC supernatants when T-cell stimulatory activity was measured by IFN- γ secretion and proliferation of allogeneic T cells (Figure 3A). However, such a DC suppressive activity of culture supernatants was significantly reduced by pretreatment of JHOC-5 cells with DHMEQ. Addition of a neutralising anti-IL-6 antibody in the culture supernatants of JHOC-5 cells partially restored the DC activity, indicating that IL-6 is one of the molecules responsible for DC suppression by EOC-derived factors, and other factors also appear to be involved in the suppression (Figure 3A).
EOC cells produce suppressive factors for the generation of Mo-DCs in an NF- κ B-dependent manner. (A) Human Mo-DCs with a lower T-cell stimulatory activity was generated from CD14+ peripheral blood monocytes when cultured with culture supernatants (CS) of JHOC-5 cells. However, pretreatment of JHOC-5 cells with DHMEQ (5 μg ml−1) or addition of anti-IL6 Ab in the DC generation culture restored DC activity to stimulate T cells. T-cell stimulatory activity was evaluated by IFN-γ production of T cells (left) and BrdU proliferation (right) in allogeneic MLR assays. In the experiments, residual DHMEQ in EOC culture supernatants was removed by dialysis before adding to the DC generation cultures to avoid direct DHMEQ effects on DC. Data are representative of four independent experiments. (B) IL-12 production by LPS-stimulated human Mo-DCs (B, left) was increased, and IL-10 production (B, right) was decreased when DCs were generated from CD14+ monocytes with culture supernatants of JHOC-5 cells. However, pretreatment of JHOC-5 cells with DHMEQ (5 μg ml−1) or addition of anti-IL6 Ab in the DC generation culture restored IL12 production by Mo-DCs and reduced IL10 production. Error bars indicate s.d. Data are representative of three independent experiments. *P<0.05.
Compared with DCs generated with culture supernatants of untreated JHOC-5 cells, IL-12 production was increased and IL-10 production was decreased when DCs were generated in cultures with supernatants of DHMEQ-pretreated JHOC-5 cells (Figure 3B). In this experiment, residual DHMEQ in EOC culture supernatants was removed by dialysis before adding to the DC generation cultures to avoid direct DHMEQ effects on DC. Addition of a neutralising anti-IL-6 antibody in the culture supernatants of JHOC-5 cells partially recovered IL-12 production by DCs, indicating that IL-6 and other factors are involved in the generation of DCs with decreased IL-12 production. These results indicate that human EOC cells produce NF-κB-dependent suppressive factors including IL-6 in the generation of high IL-10-producing DCs with impaired IL-12 production and T-cell stimulatory activities, and that the NF-κB inhibitor is able to restore the generation of DCs with a T-cell stimulatory activity.
NF-κB signalling is involved in the generation of immunosuppressive human macrophages induced by EOC cell-derived factors
Next, we evaluated the role of NF-κB in the generation of immunosuppressive human macrophages. Macrophages with a suppressive activity on T-cell proliferation could be generated by culturing human peripheral blood monocytes for 2 days in the presence of EOC culture supernatants (Figure 4A). The viability of macrophages was not affected by DHMEQ. Following induction of the macrophages, DHMEQ was washed away and, after adjusting cell numbers by counting, the macrophage was cocultured with allogeneic T cells. Addition of DHMEQ to macrophage cultures resulted in the generation of macrophages with a lower T-cell suppressive activity along with less production of arginase, which has an immunosuppressive activity on T cells via depletion of arginine (Figure 4A), indicating that NF-κB in monocytes appears to be involved in the generation of immunosuppressive macrophages producing immunosuppressive arginase, and NF-κB inhibitor has an ability to prevent such an effect.
NF- κ B signalling is involved in the generation of immunosuppressive human macrophages induced by EOC cell-derived factors, and IL-8 is possibly involved in the increase of arginase in EOC patients. (A) Human monocyte-derived suppressor (MoS) macrophages with ariginase production (right), which suppressed T-cell proliferation in allogeneic MLR assays (measured by BrdU incorporation) were generated from CD14+ monocytes by culture with EOC culture supernatants (left). However, addition of DHMEQ in the macrophage culture reduced T-cell suppressive activity (right) and arginase expression (left) in a dose-dependent manner. Data are representative of four independent experiments. Error bars indicate s.d. *P<0.05. (B) Higher arginase activity in the plasma of EOC patients (n=24) was observed than that of healthy donors (n=14). *P<0.05. (C) Positive correlation of plasma arginase activity with plasma IL-8 levels (left) (P<0.05), but not with plasma IL-6 levels (right) was observed in EOC patients.
Possible involvement of IL-8 in the increase of arginase in EOC patients
We investigated the possibility that EOC-derived IL-8 is also involved in the immunosuppression of EOC patients. Because IL-8 has been previously reported to promote secretion of arginase from neutrophils in lung cancer patients (Rotondo et al, 2009), we measured arginase activity in the plasma of EOC patients. Arginase activity was significantly higher in EOC patient plasma than that in healthy donor plasma (Figure 4B). The plasma arginase levels correlated with plasma IL-8 levels, but not plasma IL-6 levels (Figure 4C), indicating that EOC-derived IL-8 may also be involved in the immunosuppression via an increase of arginase in EOC patients.
In vivo immunosuppression in nude mice implanted with a human EOC cell line and its reversal by systemic administration of an NF-κB inhibitor
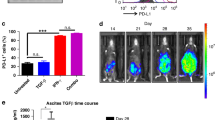
To investigate the in vivo effect of constitutively activated NF-κB signalling in human EOC, we used nude mice implanted with the human EOC cell line JHOC-5, because murine ovarian cancer cell lines producing high amounts of IL-6 in an NF-κB-dependent manner was not available, and human IL-6 binds to murine IL6R and has a biological activity on murine cells, while murine IL-6 does not have an activity on the human cells (van Dam et al, 1993). Interleukin -6 production was detected in sera from JHOC-5 cell-implanted nude mice, although murine IL-6 was not detected. Intraperitoneal administration of 5 mg of DHMEQ every day from day 14 after EOC cell inoculation did not affect tumour growth in each group (Figure 5A), but the serum IL-6 level was reduced in the DHMEQ-treated group on the day of being killed (Figure 5B). To avoid immunological effects by tumour size difference, we intentionally set up the condition in which 5 mg of DHMEQ inhibits IL-6 production without affecting tumour volume until day 32 of tumour inoculation. In this setting, MDSC did not appear to be essential in tumour growth, although administration of 10 mg DHMEQ inhibited tumour growth possibly by multiple mechanisms including direct tumour effects (data not shown). The numbers of CD11b+Gr-1+MDSCs including Gr-1high granulocytic MDSCs and Gr-1intermediate MDSCs were reduced in DHMEQ-treated mice (Figure 5C). The arginase activity of CD11b+MDSCs in tumours was also reduced in DHMEQ-treated mice (Figure 5D). Compared with untreated mice, splenic DCs in DHMEQ-treated mice showed a higher T-cell stimulatory activity when measured by IFN-γ secretion from autologous T cells with anti-CD3 simulation (Figure 5E). When CD90.2+ naive T cells were transferred into EOC cell-implanted nude mice, anti-tumour T cells capable of rejecting human EOC cells were induced in vivo (Figure 5F). In mice transferred with naive T cells, administration of DHMEQ intraperitoneally enhanced the antitumour effect of the transferred T cells compared with control DMSO administration. (Figure 5F). We have not clarified the tumour recognition mechanisms of the transferred naive murine T cells, although we hypothesise typical T-cell receptor-dependent recognition of xenogeneic MHC (HLA) on human EOC cells. These results indicated that human EOC cells induce immunosuppressive conditions in vivo through NF-κB-dependent mechanisms that impair both the T-cell stimulatory activity of DCs and expansion of arginase-producing MDSCs in the spleen and tumours. In addition, systemic administration of an appropriate dose of NF-κB inhibitor restores immunocompetence of cancer-bearing hosts through reversal of the immunosuppressive status of DCs and MDSCs without inhibiting induction of antitumour T-cell responses.
In vivo immunosuppression in nude mice implanted with a human EOC cell line and its reversal by administration of an NF- κ B inhibitor. (A) Tumour sizes of nude mice implanted with human EOC cell line, JHOC-5 were not different between mice with or without daily intraperitoneal (i.p.) administration of DHMEQ (5 mg kg−1 per day) during a 32-day experiment course. (B) Human IL-6 in serum was decreased on day 32 in the nude mice by DHMEQ administration. Error bars indicate s.d. Results were representative of six independent experiments. *P<0.05. (C) The numbers of MDSCs (Gr-1high granulocytic MDSCs and Gr-1intermediate MDSCs) in the spleen (left) and tumours (right) of JHOC-5-implanted nude mice was decreased by DHMEQ administration. Results were representative of six independent experiments. (D) Arginase activity of CD11b+ cells in tumours of JHOC-5-implanted nude mice was reduced by DHMEQ administration. Results were representative of four independent experiments. Error bars indicate s.d. *P<0.05. (E) T-cell stimulatory activity of mouse splenic CD11c+DCs in JHOC-5-implanted nude mice was restored by DHMEQ administration. T-cell stimulatory activity of splenic CD11c+DCs was measured by IFN-γ production of T cells obtained from BALB/c mice in the presence of an anti-CD3 antibody. Results were representative of six independent experiments. Error bars indicate s.d. *P<0.05. (F) Antitumour effects of transferred naive mouse T cells into JHOC-5-implanted nude mice was enhanced by DHMEQ administration. Tumour sizes of JHOC-5 in nude mice with T-cell transfer without DHMEQ administration (○-○) and T-cell transfer with DHMEQ administration (□-□) were measured. Control mice with DHMEQ administration (●-●) or without DHMEQ administration were also measured (▪-▪). DHMEQ treatment (i.p.) was started on day 13 and continued until day 31. CD90.2+ T cells were injected on day 23. Results were representative of four independent experiments. Error bars indicate s.d.. *P<0.05. The color reproduction of this figure is available on the British Journal of Medicine journal online
Taken together, this study demonstrates that constitutively activated NF-κB signalling in human EOC is involved in immunosuppression partly via high production of IL-6 and IL-8, leading to DC impairment and induction of immunosuppressive arginase-producing MDSCs, and that NF-κB inhibitors may be useful for reversal of immunosuppression and subsequent induction of antitumour T cells. Because NF-κB is also involved in other malignant features of EOC including cell proliferation, survival, chemotherapy resistance, and angiogenesis, NF-κB inhibition may be an attractive strategy for treatment of patients who have EOC with activated NF-κB.
Discussion
One of the major reasons for the relatively low response to current immunotherapies is thought to be immunosuppression in cancer patients, which is triggered by oncogene activation and dysregulated signalling in cancer cells (Yaguchi et al, 2011). However, the downstream mechanisms leading to the production and induction of immunosuppressive molecules and cells are not fully understood. In this study, we have shown that activated NF-κB signalling in human EOC cells causes immunosuppression partly through high production of IL-6 and IL-8. Interleukin -6 abundantly produced by human EOC cells in an NF-κB-dependent manner appears to impair DC production of cytokines such as IL-12, which is important for induction of antitumour T cells, as well as expansion of immunosuppressive arginase-producing monocyte–macrophage populations including MDSCs. Interleukin -8 is also abundantly produced by human EOC cells in an NF-κB-dependent manner, and it appears to induce immunosuppression possibly through promoting production of arginase that depletes arginine, an important amino acid for T-cell proliferation(Raber et al, 2012). Interleukin-6 and IL-8 also contribute to the accumulation of human Tregs through IL-8-dependent recruitment of Tregs that express CXCR1, which is induced by IL-6 (Eikawa et al, 2010). This mechanism may also be involved in the immunosuppression of EOC patients. The chemokine CCL2 is also produced in an NF-κB-dependent manner by some EOC cell lines including JHOC-5 that was used for the xenograft mouse model in this study (data not shown). Because CCL2 is the major chemokine for the recruitment of MDSCs to tumours (Ben-Baruch, 2012; Viola et al, 2012), and human CCL2 acts on murine cells, CCL2 may also be involved in the increased accumulation of MDSCs in the spleen and tumours, and their decrease by DHMEQ administration in our mouse model.
Hallmarks of cancer including immunosuppression have been proposed previously (Hanahan and Weinberg, 2011). Nuclear factor-κB is a transcription factor constitutively activated in various cancers, and it is involved in the various hallmarks of cancer (Karin and Greten, 2005; Karin, 2006; He and Karin, 2010; Surh et al, 2010; Rushworth et al, 2012). Nuclear factor-κB is associated with the upregulation of cell proliferation-related molecules such as cyclin D and c-myc, cell survival-related molecules such as BCL-2 and XIAP, proangiogenic factors such as IL-8 and VEGF, drug resistance-related molecules such as Nrf2, and inflammatory cytokines such as IL-6 and TNF-α(Karin, 2006). High levels of IL-6 and IL-8 in serum and ascites of EOC patients and high NK-κB expression are associated with poor clinical outcomes (Kassim et al, 2004; Annunziata et al, 2010; Coward et al, 2011). In this study, we have clarified the roles of NF-κB in the immunosuppressive phenotypes of EOC. Therefore, NF-κB inhibition may be an attractive strategy for cancer treatment through simultaneous inhibition of multiple hallmarks of EOC.
DHMEQ is a specific NF-κB inhibitor that inhibits NF-κB signalling by interfering with NF-κB nuclear localisation and DNA binding by covalently binding to cysteine element of p65 and other Rel homology proteins (Ariga et al, 2002; Yamamoto et al, 2008). DHEMQ has been previously reported to induce apoptosis, cell cycle arrest, and proinflammatory cytokine reduction in cancer cell lines including EOC (Starenki et al, 2004; Matsumoto et al, 2005; Miyanishi et al, 2010). As NF-κB is essential for both innate and adaptive immunity, NK-κB inhibitors may cause adverse effects including inhibition of antitumour T-cell induction (Siebenlist et al, 2005). However, administration of appropriate doses of NFκB inhibitors appears to have antitumour effects without affecting induction of antitumour T cells as shown in this study.
Recently, immunological conditions before cancer treatment, particularly infiltration of memory CD8+ T cells into tumours, were reported to be associated with a better prognosis of patients with various cancers including EOC (Hamanishi et al, 2011; Nielsen et al, 2012), and are also associated with better responses of melanoma to immunotherapy and colon cancer to chemotherapy (Halama et al, 2011; Gajewski et al, 2013). Mechanisms for varied CD8+ T-cell infiltration into tumours among patients have not been revealed. The NF-κB-dependent immunosuppression shown in this study may be one of the mechanisms for differential T-cell infiltration into tumours. Further study to examine the correlation between NF-κB activation, IL-6/IL-8 production, and tumour infiltration of CD8+ T cells is intriguing and needed.
In this study, histology of three ovarian cell lines that produce relatively high IL-6 and IL-8 levels via NF-κB activation is a clear-cell type. Clear-cell ovarian cancer represents 20% of Japanese patients and <10% of Caucasian patients, and it is known to be refractory to platinum-based chemotherapy (Sugiyama et al, 2000; Anglesio et al, 2011). Clear-cell ovarian cancer shows different gene signatures from those of other types of EOCs (Anglesio et al, 2011). Nuclear factor-κB-dependent immunosuppression may be more relevant to patients with clear-cell ovarian cancer. However, an increase of plasma IL-6 in patients with other types of EOCs suggests the general importance of this mechanism in EOC patients.
In summary, we have shown that constitutively active NF-κB in human EOC cells is the major mechanism for immunosuppression partly through IL-6-dependent impairment of DCs and generation and recruitment of immunosuppressive MDSCs in tumours, as well as an IL-8-related increase of immunosuppressive arginase. An appropriate dose of an NF-κB inhibitor may be useful for reversal of immunosuppressive conditions in EOC, which may increase responses to various cancer therapies including immunotherapy and chemotherapy. Because NF-κB is involved in the various malignant features of EOC, including cell proliferation, survival, chemotherapy resistance, and angiogenesis, NF-κB inhibition in combination with various cancer therapies may be an attractive strategy for EOC treatment.
Change history
10 June 2014
This paper was modified 12 months after initial publication to switch to Creative Commons licence terms, as noted at publication
References
Anglesio MS, George J, Kulbe H, Friedlander M, Rischin D, Lemech C, Power J, Coward J, Cowin PA, House CM, Chakravarty P, Gorringe KL, Campbell IG, Okamoto A, Birrer MJ, Huntsman DG, de Fazio A, Kalloger SE, Balkwill F, Gilks CB, Bowtell DD (2011) IL6-STAT3-HIF signaling and therapeutic response to the angiogenesis inhibitor sunitinib in ovarian clear cell cancer. Clin Cancer Res 17 (8): 2538–2548.
Annunziata CM, Stavnes HT, Kleinberg L, Berner A, Hernandez LF, Birrer MJ, Steinberg SM, Davidson B, Kohn EC (2010) Nuclear factor kappaB transcription factors are coexpressed and convey a poor outcome in ovarian cancer. Cancer 116 (13): 3276–3284.
Ariga A, Namekawa J, Matsumoto N, Inoue J, Umezawa K (2002) Inhibition of tumor necrosis factor-alpha-induced nuclear translocation and activation of NF-kappa B by dehydroxymethylepoxyquinomicin. J Biol Chem 277 (27): 24625–24630.
Baud V, Karin M (2009) Is NF-kappaB a good target for cancer therapy? Hopes and pitfalls. Nat Rev Drug Discov 8 (1): 33–40.
Ben-Baruch A (2012) The tumor-promoting flow of cells into, within and out of the tumor site: regulation by the inflammatory axis of TNFalpha and chemokines. Cancer Microenviron 5 (2): 151–164.
Coward J, Kulbe H, Chakravarty P, Leader DA, Vassileva V, Leinster DA, Thompson R, Schioppa T, Nemeth JA, Vermeulin J, Singh N, Avril NE, Cummings J, Rexhepaj E, Jirstrom K, Gallagher WM, Brennan DJ, McNeish IA, Balkwill FR (2011) Interleukin-6 as a therapeutic target in human ovarian cancer. Clin Cancer Res 17 (18): 6083–6096.
Cubillos-Ruiz JR, Rutkowski M, Conejo-Garcia JR (2010) Blocking ovarian cancer progression by targeting tumor microenvironmental leukocytes. Cell Cycle 9 (2): 260–268.
Eikawa S, Ohue Y, Kitaoka K, Aji T, Uenaka A, Oka M, Nakayama E (2010) Enrichment of Foxp3+ CD4 regulatory T cells in migrated T cells to IL-6- and IL-8-expressing tumors through predominant induction of CXCR1 by IL-6. J Immunol 185 (11): 6734–6740.
Fridman WH, Galon J, Pages F, Tartour E, Sautes-Fridman C, Kroemer G (2011) Prognostic and predictive impact of intra- and peritumoral immune infiltrates. Cancer Res 71 (17): 5601–5605.
Gajewski TF, Woo SR, Zha Y, Spaapen R, Zheng Y, Corrales L, Spranger S (2013) Cancer immunotherapy strategies based on overcoming barriers within the tumor microenvironment. Curr Opin Immunol 25 (2): 268–276.
Goto Y, Ferrone S, Arigami T, Kitago M, Tanemura A, Sunami E, Nguyen SL, Turner RR, Morton DL, Hoon DS (2008) Human high molecular weight-melanoma-associated antigen: utility for detection of metastatic melanoma in sentinel lymph nodes. Clin Cancer Res 14 (11): 3401–3407.
Greenlee RT, Hill-Harmon MB, Murray T, Thun M (2001) Cancer statistics, 2001. CA Cancer J Clin 51 (1): 15–36.
Grivennikov SI, Karin M (2010) Dangerous liaisons: STAT3 and NF-kappaB collaboration and crosstalk in cancer. Cytokine Growth Factor Rev 21 (1): 11–19.
Halama N, Michel S, Kloor M, Zoernig I, Benner A, Spille A, Pommerencke T, von Knebel DM, Folprecht G, Luber B, Feyen N, Martens UM, Beckhove P, Gnjatic S, Schirmacher P, Herpel E, Weitz J, Grabe N, Jaeger D (2011) Localization and density of immune cells in the invasive margin of human colorectal cancer liver metastases are prognostic for response to chemotherapy. Cancer Res 71 (17): 5670–5677.
Hamanishi J, Mandai M, Abiko K, Matsumura N, Baba T, Yoshioka Y, Kosaka K, Konishi I (2011) The comprehensive assessment of local immune status of ovarian cancer by the clustering of multiple immune factors. Clin Immunol 141 (3): 338–347.
Hanahan D, Weinberg RA (2011) Hallmarks of cancer: the next generation. Cell 144 (5): 646–674.
He G, Karin M (2010) NF-kappaB and STAT3 – key players in liver inflammation and cancer. Cell Res 21 (1): 159–168.
Hwang WT, Adams SF, Tahirovic E, Hagemann IS, Coukos G (2012) Prognostic significance of tumor-infiltrating T cells in ovarian cancer: a meta-analysis. Gynecol Oncol 124 (2): 192–198.
Ivarsson K, Ekerydh A, Fyhr IM, Janson PO, Brannstrom M (2000) Upregulation of interleukin-8 and polarized epithelial expression of interleukin-8 receptor A in ovarian carcinomas. Acta Obstet Gynecol Scand 79 (9): 777–784.
Iwata-Kajihara T, Sumimoto H, Kawamura N, Ueda R, Takahashi T, Mizuguchi H, Miyagishi M, Takeda K, Kawakami Y (2011) Enhanced cancer immunotherapy using STAT3-depleted dendritic cells with high Th1-inducing ability and resistance to cancer cell-derived inhibitory factors. J Immunol 187 (1): 27–36.
Karin M (2006) Nuclear factor-kappaB in cancer development and progression. Nature 441 (7092): 431–436.
Karin M, Greten FR (2005) NF-kappaB: linking inflammation and immunity to cancer development and progression. Nat Rev Immunol 5 (10): 749–759.
Kassim SK, El-Salahy EM, Fayed ST, Helal SA, Helal T, Azzam Eel D, Khalifa A (2004) Vascular endothelial growth factor and interleukin-8 are associated with poor prognosis in epithelial ovarian cancer patients. Clin Biochem 37 (5): 363–369.
Kawakami Y, Fujita T, Matsuzaki Y, Sakurai T, Tsukamoto M, Toda M, Sumimoto H (2004) Identification of human tumor antigens and its implications for diagnosis and treatment of cancer. Cancer Sci 95 (10): 784–791.
Leffers N, Lambeck AJ, Gooden MJ, Hoogeboom BN, Wolf R, Hamming IE, Hepkema BG, Willemse PH, Molmans BH, Hollema H, Drijfhout JW, Sluiter WJ, Valentijn AR, Fathers LM, Oostendorp J, van der Zee AG, Melief CJ, van der Burg SH, Daemen T, Nijman HW (2009) Immunization with a P53 synthetic long peptide vaccine induces P53-specific immune responses in ovarian cancer patients, a phase II trial. Int J Cancer 125 (9): 2104–2113.
Matsumoto G, Namekawa J, Muta M, Nakamura T, Bando H, Tohyama K, Toi M, Umezawa K (2005) Targeting of nuclear factor kappaB pathways by dehydroxymethylepoxyquinomicin, a novel inhibitor of breast carcinomas: antitumor and antiangiogenic potential in vivo. Clin Cancer Res 11 (3): 1287–1293.
Miyanishi N, Suzuki Y, Simizu S, Kuwabara Y, Banno K, Umezawa K (2010) Involvement of autocrine CXCL12/CXCR4 system in the regulation of ovarian carcinoma cell invasion. Biochem Biophys Res Commun 403 (1): 154–159.
Nielsen JS, Sahota RA, Milne K, Kost SE, Nesslinger NJ, Watson PH, Nelson BH (2012) CD20+ tumor-infiltrating lymphocytes have an atypical CD27− memory phenotype and together with CD8+ T cells promote favorable prognosis in ovarian cancer. Clin Cancer Res 18 (12): 3281–3292.
Nilsson MB, Langley RR, Fidler IJ (2005) Interleukin-6, secreted by human ovarian carcinoma cells, is a potent proangiogenic cytokine. Cancer Res 65 (23): 10794–10800.
Raber P, Ochoa AC, Rodriguez PC (2012) Metabolism of L-arginine by myeloid-derived suppressor cells in cancer: mechanisms of T cell suppression and therapeutic perspectives. Immunol Invest 41 (6-7): 614–634.
Rotondo R, Barisione G, Mastracci L, Grossi F, Orengo AM, Costa R, Truini M, Fabbi M, Ferrini S, Barbieri O (2009) IL-8 induces exocytosis of arginase 1 by neutrophil polymorphonuclears in nonsmall cell lung cancer. Int J Cancer 125 (4): 887–893.
Rushworth SA, Zaitseva L, Murray MY, Shah NM, Bowles KM, MacEwan DJ (2012) The high Nrf2 expression in human acute myeloid leukemia is driven by NF-kappaB and underlies its chemo-resistance. Blood 120 (26): 5188–5198.
Siebenlist U, Brown K, Claudio E (2005) Control of lymphocyte development by nuclear factor-kappaB. Nat Rev Immunol 5 (6): 435–445.
Starenki DV, Namba H, Saenko VA, Ohtsuru A, Maeda S, Umezawa K, Yamashita S (2004) Induction of thyroid cancer cell apoptosis by a novel nuclear factor kappaB inhibitor, dehydroxymethylepoxyquinomicin. Clin Cancer Res 10 (20): 6821–6829.
Sugiyama T, Kamura T, Kigawa J, Terakawa N, Kikuchi Y, Kita T, Suzuki M, Sato I, Taguchi K (2000) Clinical characteristics of clear cell carcinoma of the ovary: a distinct histologic type with poor prognosis and resistance to platinum-based chemotherapy. Cancer 88 (11): 2584–2589.
Sumimoto H, Imabayashi F, Iwata T, Kawakami Y (2006) The BRAF-MAPK signaling pathway is essential for cancer-immune evasion in human melanoma cells. J Exp Med 203 (7): 1651–1656.
Surh YJ, Bode AM, Dong Z (2010) Breaking the NF-kappaB and STAT3 alliance inhibits inflammation and pancreatic tumorigenesis. Cancer Prev Res (Phila) 3 (11): 1379–1381.
van Dam M, Mullberg J, Schooltink H, Stoyan T, Brakenhoff JP, Graeve L, Heinrich PC, Rose-John S (1993) Structure-function analysis of interleukin-6 utilizing human/murine chimeric molecules. Involvement of two separate domains in receptor binding. J Biol Chem 268 (20): 15285–15290.
Viola A, Sarukhan A, Bronte V, Molon B (2012) The pros and cons of chemokines in tumor immunology. Trends Immunol 33 (10): 496–504.
Yaguchi T, Goto Y, Kido K, Mochimaru H, Sakurai T, Tsukamoto N, Kudo-Saito C, Fujita T, Sumimoto H, Kawakami Y (2012) Immune suppression and resistance mediated by constitutive activation of Wnt/beta-catenin signaling in human melanoma cells. J Immunol 189 (5): 2110–2117.
Yaguchi T, Sumimoto H, Kudo-Saito C, Tsukamoto N, Ueda R, Iwata-Kajihara T, Nishio H, Kawamura N, Kawakami Y (2011) The mechanisms of cancer immunoescape and development of overcoming strategies. Int J Hematol 93 (3): 294–300.
Yamamoto M, Horie R, Takeiri M, Kozawa I, Umezawa K (2008) Inactivation of NF-kappaB components by covalent binding of (−)-dehydroxymethylepoxyquinomicin to specific cysteine residues. J Med Chem 51 (18): 5780–5788.
Acknowledgements
We thank Kenji Morii for in vivo experiments and flow cytometric analyses. We also thank Misako Horikawa and Ryoko Suzuki for preparation of the manuscript. This work was supported by grants-in-aid for scientific research and a research program of the Project for Development of Innovative Research on Cancer Therapeutics (P-Direct) from the Ministry of Education, Culture, Sports, Science and Technology of Japan (90445239, 23240128, and 21591445), and a Keio University grant-in-aid for encouragement of young medical scientists.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
These authors declare no conflict of interest.
Additional information
This work is published under the standard license to publish agreement. After 12 months the work will become freely available and the license terms will switch to a Creative Commons Attribution-NonCommercial-Share Alike 3.0 Unported License.
Rights and permissions
From twelve months after its original publication, this work is licensed under the Creative Commons Attribution-NonCommercial-Share Alike 3.0 Unported License. To view a copy of this license, visit http://creativecommons.org/licenses/by-nc-sa/3.0/
About this article
Cite this article
Nishio, H., Yaguchi, T., Sugiyama, J. et al. Immunosuppression through constitutively activated NF-κB signalling in human ovarian cancer and its reversal by an NF-κB inhibitor. Br J Cancer 110, 2965–2974 (2014). https://doi.org/10.1038/bjc.2014.251
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/bjc.2014.251
Keywords
This article is cited by
-
Tumor PKCδ instigates immune exclusion in EGFR-mutated non–small cell lung cancer
BMC Medicine (2022)
-
Gene polymorphisms of interleukin 10 (− 819 C/T and − 1082 G/A) in women with ovarian cancer
Beni-Suef University Journal of Basic and Applied Sciences (2022)
-
Tumor-immune profiling of CT-26 and Colon 26 syngeneic mouse models reveals mechanism of anti-PD-1 response
BMC Cancer (2021)
-
Hypoxia and the phenomenon of immune exclusion
Journal of Translational Medicine (2021)
-
NF-кB inhibition by DHMEQ: in vitro antiproliferative effects on pilocytic astrocytoma and concise review of the current literature
Child's Nervous System (2020)