Abstract
Background:
Levels of the pro-tumorigenic prostaglandin PGE2 are increased in colorectal cancer, previously attributed to increased synthesis through COX-2 upregulation and, more recently, to decreased catabolism. The functionally linked genes 15-prostaglandin dehydrogenase (15-PGDH) and the prostaglandin transporter PGT co-operate in prostaglandin degradation and are downregulated in colorectal cancer. We previously reported repression of 15-PGDH expression by the Wnt/β-catenin pathway, commonly deregulated during early colorectal neoplasia. Here we asked whether β-catenin also regulates PGT expression.
Methods:
The effect of β-catenin deletion in vivo was addressed by PGT immunostaining of β-catenin−/lox-villin-cre-ERT2 mouse tissue. The effect of siRNA-mediated β-catenin knockdown and dnTCF4 induction in vitro was addressed by semi-quantitative and quantitative real-time RT-PCR and immunoblotting.
Results:
This study shows for the first time that deletion of β-catenin in murine intestinal epithelium in vivo upregulates PGT protein, especially in the crypt epithelium. Furthermore, β-catenin knockdown in vitro increases PGT expression in both colorectal adenoma- and carcinoma-derived cell lines, as does dnTCF4 induction in LS174T cells.
Conclusions:
These data suggest that β-catenin employs a two-pronged approach to inhibiting prostaglandin turnover during colorectal neoplasia by repressing PGT expression in addition to 15-PGDH. Furthermore, our data highlight a potential mechanism that may contribute to the non-selective NSAID aspirin’s chemopreventive efficacy.
Similar content being viewed by others
Main
Recent studies in the Lancet (Algra and Rothwell, 2012; Rothwell et al, 2012a, 2012b) have reinforced interest in the potential value of using NSAIDs, such as aspirin, in colorectal cancer chemoprevention. Over much of the last few decades, a major focus of colorectal cancer chemoprevention has been inhibition of COX-2, an inducible cyclooxygenase isoform that is upregulated at the medium/large adenoma stage, and to which the elevated levels of the protumorigenic prostaglandin PGE2 have previously been attributed (Rigas et al, 1993; Eberhart et al, 1994; Elder et al, 2002). However, several lines of evidence suggest a potential role for COX-1 in colorectal neoplasia. For example, tumorigenesis in animal models can be suppressed by deletion of either COX-1 or COX-2 genes (Chulada et al, 2000), or by administration of a COX-1-selective inhibitor (Kitamura et al, 2002), though the precise role of COX-1 in intestinal neoplasia is unclear. Our recent paper in Gut (Smartt et al, 2012) highlighted a mechanism by which COX-1 could contribute to early colorectal cancer development. We showed that β-catenin, activated at the earliest stages of colorectal neoplasia, can repress expression of the colorectal tumour suppressor and prostaglandin catabolising enzyme 15-prostaglandin dehydrogenase (15-PGDH). Here, we now show that β-catenin also represses expression of a second gene crucial for prostaglandin catabolism, the prostaglandin transporter PGT. PGT (aka SLCO2A1) mediates uptake of secreted prostaglandins, enabling their oxidative inactivation by cytoplasmic 15-PGDH (Nomura et al, 2004). Like 15-PGDH, downregulation of PGT has been reported in both human colorectal tumours and in pre-malignant adenomas in APCmin/+ mice, and this was suggested to result, at least in part, from epigenetic silencing (Holla et al, 2008). However, we hypothesised that β-catenin may also have a role in repression of PGT expression in colorectal cancer, as we reported previously for 15-PGDH. Here we show that modulating β-catenin expression or function increases PGT expression, both in the intestinal epithelium in vivo, and in colorectal adenoma and carcinoma cells in vitro. Our data suggest that β-catenin co-ordinately regulates prostaglandin turnover through the negative regulation of both PGT and 15-PGDH expression, and highlight a potential mechanism that could contribute to the chemopreventive efficacy of the non-selective NSAID aspirin.
Materials and methods
The colon carcinoma-derived cell lines HCT15, HCT116, HT29, LOVO, LS174T, SW480 and SW620, obtained from the American Type Culture Collection (Rockville, MD, USA); the HCA7 colony 29 (HCA7) colon carcinoma cell line, a kind gift of Susan Kirkland (Kirkland, 1985); the dox-inducible dnTCF4-expressing LS174T/dnTCF4 cell line, a kind gift from Hans Clevers (van de Wetering et al, 2002); and colon adenoma-derived cell lines PC/AA/C1, PC/AA/C1/SB10C, PC/BH/C1, S/AN/C1 and S/RG/C2 derived in this laboratory (Paraskeva et al, 1984, 1989; Williams et al, 1990) were maintained as described previously (Paraskeva et al, 1984; Moore et al, 2009), except for PC/AA/C1 and PC/AA/C1/SB10C, which were maintained on conditioned medium (Williams et al, 1990). Immunohistochemical staining using a rabbit polyclonal PGT antibody (kind gift of Michel Fortier, Quebec, Canada) and inducible intestinal β-catenin ablation in mice were carried out and validated as previously described (Smartt et al, 2012), as was intestinal epithelial cell fractionation (see also Mariadason et al, 2005). RNA interference, immunoblotting and mRNA preparation were also performed as previously described (Smartt et al, 2012). Semi-quantitative RT-PCR was carried out as in Chell et al (2006), with minor modifications, and quantitative real-time RT-PCR was carried out as described previously (Moore et al, 2009), using PGT primers from Qiagen (Crawley, West Sussex, UK).
Results
Preliminary studies suggested that, similar to 15-PGDH, PGT also shows an expression gradient in the human intestinal epithelium, being highest in the differentiated luminal/villus compartment (Figure 1A). A similar PGT expression gradient was also observed in the murine small intestinal epithelium, both at the mRNA (Figure 1B) and protein level (Figure 1C). As Wnt/β-catenin transcriptional activity is known to be highest in the proliferative crypt compartment (van de Wetering et al, 2002; Kosinski et al, 2007), we hypothesised that PGT may also be repressed by β-catenin in intestinal epithelial cells. Importantly, the gradient of PGT expression was lost following inducible β-catenin ablation (Figure 1D; Fevr et al, 2007). Elevated PGT expression was particularly noticeable in crypt epithelia (compare Figure 1F with E), where β-catenin activity is normally highest (Batlle et al, 2002; van de Wetering et al, 2002). This increase is consistent with previously published microarray analysis (1.67-fold increase, Fevr et al, 2007), confirming that β-catenin represses PGT expression in the normal murine intestinal epithelium.
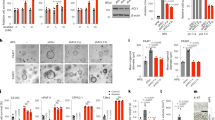
(A, B) Gradient of PGT protein and mRNA expression with differentiation along the crypt–villus axis in intestinal epithelium. (A) PGT immunohistochemistry shows high PGT expression in the differentiated human villus epithelium. Scale bar represents 50 μm. (B) Differential fractionation of the murine intestinal epithelium followed by microarray gene expression analysis (Mariadason et al, 2005) shows that, like the differentiation marker villin, PGT mRNA expression increases along the crypt–villus axis. In contrast, expression of the proliferation marker PCNA and the Wnt/β-catenin target c-Myc both decrease along the crypt–villus axis. Data represents expression relative to fraction 10 in fractions 10, 8, 6, 4, 2 and 1. This gradient of PGT expression is confirmed at the protein level by immunohistochemistry (see C). (C–F) Inducible β-catenin ablation increases crypt epithelial PGT expression levels. Deletion of β-catenin was induced in β-catenin−/lox-villin-creERT2 mice by tamoxifen injection (D, F); injected β-catenin+/lox-villin-creERT2 mice (C, E) were used as a control. PGT staining shows PGT expression throughout the crypt–villus axis in the absence of β-catenin (D), particularly evident in crypt and lower villus epithelium (F as compared with E) (representative examples from 96 h post induction). Scale bars represent 50 μm.
We then hypothesised that β-catenin may also repress PGT expression in human colorectal cancer cells, as is the case for 15-PGDH. Indeed, in line with this hypothesis, basal PGT levels are reportedly very low to undetectable in most colorectal carcinoma cell lines (Holla et al, 2008). We confirmed and extended this observation to include cell lines derived from sporadic (S/RG/C2, S/AN/C1) and familial adenomatous polyposis patient (PC/AA/C1, PC/BH/C1) adenomas and one in-vitro-transformed adenoma cell line (PC/AA/C1/SB10C) (Figure 2A). Indeed, in our hands, PGT mRNA was only readily detectable in LoVo carcinoma-derived and PC/BH/C1 adenoma-derived cells under basal conditions. Notably, siRNA-mediated knockdown of β-catenin increased PGT mRNA expression in both adenoma- and carcinoma-derived cell lines (Figure 2B and C). In addition, PGT mRNA levels were consistently increased in the colorectal carcinoma cell line LS174T/dnTCF4, 48 h following induction of dnTCF4, a dominant-negative form of this β-catenin-binding partner that is unable to bind β-catenin (Figure 2D and E). Hence, taken together, these data suggest that β-catenin represses PGT expression in both the normal intestinal epithelium and in colorectal cancer.
(A) PGT mRNA expression screen in colorectal adenoma- and carcinoma-derived cell lines. PC/AA/C1, S/AN/C1, PC/BH/C1 and S/RG/C2 are adenoma-derived cell lines, PC/AA/C1/SB10C is an in-vitro-transformed adenoma-derived cell line and the remainder are carcinoma-derived. Semi-quantitative real-time PCR analysis confirmed that most colorectal carcinoma-derived cell lines express low levels of PGT with the exception of LoVo. Interestingly, a similar pattern was seen in our adenoma-derived cell lines, with mostly very low expression with the exception of PC/BH/C1 cells (NTC=no template control, −RT=no reverse transcriptase enzyme control). (B, C) β-catenin siRNA knockdown increases PGT expression. (B) Immunoblotting (IB) demonstrating that transient β-catenin siRNA transfection effectively reduced β-catenin protein levels in S/RG/C2, SW480 and LoVo cell lines (48 h). Semi-quantitative PCR analysis (PCR) revealed a marked and consistent increase in PGT mRNA levels in S/RG/C2, SW480 and LoVo cells following β-catenin siRNA-mediated knockdown (48 h). (C) Quantitative real-time PCR analysis confirms the increase in PGT mRNA apparent in B. (D) Induction of dnTCF4 increases PGT expression immunoblotting demonstrates effective induction in LS174T/dnTCF4 cells of dnTCF4 with 1 μg ml−1 doxycycline (dox; 48 h). Semi-quantitative PCR analysis (PCR) demonstrates a consistent increase in PGT mRNA levels in LS174T/dnTCF4 cells following dox-mediated induction of dnTCF4 (48 h). (E) Quantitative real-time PCR analysis confirms the increase in PGT mRNA apparent in D. Results shown are representative of a minimum of three independent repeat experiments. α-tubulin and β-actin serve as loading controls.
Discussion
In this article, we have identified a novel link between two important pathways in colorectal neoplasia, Wnt/β-catenin and PGE2 signalling, through the negative regulation of PGT expression. Therefore, similar to 15-PGDH, PGT expression could be widely downregulated at a very early stage of colorectal neoplasia in sporadic tumours as well as those arising in the context of a germline APC mutation. Downregulation of PGT, in addition to 15-PGDH, may constitute a very effective means of increasing local PGE2 levels as impaired PGT-mediated prostaglandin import would be expected to directly increase extracellular prostaglandin concentrations available to interact with cell surface receptors.
The ability of β-catenin to downregulate both 15-PGDH and PGT, two crucial regulators of prostaglandin catabolism, points towards the importance of elevated COX-1-derived prostaglandin levels during early colorectal neoplasia before COX-2 upregulation, and may go some way to explain the particular efficacy in colorectal cancer chemoprevention of the non-selective NSAID aspirin.
Change history
11 October 2012
This paper was modified 12 months after initial publication to switch to Creative Commons licence terms, as noted at publication
References
Algra AM, Rothwell PM (2012) Effects of regular aspirin on long-term cancer incidence and metastasis: a systematic comparison of evidence from observational studies versus randomised trials. Lancet Oncol 13 (5): 518–527
Batlle E, Henderson JT, Beghtel H, van den Born MM, Sancho E, Huls G, Meeldijk J, Robertson J, van de Wetering M, Pawson T, Clevers H (2002) Beta-catenin and TCF mediate cell positioning in the intestinal epithelium by controlling the expression of EphB/ephrinB. Cell 111 (2): 251–263
Chell SD, Witherden IR, Dobson RR, Moorghen M, Herman AA, Qualtrough D, Williams AC, Paraskeva C (2006) Increased EP4 receptor expression in colorectal cancer progression promotes cell growth and anchorage independence. Cancer Res 66 (6): 3106–3113
Chulada PC, Thompson MB, Mahler JF, Doyle CM, Gaul BW, Lee C, Tiano HF, Morham SG, Smithies O, Langenbach R (2000) Genetic disruption of Ptgs-1, as well as Ptgs-2, reduces intestinal tumorigenesis in Min mice. Cancer Res 60 (17): 4705–4708
Eberhart CE, Coffey RJ, Radhika A, Giardiello FM, Ferrenbach S, DuBois RN (1994) Up-regulation of cyclooxygenase 2 gene expression in human colorectal adenomas and adenocarcinomas. Gastroenterology 107 (4): 1183–1188
Elder DJ, Baker JA, Banu NA, Moorghen M, Paraskeva C (2002) Human colorectal adenomas demonstrate a size-dependent increase in epithelial cyclooxygenase-2 expression. J Pathol 198 (4): 428–434
Fevr T, Robine S, Louvard D, Huelsken J (2007) Wnt/beta-catenin is essential for intestinal homeostasis and maintenance of intestinal stem cells. Mol Cell Biol 27 (21): 7551–7559
Holla VR, Backlund MG, Yang P, Newman RA, DuBois RN (2008) Regulation of prostaglandin transporters in colorectal neoplasia. Cancer Prev Res (Phila) 1 (2): 93–99
Kirkland SC (1985) Dome formation by a human colonic adenocarcinoma cell line (HCA-7). Cancer Res 45 (8): 3790–3795
Kitamura T, Kawamori T, Uchiya N, Itoh M, Noda T, Matsuura M, Sugimura T, Wakabayashi K (2002) Inhibitory effects of mofezolac, a cyclooxygenase-1 selective inhibitor, on intestinal carcinogenesis. Carcinogenesis 23 (9): 1463–1466
Kosinski C, Li VS, Chan AS, Zhang J, Ho C, Tsui WY, Chan TL, Mifflin RC, Powell DW, Yuen ST, Leung SY, Chen X (2007) Gene expression patterns of human colon tops and basal crypts and BMP antagonists as intestinal stem cell niche factors. Proc Natl Acad Sci USA 104 (39): 15418–15423
Mariadason JM, Nicholas C, L’Italien KE, Zhuang M, Smartt HJ, Heerdt BG, Yang W, Corner GA, Wilson AJ, Klampfer L, Arango D, Augenlicht LH (2005) Gene expression profiling of intestinal epithelial cell maturation along the crypt-villus axis. Gastroenterology 128 (4): 1081–1088
Moore AE, Greenhough A, Roberts HR, Hicks DJ, Patsos HA, Williams AC, Paraskeva C (2009) HGF/Met signalling promotes PGE(2) biogenesis via regulation of COX-2 and 15-PGDH expression in colorectal cancer cells. Carcinogenesis 30 (10): 1796–1804
Nomura T, Lu R, Pucci ML, Schuster VL (2004) The two-step model of prostaglandin signal termination: in vitro reconstitution with the prostaglandin transporter and prostaglandin 15 dehydrogenase. Mol Pharmacol 65 (4): 973–978
Paraskeva C, Buckle BG, Sheer D, Wigley CB (1984) The isolation and characterization of colorectal epithelial cell lines at different stages in malignant transformation from familial polyposis coli patients. Int J Cancer 34 (1): 49–56
Paraskeva C, Finerty S, Mountford RA, Powell SC (1989) Specific cytogenetic abnormalities in two new human colorectal adenoma-derived epithelial cell lines. Cancer Res 49 (5): 1282–1286
Rigas B, Goldman IS, Levine L (1993) Altered eicosanoid levels in human colon cancer. J Lab Clin Med 122 (5): 518–523
Rothwell PM, Price JF, Fowkes FG, Zanchetti A, Roncaglioni MC, Tognoni G, Lee R, Belch JF, Wilson M, Mehta Z, Meade TW (2012a) Short-term effects of daily aspirin on cancer incidence, mortality, and non-vascular death: analysis of the time course of risks and benefits in 51 randomised controlled trials. Lancet 379 (9826): 1602–1612
Rothwell PM, Wilson M, Price JF, Belch JF, Meade TW, Mehta Z (2012b) Effect of daily aspirin on risk of cancer metastasis: a study of incident cancers during randomised controlled trials. Lancet 379 (9826): 1591–1601
Smartt HJ, Greenhough A, Ordonez-Moran P, Talero E, Cherry CA, Wallam CA, Parry L, Al Kharusi M, Roberts HR, Mariadason JM, Clarke AR, Huelsken J, Williams AC, Paraskeva C (2012) Beta-catenin represses expression of the tumour suppressor 15-prostaglandin dehydrogenase in the normal intestinal epithelium and colorectal tumour cells. Gut 61 (9): 1306–1314
van de Wetering M, Sancho E, Verweij C, de Lau W, Oving I, Hurlstone A, van der Horn K, Batlle E, Coudreuse D, Haramis AP, Tjon-Pon-Fong M, Moerer P, van den Born M, Soete G, Pals S, Eilers M, Medema R, Clevers H (2002) The beta-catenin/TCF-4 complex imposes a crypt progenitor phenotype on colorectal cancer cells. Cell 111 (2): 241–250
Williams AC, Harper SJ, Paraskeva C (1990) Neoplastic transformation of a human colonic epithelial cell line: in vitro evidence for the adenoma to carcinoma sequence. Cancer Res 50 (15): 4724–4730
Acknowledgements
This work was supported by a Programme Grant (C19/A5301) from Cancer Research UK and by the John James Bristol Foundation. We thank Professor Victor Schuster for valuable discussion.
Author information
Authors and Affiliations
Corresponding author
Additional information
This work is published under the standard license to publish agreement. After 12 months the work will become freely available and the license terms will switch to a Creative Commons Attribution-NonCommercial-Share Alike 3.0 Unported License.
Rights and permissions
From twelve months after its original publication, this work is licensed under the Creative Commons Attribution-NonCommercial-Share Alike 3.0 Unported License. To view a copy of this license, visit http://creativecommons.org/licenses/by-nc-sa/3.0/
About this article
Cite this article
Smartt, H., Greenhough, A., Ordóñez-Morán, P. et al. β-catenin negatively regulates expression of the prostaglandin transporter PGT in the normal intestinal epithelium and colorectal tumour cells: a role in the chemopreventive efficacy of aspirin?. Br J Cancer 107, 1514–1517 (2012). https://doi.org/10.1038/bjc.2012.430
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/bjc.2012.430
Keywords
This article is cited by
-
Metabolic stress induces a Wnt-dependent cancer stem cell-like state transition
Cell Death & Disease (2015)
-
Intracellular EP2 prostanoid receptor promotes cancer-related phenotypes in PC3 cells
Cellular and Molecular Life Sciences (2015)