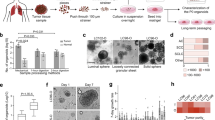
Abstract
A total of 83 specimens of surgically resected tumours from 78 patients with oesophageal cancer were assayed for drug sensitivity using an adhesive tumour cell culture system (LifeTrac CSA assay). Seventyone of 83 specimens had a sufficient number of cells to permit growth in culture and 57 of 71 (80%) were evaluable for drug response. Cells (3 x 10(3) ml-1 well-1) were cultured for 14 days and exposed to drugs on days 3-8. Growing cells were confirmed as cancer cells by immunohistochemical staining. IC90 values against several anti-cancer drugs were determined and population distributions of IC90 for each drug served as the basis for judging sensitivity. The 10th percentiles of IC90 (microgram ml-1) for CDDP, 5-FU, DOX, CPM, MTX, VP16, IFOS, VDS, BLM and CDDP + 5-FU were 0.3, 0.16, 0.005, 0.9, 0.006, 0.09, 0.8, 0.006, 0.04 and 0.15 + 0.09 respectively. The population distribution of IC90 against each drug showed a specific pattern that was very similar among histopathological gradings and stages of the disease. This system appeared to be a clinically applicable drug sensitivity test for human oesophageal cancer.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 24 print issues and online access
$259.00 per year
only $10.79 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Terashima, M., Hayashi, K., Fukushima, M. et al. Drug sensitivity testing for clinical samples from oesophageal cancer using adhesive tumour cell culture system. Br J Cancer 74, 73–77 (1996). https://doi.org/10.1038/bjc.1996.318
Issue Date:
DOI: https://doi.org/10.1038/bjc.1996.318
This article is cited by
-
How Each Component of Betel Quid Is Involved in Oral Carcinogenesis: Mutual Interactions and Synergistic Effects with Other Carcinogens—a Review Article
Current Oncology Reports (2019)
-
Betel Nut Use among First and Second Generation Bangladeshi Women in London, UK
Journal of Immigrant and Minority Health (2007)
-
Cancer incidence in the south Asian population of England (1990–92)
British Journal of Cancer (1999)