Abstract
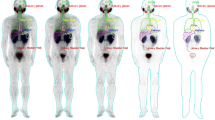
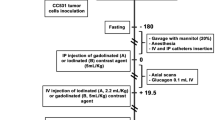
The effect of photodynamic therapy (PDT) on tumour perfusion in both anaplastic (R3327-AT) and well differentiated (R3327-H) Dunning prostatic tumours was studied using the radiopharmaceutical 99Technetium hexamethylpropyleneamine oxime (99mTc-HMPAO). Tumours in the left flanks of rats (Copenhage x Fischer, F1 hybrids) were treated with interstitial PDT when their volumes reached 2-3 cm3. Qualitative and quantitative data from pre- and post-PDT scintigraphy revealed a light-dose-dependent shut-down of tumour perfusion which was also time-dependent. Maximal shut-down, following a 1,600 J light-dose, occurred about 8 h post-PDT. Light exposure 2 h after the intravenous administration of the photosensitiser (Photofrin II) produced a greater vascular shut-down than did light exposure 24 h after the administration of the drug. Regional differences in perfusion within treated and non-treated tumours were measured by tomographic procedures. Light-dose-dependent volumes of perfusion shut-down were demonstrated in addition to the naturally occurring regional differences in tumour perfusion. This radiopharmaceutical may have future utility for monitoring the clinical treatment of solid tumours with PDT.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 24 print issues and online access
$259.00 per year
only $10.79 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Moore, R., Chapman, J., Mokrzanowski, A. et al. Non-invasive monitoring of photodynamic therapy with 99technetium HMPAO scintigraphy. Br J Cancer 65, 491–497 (1992). https://doi.org/10.1038/bjc.1992.102
Issue Date:
DOI: https://doi.org/10.1038/bjc.1992.102