Abstract
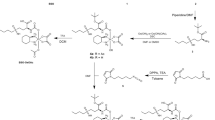
The prodrug N-[4-(daunorubicin-N-carbonyl-oxymethyl)phenyl] O-beta-glucuronyl carbamate (DNR-GA3) was synthesized for specific activation by human beta-glucuronidase, released in necrotic areas of tumour lesions. In vitro, DNR-GA3 was 18 times less toxic than daunorubicin (DNR) and the prodrug was completely activated to the parent drug by human beta-glucuronidase. The maximum tolerated dose of DNR-GA3 in nude mice bearing s.c. human ovarian cancer xenografts was 6-10 times higher than that of DNR. The prodrug was cleared more rapidly from the circulation (elimination t1/2 = 20 min) than the parent drug (elimination t1/2 = 720 min). The anti-tumour effects of DNR-GA3 and DNR were investigated in four different human ovarian cancer xenografts OVCAR-3, FMa, A2780 and MRI-H-207 at a mean tumour size between 100 and 200 mm3. In three out of four of these tumour lines, the prodrug given i.v. at the maximum tolerated dose ranging from 150 to 250 mg kg(-1) resulted in a maximum tumour growth inhibition from 82% to 95%. The standard treatment with DNR at a dose of 8 mg kg(-1) given i.v. weekly x 2 resulted only in a maximum tumour growth inhibition from 40% to 47%. Tumour line FMa did not respond to DNR, nor to DNR-GA3. Treatment with DNR-GA3 was also given to mice with larger tumours that would contain more necrosis (mean size 300-950 mm3). The specific growth delay by DNR-GA3 was extended from 2.1 to 4.4 in OVCAR-3 xenografts and from 4.4 to 6.0 in MRI-H-207 xenografts. Our data indicate that DNR-GA3 is more effective than DNR and may be especially of use for treatment of tumours with areas of necrosis.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 24 print issues and online access
$259.00 per year
only $10.79 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Houba, P., Boven, E., Erkelens, C. et al. The efficacy of the anthracycline prodrug daunorubicin-GA3 in human ovarian cancer xenografts. Br J Cancer 78, 1600–1606 (1998). https://doi.org/10.1038/bjc.1998.729
Issue Date:
DOI: https://doi.org/10.1038/bjc.1998.729
This article is cited by
-
Evaluation of Cytotoxic Properties of a Cyclopamine Glucuronide Prodrug in Rat Glioblastoma Cells and Tumors
Journal of Molecular Neuroscience (2015)
-
Anti-tumour activity and toxicity of the new prodrug9-aminocamptothecin glucuronide (9ACG) in mice
British Journal of Cancer (2002)