Abstract
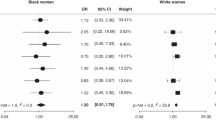
A collaborative, hospital-based case-control study was conducted at 12 participating centres in 10 countries. Based on data from personal interviews of 2,116 women with newly diagnosed breast cancer and 12,077 controls, the relative risk of breast cancer in women who ever used oral contraceptives was estimated to be 1.15 (1.02, 1.29). Estimated values of this relative risk based on data from three developed and seven developing countries were 1.07 (0.91, 1.26) and 1.24 (1.05, 1.47) respectively; these estimates are not significantly different (P = 0.22). Estimates for women under and over age 35 were 1.26 (0.95, 1.66) and 1.12 (0.98, 1.27), respectively, and these estimates are also not significantly different (P = 0.38). Risk was highest in recent and current users and declined with time since last use regardless of use. Risk did not increase with duration of use after stratifying on time since last use. Risk did not increase significantly with increasing duration of use before age 25 or before a first live birth. However, a relative risk of 1.5 that was of borderline statistical significance was observed in women who used oral contraceptives for more than 2 years before age 25. No single source of bias or confounding was identified that could explain the small increases in risk that were observed. Chance alone is also an unlikely explanation. The results could be due to a combination of chance and potential sources of bias, or they could represent a weak causal relationship.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 24 print issues and online access
$259.00 per year
only $10.79 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
Author information
Consortia
Additional information
Participating investigators are listed at the end of this paper.
Rights and permissions
About this article
Cite this article
The WHO Collaborative Study of Neoplasia and Steroid Contraceptives*. Breast cancer and combined oral contraceptives: results from a multinational study. Br J Cancer 61, 110–119 (1990). https://doi.org/10.1038/bjc.1990.23
Issue Date:
DOI: https://doi.org/10.1038/bjc.1990.23
This article is cited by
-
Reproductive factors and incidence of breast cancer: An international ecological study
Sozial- und Präventivmedizin SPM (2000)
-
Educational Review Hormone Replacement Therapy and Breast Cancer
Annals of Surgical Oncology (1999)
-
Recent oral contraceptive use and risk of breast cancer (United States)
Cancer Causes and Control (1996)
-
Oral contraceptive use and breast cancer risk among African-American women
Cancer Causes and Control (1995)
-
Prognostic value of proliferating cell nuclear antigen and c-erbB-2 compared with conventional histopathological factors in breast cancer
Journal of Cancer Research and Clinical Oncology (1995)