Abstract
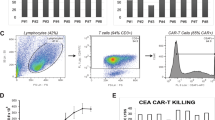
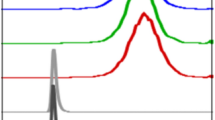
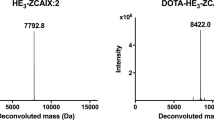
The monoclonal antibody A33 recognises a tumour-associated antigen on human colorectal carcinoma, and has undergone preliminary evaluation in the clinic where selective localisation to hepatic metastases has been demonstrated [Welt et al. (1994) J. Clin. Oncol. 12, 1561-1571]. A33 and an A33 tri-fab fragment (TFM) were labelled with 90Y via a stable macrocyclic ligand for biodistribution and therapy studies in nude mice bearing SW1222 colon carcinoma xenografts. Biodistribution studies demonstrated tumour localisation for both A33 IgG and TFM with low bone, liver and kidney levels. Clearance of TFM from the blood was much faster than IgG and this led to lower tumour accumulation for TFM but superior tumour-blood ratios. The maximum per cent injected dose per g localised to tumour was 35.9% +/- 5.3% for A33 IgG and 12.9% +/- 4.6% for A33 TFM with tumour-blood ratios at 48 h after administration of 5.6 +/- 1.8 and 29.2 +/- 9.8 respectively. Autoradiography studies with 125I-labelled A33 IgG and TFM demonstrated a homogeneous distribution within tumour tissue which was not observed with other anti-colorectal tumour antibodies. TFM penetrated into the tumour tissue more rapidly than IgG. In therapy studies, a single dose of 90Y-A33 IgG (250 microCi per mouse) or 90Y-A33 TFM (300 microCi per mouse) led to complete regression of 2-week-old tumour xenografts with long-term tumour-free survivors. A transient drop in white blood cell count was observed with both IgG and TFM but was significantly more pronounced with IgG. The cell count fell to 8.4% of control for IgG, whereas with TFM cell counts fell to 51% of control before recovery. These results indicate that the more rapid blood clearance of 90Y-TFM confers reduced toxicity compared with 90Y-IgG although similar therapeutic effects are achieved. When the dose of 90Y-IgG was adjusted to give the same dose to tumour achieved with 300 microCi 90Y-TFM, a lesser therapeutic effect was observed. This may be owing to more rapid tumour penetration achieved with TFM. Both A33 IgG and TFM demonstrated potent anti-tumour effects against human tumour xenografts in this mouse model system. The stability of these 90Y-labelled conjugates and their effective tumour penetration are promising for the development of humanised reagents for clinical studies.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 24 print issues and online access
$259.00 per year
only $10.79 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Antoniw, P., Farnsworth, A., Turner, A. et al. Radioimmunotherapy of colorectal carcinoma xenografts in nude mice with yttrium-90 A33 IgG and Tri-Fab (TFM). Br J Cancer 74, 513–524 (1996). https://doi.org/10.1038/bjc.1996.395
Issue Date:
DOI: https://doi.org/10.1038/bjc.1996.395
This article is cited by
-
Theranostic pretargeted radioimmunotherapy of colorectal cancer xenografts in mice using picomolar affinity 86Y- or 177Lu-DOTA-Bn binding scFv C825/GPA33 IgG bispecific immunoconjugates
European Journal of Nuclear Medicine and Molecular Imaging (2016)
-
Multi-Specific Antibodies for Cancer Immunotherapy
BioDrugs (2014)
-
Protein-based tumor molecular imaging probes
Amino Acids (2011)
-
Transcriptional regulation of A33 antigen expression by gut-enriched Krüppel-like factor
Oncogene (2003)
-
Dosimetric evaluation and radioimmunotherapy of anti-tumour multivalent Fab′ fragments
British Journal of Cancer (1999)