Abstract
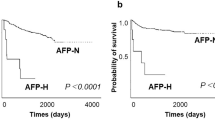
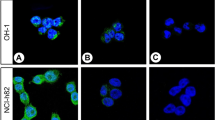
p53 expression was examined in 55 gastric and 107 colorectal carcinomas with an immunoperoxidase technique, using the polyclonal antibody CM1 on routinely fixed, paraffin embedded tissue. p53 protein was detected in 47% gastric and in 46% colorectal carcinomas and found to correlate with stage of disease and unfavourable clinical outcome (P less than 0.001). Thus, the proportion of positively reacting neoplasms increased as the stage progressed, tumours which had invaded regional lymph-nodes overexpressed p53 more frequently than localised carcinomas and an elevated level of p53 was associated with early relapse and death. In colorectal carcinoma p53 positivity was also linked with site and macroscopic configuration of the primary tumour and was most frequently expressed in carcinomas from the rectum and in ulcerative tumours. p53 overexpression was irrespective of tumour grade. Uniform negative reactivity with anti-p53 antibody was seen in normal epithelium adjacent to carcinoma, intestinal metaplasia, atrophic gastritis and in colonic adenomas. There was a good correlation between immunohistochemical staining on paraffin and frozen sections. These studies suggest that in gastric and colorectal carcinoma, immunohistochemical detection of p53 protein in routinely fixed tissue can be used along with other established parameters to assess prognostic outcome, especially to identify patients with poor short-term prognosis.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 24 print issues and online access
$259.00 per year
only $10.79 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Starzynska, T., Bromley, M., Ghosh, A. et al. Prognostic significance of p53 overexpression in gastric and colorectal carcinoma. Br J Cancer 66, 558–562 (1992). https://doi.org/10.1038/bjc.1992.314
Issue Date:
DOI: https://doi.org/10.1038/bjc.1992.314
This article is cited by
-
Different effects of p53 protein overexpression on the survival of gastric cancer patients according to Lauren histologic classification: a retrospective study
Gastric Cancer (2021)
-
Immunohistochemical investigation of prognostic biomarkers in resected colorectal liver metastases: a systematic review and meta-analysis
Cancer Cell International (2018)
-
Prognostic values of apoptosis-stimulating P53-binding protein 1 and 2 and their relationships with clinical characteristics of esophageal squamous cell carcinoma patients: a retrospective study
Chinese Journal of Cancer (2017)
-
Poorly differentiated adenocarcinoma of the colon: subsite location and clinicopathologic features
International Journal of Colorectal Disease (2015)
-
CELLFOOD™ induces apoptosis in human mesothelioma and colorectal cancer cells by modulating p53, c-myc and pAkt signaling pathways
Journal of Experimental & Clinical Cancer Research (2014)