Abstract
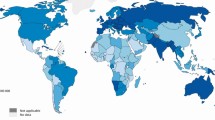
This is a study of 5595 head and neck cancer patients treated during 1987-89 at TMH, Mumbai. The study included 1970 oral cancers (ICD 140-145), 1495 oropharyngeal cancers (ICD 1410, 1453, 146), 1255 hypopharyngeal cancers (ICD 148), 125 nasopharyngeal cancers (ICD 147) and 750 laryngeal cancers (ICD 161). The clinical extent of disease at presentation was based on TNM group staging (UICC 1978). For the majority of sites, patients attended the hospital during stage III and stage IV of the disease; the only exception was for cancers of the lower lip, anterior tongue and vocal cord when between 46.2% and 56.5% of patients with localized cancer (stage I and II) were seen. Generally, surgery either alone or with radiation has been administered for oral cancer patients whereas radiation either alone or in combination with chemotherapy was administered for other head and neck sites. The overall 5-year survival rate was in the range of 20-43% for oral cancer, 8-25% for pharyngeal cancers and 25-62% for laryngeal cancer. The 5-year relative survival rates were more or less in agreement with the results published by the Eurocare study for head and neck cancers. The importance of primary prevention in head and neck cancer is stressed.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 24 print issues and online access
$259.00 per year
only $10.79 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Rao, D., Shroff, P., Chattopadhyay, G. et al. Survival analysis of 5595 head and neck cancers -- results of conventional treatment in a high-risk population. Br J Cancer 77, 1514–1518 (1998). https://doi.org/10.1038/bjc.1998.249
Issue Date:
DOI: https://doi.org/10.1038/bjc.1998.249
This article is cited by
-
Hard Palate Metastasis from Rectal Adenocarcinoma
Clinical Journal of Gastroenterology (2022)
-
Mundhöhlen- und Pharynxkarzinome: Inzidenz, Mortalität und Überleben in Deutschland
Bundesgesundheitsblatt - Gesundheitsforschung - Gesundheitsschutz (2021)
-
Multiple distant metastasis of tongue squamous cell carcinoma after surgical operation and radiotherapy — a case report and literature review
The Chinese-German Journal of Clinical Oncology (2010)
-
Distant metastases of a squamous cell carcinoma of the tongue in peripheral skeletal muscles and adjacent soft tissues
Head & Face Medicine (2008)
-
Replication-Competent Herpes Simplex Virus Vector G207 and Cisplatin Combination Therapy for Head and Neck Squamous Cell Carcinoma
Neoplasia (1999)