Abstract
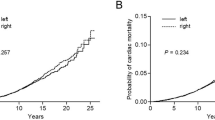
To examine the hypothesis that radiotherapy for breast cancer can cause myocardial infarction, cause-specific mortality by laterality of the primary tumour was analysed among 54,617 breast cancer patients reported to the Swedish Cancer Registry during 1970-1985. The rationale was that radiotherapy for a left-sided breast cancer invariably results in higher doses of radiation to the myocardium than a similar treatment given for a right-sided tumour whereas other possible risk factors for cardiovascular disease probably are unrelated to the laterality of the tumour. The median follow-up was 9 years (range 1-17 years). Patients with left-sided tumours were found to have a higher mortality due to myocardial infarction than patients with right-sided tumours (P less than 0.01) but there was no difference in regard to total intercurrent mortality. Further analyses of individual radiotherapy studies are warranted to quantify the excess risk associated with radiation and to study the significance of the type of radiation, portal arrangements, total dose and fractionation. It seems reasonable to assume that adverse effects of radiation are dose-related and may thus be minimised or prevented by the use of appropriate treatment techniques.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 24 print issues and online access
$259.00 per year
only $10.79 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Rutqvist, L., Johansson, H. Mortality by laterality of the primary tumour among 55,000 breast cancer patients from the Swedish Cancer Registry. Br J Cancer 61, 866–868 (1990). https://doi.org/10.1038/bjc.1990.193
Issue Date:
DOI: https://doi.org/10.1038/bjc.1990.193
This article is cited by
-
Die Herzmortalität nach Strahlentherapie, Chemotherapie und endokriner Therapie des Mammakarzinoms
Strahlentherapie und Onkologie (2020)
-
Risk of coronary events 55 Years after Thymic irradiation in the Hempelmann cohort
Cardio-Oncology (2018)
-
Preliminary toxicity results using partial breast 3D-CRT with once daily hypo-fractionation and deep inspiratory breath hold
Radiation Oncology (2018)
-
Valvular Heart Disease in Cancer Patients: Etiology, Diagnosis, and Management
Current Treatment Options in Cardiovascular Medicine (2017)
-
Breast cancer therapy-associated cardiovascular disease
Nature Reviews Clinical Oncology (2016)