Abstract
A variety of cardiovascular diseases is accompanied by the loss of vascular contractility. This study sought to investigate the effects of curcumin, a natural polyphenolic compound present in turmeric, on mouse vascular contractility and the underlying mechanisms. After mice were administered curcumin (100 mg·kg-1·d-1, ig) for 6 weeks, the contractile responses of the thoracic aorta to KCl and phenylephrine were significantly enhanced compared with the control group. Furthermore, the contractility of vascular smooth muscle (SM) was significantly enhanced after incubation in curcumin (25 μmol/L) for 4 days, which was accompanied by upregulated expression of SM marker contractile proteins SM22α and SM α-actin. In cultured vascular smooth muscle cells (VSMCs), curcumin (10, 25, 50 μmol/L) significantly increased the expression of myocardin, a “master regulator” of SM gene expression. Curcumin treatment also significantly increased the levels of caveolin-1 in VSMCs. We found that as a result of the upregulation of caveolin-1, curcumin blocked the activation of notch1 and thereby abolished Notch1-inhibited myocardin expression. Knockdown of caveolin-1 or activation of Notch1 signaling with Jagged1 (2 μg/mL) diminished these effects of curcumin in VSMCs. These findings suggest that curcumin induces the expression of myocardin in mouse smooth muscle cells via a variety of mechanisms, including caveolin-1-mediated inhibition of notch1 activation and Notch1-mediated repression of myocardin expression. This may represent a novel pathway, through which curcumin protects blood vessels via the beneficial regulation of SM contractility.
Similar content being viewed by others
Introduction
Blood vessels, which are part of the circulatory system, are responsible for the transport of blood and delivery of essential nutrients to downstream tissues. The primary structural, muscular, and functional unit of a blood vessel is the medial wall, which is composed primarily of vascular smooth muscle (SM). Vascular SM provides a critical regulatory role in vessel relaxation and contraction to ensure adequate tissue blood flow and to maintain proper localized arterial blood pressures and perfusion of downstream tissues. Vascular dysfunction is the root cause of a variety of important disease processes, including hypertension, myocardial infarction, and atherosclerosis. The underlying pathophysiology of vascular dysfunction occurs in numerous forms and often involves vascular SM losing its contractile characteristics1,2,3. Recent studies also point to dysfunctional vascular SM as an underlying factor of cardiovascular disease, such as atherosclerosis and vascular aging4,5. Logically, therapeutically targeting vascular SM for further discovery and potential therapeutic utility against cardiovascular disease is highly significant and essential. Vascular smooth muscle cells (VSMCs) are highly specialized cells that constitute basic structural and functional elements of vascular SM. By contracting and relaxing, they regulate lumen caliber and thus arterial and venous tone and vascular resistance, which enables vascular SM to control the distribution of blood flow throughout the body. However, VSMCs are also thought to play a major role in vascular dysfunction in a variety of disease states6,7. Mature VSMCs are normally highly differentiated and characterized by the expression of a range of SM-specific contractile proteins, including SM α-actin, SM22α, and h1-calponin8,9. A number of works have shown that the transcription of these muscle genes and almost all SM genes were regulated by myocardin10. Myocardin is a master regulator of VSMC differentiation that is found only in smooth and cardiac muscle and regulates gene expression by forming a higher order complex with serum response factor (SRF)[11]. Critical roles of myocardin in SM have been revealed in mice with global or conditional knockout of the myocardin gene. Mice with homozygous null mutations for myocardin die during early aortic development, and embryos fail to express SMC markers12. Mice with myocardin conditional mutations in SMCs also died at six months and exhibited deformation of the structure of the great arteries, along with increased dilation of the stomach, small intestine, bladder and ureters13. Forced expression of myocardin increases smooth muscle contractile proteins and contributes to the development of SM contractility14. Thus, myocardin could be a prime target for regulation of vascular contractility.
Curcumin is a natural polyphenolic compound present in turmeric and one of the most extensively studied natural products. Curcumin exerts a wide range of bioactivities implicated in anti-oxidant, anti-inflammatory, anti-carcinogenic and wound-healing effects15,16,17,18,19. It is renowned for its medical properties and as a cure for several types of diseases, including diabetes, cancers and cardiovascular diseases. Mounting evidence suggests that curcumin has vascular protective effects in cardiovascular disease20,21. Our study found that curcumin increased vascular contractility in C57BL/6 mice. However, it remains unknown whether curcumin enhances contractility of blood vessels via upregulation of myocardin and its target genes. To test the hypothesis that curcumin improves vascular SM function via the induction of myocardin, we examined myocardin expression in vascular tissues from mice treated with curcumin and their contractility in vitro. The underlying mechanisms were further investigated using cultured VSMCs.
Materials and methods
Reagents and antibodies
Fetal bovine serum (FBS) and Dulbecco's minimum essential medium (DMEM) were purchased from Gibco (Grand Island, USA). KCl and phenylephrine (PE) were purchased from Sigma Aldrich (Sigma-Aldrich, USA). Jagged1 recombinant human protein was purchased from Thermo Fisher Scientific (Waltham, USA), and Human Caveolin-1 Adenovirus (Ad-Caveolin-1) from Vector BioLabs (Cat. No. 1364). Curcumin (purity >98%) was purchased from Sinopharm Chemical Reagent Co, Ltd (Shanghai, China). For use in cell culture, curcumin was dissolved in dimethyl sulfoxide (DMSO) to give a 50 mmol/L stock solution. The concentration of DMSO in the experimental solutions was less than 0.1%. Antibodies specific for SM α-actin, SM22α, myocardin, caveolin-1 and cleaved Notch1 (NICD) were purchased from Abcam (Cambridge, USA). β-actin and horseradish peroxidase-conjugated secondary antibodies were obtained from Santa Cruz Biotechnology (Santa Cruz, USA).
Animals
C57BL/6 male mice, 6–8 weeks of age, were purchased from Jingda Laboratory Animal Technology Co Ltd (Changsha, China). Male homozygous caveolin-1 knockout (caveolin-1 KO) mice with a C57BL/6 genetic background were purchased from the Jackson Laboratory (Stock No: 007083). All mice were acclimatized with 12 h dark-light cycles under a constant temperature (22±2 °C) and had free access to water and food. All experiments were carried out in accordance with the internationally accepted guide for the care and use of laboratory animals and were approved by the Animal Ethics Committee of Hunan University of Chinese Medicine. One set of mice was fed with curcumin. The curcumin was dissolved in ethanol and administered to the mice via gavages of 100 mg/kg body weight/day for 6 weeks. An equivalent amount of ethanol was used for the control group.
Cells
Human VSMCs were purchased from Cell Bank of Chinese Academy of Sciences in Shanghai. Cells were grown in high glucose DMEM medium with supplements (10% FBS, 100 U/mL penicillin G, 100 μg/mL streptomycin, and 2 mmol/L glutamine). According to the IC50 value of VSMCs determined previously by us, curcumin was applied at an end concentration of 10–50 μmol/L for all assays. For controls, the carrier (DMSO) diluted accordingly to the curcumin working solutions was applied to the cells.
RNA interference studies
RNA interference was based on the pGreenPuro system (Addgene, USA) expressing small-hairpin RNA (shRNA). pGreenpuro-caveolin-1-shRNA and pGreenPuro-vector constructs, encoding shRNA for caveolin-1 or a negative control (vector), were prepared by inserting the target sequence into pGreenPuro. The shRNA oligonucleotide was designed with 19 bases in the sense strand (5'-ACCAGAAGGGACACACAGT-3') and the antisense strand (5'-ACTGTGTGTCCCTTCTGGT-3'), which targeted region nt 424–442 of the caveolin-1 coding sequence, separated by a hairpin loop (TTCAAGAGA). The ligation products were transformed into E coli, clones with the shRNA insert were selected and amplified, the plasmid DNA was isolated, and selected reconstructed plasmids for transfection were purified with a plasmid purification mini kit (ComWin Biotech Co, Ltd, China). For transfection, VSMCs were seeded in 6-well plates at 1 × 106 cells/well and allowed to grow overnight to 80%–90% confluency. They were transfected with a mixture of 2 μg plasmid DNA and 10 μL lipofectamine 2000 (Invitrogen, USA) in 2 mL serum-free medium. At 6 h after transfection, 500 μL FBS/well was added. At 26 h after transfection, the medium was replaced by normal medium containing 10% FBS and antibiotics. VSMCs transfected with caveolin-1 shRNA or the control vector were selected by 1 μg/mL of puromycin.
Western blot analysis
VSMCs were washed with ice-cold PBS three times and lysed with RIPA lysis buffer [50 mmol/L Tris–HCl, pH 7.4, 150 mmol/L sodium chloride, 10 mmol/L NP-40, 5 mmol/L deoxycholic acid, 1 mmol/L sodium dodecyl sulfate (SDS), 1 mmol/L EDTA, and 1 mmol/L phenylmethylsulfonyl fluoride] for 10–15 min on ice. Crude lysates were centrifuged at 13000 × g for 10 min at 4 °C. Protein concentrations in the supernatants were determined by a BCA protein assay kit according to the manufacturer's instructions, and the samples were stored at -80 °C. For vascular tissues, three mice from each group were used for the Western blotting. All vascular tissues were collected and stored in liquid nitrogen for protein extraction. Liquid nitrogen-frozen tissues were cut into pieces, homogenized in lysis buffer, and left on ice for 30 min. After centrifugation, protein concentrations were determined with the BCA assay. The Western blot analysis procedures were performed as described elsewhere. Equal amounts of protein from each lysate were mixed with loading buffer at 95°C for 5 min to denature the protein. Proteins were separated by SDS-PAGE and electro-transferred to polyvinylidene difluoride membranes. Nonspecific antigens were blocked by incubation at room temperature for 2 h with 5% nonfat milk in TBST (20 mmol/L Tris-HCl pH 7.6, 136 mmol/L NaCl, and 0.1% Tween-20). The membranes were probed for 1.5 h or overnight with the following primary antibodies: SM α-actin, SM22α, myocardin, NICD, caveolin-1, and β-actin. After five washes in TBST, the membranes were incubated with horseradish peroxidase-conjugated secondary antibody for 1.5 h at room temperature. The membranes were washed five times in TBST, and the protein was detected by using the ECL reagent (Beyotime, China). Emitted light was quantified using the AlphaImager gel documentation systems (formerly Alpha Innotech), and signal intensities were normalized to β-actin using Quantity One software (Bio-Rad Laboratories).
Adenovirus infection
For in vivo adenovirus infection, mice were injected with 109 PFU of Ad-caveolin-1 via the tail vein once every 7 d. For cell adenovirus infection, VSMCs were grown in 6-well plates at a density of 2 × 105 cells/well. After 24 h, cells were incubated in a low FBS medium (2%) in the presence of the Ad-caveolin-1 virus (100 MOI) for 6 h, then returned to a 10% FBS medium. On the fourth day post infection, the caveolin-1 levels were determined by Western blot.
Vascular tissue myography
The mice were sacrificed by cervical dislocation for vascular tissue collection. Thoracic aortas were excised from the mice and transferred into a dish containing cold PBS. Periaortic fibroadipose tissues were carefully removed under surgical microscopy. The aortas were cut into 2 mm length rings, and endothelium was removed by gently rubbing the intimal surface of the vessels. The aortic rings were mounted horizontally in the 5 mL wire myograph chamber of a Multi Wire Myograph System (Danish Myo Technology, Skejbyparken, Denmark), maintained at 37°C in PSS solution (114 mmol/L NaCl, 4.7 mmol/L KCl, 0.8 mmol/L KH2PO4, 1.2 mmol/L MgCl2, 11 mmol/L D-glucose, 25 mmol/L NaHCO3, and 2.5 mmol/L CaCl2, pH 7.4), and gassed with a 95% O2-5% CO2 mixture at a resting tension of 1 g (9.8 mN). Two tungsten wires (25 μm in diameter) were guided through the lumen of each ring segment. Vascular tissues were allowed to equilibrate for 60 min before the experiments were carried out. Isometric tension was recorded using MyoDaq/MyoData 2.1 software (Danish Myo Technology). One set of the aortic rings was then cultured in DMEM medium with or without addition of curcumin for 4 d, and KCl (50 mmol/L)- and PE (1 μmol/L)-induced contractile responses were measured by the tissue myograph system after culture.
Statistical analysis
Data are presented as either representative recordings or mean±SEM. The number of replicates (n) represents the number of independent assays. Differences were evaluated using Student's t-test or one-way ANOVA. P<0.05 was considered statistically significant.
Results
Curcumin increased vascular contractility
To determine whether curcumin affects vascular contractility, C57BL/6 mice received curcumin (100 mg/kg) daily for 6 weeks by gavage. Thoracic aortas were excised from the mice and cut into rings (approximately 2 mm in length). We examined the contractile responses of the aortic rings to membrane depolarization with KCl (50 mmol/L) and α1-adrenoceptor activation by PE (1 μmol/L). The results showed that administration of curcumin exhibited a significantly increased (P<0.05) vascular contractility (Figure 1).
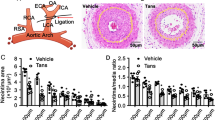
Curcumin increased vascular contractility. Thoracic aortas were excised from mice treated with or without curcumin and cut into rings (about 2 mm in length). The contractile responses of the aortic rings to KCl and PE were examined. (A) KCl (50 mmol/L) and PE (1 μmol/L) responses of control mouse aortic rings. (B) KCl and PE responses of aortic rings from mice received curcumin (100 mg/kg) daily for 6 weeks. (C and D) Cumulative data showing the effects of curcumin on vascular contractile response to KCl and PE. n=6. Mean±SEM. *P<0.05.
The contractility of vascular smooth muscle (SM) was enhanced after exposure to curcumin
We then observed the effects of curcumin on the regulation of vascular SM functions. Thoracic aortas were removed from the mice and dissected, as previously described. The endothelium was removed by gently rubbing the intimal surface of the vessels. Contractile responses of the vascular tissues were examined by the tissue myograph system and then cultured in DMEM medium with or without the addition of curcumin (25 μmol/L) in a 5% CO2 incubator at 37 °C for 4 d. After culture, the contractile responses of the vascular tissues to KCl and PE were examined again by the myograph system. We also detected the expression of contractile protein in vascular tissues after exposure to curcumin. Our results showed that the contractile responses of vascular tissues to KCl and PE were conserved after 4 d incubation with vehicle (Figure 2A). However, after treatment with curcumin for 4 d, the vascular tissues exhibited an enhanced contractile response to KCl and PE (Figure 2B), and the expression of contractile proteins SM α-actin and SM22α were increased (Figure 2E).
The contractility of vascular smooth muscle (SM) was enhanced after exposure to curcumin. Thoracic aortas were excised, cut into rings, removed the endothelium, and then incubated with vehicle or curcumin. (A) KCl (50 mmol/L) and PE (1 μmol/L) responses of vascular tissues before and after 4-d treatment with vehicle (DMSO, 0.1% v/v). (B) KCl and PE responses of vascular tissues before and after 4-d treatment with 25 μmol/L curcumin. (C and D) cumulative data showing the effects of curcumin and vehicle on vascular contractile response to KCl and PE. n=4. Mean±SEM. *P<0.05. Mouse thoracic aortas were excised from mice and removed the endothelium, then cultured in DMEM medium with 25 μmol/L curcumin for 4 d. After culture, the vascular tissues were harvested for measurement of the level of SM α-actin and SM22α. (E) Western blot detection of the expression of contractile proteins SM α-actin and SM22α. Left: representative Western blots. Right: cumulative data showing the relative amounts of SM α-actin and SM22α after curcumin treatment as indicated. n=4. Mean±SEM. *P<0.05.
Contractile protein expression was upregulated by curcumin in VSMCs
To study the underlying mechanisms of curcumin-induced increases in vascular SM contractility, we examined the effect of curcumin on the expression of contractile proteins in cultured human vascular smooth muscle cells (VSMCs). VSMCs were incubated with different concentrations of curcumin (10, 25, 50 μmol/L) for 24 h. Western blotting was used to detect the expression of SM α-actin and SM22α in VSMCs. The results showed that the expression of SM α-actin and SM22α in VSMCs increased significantly in a dose-dependent manner when exposed to curcumin (Figure 3).
Contractile protein expression was upregulated by curcumin in VSMCs. VSMCs were incubated with different concentrations of curcumin for 24 h. Representative western blot and quantitative analysis of SM α-actin and SM22α in VSMCs after treatment. n=3. Mean±SEM. *P<0.05.
Curcumin increased the expression of myocardin
Since most SM contractile genes, including SM α-actin and SM22α, are controlled by myocardin, we incubated VSMCs with varying concentrations of curcumin (10, 25, 50 μmol/L) for 24 h or incubated VSMCs with 25 μmol/L curcumin for different amounts of time (12, 24, 48 h). Western blotting was used to evaluate the expression of myocardin in VSMCs after curcumin treatment. Similar to the effects of curcumin on the expression of contractile proteins in vascular tissues, Western blotting of the VSMCs showed that the expression of myocardin increased significantly in a dose- and time-dependent manner following induction with curcumin (Figure 4).
Curcumin increased the expression of myocardin. VSMCs were incubated with varying concentrations of curcumin for 24 h, or incubated with 25 μmol/L curcumin for different times. (A) Representative Western blot and quantitative analysis of myocardin in VSMCs after incubation with different concentrations of curcumin for 24 h. (B) Representative Western blot and quantitative analysis of myocardin in VSMCs after incubation with 25 μmol/L curcumin for different time. n=3. Mean±SEM. *P<0.05.
Curcumin upregulated expression of myocardin by repressing Notch1 activation
It has been demonstrated that notch signaling represses myocardin-induced VSMC differentiation. Binding of ligand Jagged1 to the Notch1 receptor releases NICD (Notch1 intracellular domain) to the nucleus, which inhibits myocardin-dependent transcription of SM-restricted genes22. To identify whether curcumin-induced myocardin expression depends on the inhibition of Notch1 activity, we pretreated VMSCs with 2 μg/mL of Jagged1 to activate Notch1 signaling, followed by incubation with or without curcumin (25 μmol/L) for 24 h. We found that curcumin decreased the generation of NICD (Figure 5A) and upregulated the expression of myocardin (Figure 5B). However, curcumin-induced expression of myocardin was abrogated by Jagged1, and exogenous Jagged1 significantly inhibited the expression of myocardin (Figure 5B). These results suggest that curcumin enhances the expression of myocardin by repressing Notch1 activation.
Curcumin upregulated expression of myocardin by repressing Notch1 activation. VSMCs were treated with different concentrations of curcumin for 24 h. (A) Representative Western blot and quantitative analysis of NICD in VSMCs after treatment. VMSCs were pretreated with 2 μg/mL of Jagged1 to activate Notch1 signaling, followed by incubation with or without curcumin (25 μmol/L) for 24 h. (B) Representative Western blot and quantitative analysis of NICD and myocardin in VSMCs after incubation. n=3. Mean±SEM. *P<0.05.
Repression of notch1 by curcumin was caveolin-1 dependent
Our previous study demonstrated that curcumin regulated intracellular cholesterol content via induction of caveolin-1 expression23. In this study, we determined if caveolin-1 plays a role in the regulation of vascular contractility. Male homozygous caveolin-1 knockout (caveolin-1 KO) mice with a C57/BL6 genetic background, C57/BL6 mice injected with adenovirus encoding caveolin-1 (Ad-caveolin-1), and age-matched C57/BL6 wild-type (WT) mice were used in this experiment. The contractile responses of aortic rings removed from 6-week-old mice (caveolin-1 KO, Ad-caveolin-1 and WT) were examined using a tissue myograph system. VSMCs stably expressing caveolin-1-shRNA and VSMCs infected with Ad-caveolin-1 were used in this experiment to observe the effects of caveolin-1 on the expression of myocardin and contractile proteins. Our results showed that the contractility of aortic rings from caveolin-1 KO mice declined by approximately 20% compared to those from wild-type mice but increased in Ad-caveolin-1 mice (Figure 6B, C and D). In cultured VSMCs, infection of adenovirus encoding caveolin-1 markedly increased the expression of myocardin, SM α-actin and SM22α (Figure 6G). To determine whether caveolin-1 is involved in curcumin-enhanced SM contractility, the contractile responses of caveolin-1 KO mouse aortic rings to KCl and PE were examined, and the activity of Notch1 in wild-type, caveolin-1 overexpressed and knocked-down (caveolin-1-shRNA) VSMCs was analyzed by Western blot after curcumin (25 μmol/L) treatment. As shown in Fig. 6, curcumin increased the contractile responses of WT mice but had little effect on caveolin-1 KO mice (Figure 6H and I). Western blot revealed that curcumin inhibited the expression of NICD in normal VSMCs and the inhibitory effect of curcumin on notch1 was less or disappeared in caveolin-1-shRNA VSMCs, while in Ad-caveolin-1 VSMCs, overexpression of caveolin-1 enhanced the inhibitory effect on Notch1 (Figure 6L). These results suggest that caveolin-1 plays a role in the regulation of vascular contractility and contributes to curcumin-mediated NICD down-regulation.
Repression of Notch1 by curcumin was caveolin-1 dependent. (A) Representative Western blot and quantitative analysis of caveolin-1 in VSMCs after treatment with different concentrations of curcumin for 24 h. n=3. Mean±SEM. *P<0.05. The contractile responses of aortic rings excised from 6 weeks old mice (caveolin-1 KO, Ad-caveolin-1 and WT) were examined by a tissue myograph system. (B) KCl and PE responses of aortic rings from WT mice. (C) KCl and PE responses of aortic rings from caveolin-1 KO mice. (D) KCl and PE responses of aortic rings from mice injected with Ad-caveolin-1 adenovirus. (E and F) Cumulative data showing the effects of caveolin-1 on aortic rings contractile response to KCl and PE. n=6. Mean±SEM. *P<0.05.
(G) Representative Western blot and quantitative analysis of myocardin, SM α-actin and SM22α in VSMCs (caveolin-1-shRNA, Ad-caveolin-1 and wild-type). (H) KCl and PE responses of aortic rings from caveolin-1 KO mice. (I) KCl and PE responses of aortic rings from caveolin-1 KO mice treated with curcumin (100 mg/kg) daily for 6 weeks. (J and K) Cumulative data showing the effects of curcumin on aortic rings contractile response to KCl and PE in caveolin-1 KO mice. (L) Representative Western blot and quantitative analysis of NICD in wild-type, caveolin-1 overexpressed and knocked-down VSMCs after curcumin (25 μmol/L) treatment. n=3. Mean±SEM. *P<0.05. WT, wild-type; CAV1-shR, caveolin-1-shRNA; Ad-CAV1, Ad-caveolin-1.
Discussion
Turmeric is commonly used as a food additive to enhance the taste and flavor of food. It has medicinal uses because of the discovered therapeutic effects24,25. Curcumin, a natural polyphenolic compound present in turmeric, is considered one of the active ingredients that contributes to the health function of turmeric and has been extensively investigated for its chemopreventive potential26,27. The putative mechanisms of action for curcumin are numerous, among which are its anti-inflammatory, antiproliferative, antiangiogenic, proapoptotic and immune-modulatory properties28,29,30. In addition, mounting evidence suggests that curcumin has vascular protective effects in aging animals and humans. In this study, curcumin was found to be effective in regulating vascular contractility.
Vascular contractility depends on vascular SM function. It is well known that contractility of vascular SM is critical in the regulation of the lumenal diameter of the resistance vessels, thereby contributing significantly to setting the level of blood pressure and blood flow to vascular beds. SM contractility can be regulated by various signaling pathways31,32,33,34. We harvested thoracic aortas from C57BL/6 mice, treated them with curcumin to determine the effects of curcumin on SM contractility, and found that the contractility of vascular SM was enhanced after incubation with curcumin and the expression of contractile proteins in vascular tissues was increased. VSMCs are highly specialized cells that constitute basic structural and functional elements in vascular SM. By contracting and relaxing, they alter the tension of vascular smooth muscle, enabling vascular SM to maintain an appropriate blood pressure. Mature VSMCs are characterized by the expression of a range of SM-specific contractile proteins, such as SM α-actin, SM22α, and h1-calponin. The findings of the present study well demonstrate that the expression of contractile proteins, SM α-actin and SM22α was dramatically increased by curcumin in VSMCs. It has been known that most SM contractile genes, such as SM α-actin and SM22α, are controlled by myocardin. Myocardin was reported to be a key regulator of cardiac and SM differentiation, forming a ternary complex with SRF on a sequence known as a CarG box, and specifically induces the expression of smooth and cardiac muscle-specific genes. In VSMCs, the level of myocardin is abundantly expressed along with key SM-restricted genes and decreases in parallel with the loss or attenuation of SM marker expression. Although the importance of myocardin in SM development is firmly established, the regulatory mechanism of myocardin is not well understood.
Multiple signaling pathways are expected to modulate myocardin, such as Nkx2.5 and notch1[22, 35-37]. In the present study, we found that curcumin induced the expression of contractile proteins, as well as myocardin, in a concentration- and time-dependent manner in VSMCs. So far, there is no direct evidence for the role of curcumin in the regulation of Nkx2.5, notch1 or myocardin. Critically, it was demonstrated that caveolin-1 was involved in the regulation of Notch1 activation38, and our previous study showed that curcumin upregulated the expression of caveolin-1 in VSMCs23. It is possible that caveolin-1 mediates the effect of curcumin on myocardin expression by the regulation of notch signaling. The Notch signaling pathway is a highly conserved cell signaling system present in most multicellular organisms. Mammals possess four different notch receptors, referred to as Notch1–4. The constitutive expression of the Notch family has been reported in a variety of tissues, such as vascular endothelial and smooth muscle cells. Notch1 belongs to a family of transmembrane receptors that regulate fate decisions and differentiation during normal development39. Binding of the ligand Jagged1 to the extracellular domain of notch1 induces proteolytic cleavage and release of the intracellular domain NICD, which translocates to the nucleus and forms complexes with specific DNA-binding proteins and transcriptionally regulates target genes40. It was reported that notch1 signaling repressed myocardin-induced SM-specific contractile proteins expression22. In our experiments, curcumin-induced expression of myocardin was abrogated by Jagged1, and exogenous Jagged1 significantly inhibited the expression of myocardin. These results suggest that curcumin upregulates the expression of myocardin by repressing notch1 activation.
Caveolin-1 is an anchoring protein in the plasma membrane of most animal cells that interacts with several signaling mechanisms and participates in many important physiological processes, including the ability to regulate blood vessel function41,42,43,44. One of the most important functions of caveolin-1 is to promote the formation of caveolae, a special type of lipid raft, on the surface of VSMCs45,46. A number of signaling molecules and enzymes are located in the caveolae/raft including γ-secretase47, which is required for the cleavage and activation of notch1[48]. γ-Secretase activity has been reported to be enriched in caveolae/raft microdomains49, but the proteolytic cleavage of notch1 occurs primarily in non-raft membranes50. It is highly conceivable that caveolin-1 could intensify the spatial segregation of γ-secretase imposed by caveolae/raft membrane domains and inhibit its switching to non-raft membranes where notch1 becomes easily accessible to this protease. To determine whether caveolin-1 mediates the effects of curcumin on notch1 activation, we analyzed the expression of NICD, an activated form of notch1, in caveolin-1-overexpressed and knocked-down VSMCs after treatment with curcumin. Our experiments showed that curcumin inhibited the expression of NICD in normal VSMCs but had no effect in caveolin-1 knocked-down VSMCs, while overexpression of caveolin-1 enhanced the inhibitory effect of curcumin on NICD. We also observed the effect of caveolin-1 on vascular contractility and found that mice with homozygous null mutations for caveolin-1 showed an impaired vascular contractility, and Ad-caveolin-1 mice exhibited an enhanced contractility. These results suggest that caveolin-1 critically contributes to regulate SM contractility by mediating the effect of curcumin on Notch1 activity.
In summary, we identified a previously unknown role for curcumin as a regulator of the vascular contractile response by inducing myocardin, which increases contractile protein expression and vascular contractility. Curcumin upregulated the expression of myocardin via a variety of mechanisms, including caveolin-1–mediated inhibition of Notch1 activation and Notch1-mediated repression of myocardin expression. This study extends our understanding of the role of curcumin in vascular protection and may represent a new approach for the treatment of vascular diseases.
Author contribution
Duan-fang LIAO designed research; Wen-juan TONG, Zi-fen GUO, Qin-hui TUO and Cai-ping ZHANG performed research; Jian-xiong CHEN contributed new analytical tools and reagents; Xiao-yong LEI analyzed data; Shao-wei SUN wrote the paper.
References
Brunner F, Wolkart G, Pfeiffer S, Russell JC, Wascher TC . Vascular dysfunction and myocardial contractility in the JCR:LA-corpulent rat. Cardiovasc Res 2000; 47: 150–8.
Kang S, Woo HH, Kim K, Lim KM, Noh JY, Lee MY, et al. Dysfunction of vascular smooth muscle and vascular remodeling by simvastatin. Toxicol Sci 2014; 138: 446–556.
Wurster S, Wang P, Dean R, Chaudry I . Vascular smooth muscle contractile function is impaired during early and late stages of sepsis. J Surg Res 1994; 56: 556–61.
El Assar M, Angulo J, Vallejo S, Peiro C, Sanchez-Ferrer C, Rodriguez-Manas L . Mechanisms involved in the aging-induced vascular dysfunction. Front Physiol 2012; 3: 132.
Dupasquier CMC, Weber A-M, Ander BP, Rampersad PP, Steigerwald S, Wigle JT, et al. Effects of dietary flaxseed on vascular contractile function and atherosclerosis during prolonged hypercholesterolemia in rabbits. Am J Physiol Heart Circ Physiol 2006; 291: H2987–96.
Bennett MR, Sinha S, Owens GK . Vascular smooth muscle cells in atherosclerosis. Circ Res 2016; 118: 692–702.
Michel J-B, Li Z, Lacolley P . Smooth muscle cells and vascular diseases. Cardiovasc Res 2012; 95: 135–7.
Yoshida T, Owens GK . Molecular determinants of vascular smooth muscle cell diversity. Circ Res 2005; 96: 280–91.
Owens G . Molecular control of vascular smooth muscle cell differentiation. Acta Physiol Scand 1998; 164 : 623–35.
Wang Z, Wang D-Z, Pipes GCT, Olson EN . Myocardin is a master regulator of smooth muscle gene expression. Proc Natl Acad Sci U S A 2003; 100 : 7129–34.
Zhou N, Lee J-J, Stoll S, Ma B, Wiener R, Wang C, et al. Inhibition of SRF/myocardin reduces aortic stiffness by targeting vascular smooth muscle cell stiffening in hypertension. Cardiovasc Res 2016: cvw222.
Li S, Wang D-Z, Wang Z, Richardson JA, Olson EN . The serum response factor coactivator myocardin is required for vascular smooth muscle development. Proc Natl Acad Sci U S A 2003; 100: 9366–70.
Huang J, Wang T, Wright AC, Yang J, Zhou S, Li L, et al. Myocardin is required for maintenance of vascular and visceral smooth muscle homeostasis during postnatal development. Proc Natl Acad Sci U S A 2015; 112: 4447–52.
Yoshida T, Kawai-Kowase K, Owens GK . Forced expression of myocardin is not sufficient for induction of smooth muscle differentiation in multipotential embryonic cells. Arterioscler Thromb Vasc Biol 2004; 24: 1596–601.
Chadalapaka G, Jutooru I, Chintharlapalli S, Papineni S, Smith R III, Li X, et al. Curcumin decreases specificity protein expression in bladder cancer cells. Cancer Res 2008; 68: 5345–54.
Na HS, Cha MH, Oh D-R, Cho C-W, Rhee JH, Kim YR . Protective mechanism of curcumin against Vibrio vulnificus infection. FEMS Immunol Med Microbiol 2011; 63: 355–62.
Scapagnini G, Foresti R, Calabrese V, Stella AMG, Green CJ, Motterlini R . Caffeic acid phenethyl ester and curcumin: a novel class of heme oxygenase-1 inducers. Mol Pharmacol 2002; 61: 554–61.
Shankar S, Srivastava RK . Bax and Bak genes are essential for maximum apoptotic response by curcumin, a polyphenolic compound and cancer chemopreventive agent derived from turmeric, Curcuma longa. Carcinogenesis 2007; 28: 1277–86.
Zhang L, Luo J, Zhang M, Yao W, Ma X, Yu SY . Effects of curcumin on chronic, unpredictable, mild, stress-induced depressive-like behaviour and structural plasticity in the lateral amygdala of rats. Int J Neuropsychopharmacol 2014; 17: 793–806.
Fleenor B, Sindler A, Marvi N, Howell K, Zigler M, Yoshizawa M, et al. Curcumin ameliorates arterial dysfunction and oxidative stress with aging. Exp Gerontol 2013; 48: 269–76.
Zhao J, Ching L, Huang Y, Chen C, Chiang A, Kou Y, et al. Molecular mechanism of curcumin on the suppression of cholesterol accumulation in macrophage foam cells and atherosclerosis. Mol Nutr Food Res 2012; 56: 691–701.
Proweller A, Pear WS, Parmacek MS . Notch signaling represses myocardin-induced smooth muscle cell differentiation. J Biol Chem 2005; 280: 8994–9004.
Yuan HY, Kuang SY, Zheng X, Ling HY, Yang YB, Yan PK, et al. Curcumin inhibits cellular cholesterol accumulation by regulating SREBP-1/caveolin-1 signaling pathway in vascular smooth muscle cells. Acta Pharmacol Sin 2008; 29: 555–63.
Park S, Lim H, Hwang S . Evaluation of antioxidant, rheological, physical and sensorial properties of wheat flour dough and cake containing turmeric powder. Food Sci Technol Int 2012; 18: 435–43.
Rao S, Dinkar C, Vaishnav LK, Rao P, Rai MP, Fayad R, et al. The Indian spice turmeric delays and mitigates radiation-induced oral mucositis in patients undergoing treatment for head and neck cancer: an investigational study. Integr Cancer Ther 2014; 13: 201–10.
Gowda NKS, Ledoux DR, Rottinghaus GE, Bermudez AJ, Chen YC . Efficacy of turmeric (Curcuma longa), containing a known level of curcumin, and a hydrated sodium calcium aluminosilicate to ameliorate the adverse effects of aflatoxin in broiler chicks. Poult Sci 2008; 87: 1125–30.
Keshavarz K . The Influence of turmeric and curcumin on cholesterol concentration of eggs and tissues. Poult Sci 1976; 55: 1077–83.
Bengmark S . Curcumin, an atoxic antioxidant and natural NF{kappa}B, cyclooxygenase-2, lipooxygenase, and inducible nitric oxide synthase inhibitor: a shield against acute and chronic diseases. J Parenter Enteral Nutr 2006; 30: 45–51.
Heger M, van Golen RF, Broekgaarden M, Michel MC . The molecular basis for the pharmacokinetics and pharmacodynamics of curcumin and its metabolites in relation to cancer. Pharmacol Rev 2013; 66: 222–307.
Lopresti AL, Hood SD, Drummond PD . Multiple antidepressant potential modes of action of curcumin: a review of its anti-inflammatory, monoaminergic, antioxidant, immune-modulating and neuroprotective effects. J Psychopharmacol 2012; 26: 1512–24.
Ye GJ, Nesmith AP, Parker KK . The role of mechanotransduction on vascular smooth muscle myocytes' [corrected] cytoskeleton and contractile function. Anat Rec (Hoboken) 2014; 297: 1758–69.
Schauwienold D, Plum C, Helbing T, Voigt P, Bobbert T, Hoffmann D, et al. ERK1/2-Dependent Contractile Protein Expression in Vascular Smooth Muscle Cells. Hypertension 2003; 41: 546–52.
Dietrich A, Mederos y Schnitzler M, Gollasch M, Gross V, Storch U, Dubrovska G, et al. Increased vascular smooth muscle contractility in TRPC6-/- mice. Mol Cell Biol 2005; 25: 6980–9.
Stull JT, Gallagher PJ, Herring BP, Kamm KE . Vascular smooth muscle contractile elements. Cellular regulation. Hypertension 1991; 17: 723–32.
Creemers EE, Sutherland LB, McAnally J, Richardson JA, Olson EN . Myocardin is a direct transcriptional target of Mef2, Tead and Foxo proteins during cardiovascular development. Development 2006; 133: 4245–56.
Ueyama T, Kasahara H, Ishiwata T, Nie Q, Izumo S . Myocardin expression is regulated by Nkx2.5, and its function is required for cardiomyogenesis. Mol Cell Biol 2003; 23: 9222–32.
Xie WB, Li Z, Miano JM, Long X, Chen SY . Smad3-mediated myocardin silencing: a novel mechanism governing the initiation of smooth muscle differentiation. J Biol Chem 2011; 286: 15050–7.
Kapoor A, Hsu W, Wang B, Wu G, Lin T, Lee S, et al. Caveolin-1 regulates γ-secretase-mediated AβPP processing by modulating spatial distribution of γ-secretase in membrane. J Alzheimers Dis 2010; 22: 423–42.
Fiuza UM, Arias AM . Cell and molecular biology of Notch. J Endocrinol 2007; 194: 459–74.
Bray SJ . Notch signalling in context. Nat Rev Mol Cell Biol 2016; 17: 722–35.
Parat MO, Riggins GJ . Caveolin-1, caveolae, and glioblastoma. Neuro Oncol 2012; 14: 679–88.
Frank P, Lisanti M . Role of caveolin-1 in the regulation of the vascular shear stress response. J Clin Invest 2006; 116: 1222–5.
Jia G, Sowers JR . Caveolin-1 in cardiovascular disease: a double-edged sword. Diabetes 2015; 64: 3645–7.
Hardin CD, Vallejo J . Caveolins in vascular smooth muscle: Form organizing function. Cardiovasc Res 2006; 69: 808–15.
Cohen AW, Hnasko R, Schubert W, Lisanti MP . Role of caveolae and caveolins in health and disease. Physiol Rev 2004; 84: 1341–79.
Gratton JP, Bernatchez P, Sessa WC . Caveolae and caveolins in the cardiovascular system. Circ Res 2004; 94: 1408–17.
Matsumura N, Takami M, Okochi M, Wada-Kakuda S, Fujiwara H, Tagami S, et al. γ-Secretase associated with lipid rafts: multiple interactive pathways in the stepwise processing of β-carboxyl-terminal fragment. J Biol Chem 2014; 289: 5109–21.
Olsauskas-Kuprys R, Zlobin A, Osipo C . Gamma secretase inhibitors of Notch signaling. Onco Targets Ther 2013; 6: 943–55.
Urano Y, Hayashi I, Isoo N, Reid PC, Shibasaki Y, Noguchi N, et al. Association of active γ-secretase complex with lipid rafts. J Lipid Res 2005; 46: 904–12.
Vetrivel KS, Cheng H, Kim SH, Chen Y, Barnes NY, Parent AT, et al. Spatial segregation of γ-secretase and substrates in distinct membrane domains. J Biol Chem 2005; 280: 25892–900.
Acknowledgements
This work was supported by grants from the National Natural Science Foundation of China (No 31371161, 81670268, 30971170 and 30971267) and Natural Science Foundation of Hu-nan Province (No 2016JJ3109).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Sun, Sw., Tong, Wj., Guo, Zf. et al. Curcumin enhances vascular contractility via induction of myocardin in mouse smooth muscle cells. Acta Pharmacol Sin 38, 1329–1339 (2017). https://doi.org/10.1038/aps.2017.18
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/aps.2017.18
Keywords
This article is cited by
-
Photoacoustic Spectroscopy in the Characterization of Bread with Turmeric Addition
Food and Bioprocess Technology (2020)