Abstract
Background:
Radiotherapy can be an effective treatment for prostate cancer, but radiorecurrent tumours do develop. Considering prostate cancer heterogeneity, we hypothesised that primitive stem-like cells may constitute the radiation-resistant fraction.
Methods:
Primary cultures were derived from patients undergoing resection for prostate cancer or benign prostatic hyperplasia. After short-term culture, three populations of cells were sorted, reflecting the prostate epithelial hierarchy, namely stem-like cells (SCs, α2β1integrinhi/CD133+), transit-amplifying (TA, α2β1integrinhi/CD133−) and committed basal (CB, α2β1integrinlo) cells. Radiosensitivity was measured by colony-forming efficiency (CFE) and DNA damage by comet assay and DNA damage foci quantification. Immunofluorescence and flow cytometry were used to measure heterochromatin. The HDAC (histone deacetylase) inhibitor Trichostatin A was used as a radiosensitiser.
Results:
Stem-like cells had increased CFE post irradiation compared with the more differentiated cells (TA and CB). The SC population sustained fewer lethal double-strand breaks than either TA or CB cells, which correlated with SCs being less proliferative and having increased levels of heterochromatin. Finally, treatment with an HDAC inhibitor sensitised the SCs to radiation.
Interpretation:
Prostate SCs are more radioresistant than more differentiated cell populations. We suggest that the primitive cells survive radiation therapy and that pre-treatment with HDAC inhibitors may sensitise this resistant fraction.
Similar content being viewed by others
Main
Precision radiotherapy (external beam or brachytherapy) is an important treatment for localised prostate cancer. However, despite improvements in targeting and dose, one-third of patients still fail because of local or systemic resistance (Brawer, 2002; Catton et al, 2003; Ishkanian et al, 2010). Metastases following radiotherapy are a significant clinical problem that requires an improved understanding of the biology of treatment-resistant phenotypes (Zafarana and Bristow, 2010; Jones, 2011). The use of in vitro cell line models of prostate cancer has demonstrated that clones of radioresistant cells emerge post irradiation (Bromfield et al, 2003; van Oorschot et al, 2013). There have also been radiation response studies using normal prostate tissue and primary cells from normal biopsies (Kiviharju-af Hallstrom et al, 2007; Jaamaa et al, 2010; Zhang et al, 2011). However, none of these studies addressed the phenotype of the resistant clones. We, and others, have shown that a cellular hierarchy exists in several cancer types and in both prostate cancer epithelium and normal prostate epithelium (Collins et al, 2001; Hudson et al, 2001; Miller et al, 2005; Visvader and Lindeman, 2008; Maitland et al, 2010; Clevers, 2011). These studies demonstrated that the more stem-like cells (SCs), at the beginning of the hierarchy, have more clonogenic and tumourigenic potential than the more differentiated cells. Moreover, in glioblastoma, it was demonstrated that the primitive cells were more resistant to radiotherapy than the majority of cells within the tumour (Bao et al, 2006). This finding has been backed up by other studies suggesting that the SCs may be directly responsible for tumour recurrence (Chiou et al, 2008; Diehn et al, 2009b; Conley et al, 2012; Chen et al, 2013). In light of these findings, we hypothesised that the SCs in prostate cancer would be more resistant to irradiation than the more differentiated populations. Using the same markers we had previously used to isolate the normal and malignant prostate hierarchy (Collins et al, 2001; Richardson et al, 2004; Collins et al, 2005), we show here that the most undifferentiated cells in both benign and malignant primary cultures are more resistant to irradiation. This resistance is conferred by heterochromatin, which protects the cells from the DNA-damaging effects of radiation.
Materials and methods
Tissue collection, isolation and culture of tumour cells
Human prostate tissue was obtained with patient’s consent and full ethical approval from patients undergoing radical prostatectomy and channel transurethral resection (TURP) for prostate cancer and from patients undergoing transurethral resection for benign prostatic hyperplasia (BPH) (Table 1). Grade and stage of tumour were confirmed by histologic examination of representative fragments by a uropathologist. Epithelial cultures were prepared and characterised as described previously (Collins et al, 2001). Cell cultures were maintained in stem cell media (SCM) consisting of keratinocyte growth medium supplemented with EGF, bovine pituitary extract (Life Technologies Ltd, Paisley, UK), 2 ng ml−1 stem cell factor (SCF) (First Link UK Ltd, Wolverhampton, UK), 100 ng ml−1 cholera toxin (Sigma-Aldrich Company Ltd, Gillingham, UK) and 1 ng ml−1 granulocyte macrophage colony-stimulating factor (GM-CSF) (First Link UK Ltd). Cells were cultured in the presence of irradiated (60 Gy) STO (mouse embryonic fibroblast) cells. After expansion, CD133+/α2β1integrinhi (stem-like (SC)), CD133−/α2β1integrinhi (transit-amplifying (TA)) and α2β1integrinlo (committed basal (CB)) cells were isolated by magnetic-activated cell sorting (MACS; Miltenyi Biotec, Surrey, UK) as described previously (Richardson et al, 2004; Collins et al, 2005). SC cells are the most primitive cells, with TA cells being a progenitor population and CB cells being further along the differentiation hierarchy.
Irradiation of cells
To irradiate cells, an RS2000 X-Ray Biological Irradiator was used that contains a Comet MXR-165 X-Ray Source (Rad-Source Technologies Inc., Suwanee, GA, USA). A dose of 2 or 10 Gy was administered with a dose rate of 0.02 or 0.08 Gy s−1. To determine colony-forming ability post irradiation, primary cultures were irradiated as a whole population and subsequently sorted. To assay DNA damage, in response to radiation, primary cells were sorted into their respective populations before irradiation because of the rapid nature of DNA damage formation.
Clonogenic recovery
Primary prostate cultures were irradiated (2 Gy) and immediately sorted into subpopulations (SC, TA and CB), counted and plated on to 35-mm collagen-coated plates (BD Biocoat, BD Biosciences, Oxford, UK) at a density of 100 cells per well in the presence of irradiated STO feeder cells. For treatment with HDAC inhibitor, cells were treated with 0.6 μ M of Trichostatin A (TSA; Sigma-Aldrich Company Ltd, T1952) for 1 h and 30 min and then irradiated (2 Gy) and treated as above. Colonies were subsequently scored if they contained >32 cells (at least 5 population doublings, which are considered as self-sustaining colonies with proliferation potential (Puck and Marcus, 1956; Francipane et al, 2008), usually ∼14 days after treatment. Colonies were visualised by staining with 1% crystal violet/10% ethanol/PBS.
Alkaline and neutral comet assays
Comet assays were modified from Sturmey et al (2009). Primary prostate epithelial cells were separated into SC, TA and CB cells, resuspended in 25 μl PBS and irradiated. At 30 min post irradiation, 225 μl of low-melting-point (LMP) agarose was added to the cells, mixed and pipetted onto an agarose-coated slide (1% agarose in PBS). A clean coverslip was placed on top and slides placed at 4 °C for 15 min. Once set, coverslips were removed and slides placed in lysis buffer (2.5 M NaCl, 1 mM EDTA, 10 mM Tris, 10% DMSO, 1% Triton X-100, pH 10) overnight at 4 °C. For the alkaline comet assays, slides were incubated in alkaline solution (0.3 M NaOH, 1 mM EDTA, pH 13) for 40 min at 4 °C, and then electrophoresed at 23 V, 300 mA in the same alkaline solution (for 40 min on ice). Subsequently, they were incubated for 2 × 10 min in neutralising buffer (0.4 M Tris, pH 7.5). For the neutral comet assays, slides were incubated in TBE electrophoresis buffer at 4 °C for 40 min and electrophoresed at 25 V for 20 min. For both assays SYBRgold was applied (1 : 10 000 in TE buffer, 10 mM Tris-Cl, pH 7.5, 1 mM EDTA) to stain the DNA. Comets were measured using CometScore freeware (TriTek Corp., Sumerduck, VA, USA) following image capture using a Nikon Eclipse TE300 fluorescent microscope (Nikon, Surrey, UK) with a × 10 lens.
Immunofluorescence
Immunocytochemistry was conducted on sorted α2β1integrinhi/CD133+ (SC), α2β1integrinhi/CD133− (TA) and α2β1integrinlo (CB) primary cells. The cell isolates were allowed to adhere for 2 h onto collagen-coated slides, and in some experiments were treated with 0.6 μ M of TSA (Sigma-Aldrich Company Ltd T1952) for 1 h and 30 min and irradiated (2 Gy) before fixing in 2% paraformaldehyde/PBS/0.2% Triton X-100, pH 8.2 (20 min), then permeabilised with 0.5% NP40/PBS (20 min). Cells were then blocked (2% BSA/1% normal goat serum/PBS) and incubated in primary antibody in 3% BSA/PBS at 4 °C overnight followed by washes in 0.5% BSA/0.175% Tween-20/PBS. Secondary antibody was added for 45 min in 3% BSA/PBS followed by washes. Slides were mounted with Vectashield with DAPI (Vector Laboratories, Peterborough, UK). Primary antibodies used were as follows: anti-phospho-Histone H2A.X (Ser139), clone JBW301 (Millipore, Watford, UK); 53BP1 (Alexis Biochemicals, Exeter, UK, ALK-210-419 or Abcam, Cambridge, UK, ab36823); phospho-Chk2 (Thr68; Cell Signaling Technology, Hitchin, UK, 2661); phospho-(Ser/Thr) ATM/ATR substrate antibody (Cell Signaling Technology 2851); H3K9me3 (histone H3(trimethylated at lysine 9); Diagenode, Denville, NJ, USA, pAb-056-050); Ki67 (Abcam ab15580); H3K27me3 (histone H3(trimethylated at lysine 27); Millipore 17-622). Secondary antibodies were goat anti-mouse AlexaFluor-488 (Life Technologies Ltd A11029) and goat anti-rabbit AlexaFluor-568 (Life Technologies Ltd A11036).
Confocal images were acquired on Zeiss LSM 510 and Zeiss LSM Meta Laser confocal microscopes (Zeiss, Cambridge, UK). Colocalisation analysis, Pearson’s correlation, line scan analysis and fluorescence intensity measurements were carried out using Volocity software (Improvision, Perkin Elmer, Waltham, MA, USA). For foci counting, images were captured using a Nikon Eclipse TE300 fluorescent microscope (Nikon, Surrey, UK) with a × 63 oil immersion lens and foci were counted using the multi-point tool in ImageJ software (Town of Mount Royal, QC, Canada).
Flow cytometry
Primary cultures were trypsinised, resuspended in MACs buffer and incubated with antibodies to the α2 subunit of integrin α2β1 (CD49b-RPE, MCA743PET, AbD Serotec, Kidlington, UK) and CD133/2 (293C)-APC (130-090-854, Miltenyi Biotec) for 10 min at 4 °C.
For the detection of heterochromatin, the cells were then permeabilised in MACs buffer with 0.5% W/V saponin and 20% normal goat serum (NGS) and then incubated with the H3K9me3 antibody (Diagenode) or H3K27me3 antibody (Millipore 17-622) in MACs buffer with 20% NGS. Cells were then washed and incubated with goat anti-rabbit AlexaFluor-488 secondary antibody (Life Technologies Ltd) in MACs buffer with 20% NGS. Finally, cells were analysed on a CyAn-ADP flow cytometer (Beckman Coulter, High Wycombe, UK) and data processed using Summit v4.3 software (Beckman Coulter).
Statistical analysis
Median values of each analysis were calculated. Significance was assessed using the Wilcoxon rank-sum test or t-test for smaller sample numbers where stated (GraphPad Prism, La Jolla, CA, USA). The P-values indicating statistical significance are displayed.
Results
SCs are more radioresistant than progenitor cells
To establish whether prostate SCs are more resistant to irradiation than progenitors, we determined the potential of each population to initiate colonies (at clonal density) following irradiation. Our rationale for using 2 Gy was to mimic the clinical daily dose of 2 Gy that has been routinely administered to patients (Bromfield et al, 2003). Primary cells, derived from patients with BPH, and prostate cancer, including those who had undergone androgen-ablation therapy, were irradiated, sorted into SCs and progenitors (TA and CB) and plated to determine colony-forming efficiency (CFE) that is represented as surviving fraction (SF) after 2 Gy (SF2Gy; Figure 1A and B). The highest SF2Gy (post irradiation) was observed in the SCs, independent of disease status (Figure 1A and B). To investigate the consequences of irradiation on each cell type, DNA damage was measured following radiation in each population (Figure 1C and D). To do this we used comet assays to measure DNA damage directly, following radiation doses of 2 and 10 Gy. Alkaline comet assays were used to measure single-strand breaks (SSBs), double-strand breaks (DSBs), alkali labile sites, DNA crosslinks and incomplete excision repair (Singh et al, 1988; Tice et al, 2000; Nandhakumar et al, 2011; Swain and Subba Rao, 2011). We observed comparable damage in each population, with a clear dose-dependent increase (up to 10 Gy; Figure 1C). In contrast, using the neutral comet assay, we observed that the SCs incurred significantly less damage than either the TA or CB populations (Figure 1D). Moreover, there was no significant difference in DNA damage with increasing dose. The neutral comet assay has a bias for measuring lethal DSBs (Ostling and Johanson, 1984; Singh et al, 1988; Lemay and Wood, 1999; Wojewodzka et al, 2002; Van Kooij et al, 2004; Swain and Subba Rao, 2011). This suggests that the SCs are protected from this specific type of damage compared with the progenitor (TA) and more differentiated (CB) cells. As observed with the colony-forming assay, this effect on DNA damage was independent of disease status.
Stem-like cells (SCs) from benign and cancer cultures are less radiosensitive and have a differential DNA damage response compared to progenitor TA cells and more differentiated CB cells. (A and B) Benign and malignant primary prostate epithelial cultures were treated with 2 Gy radiation and cell populations sorted and plated for clonogenic assays. Surviving fraction following 2 Gy (SF2Gy) was calculated and plotted for each cell subpopulation. Each symbol represents a different patient sample (red symbols indicate prostate cancer and blue symbols indicate BPH) and the black bar represents the median. (C and D) Benign and malignant primary prostate epithelial cultures were sorted into cell subpopulations and treated with 2 Gy radiation, and then processed in alkaline (C) and neutral (D) comet assays. Each symbol represents a different patient sample (red symbols indicate prostate cancer and blue symbols indicate BPH) and the black bar represents the median. Statistical significance values were measured using the Wilcoxon rank-sum test (*P<0.05, **P<0.01, ***P<0.001).
SCs sustain less DSBs than progenitors
To confirm this finding, we investigated the DSB DNA damage response further. Primary cells were sorted, irradiated and fixed at 30 min post irradiation. Cells were then stained for γH2AX and 53BP1 DNA damage nuclear foci, indicative of DSBs (Paull et al, 2000; Belyaev, 2010; Mah et al, 2010) (Figure 2A). Approximately 90% of TA and CB cell nuclei showed evidence of DSBs, whereas significantly fewer (30–50%) SCs sustained DSBs (Figure 2B–E). These results are in agreement with our findings using the neutral comet assay, showing evidence of DSBs in the majority of TA and CB cells, but only in a minority of SCs.
Fewer SCs from benign and malignant primary epithelial cultures contain DNA damage foci relative to TA and CB cells post irradiation. (A) Cells from benign and malignant primary prostate epithelial cultures were sorted then fixed and stained for γH2AX and 53BP1 at 30 min post irradiation. Representative images are shown of nuclei showing (i) negative (ii) and positive staining for DNA damage foci (γH2AX (green), 53BP1 (red) and DAPI nuclear staining (blue)). Image squares containing a single nucleus measured 27.35 μm by 27.35 μm. (B–E) Cell nuclei were scored for foci and ∼100 nuclei per sample were counted. The graphs indicate the percentage of cell nuclei containing foci. Each symbol represents a different patient sample (red symbols indicate prostate cancer and blue symbols indicate BPH). Boxplots show minimum, 25%, median, 75% and maximum. Statistical significance values were measured using the Wilcoxon rank-sum test (**P<0.01, ***P<0.001).
We also investigated the downstream events following induction of DNA damage by staining the cell populations for members of the ATM-Chk2 DSB DNA damage pathway (Figure 3). Again, we observed that the percentage of SCs containing ATM/ATR phosphorylated substrates and phospho-Chk2Thr68 was significantly less than either of the progenitor populations, again reinforcing our findings that SCs sustain less DSBs.
Fewer prostate SCs from benign and malignant primary epithelial cultures have an active ATM/Chk2 DNA damage response post irradiation. Nuclear DNA damage foci were scored as in Figure 2, after staining with ATM/ATR substrate antibody (A) and pChk2Th68 antibody (B). Percentage of cell nuclei that contain foci is represented. Each symbol represents a different patient sample (red symbols indicate prostate cancer and blue symbols indicate BPH). Representative images of nuclei showing co-staining of γH2AX antibody (green), (Ai) ATM/ATR substrate antibody or (Bi) pChk2Th68 antibodies (red) and DAPI nuclear stain (blue) are shown. Boxplots show minimum, 25%, median, 75% and maximum. Statistical significance values were measured using the Wilcoxon rank-sum test (*P<0.05, **P<0.01).
Although the majority of SCs appear to sustain no damage, we wanted to know if the minority subpopulation that did sustain damage could undertake DNA repair. To do this, the number of foci per cell nucleus was quantified. It was clear that in all cell types (SC, TA, CB), and in all patients, DNA repair was taking place, as evidenced by a significant reduction in the number of foci per cell nucleus at 24 h compared with 30 min (Figure 4).
All cell types are equally capable of undergoing DNA repair post irradiation. Number of foci per cell nucleus were counted at 30 min and 24 h post irradiation in SCs (A), TA (B) and CB (C) cells. Each symbol represents a single cell (red symbols indicate prostate cancer and blue symbols indicate BPH). Boxplots show minimum, 25%, median, 75% and maximum. Statistical significance values were measured using the Wilcoxon rank-sum test (*P<0.05, **P<0.01, ***P<0.001).
SCs are less proliferative and have increased heterochromatin
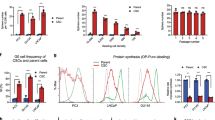
As SCs appeared to sustain less DNA damage following irradiation, we hypothesised that they may have an inherent protection mechanism. We had previously demonstrated that the SCs are less proliferative (Lang et al, 2010), and hence we quantified the number of cells expressing the proliferation marker Ki67 (Figure 5A). Primary cells from six patients were sorted as previously described and stained with an antibody against Ki67. We found that the percentage of SCs expressing Ki67 was significantly less than either the TA or CB cells, suggesting that the progenitor (TA) and more differentiated (CB) cells are more proliferative than the SCs (Figure 5A).
Stem-like cells (SCs) from benign and malignant primary epithelial cultures are less proliferative and have more heterochromatin than more differentiated TA and CB cells. (A) Cells were stained for Ki67 and scored for positive staining and presented as a percentage of the total cell number. Each symbol represents a different patient sample (red symbols indicate prostate cancer and blue symbols indicate BPH). Boxplots show minimum, 25%, median, 75% and maximum. (B) Staining for H3K9me3 (heterochromatin). (C) Cells were analysed for amount of heterochromatin using intensity of immunofluorescence staining (analysis using Volocity software) (i) H3K9me3 (ii) H3K27me3. (D) Cells were analysed for heterochromatin content using flow cytometry analysis (i) H3K9me3 (ii) H3K27me3. Each symbol represents a different patient sample (red symbols indicate prostate cancer and blue symbols indicate BPH) and the black bar represents the mean of the total fluorescence of each cell population divided by the median of the CB value. (E) Co-staining of γH2AX and H3K9me3 (heterochromatin). (i) The γH2AX-positive SC, TA and CB cells were analysed for colocalisation with heterochromatin (analysis using Volocity software). (ii) Representative images of SCs negative for γH2AX nuclear foci. Statistical significance values were measured using the Wilcoxon rank-sum test (*P<0.05, **P<0.01).
One other mechanism by which a cell could sustain less damage is by packing more DNA into heterochromatin. Storch et al (2010) found that growing cells in a 3D formation led to increased chromatin condensation, which subsequently resulted in radioresistance. Furthermore, when measuring the number of DSBs in euchromatin vs heterochromatin in monolayer cells, the authors found a ratio of 2 : 1, that is, fewer breaks in heterochromatin. When we examined heterochromatin marks (H3K27me3 and H3K9me3) in each cell population, we observed that a proportion of SCs appeared to have increased heterochromatin content compared with the other cell types (TA and CB) (Figure 5B). We quantified heterochromatin by measuring the fluorescence intensity of sorted cells (Figure 5C) as well as flow cytometry where cells were co-stained with CD49b (α2β1integrin) and CD133 to distinguish the three populations (Figure 5D). This showed that SCs had significantly increased heterochromatin compared with the progenitor (TA) and more differentiated (CB ) cells.
To confirm that heterochromatin conferred a protective effect to the cells, we carried out dual staining of DNA damage foci and heterochromatin that showed preferential formation of foci located almost exclusively at nuclear sites devoid of heterochromatin staining (Figure 5Ei). In addition, several SCs were observed to have high levels of heterochromatin throughout the nucleus that corresponded with an absence of foci (Figure 5Eii).
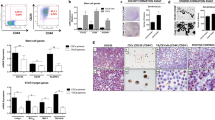
Combination treatment of HDAC inhibitor and radiation results in increased DNA damage and reduced clonogenic survival in the SCs
Based on the heterochromatic patterns, we hypothesised that manipulating chromatin status in the SCs would render them more sensitive to radiation treatment. To achieve this, cells were sorted and treated with a low dose of HDAC inhibitor (0.6 μ M TSA) for 1 h and 30 min followed by 2 Gy irradiation. The treated cells were then fixed 30 min post irradiation and subsequently stained for DNA damage foci (Figure 6A). The effect of TSA was confirmed by western blot using lysates from unsorted cells for acetylated histones where we observed an increase in histone acetylation following treatment (Figure 6B). This is known to correlate with chromatin decondensation (Toth et al, 2004). Following the combination treatment, the number of SCs sustaining DSBs, as evidenced by increased number of cells containing foci, significantly increased (Figure 6Ai). There was no significant increase in the percentage of TA or CB cells containing foci as the majority of these cells contain foci following radiation alone, and hence the effect is already saturated. On quantifying foci number in the SCs we found no increase in number of foci per cell nucleus following TSA treatment (Figure 6Aii). We then assessed the effect of combination treatment on clonogenic recovery and found that the SCs formed significantly fewer colonies following combination treatment compared with irradiation alone (Figure 6C). We concluded from this experiment that the HDAC inhibitor had sensitised the SCs to radiation treatment.
Treatment with an HDAC inhibitor radiosensitises stem cells from benign and malignant primary epithelial cultures (Ai) Stem-like cells (SCs), TA and CB cells were treated with 0.6 μ M TSA for 90 min, irradiated (2 Gy) and then fixed 30 min post IR and stained for γH2AX. Each symbol represents a different patient sample (red symbols indicate prostate cancer and blue symbols indicate BPH) and the black bar represents the median. (Aii) Number of foci per cell nucleus of SCs, following irradiation or TSA plus irradiation. (B) Western blot for acetyl-H3 in unsorted cell lysates following treatment with 0.6 μ M TSA for 2 h. (C) Whole populations of primary epithelial cell cultures were treated with 0.6 μ M TSA for 90 min, irradiated (2 Gy) and sorted into subpopulations 30 min post IR. Surviving fraction following 2 Gy (SF2Gy) and surviving fraction following TSA treatment and 2Gy (SF-TSA-2Gy) were calculated and plotted for SCs following clonogenic assays. Each symbol represents a different patient sample (red symbols indicate prostate cancer and blue symbols indicate BPH), Boxplots show minimum, 25%, median, 75% and maximum. Statistical significance values were measured using the Wilcoxon rank-sum test (*P<0.05).
Discussion
In this study, we present evidence demonstrating that primitive prostate SCs, from freshly cultured patient tissues, are more radioresistant than more differentiated cells, which we show to be independent of patient disease status. We propose that the SCs, by having higher levels of heterochromatin, sustain fewer lethal DSBs, which contributes to increased survival. Significantly, by treating this population with an HDAC inhibitor, DNA damage was increased, resulting in sensitisation of the cells to radiation, thus reducing survival.
Using colony-forming assays, we were able to demonstrate that SCs were less affected by irradiation as compared with the progenitor cells. Although the overall induction of DNA damage was similar between populations (alkaline comet assays), we observed a significant reduction in the percentage of SCs sustaining lethal DSBs (neutral comet assays and DNA damage foci). Lack of activation of the ATM/ATR DNA damage signaling pathways correlated with this population. By quantifying the number of foci in the minority of SCs positive for foci, as well as TA and CB cells, we confirmed that DNA repair was undertaken in all cell types.
We present evidence here that SCs sustain less DNA damage because of increased heterochromatin content. Our results pointed towards the use of HDAC inhibitors, in combination with radiation, as a therapy for prostate cancer. HDAC inhibitors have been heavily investigated for their clinical use and are also in clinical trials for prostate cancer (Marchion and Munster, 2007; Frew et al, 2009; Atadja, 2011). There are encouraging results with HDAC inhibitors targeting proliferating and nonproliferating cells (Burgess et al, 2004). However, they are often being employed as toxins, rather than response modifiers, the latter being what we propose based on the data in Figure 6. Our work shows that a short exposure to sublethal doses of HDAC inhibitors may be enough to sensitise prostate SCs.
It is also possible that less damage is sustained because of the less proliferative nature of SCs. It has previously been shown that adult SCs are predominantly quiescent and that this can reduce accumulation of mutations through DNA replication and contribute to therapy resistance (Mohrin et al, 2010; Blanpain et al, 2011; Li and Bhatia, 2011). Using the vital dye PKH26, we were able to show that prostate stem cells undergo up to four population doublings (in monolayer culture) before exiting the cell cycle (Lang et al, 2010). We also observed here that significantly more progenitor and more differentiated cells (TA and CB cells) are in cycle compared with the SCs.
In summary, radiorecurrent prostate cancer is a significant problem for both physicians and patients because of local and systemic resistance (Ishkanian et al, 2010). The heterogeneity of prostate cancers has been well documented, yet we are the first to report the radiation-resistant phenotype of the primitive SCs and the mechanism behind this resistance. Other radiation resistance mechanisms have been documented, such as increased scavenging of reactive oxygen species (ROS) in breast cancer stem cells and increased efficiency of DNA repair and DNA damage response in glioblastoma cancer stem cells (Bao et al, 2006; Woodward and Bristow, 2009; Diehn et al, 2009a). It remains to be seen whether those play an additional role in radiation resistance of prostate tumours.
Change history
10 December 2013
This paper was modified 12 months after initial publication to switch to Creative Commons licence terms, as noted at publication
References
Atadja PW (2011) HDAC inhibitors and cancer therapy. Prog Drug Res 67: 175–195.
Bao S, Wu Q, McLendon RE, Hao Y, Shi Q, Hjelmeland AB, Dewhirst MW, Bigner DD, Rich JN (2006) Glioma stem cells promote radioresistance by preferential activation of the DNA damage response. Nature 444 (7120): 756–760.
Belyaev IY (2010) Radiation-induced DNA repair foci: spatio-temporal aspects of formation, application for assessment of radiosensitivity and biological dosimetry. Mutat Res 704 (1-3): 132–141.
Blanpain C, Mohrin M, Sotiropoulou PA, Passegue E (2011) DNA-damage response in tissue-specific and cancer stem cells. Cell Stem Cell 8 (1): 16–29.
Brawer MK (2002) Radiation therapy failure in prostate cancer patients: risk factors and methods of detection. Rev Urol 4 (Suppl 2): S2–S11.
Bromfield GP, Meng A, Warde P, Bristow RG (2003) Cell death in irradiated prostate epithelial cells: role of apoptotic and clonogenic cell kill. Prostate Cancer Prostatic Dis 6 (1): 73–85.
Burgess A, Ruefli A, Beamish H, Warrener R, Saunders N, Johnstone R, Gabrielli B (2004) Histone deacetylase inhibitors specifically kill nonproliferating tumour cells. Oncogene 23 (40): 6693–6701.
Catton C, Milosevic M, Warde P, Bayley A, Crook J, Bristow R, Gospodarowicz M (2003) Recurrent prostate cancer following external beam radiotherapy: follow-up strategies and management. Urol Clin North Am 30 (4): 751–763.
Chen K, Huang YH, Chen JL (2013) Understanding and targeting cancer stem cells: therapeutic implications and challenges. Acta Pharmacol Sin 34 (6): 732–740.
Chiou SH, Kao CL, Chen YW, Chien CS, Hung SC, Lo JF, Chen YJ, Ku HH, Hsu MT, Wong TT (2008) Identification of CD133-positive radioresistant cells in atypical teratoid/rhabdoid tumor. PLoS One 3 (5): e2090.
Clevers H (2011) The cancer stem cell: premises, promises and challenges. Nat Med 17 (3): 313–319.
Collins AT, Berry PA, Hyde C, Stower MJ, Maitland NJ (2005) Prospective identification of tumorigenic prostate cancer stem cells. Cancer Res 65 (23): 10946–10951.
Collins AT, Habib FK, Maitland NJ, Neal DE (2001) Identification and isolation of human prostate epithelial stem cells based on alpha(2)beta(1)-integrin expression. J Cell Sci 114 (Pt 21): 3865–3872.
Conley SJ, Gheordunescu E, Kakarala P, Newman B, Korkaya H, Heath AN, Clouthier SG, Wicha MS (2012) Antiangiogenic agents increase breast cancer stem cells via the generation of tumor hypoxia. Proc Natl Acad Sci USA 109 (8): 2784–2789.
Diehn M, Cho RW, Clarke MF (2009a) Therapeutic implications of the cancer stem cell hypothesis. Semin Radiat Oncol 19 (2): 78–86.
Diehn M, Cho RW, Lobo NA, Kalisky T, Dorie MJ, Kulp AN, Qian D, Lam JS, Ailles LE, Wong M, Joshua B, Kaplan MJ, Wapnir I, Dirbas FM, Somlo G, Garberoglio C, Paz B, Shen J, Lau SK, Quake SR, Brown JM, Weissman IL, Clarke MF (2009b) Association of reactive oxygen species levels and radioresistance in cancer stem cells. Nature 458 (7239): 780–783.
Francipane MG, Alea MP, Lombardo Y, Todaro M, Medema JP, Stassi G (2008) Crucial role of interleukin-4 in the survival of colon cancer stem cells. Cancer Res 68 (11): 4022–4025.
Frew AJ, Johnstone RW, Bolden JE (2009) Enhancing the apoptotic and therapeutic effects of HDAC inhibitors. Cancer Lett 280 (2): 125–133.
Hudson DL, Guy AT, Fry P, O'Hare MJ, Watt FM, Masters JR (2001) Epithelial cell differentiation pathways in the human prostate: identification of intermediate phenotypes by keratin expression. J Histochem Cytochem 49 (2): 271–278.
Ishkanian AS, Zafarana G, Thoms J, Bristow RG (2010) Array CGH as a potential predictor of radiocurability in intermediate risk prostate cancer. Acta Oncol 49 (7): 888–894.
Jaamaa S, Af Hallstrom TM, Sankila A, Rantanen V, Koistinen H, Stenman UH, Zhang Z, Yang Z, De Marzo AM, Taari K, Ruutu M, Andersson LC, Laiho M (2010) DNA damage recognition via activated ATM and p53 pathway in nonproliferating human prostate tissue. Cancer Res 70 (21): 8630–8641.
Jones JS (2011) Radiorecurrent prostate cancer: an emerging and largely mismanaged epidemic. Eur Urol 60 (3): 411–412.
Kiviharju-af Hallstrom TM, Jaamaa S, Monkkonen M, Peltonen K, Andersson LC, Medema RH, Peehl DM, Laiho M (2007) Human prostate epithelium lacks Wee1A-mediated DNA damage-induced checkpoint enforcement. Proc Natl Acad Sci USA 104 (17): 7211–7216.
Lang SH, Anderson E, Fordham R, Collins AT (2010) Modeling the prostate stem cell niche: an evaluation of stem cell survival and expansion in vitro. Stem Cells Dev 19 (4): 537–546.
Lemay M, Wood KA (1999) Detection of DNA damage and identification of UV-induced photoproducts using the CometAssay kit. Biotechniques 27 (4): 846–851.
Li L, Bhatia R (2011) Stem cell quiescence. Clin Cancer res 17 (15): 4936–4941.
Mah LJ, El-Osta A, Karagiannis TC (2010) gammaH2AX: a sensitive molecular marker of DNA damage and repair. Leukemia 24 (4): 679–686.
Maitland NJ, Frame FM, Polson ES, Lewis JL, Collins AC (2010) Prostate cancer stem cells: do they have a basal or luminal phenotype? Horm Cancer 2 (1): 47–61.
Marchion D, Munster P (2007) Development of histone deacetylase inhibitors for cancer treatment. Expert Rev Anticancer Ther 7 (4): 583–598.
Miller SJ, Lavker RM, Sun TT (2005) Interpreting epithelial cancer biology in the context of stem cells: tumor properties and therapeutic implications. Biochim Biophys Acta 1756 (1): 25–52.
Mohrin M, Bourke E, Alexander D, Warr MR, Barry-Holson K, Le Beau MM, Morrison CG, Passegue E (2010) Hematopoietic stem cell quiescence promotes error-prone DNA repair and mutagenesis. Cell Stem Cell 7 (2): 174–185.
Nandhakumar S, Parasuraman S, Shanmugam MM, Rao KR, Chand P, Bhat BV (2011) Evaluation of DNA damage using single-cell gel electrophoresis (Comet Assay). J Pharmacol Pharmacother 2 (2): 107–111.
Ostling O, Johanson KJ (1984) Microelectrophoretic study of radiation-induced DNA damages in individual mammalian cells. Biochem Biophys Res Commun 123 (1): 291–298.
Paull TT, Rogakou EP, Yamazaki V, Kirchgessner CU, Gellert M, Bonner WM (2000) A critical role for histone H2AX in recruitment of repair factors to nuclear foci after DNA damage. Curr Biol 10 (15): 886–895.
Puck TT, Marcus PI (1956) Action of x-rays on mammalian cells. J Exp Med 103 (5): 653–666.
Richardson GD, Robson CN, Lang SH, Neal DE, Maitland NJ, Collins AT (2004) CD133, a novel marker for human prostatic epithelial stem cells. J Cell Sci 117 (Pt 16): 3539–3545.
Singh NP, McCoy MT, Tice RR, Schneider EL (1988) A simple technique for quantitation of low levels of DNA damage in individual cells. Exp Cell Res 175 (1): 184–191.
Storch K, Eke I, Borgmann K, Krause M, Richter C, Becker K, Schrock E, Cordes N (2010) Three-dimensional cell growth confers radioresistance by chromatin density modification. Cancer Res 70 (10): 3925–3934.
Sturmey RG, Hawkhead JA, Barker EA, Leese HJ (2009) DNA damage and metabolic activity in the preimplantation embryo. Hum Reprod 24 (1): 81–91.
Swain U, Subba Rao K (2011) Study of DNA damage via the comet assay and base excision repair activities in rat brain neurons and astrocytes during aging. Mech Ageing Dev 132 (8-9): 374–381.
Tice RR, Agurell E, Anderson D, Burlinson B, Hartmann A, Kobayashi H, Miyamae Y, Rojas E, Ryu JC, Sasaki YF (2000) Single cell gel/comet assay: guidelines for in vitro and in vivo genetic toxicology testing. Environ Mol Mutagen 35 (3): 206–221.
Toth KF, Knoch TA, Wachsmuth M, Frank-Stohr M, Stohr M, Bacher CP, Muller G, Rippe K (2004) Trichostatin A-induced histone acetylation causes decondensation of interphase chromatin. J Cell Sci 117 (Pt 18): 4277–4287.
Van Kooij RJ, de Boer P, De Vreeden-Elbertse JM, Ganga NA, Singh N, Te Velde ER (2004) The neutral comet assay detects double strand DNA damage in selected and unselected human spermatozoa of normospermic donors. Int J Androl 27 (3): 140–146.
van Oorschot B, Hovingh SE, Rodermond H, Guclu A, Losekoot N, Geldof AA, Barendsen GW, Stalpers LJ, Franken NA (2013) Decay of gamma-H2AX foci correlates with potentially lethal damage repair in prostate cancer cells. Oncol Rep 29 (6): 2175–2180.
Visvader JE, Lindeman GJ (2008) Cancer stem cells in solid tumours: accumulating evidence and unresolved questions. Nat Rev Cancer 8 (10): 755–768.
Wojewodzka M, Buraczewska I, Kruszewski M (2002) A modified neutral comet assay: elimination of lysis at high temperature and validation of the assay with anti-single-stranded DNA antibody. Mutat Res 518 (1): 9–20.
Woodward WA, Bristow RG (2009) Radiosensitivity of cancer-initiating cells and normal stem cells (or what the Heisenberg uncertainly principle has to do with biology). Semin Radiat Oncol 19 (2): 87–95.
Zafarana G, Bristow RG (2010) Tumor senescence and radioresistant tumor-initiating cells (TICs): let sleeping dogs lie!. Breast Cancer Res 12 (4): 111.
Zhang Z, Yang Z, Jaamaa S, Liu H, Pellakuru LG, Iwata T, Af Hallstrom TM, De Marzo AM, Laiho M (2011) Differential epithelium DNA damage response to ATM and DNA-PK pathway inhibition in human prostate tissue culture. Cell Cycle 10 (20): 3545–3553.
Acknowledgements
This work was supported by a Yorkshire Cancer Research (YCR) Core Grant. FM Frame was funded by a YCR Project Grant (Y253), and D Pellacani was funded by The Freemasons Grand Charity, administered through YCR Project Grant Y256. Additional generous support was received from the Estate of the late Dr E Stout. We thank Urology surgeons Mr(s) L Coombes, G Cooksey and J Hetherington (Castle Hill Hospital, Cottingham) and Mr Mike Stower (York District Hospital) for assistance in supplying prostate tissue. Sincere appreciation goes to the patients from York District Hospital, York and Castle Hill Hospital, Cottingham, for providing prostate tissue. We thank Michael Fraser for the immunofluorescence protocol. We sincerely thank Dr Sheelagh Frame, Dr Stephanie Swift, Dr Gaetano Zafarano and Adam Hirst for critical evaluation of the manuscript.
Author information
Authors and Affiliations
Corresponding author
Additional information
This work is published under the standard license to publish agreement. After 12 months the work will become freely available and the license terms will switch to a Creative Commons Attribution-NonCommercial-Share Alike 3.0 Unported License.
Rights and permissions
From twelve months after its original publication, this work is licensed under the Creative Commons Attribution-NonCommercial-Share Alike 3.0 Unported License. To view a copy of this license, visit http://creativecommons.org/licenses/by-nc-sa/3.0/
About this article
Cite this article
Frame, F., Pellacani, D., Collins, A. et al. HDAC inhibitor confers radiosensitivity to prostate stem-like cells. Br J Cancer 109, 3023–3033 (2013). https://doi.org/10.1038/bjc.2013.691
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/bjc.2013.691
Keywords
This article is cited by
-
DNA damage response signaling pathways and targets for radiotherapy sensitization in cancer
Signal Transduction and Targeted Therapy (2020)
-
Phenotype-independent DNA methylation changes in prostate cancer
British Journal of Cancer (2018)
-
Phospholipase D inhibitors reduce human prostate cancer cell proliferation and colony formation
British Journal of Cancer (2018)
-
The immunosuppressive cytokine interleukin-4 increases the clonogenic potential of prostate stem-like cells by activation of STAT6 signalling
Oncogenesis (2017)
-
Latent Kaposi’s sarcoma-associated herpesvirus infection in bladder cancer cells promotes drug resistance by reducing reactive oxygen species
Journal of Microbiology (2016)