Abstract
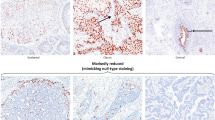
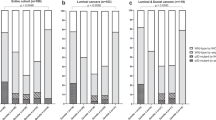
Primary carcinomas from 46 patients were screened for TP53 alterations. Immunohistochemistry demonstrated nuclear TP53 protein accumulation in 22 (48%) cases using the polyclonal CM1 antiserum, whereas 15 (33%) cases showed positive nuclear staining with the mononuclear antibody PAb 1801. Constant denaturant gel electrophoresis (CDGE) was used to screen 27 of the vaginal carcinomas for mutations in the conserved regions of the TP53 gene (exons 5-8). Six of these tumours (22%) contained mutations: four were found in exon 5 and two in exon 8. A total of 50% of the primary vaginal carcinomas carried a TP53 alteration. These results indicate that TP53 abnormalities may be involved in the development of these tumours. However, there was no significant association between TP53 abnormalities and survival.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 24 print issues and online access
$259.00 per year
only $10.79 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Skomedal, H., Kristensen, G., Helland, Å. et al. TP53 gene mutations and protein accumulation in primary vaginal carcinomas. Br J Cancer 72, 129–133 (1995). https://doi.org/10.1038/bjc.1995.288
Issue Date:
DOI: https://doi.org/10.1038/bjc.1995.288