Abstract
Aim:
To investigate the effects of nitric oxide (NO) donors on the function and expression of P-glycoprotein (P-gp) in Caco-2 cells.
Methods:
Caco-2 cells were exposed to NO donors for designated times. P-gp function and expression were assessed using Rhodamine123 uptake assay and Western blotting, respectively. Intracellular reactive oxygen species (iROS) and intracellular reactive nitrogen species (iRNS) levels were measured using ROS and RNS assay kits, respectively.
Results:
Exposure of Caco-2 cells to 0.1 or 2 mmol/L of sodium nitroprusside (SNP) affected the function and expression of P-gp in concentration- and time-dependent manners. A short-term (4 h) exposure reduced P-gp function and expression accompanied with significantly increased levels of iROS and iRNS. In contrast, a long-term (24 h) exposure stimulated the P-gp function and expression. The stimulatory effects of 2 mmol/L SNP was less profound as compared to those caused by 0.1 mmol/L SNP. The other NO donors SIN-1 and SNAP showed similar effects. Neither the NO scavenger PTIO (2 mmol/L) nor soluble guanylate cyclase inhibitor ODQ (50 μmol/L) reversed the SNP-induced alteration of P-gp function. On the other hand, free radical scavengers ascorbate, glutathione and uric acid (2 mmol/L for each), PKC inhibitor chelerythrine (5 μmol/L), PI3K/Akt inhibitor wortmannin (1 μmol/L) and p38 MAPK inhibitor SB203580 (10 μmol/L) reversed the upregulation of P-gp function by the long-term exposure to SNP, but these agents had no effect on the impaired P-gp function following the short-term exposure to SNP.
Conclusion:
NO donors time-dependently regulate P-gp function and expression in Caco-2 cells: short-term exposure impairs P-gp function and expression, whereas long-term exposure stimulates P-gp function and expression. The regulation occurs via a NO-independent mechanism.
Similar content being viewed by others
Introduction
P-glycoprotein (P-gp), an ATP-binding cassette (ABC) drug efflux transporter, is widely expressed in various tissues including brain, lungs, liver, kidney, gastrointestinal tract, skin and muscle tissue1. P-gp has a wide range of substrates, including anticancer agents, calcium channel blockers, antibiotics, cardiac glycosides and immunosuppressants2. Clinical reports have underlined the effect of changes in the functional activity of P-gp on the bioavailability and disposition of therapeutic agents3.
Previous reports have indicated that the expression and function of P-gp are dysregulated under pathophysiological situations such as diabetes mellitus4, 5, chronic renal failure6 and inflammation7. It is becoming increasingly clear that nitric oxide and its related nitrogen species (NOx)8 are crucial regulatory mediators of the function and expression of P-gp and other transporters under pathophysiological conditions8,9,10,11,12,13,14. NO-mediated nitrosative stress was reported to stimulate the function and expression of P-gp in the blood-brain barrier of streptozotocin-treated diabetic rats8. Activation of inductible nitric oxide synthase (iNOS) seemed to explain the increase in the expression and function of intestinal P-gp in interferon-γ-induced human intestinal cells, as evidenced by the fact that coadministration of the iNOS inhibitor L-N6-(1-iminoethyl)-lysin abrogated the cytokine-mediated increase in P-gp expression and function9. LPS-induced upregulation of Abca1 and Abcb1/P-gp in the kidney occurred via alteration of NO production by iNOS; this induction may be attenuated by co-administration of the iNOS inhibitor aminoguanidine14. However, contradictory results were also reported. In HT29/HT29-dx cell cultures, nitric oxide production reversed resistance to the P-gp substrate doxorubicin, suggesting that NO decreased the activity of P-gp10. NG-monomethyl-L-arginine, a NO synthase inhibitor, markedly blocked cyclosporin A-induced impairment of P-gp function in cocultures of MBEC and rat astrocytes11. NO was also reported to be involved in the decreased expression of intestinal P-gp in the early stages of intestinal ischemia and reperfusion12. Recently, Nawa et al reported that iNOS were involved in downregulation of intestinal P-gp expression in streptozotocin-treated diabetic mice13. Further studies, however, showed that iNOS regulated the activity of intestinal P-gp in a bidirectional way, inhibiting their effect at earlier stages of diabetes and intensifying their effect at later stages15.
The aim of this study was to further investigate the effects of NO on intestinal P-gp activity using the Caco-2 cell model; the Caco-2 cell monolayers have tight junctions, microvilli and various types of enzymes and transporters, thereby resembling the intestinal epithelium. In addition, Caco-2 cells express high levels of P-gp and have been widely used for the study of P-gp function and intestinal absorption16. Three different types of NO donors, SNP, SIN-1, and SNAP8, 17 were used as source of NO. The function of P-gp was assessed using uptake of Rhodamine123 (Rho123) by Caco-2 cells. P-gp protein levels were measured using western blotting. Our preliminary study showed that the effects of NO on the function of P-gp in Caco-2 cells were dependent on both the exposure time and the concentration of NO donors.
Materials and methods
Materials
Rhodamine123 (Rho123), chelerythrine, wortmannin, SB203580, SNAP (S-nitroso-N-acetylpenicillamine), 3-morpholinosydnonimine (SIN-1), 2-phenyl-4,4,5,5-tetramethyl-imidazoline-l-oxyl-3-oxide (PTIO), reduced glutathione (GSH) and 1H-[1,2,4]oxadiazolol[4,3-a]quinoxalin-1-one (ODQ) were purchased from Sigma Chemical Co (St Louis, MO, USA). Sodium nitroprusside (SNP), uric acid and ascorbate were purchased from Sinopharm Chemical Reagent Co Ltd (Shanghai, China); reactive oxygen species (ROS) and reactive nitrogen species (RNS) assay kits were purchased from Beyotime Institute of Biotechnology (Nantong, China); anti-P-gp monoclonal antibody C219 was purchased from Calbiochem-Novabiochem (Seattle, WA, USA); Blueranger prestained protein molecular weight marker mix was purchased from Pierce (Rockford, IL, USA); and goat anti-mouse secondary antibodies conjugated with the appropriate horseradish peroxidase and polyclonal anti-β-actin antibodies were purchased from Boshide Biotech Co (Wuhan, China). All other reagents were commercially available and were of analytical grade.
Cell culture
Caco-2 cells were obtained from American Type Culture Collection (Manassas, VA, USA). The cells were maintained at 37 °C in a controlled atmosphere of 5% CO2 and 90% relative humidity, using DMEM (high glucose) supplemented with 2.5 mmol/L L-glutamine, 100 U/L penicillin, 100 U/L streptomycin, 3.7 g/L NaHCO3, 1% nonessential amino acids, and 10% fetal bovine serum (Gibco BRL Co Ltd, USA). The medium was changed every other day. When 80% confluent, the cultured Caco-2 cells were passaged and seeded in 24-well plastic plates (Costar, Cambridge, MA, USA). Cells were used when a significant fraction of the cell population exhibited a colonic phenotype. Cells were co-incubated with the tested agents at designated time periods, and the Rho123 uptake experiment was performed to assess the function of P-gp. The 3-(4,5-dimethyl-2-thiazolyl)-2,5-diphenyl-2H-tetrazolium bromide (MTT) assay showed that none of the tested agents in the study damaged the viability of the cells.
Caco-2 cells treated with NO donors
Krischel et al's experiments using various doses of NO donors (from 0.01 to 5 mmol/L)18 showed that the effect of low doses (lower than 0.1 mmol/L) was not obvious, whereas high doses (higher than 2 mmol/L) impaired cell viability. Therefore, 0.1 and 2 mmol/L were chosen as representative concentrations for the time-dependent research. Generally, the NO donor SNP was freshly prepared before use. The cultured Caco-2 cells were washed three times with serum-free medium. Then, the cells were incubated in the presence of 0.1 and 2 mmol/L SNP for 2, 4, 6, 8, 24, and 48 h. P-gp function was assessed by measuring the uptake of Rho123 by the cells.
Another experiment was also designed to further assess the changes of P-gp function in Caco-2 cells following 4-h and 24-h incubation times in the presence of several doses of SNP, SNAP and SIN-1. The concentration-dependent effects of SNP on P-gp function were further documented following a 24-h incubation.
Caco-2 cells co-treated with SNP and pharmacological inhibitors
The free radical scavengers ascorbate (antioxidant8, 2 mmol/L), PTIO (NO scavenger17, 2 mmol/L), GSH (active against nitrosative stress17, 2 mmol/L) and uric acid (peroxynitrite scavenger19, 2 mmol/L) as well as several signal pathway inhibitors: chelerythrine (a PKC inhibitor, 5 μmol/L), wortmannin (a PI3K/Akt inhibitor, 1 μmol/L), SB203580 (a p38 MAPK inhibitor, 10 μmol/L) and ODQ (a specific guanylate cyclase inhibitor, 50 μmol/L)20, 21 were used to investigate whether these inhibitors reverse the alteration in P-gp function induced by SNP. Caco-2 cells were pretreated with a pharmacological inhibitor for 1 h, then either SNP or normal medium was added and incubated for 4 and 24 h, respectively22. The P-gp function in the cells was measured and compared among relevant groups.
Measurement of Rho123 uptake by Caco-2 cells
The P-gp function in cells was measured using the Rho123 uptake experiment. Uptake experiments were performed according to the method previously reported23. In brief, treated cells were washed and preincubated in pH 7.4 Hanks' balanced salt solution (HBSS) at 37 °C for 30 min, then 1 mL HBSS containing 100 ng/mL Rho123 was added to initiate the uptake of Rho123. After incubation for 2 h, the uptake was stopped by rinsing the cells three times with ice-cold HBSS, and 0.5 mL of purified water was added to each incubated well. Cells were lysed by three freeze-thaw cycles, and the protein concentrations were measured using the Bradford method (1976)24. The sensitivity of Rho123 uptake as an indicator of P-gp activity was verified using the P-gp inhibitor cyclosporin A (0.625–2.5 μg/mL), which significantly increased the intracellular accumulation of Rho123.
The concentrations of Rho123 in cells were determined by HPLC25. The lowest limit of quantitation of Rho123 in cells was 0.002 ng/μg protein. The yields were higher than 85%. The relative standard derivations of intra day and inter day data were lower than 10%. The linear range of Rho123 in cells was 0.002–0.064 ng/μg protein.
Determination of the intracellular levels of ROS and RNS
The levels of intracellular ROS (iROS) and intracellular RNS (iRNS) were measured according to the manufacturer's instructions of the ROS and RNS assay kits. Briefly, Caco-2 cells were incubated with SNP for different times, then cells were rinsed three times with PBS buffer (including 1% BSA and 10 mmol/L HEPES) and treated with 2′,7′-dichlorofluorescin-diacetate (DCFH-DA, 10 μmol/L) and 4-amino-5-methylamino-2′,7′-difluorofluorescein (DAF-FM DA, 10 μmol/L) for 30 min, the intracellular DCFH was oxidized to DCF by ROS while the intracellular DAF-FM was nitrosated to DAF by RNS. Cells were washed 5 times with cold PBS. DCF was used as an indicator of ROS; it was detected with a fluorescence detector at an excitation wavelength of 488 nm and an emission wavelength of 525 nm. DAF was used as an indicator of RNS and was detected at an excitation wavelength of 495 nm and emission wavelength of 515 nm.
Western blotting analysis
Protein expression of P-gp in Caco-2 cells was assessed using western blotting according to a previously described method25, 26. Briefly, following 4-h and 24-h exposures to SNP (0.1 and 2 mmol/L), the Caco-2 cells were lysed in ice-cold lysis buffer containing 10 mmol/L Tris-HCl (pH 7.5), 1 mmol/L EGTA, 1 mmol/L MgCl2, 1 mmol/L mercaptoethanol, 1% glycerol, and a protease inhibitor cocktail containing 1 mmol/L dithiothreitol, and 2 mmol/L phenylmethylsulfonylfluoride (Sigma Chemical Co, Ltd, St Louis, MO, USA) for 30 min. The cells were then ultrasonicated five times for 10 s in an ice bath. Samples were then centrifuged at 500×g for 10 min at 4 °C. The supernatant was transferred to a new tube and centrifuged at 15 000×gfor 60 min at 4 °C. The supernatant (cytosolic proteins such as β-actin) and the pellet (membrane proteins such as P-gp) were both collected and stored at -80 °C until use. Protein concentrations were measured by the Bradford method. Samples were reconstituted in SDS-polyacrylamide gel electrophoresis sample loading buffer and were boiled for 5 min to denature the protein. The protein samples were separated on an 8% SDS-polyacrylamide gel and were transferred onto a polyvinylidene difluoride membrane (Millipore Corporation). After blotting, the membrane was blocked with 10% bovine serum albumin in Tris-buffered saline-Tween 20 (TBS-T) for 1 h at 37 °C. Immunoblots were incubated with the primary monoclonal antibody to P-gp (1:200; C219) or β-actin (1:800; Bioworld Technology, St Louis Park, MN, USA) for 24 h at 4 °C. The membrane was washed (10 min×4), incubated with the secondary antibody, horseradish peroxidase-conjugated goat anti-mouse IgG (1:800; Boster Biological Technology, Wuhan, China) for 1 h at 37 °C and then washed three times with TBS-T. The signals were detected using an enhanced chemiluminescence kit (Pierce Chemical). The P-gp protein band intensity was normalized to that of β-actin.
Statistical analysis
Results were expressed as the mean±standard deviation (SD). The overall differences between groups were determined by one-way of analysis of variance (ANOVA). If analysis indicated significance, the differences between groups were estimated using the Student-Newman-Keuls multiple comparison post-hoc test. P values of less than 0.05 indicated a significant difference.
Results
Alteration in P-gp function and expression induced by NO donors
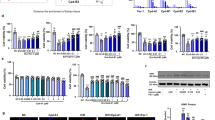
Caco-2 cells were incubated with two concentrations (0.1 and 2 mmol/L) of SNP for designated time periods (2, 4, 6, 8, 24, and 48 h), and Rho123 uptake by the cells was measured (Figure 1). The results demonstrated that the effect of SNP on Rho123 uptake was dependent on the SNP concentration and the incubation time. Short-term exposure to SNP increased cellular Rho123 uptake in a concentration-dependent manner. Maximum induction (115% and 140% of Rho123 uptake in control cells) occurred after 4-h of incubation. In contrast, long-term (24- and 48-h) exposure to SNP resulted in a decrease in cellular Rho123 uptake. The decrease of Rho123 by low concentrations (0.1 mmol/L) of SNP was more profound than that by high concentrations (2 mmol/L). To investigate whether alteration in cellular Rho123 uptake was the result of expression of P-gp, the levels of P-gp were measured using western blotting (Figure 2). As expected, 4-h of exposure to SNP decreased P-gp expression in a concentration-dependent manner, whereas 24-h of exposure to SNP induced P-gp expression in a biphasic manner.
Effects of SNP on P-gp function following different incubation time periods. Caco-2 cells were incubated with low (0.1 mmol/L) and high (2 mmol/L) concentrations of SNP for 2, 4, 6, 8, 24, and 48 h. P-gp function was measured using cellular Rho123 uptake. Cells incubated with drug-free medium served as a control. Mean±SD (n=4). bP<0.05, cP<0.01 vs control.
Effects of a 4-h exposure (A) and a 24-h exposure (B) to SNP on P-gp protein levels in Caco-2 cells. Caco-2 cells were incubated with 0.1 or 2 mmol/L SNP for 4 and 24 h, respectively, and the levels of P-gp in the cells were measured using Western blotting. Cells incubated with drug-free medium served as a control. Mean±SD (n=3–4). bP<0.05, cP<0.01 vs control.
To verify that the phenomenon induced by SNP came from NOx rather than other species derived from SNP, the effects of different types of NO donors on P-gp function were investigated following 4-h and 24-h incubations. The three donors have different structures, which release NO at different rates and by different mechanisms. SIN-1, a NO donor that releases both NO and O2−, is usually used as peroxynitrite donor27. SNAP is an S-nitrosothiol NO donor with a half-life of approximately 4 h28. Similar to the findings with SNP, 4-h of exposure to SIN-1 or SNAP decreased the efflux activity of P-gp in a concentration-dependent manner (Figure 3A), and 24-h of exposure to SIN-1 or SNAP exerted biphasic regulation effects (Figure 3B). Effects of a series of SNP concentrations on the efflux activity of P-gp were also measured following 24-h of incubation (Figure 3C). The results showed that the effect of SNP on basal P-gp activity was normally distributed. The maximal stimulation occurred at 0.1 mmol/L SNP; at higher SNP concentrations, the stimulatory effect gradually decreased (Figure 3C). Concentrations over 2 mmol/L were not tested because of cell toxicity.
Effects of a 4-h exposure (A), a 24-h exposure (B) to SNP, SIN-1 and SNAP or a 24-h exposure (C) to different levels of SNP on P-gp function in Caco-2 cells. Caco-2 cells were incubated with the tested agents for designated times. P-gp function was assessed by measuring cellular Rho123 uptake. Cells incubated with drug-free medium served as a control. Mean±SD (n=4). bP<0.05, cP<0.01 vs control. eP<0.05, fP<0.01 vs 0.1 mmol/L SNP.
Temporal profile of intracellular ROS and RNS level after exposure to SNP
iROS and iRNS levels were measured following exposure to 0.1 and 2 mmol/L of SNP for different times (Figure 4). The results showed that ROS was produced concomitantly with the nitric oxide released by SNP in Caco-2 cells. Short-term exposure to SNP significantly increased iROS and iRNS, and iROS and iRNS were sustained at relatively high levels for the first 6 h. Following 24 h of exposure to SNP, the iROS and iRNS levels were still higher than in the control cells.
Effects of SNP on intracellular ROS (A) and RNS (B) following different incubation times. Caco-2 cells were exposed to 0.1 or 2 mmol/L SNP for 0.5, 1, 4, 6, or 24 h, and iROS and iRNS levels were assessed according to the instructions of the respective assay kits. Cells incubated with drug-free medium served as a control. Mean±SD (n=4). bP<0.05, cP<0.01 vs control.
Effect of free radical scavengers on P-gp function induced by SNP
Effects of several free radical scavengers on P-gp function induced by SNP were investigated. The results showed that 2 mmol/L ascorbate, GSH and uric acid significantly reversed alteration in P-gp function by 24 h of exposure to SNP, whereas the nitric oxide scavenger PTIO had no effect (Figure 5B), indicating that the alteration in P-gp function did not result from a direct effect of NO itself but from the indirect effects of NO-derived oxidative and nitrosative stress. However, neither VC, GSH, UA nor PTIO could attenuate the impairment of P-gp function after only 4 h of exposure to SNP (Figure 5A), treatment with GSH even showed a trend toward enhancing the impaired P-gp function. Higher doses of these free radical scavengers caused cell toxicity. None of the above radical scavengers alone had a significant influence on P-gp function (Figure 5C).
Effects of free radical scavengers on short-term inhibition and long-term stimulation of P-gp function induced by exposure to SNP in Caco-2 cells. Caco-2 cells were co-incubated with SNP (0.1 and 2 mmol/L) in the presence of ascorbate (VC, 2 mmol/L), GSH (2 mmol/L), uric acid (UA, 2 mmol/L), or PTIO (2 mmol/L) for 4 h (A) and 24 h (B). (C) represents the 4-h and 24-h effects of the free radical scavengers alone on P-gp function. Cells incubated with drug-free medium served as a control. P-gp function was measured using cellular Rho123 uptake. Cells incubated with drug-free medium served as a control. Mean±SD (n=4). bP<0.05, cP<0.01 vs control; eP<0.05, fP<0.01 vs 0.1 mmol/L SNP. hP<0.05, iP<0.01 vs 2 mmol/L SNP.
Effects of signal pathway inhibitors on the alteration of P-gp function by SNP
The cGMP/PKG pathway is a typical pathway that is downstream of the NO modulation system. The soluble guanylate cyclase inhibitor ODQ was used to determine the association between the cGMP/PKG pathway and the alteration in P-gp function by SNP. ODQ did not reverse the alteration in P-gp function by 4-h or 24-h of exposure to 2 mmol/L SNP (Figure 6). This result indicated that the changes in P-gp activity by SNP are independent of the cGMP/PKG pathway, which is consistent with a previous report10. However, the compounds wortmannin (a PI3K/Akt inhibitor), chelerythrine (a PKC inhibitor) and SB203580 (a p38 MAPK inhibitor) significantly reversed the alteration in P-gp function induced by 24-h of exposure to SNP (Figure 6B), implying that the alteration in the function of P-gp by a 24-h exposure to SNP involved the PI3K/Akt, PKC, and MAPK pathways. In contrast, none of the three pharmacological inhibitors could reverse the inhibitory effect of a 4-h exposure to SNP on P-gp function (Figure 6A); in fact, the PI3K/Akt inhibitor wortmannin further decreased P-gp activity. None of the above pharmacological inhibitors alone had a significant influence on P-gp function (Figure 6C).
Effects of several pharmacological inhibitors on short-term inhibition and long-term stimulation of P-gp function induced by exposure to SNP in Caco-2 cells. Caco-2 cells were co-incubated with SNP in the presence of wortmannin (Wort, 1 μmol/L), chelerythrine (Chelery, 5 μmol/L), SB203580 (SB, 10 μmol/L) or ODQ (50 μmol/L) for 4 h (A) and 24 h (B). (C) represents the 4-h and 24-h effects of inhibitors alone on P-gp function. Cells incubated with drug-free medium served as a control. P-gp function was measured using cellular Rho123 uptake. Mean±SD (n=4). bP<0.05, cP<0.01 vs control. eP<0.05, fP<0.01 vs 0.1 mmol/L SNP. hP<0.05, iP<0.01 vs 2 mmol/L SNP.
Discussion
Accumulating evidence clearly demonstrates a link between NOx (NO and its redox-reactive derivatives) and the activity of P-gp, although the published results are often contradictory8, 10, 12, 13, 14. The present study was designed to investigate the effects of NO and its redox-reactive derivatives (NOx) on the expression and function of P-gp in Caco-2 cells using three different NOx donors. P-gp function was quantitatively assessed by measuring the cellular uptake of the P-gp substrate Rho123. Alteration of the intracellular accumulation of this compound directly correlated with the altered activity of this efflux system, which is expressed in the apical membrane of Caco-2 cells. The main finding was that the effects of the NO donor SNP on the function and expression of P-gp were dependent on incubation time. Short-term exposure to SNP impaired expression and function of P-gp in a concentration-dependent manner, whereas long-term exposure to SNP biphasically enhanced the expression and function of P-gp.
The intracellular accumulation of Rho123 in Caco-2 cells was measured following incubation with two concentrations of SNP (0.1 and 2 mmol/L). The results showed that cellular uptake of Rho123 increased with incubation time at early timepoints (2 and 4 h), peaked at 4 h, then declined gradually (Figure 1) with increased incubation time. It was also observed that long-term exposure to SNP caused biphasic regulation of P-gp function. The stimulatory effect of 0.1 mmol/L SNP was more profound than that of 2 mmol/L SNP. Western blot data showed that the altered function of P-gp in Caco-2 cells was in agreement with the alteration in P-gp protein levels, indicating that the altered function of P-gp partly came from altered P-gp protein levels.
To exclude a direct role of SNP in P-gp function and expression levels, two other donors, SIN-1 and SNAP, which possess different structures and NO release rates, were also used to investigate the roles of NO donors. A similar pattern of alteration in P-gp function was observed, suggesting that the alteration in P-gp activity resulted from NO and its reactive derivates. Biphasic regulation of P-gp function by SNP in Caco-2 cells was further verified using a 24-h exposure to different concentrations of SNP (Figure 3C).
NO is a short-lived reactive molecule: when it is released, it rapidly reacts with its specific biological target or reacts with oxygen or superoxide to generate ROS and RNS, which subsequently react with biological targets28. The sGC/cGMP pathway is considered a typical downstream pathway of NO; NO activates sGC (soluble guanylate cyclase) to produce cGMP (cyclic GMP), which regulates a series of physiological responses29, 30, 31. Our results showed that the sGC inhibitor ODQ did not reverse the alteration of P-gp function induced by NO donors, suggesting that the regulation of P-gp function by NO donors is independent of the sGC/cGMP pathway. This finding was supported by previous studies that used doxorubicin accumulation in HT29/HT29-dx cells10. In addition, the specific NO scavenger PTIO did not reverse the SNP-induced alteration of P-gp function, indicating that the effect of SNP on P-gp function occurred via an NO-independent mechanism29. This result agreed with previous studies performed in isolated perfused rat livers32. Furthermore, a significant increase in intracellular ROS (iROS) and RNS (iRNS) in Caco-2 cells was observed at early stages of SNP exposure, which indicated that iROS and iRNS were involved in the SNP-induced impairment of P-gp function. Although, the decrease in folate transporter function induced by 10 μmol/L SNAP was reversible with sufficient (10 mmol/L) ascorbate, GSH, or NO scavengers33, however these results showed that VC, GSH, UA and PTIO did not alleviate the impairment of P-gp function following a 4-h exposure to 0.1 and 2 mmol/L SNP (Figure 5A); this lack of effect was most likely due to insufficient dosing of the reversal agents (2 mmol/L) at 0.1 and 2 mmol/L NO donors. Higher doses of the reversal agents were not used because simultaneous exposure to SNP and higher doses of reversal agents led to significant cell damage. However, these scavengers significantly reversed the SNP-induced stimulation of P-gp after a 24-h exposure to SNP, suggesting that the increase in both the activity and expression of P-gp by long-term exposure to NO donors resulted from the comprehensive effects of oxidative stress and nitrosative stress. This conclusion was consistent with previous reports8 in MBEC cells.
NOx activates diverse signaling pathways to regulate gene expression20. The MAPK signaling pathway, the PKC signal pathway and the PI3K/Akt pathways have been reported to be activated by NOx20, 21, 22, 23, 33, 34. Whether or not NOx altered intestinal efflux activity by regulating these signal pathways was also studied using the corresponding pharmacological inhibitors wortmannin (a PI3K inhibitor), SB203580 (a p38 MAPK inhibitor), and chelerythrine (a PKC inhibitor). The results observed with these inhibitors were similar to the effects of free radical scavengers: although the three inhibitors did not alleviate the impairment of P-gp function induced by a 4-h exposure to 2 mmol/L SNP, they reversed the P-gp stimulation induced by long-term exposure to 0.1 mmol/L SNP. These results suggest that a 24-h exposure to NOx donors stimulated the expression and activity of P-gp via the PI3K/Akt, PKC and p38 MAPK pathways.
The pattern of changes in P-gp activity and protein expression in response to NO donors is certainly complex, as short-term exposure to NO donor decreased P-gp function and expression, whereas long-term exposure to NO donors elevated P-gp function and expression. Similar patterns have been found for MRP2 in renal proximal tubules exposed to certain tubular nephrotoxicants35 and in P-gp in rat brain capillaries exposed to TNF (tumor necrosis factor)-α and ET (endothelin-1)36. These findings seem to partly explain the contradictory reports on the regulation of P-gp by NOx when different doses or incubation times were used8, 10, 37.
The present results indicate that the effects of NO donors on P-gp function and expression were dependent on exposure time. Short-term exposure to NO donors led to a significant decrease in P-gp function and expression, whereas long-term exposure to NO donors stimulated P-gp function and expression. The regulation of P-gp function and expression by NO donors occurred via a NO-independent mechanism.
Author contribution
Ru DUAN and Xiao-dong LIU designed the experiments and analyzed the data; Ru DUAN wrote the paper; Xiao-dong LIU and Li LIU revised the paper; Ru DUAN, Nan HU, Hai-yan LIU, Jia LI, Li LIU, Hai-fang GUO, and Can LIU performed the research.
References
Brady JM, Cherrington NJ, Hartley DP, Buist SC, Li N, Klaassen CD . Tissue distribution and chemical induction of multiple drug resistance genes in rats. Drug Metab Dispos 2002; 30: 838–44.
Marchetti S, Mazzanti R, Beijnen JH, Schellens JH . Concise review: Clinical relevance of drug drug and herb drug interactions mediated by the ABC transporter ABCB1 (MDR1, P-glycoprotein). Oncologist 2007; 12: 927–41.
Fromm MF . Importance of P-glycoprotein for drug disposition in humans. Eur J Clin Invest 2003; 33: 6–9.
Liu H, Zhang D, Xu X, Liu X, Wang G, Xie L, et al. Attenuated function and expression of P-glycoprotein at blood-brain barrier and increased brain distribution of phenobarbital in streptozotocin-induced diabetic mice. Eur J Pharmacol 2007; 561: 226–32.
Zhang LL, Lu L, Jin S, Jing XY, Yao D, Hu N, et al. Tissue-specific alterations in expression and function of P-glycoprotein in streptozotocin-induced diabetic rats. Acta Pharmacol Sin 2011; 32: 956–66.
Laouari D, Yang R, Veau C, Blanke I, Friedlander G . Two apical multidrug transporters, P-gp and MRP2, are differently altered in chronic renal failure. Am J Physiol Renal Physiol 2001; 280: 636–45.
Blokzijl H, Vander Borght S, Bok LI, Libbrecht L, Geuken M, van den Heuvel FA, et al. Decreased P-glycoprotein (P-gp/MDR1) expression in inflamed human intestinal epithelium is independent of PXR protein levels. Inflamm Bowel Dis 2007; 13: 710–20.
Maeng HJ, Kim MH, Jin HE, Shin SM, Tsuruo T, Kim SG, et al. Functional induction of P-glycoprotein in the blood-brain barrier of streptozotocin-induced diabetic rats: evidence for the involvement of nuclear factor-kappaB, a nitrosative stress-sensitive transcription factor, in the regulation. Drug Metab Dispos 2007; 35: 1996–2005.
Dixit SG, Zingarelli B, Buckley DJ, Buckley AR, Pauletti GM . Nitric oxide mediates increased P-glycoprotein activity in interferon-{gamma}-stimulated human intestinal cells. Am J Physiol Gastrointest Liver Physiol 2005; 288: G533–40.
Riganti C, Miraglia E, Viarisio D, Costamagna C, Pescarmona G, Ghigo D, et al. Nitric oxide reverts the resistance to doxorubicin in human colon cancer cells by inhibiting the drug efflux. Cancer Res 2005; 65: 516–25.
Dohgu S, Yamauchi A, Nakagawa S, Takata F, Kai M, Egawa T, et al. Nitric oxide mediates cyclosporine-induced impairment of the blood-brain barrier in cocultures of mouse brain endothelial cells and rat astrocytes. Eur J Pharmacol 2004; 505: 51–9.
Takizawa Y, Kishimoto H, Kitazato T, Tomita M, Hayashi M . Effects of nitric oxide on mucosal barrier dysfunction during early phase of intestinal ischemia/reperfusion. Eur J Pharm Sci 2011; 42: 246–52.
Nawa A, Fujita Hamabe W, Tokuyama S . Inducible nitric oxide synthase-mediated decrease of intestinal P-glycoprotein expression under streptozotocin-induced diabetic conditions. Life Sci 2010; 86: 402–9.
Heemskerk S, van Koppen A, van den Broek L, Poelen GJ, Wouterse AC, Dijkman HB, et al. Nitric oxide differentially regulates renal ATP-binding cassette transporters during endotoxemia. Pflugers Arch 2007; 454: 321–34.
Nawa A, Fujita-Hamabe W, Tokuyama S . Regulatory action of nitric oxide synthase on ileal P-glycoprotein expression under streptozotocin-induced diabetic condition. Biol Pharm Bull 2011; 34: 436–8.
Meunier V, Bourrié M, Berger Y, Fabre G . The human intestinal epithelial cell line Caco-2; pharmacological and pharmacokinetic applications. Cell Biol Toxicol 1995; 11: 187–94.
Uchiyama T, Matsuda Y, Wada M, Takahashi S, Fujita T . Functional regulation of Na+-dependent neutral amino acid transporter ASCT2 by S-nitrosothiols and nitric oxide in Caco-2 cells. FEBS Lett 2005; 579: 2499–506.
Krischel V, Bruch-Gerharz D, Suschek C, Kröncke KD, Ruzicka T, Kolb-Bachofen V . Biphasic effect of exogenous nitric oxide on proliferation and differentiation in skin derived keratinocytes but not fibroblasts. J Invest Dermatol 1998; 111: 286–91.
Kean RB, Spitsin SV, Mikheeva T, Scott GS, Hooper DC . The peroxynitrite scavenger uric acid prevents inflammatory cell invasion into the central nervous system in experimental allergic encephalomyelitis through maintenance of blood-central nervous system barrier integrity. J Immunol 2000; 165: 6511–8.
Hemish J, Nakaya N, Mittal V, Enikolopov G . Nitric oxide activates diverse signaling pathways to regulate gene expression. J Biol Chem 2003; 278: 42321–9.
Barancík M, Bohácová V, Kvackajová J, Hudecová S, Krizanová O, Breier A . SB203580, a specific inhibitor of p38-MAPK pathway, is a new reversal agent of P-glycoprotein-mediated multidrug resistance. Eur J Pharm Sci 2001; 14: 29–36.
Saksena S, Goyal S, Raheja G, Singh V, Akhtar M, Nazir TM, et al. Upregulation of P-glycoprotein by probiotics in intestinal epithelial cells and in the dextran sulfate sodium model of colitis in mice. Am J Physiol Gastrointest Liver Physiol 2011; 300: 1115–23.
Liu H, Liu X, Jia L, Liu Y, Yang H, Wang G, et al. Insulin therapy restores impaired function and expression of P-glycoprotein in blood-brain barrier of experimental diabetes. Biochem Pharmacol 2008; 75: 1649–58.
Bradford MM . A rapid and sensitive method for the quantitation of microgram quantities of protein utilizing the principle of protein-dye binding. Anal Biochem 1976; 72: 248–54.
Liu H, Xu X, Yang Z, Deng Y, Liu X, Xie L . Impaired function and expression of P-glycoprotein in blood-brain barrier of streptozotocin-induced diabetic rats. Brain Res 2006; 1123: 245–52.
Zhang J, Zhou F, Wu X, Gu Y, Ai H, Zheng Y, et al. 20(S)-ginsenoside Rh2 noncompetitively inhibits P-glycoprotein in vitro and in vivo: a case for herb-drug interactions. Drug Metab Dispos 2010; 38: 2179–87.
Feelisch M . The use of nitric oxide donors in pharmacological studies. Naunyn Schmiedebergs Arch Pharmacol 1998; 358: 113–22.
Thomas DD, Ridnour LA, Isenberg JS, Flores-Santana W, Switzer CH, Donzelli S, et al. The chemical biology of nitric oxide: implications in cellular signaling. Free Radic Biol Med 2008; 45: 18–31.
Feelisch M . Nitric oxide and cyclic GMP in cell signaling and drug development. N Engl J Med 2006; 355: 2003–11.
Pfeifer A, Ruth P, Dostmann W, Sausbier M, Klatt P, Hofmann F . Structure and function of cGMP-dependent protein kinases. Rev Physiol Biochem Pharmacol 1999; 135: 105–49.
Espey MG, Miranda KM, Thomas DD, Wink DA . Distinction between nitrosating mechanisms within human cells and aqueous solution. J Biol Chem 2001; 276: 30085–91.
Parasrampuria R, Mehvar R . Divergent effects of nitric oxide donors on the biliary efflux transporters in isolated perfused rat livers: nitric oxide-independent inhibition of ABC transporters by sodium nitroprusside. Drug Metab Lett 2011; 5: 64–72.
Smith SB, Huang W, Chancy C, Ganapathy V . Regulation of the reduced-folate transporter by nitric oxide in cultured human retinal pigment epithelial cells. Biochem Biophys Res Commun 1999; 257: 279–83.
Katayama K, Yoshioka S, Tsukahara S, Mitsuhashi J, Sugimoto Y . Inhibition of the mitogen-activated protein kinase pathway results in the down-regulation of P-glycoprotein. Mol Cancer Ther 2007; 6: 2092–102.
Terlouw SA, Graeff C, Smeets PH, Fricker G, Russel FG, Masereeuw R, et al. Short- and long-term influences of heavy metals on anionic drug efflux from renal proximal tubule. J Pharmacol Exp Ther 2002; 301: 578–85.
Bauer B, Hartz AM, Miller DS . Tumor necrosis factor alpha and endothelin-1 increase P-glycoprotein expression and transport activity at the blood-brain barrier. Mol Pharmacol 2007; 71: 667–75.
Robertson SJ, Mokgokong R, Kania KD, Guedj AS, Hladky SB, Barrand MA . Nitric oxide contributes to hypoxia-reoxygenation-induced P-glycoprotein expression in rat brain endothelial cells. Cell Mol Neurobiol 2011; 31: 1103–11.
Acknowledgements
This work was supported by the National Natural Science Foundation of China (No 81072693 and 81102503), and supported by funding for Innovative Research Team in Institution of Jiangsu Higher Education.
Author information
Authors and Affiliations
Corresponding authors
Rights and permissions
About this article
Cite this article
Duan, R., Hu, N., Liu, Hy. et al. Biphasic regulation of P-glycoprotein function and expression by NO donors in Caco-2 cells. Acta Pharmacol Sin 33, 767–774 (2012). https://doi.org/10.1038/aps.2012.25
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/aps.2012.25
Keywords
This article is cited by
-
Effect of Nitric Oxide on the Functioning of the P-Glycoprotein Transporter
Bulletin of Experimental Biology and Medicine (2022)
-
The down-regulation of SLC7A11 enhances ROS induced P-gp over-expression and drug resistance in MCF-7 breast cancer cells
Scientific Reports (2017)