Abstract
Aim:
The aim of this study was to investigate the effect of topotecan (TPT) on cancer cell migration.
Methods:
Growth inhibition of TPT was analyzed by MTT assay, and cancer cell migration was measured by transwell double chamber assay. To verify the effect of TPT on the chemokine receptors CXCR4 and CCR7, quantitative PCR, semi-quantitative PCR and Western blot analysis were performed. The secretion of MMP-2 and MMP-9 was detected by enzyme-linked immunosorbent assay (ELISA) and gelatin zymography. To evaluate possible contributions of CCR7 to MMP secretion, the overexpression vectors pcDNA3.1+-CCR7 and CCR7 siRNA were transiently transfected into MDA-MB-435 cells.
Results:
TPT inhibited cancer cell migration in a dose-dependent manner. Additionally, TPT significantly decreased the expression of CCR7 in both MDA-MB-435 and MDA-MB-231 cells and moderately reduced the expression of CXCR4 in MDA-MB-435 cells. The secretion of MMPs (MMP-2, MMP-9) was also inhibited by TPT. Overexpression of CCR7 increased the secretion of MMP-2/9 and cancer cell migration, whereas knockdown of CCR7 reduced active MMP-2/9 production and migration of MDA-MB-435 cells.
Conclusion:
TPT inhibited cancer cell migration by down-regulation of CCR7 and MMPs (MMP-2 and MMP-9).
Similar content being viewed by others
Introduction
Metastasis is a multistep process responsible for most cancer deaths1, 2, 3. Although malignant cancers can spread to a wide variety of body tissues, only a few tissues, such as lymph nodes, bone, liver and lung, offer favorable conditions for metastasized cancer cell survival4. It has recently been suggested that the chemokine and chemokine receptor family1 play a significant role in this organ tropism.
Chemokines are a superfamily of chemotactic cytokines of 8- to 14-kDa molecular weight5, initially described as regulators of leukocyte trafficking to sites of inflammation. During regulation, chemokines bind to their cognate receptors, most of which belong to the G-protein-coupled receptor family, and are expressed in endothelial cells and lymphocytes. Recent studies have revealed that cancer cells can respond to chemokine stimuli through expression of their respective receptors6, altering cancer cell invasive and metastastic properties. Elevated levels of CXCR4 and CCR7 in breast carcinoma are significantly associated with increased malignancy, advanced disease and poor prognosis7, 8, 9, 10, 11. In breast cancer, CXCR4 expression increases progressively with increasing malignant potential10, and CCR7 is associated with lymph node metastasis11. In melanoma, the recruitment of CCR7-positive cancer cells by CCL21 also leads to lymph nodes metastasis12. It appears that the normal physiology of CXCR4 and CCR7 has been usurped to promote the specific metastasis of neoplastic cells to distant organs, thereby making them prime targets for therapeutic intervention in the clinic.
Proteolytic enzymes play a fundamental role in cancer progression, providing access for tumor cells to the vascular and lymphatic systems, which support tumor growth and constitute an escape route for further dissemination. Among all of the proteolytic enzymes potentially associated with tumor invasion, MMP-2 and MMP-9 play fundamental roles in that they are responsible for degradation of extracellular matrix components such as collagen and proteoglycans in disease processes such as invasion by carcinoma13, 14. Recent studies also suggest a relationship between MMPs and CXCR4 in cancer cells. CXCL12, a ligand of CXCR4, promotes the activity of the matrix metalloproteinase MMP-9 and MMP-2 in the prostate cancer cell lines PC3 and LNCap15. CXCL12 also enhances the invasiveness of lung cancer cells by increasing MMP-9 expression through the CXCR4/ERK/NF-kappaB signal transduction pathways16. All of these data therefore suggest a possible role of the chemokine and chemokine receptor family in MMP-mediated cancer metastasis.
Topotecan (TPT) is a semi-synthetic analogue of camptothecin. Similar to camptothecin, TPT suppresses DNA replication in cancer cells by inhibiting the nuclear enzyme topoisomerase I (topo I)17. TPT has been licensed to be a second line anti-cancer agent for patients who have developed small cell lung cancer (SCLC)18 and ovarian cancer19. In addition to its cytotoxic activity against solid tumors, TPT has shown potential activity against brain metastases from breast cancer20 and SCLC21in numerous clinical reports. However, the molecular mechanism for the anti-metastatic effect of TPT is unknown. Here, we explored a possible mechanism for the effect of TPT on cancer cell migration. We found that TPT decreased the expression of chemokine receptors (CXCR4 and CCR7) and MMP secretion (MMP-2 and MMP-9). We further showed that CCR7 played a key role in TPT-induced down-regulation of MMP secretion and cancer cell migration.
Materials and methods
Cell culture and reagents
MDA-MB-231 cells and MDA-MB-435 cells were obtained from the Shanghai Institute of Life Science, Chinese Academy of Sciences. MDA-MB-231 cells were cultured in RPMI-1640 medium (Sigma, St Louis, MO) supplemented with 10% fetal calf serum (Gibco, Grand Island, NY), 100 U/mL penicillin and 100 mg/mL streptomycin. MDA-MB-435 cells were maintained in DMEM medium (Sigma) with 10% FCS. Monoclonal anti-CXCR4 and anti-CCR7 antibodies were purchased from Santa Cruz (Santa Cruz, CA). The monoclonal anti-β-actin antibody and horseradish peroxidase-linked anti-mouse IgG were obtained from Sigma. Validated CCR7 siRNA (ID s3217) and negative control siRNA (ID AM4611) were purchased from Ambion (Austin, TX). TPT was kindly provided by HenRui Co Ltd (Lianyungang, China).
Cell proliferation assay
To evaluate the effect of TPT on cancer cell proliferation, cell growth was studied using the MTT assay as described previously22.
Cell migration assay
Cell migration assays were performed using 12 mm diameter transwell double chambers with a 12 μm pore size (Costar, Cambridge, MA). The surface of the membrane was coated with 30 μg of Matrigel (Sigma) for 2 h at room temperature. Cancer cells were removed from the culture dishes using 0.25% EDTA in PBS and washed twice with physiologic PBS. Cells were resuspended in warmed fresh medium, and 3×104 cells/well were seeded into the upper chamber. Different concentrations of TPT were loaded both in the upper and in the lower chambers, and 2% FCS was placed in the lower chamber as the chemoattractant. After incubation at 37 °C and 5% CO2 for 24 h, nonmigratory cells on the upper membrane were removed with a cotton swab; cells that migrated on the lower surface of the membrane were fixed in 100% ethanol and stained with 1% crystal violet (Sigma) in 0.1 mol/L borate and 2% ethanol. The number of stained cells in five randomly selected fields was counted using bright-field microscopy at 40×magnification.
Quantitative PCR
Cells (1×106) were seeded onto a 9-cm dish. The relative gene expression was analyzed by quantitative PCR as described previously22. Quantification of the amplified product was performed on a cycle-by-cycle basis via the acquisition of a fluorescent signal generated by binding of the fluorophore Sybr Green I (Roche Diagnostics) to double stranded DNA. The primers used for PCR were as follows: CXCR4 forward 5′-ATCTTCCTGCCCACCATCTACTCCATCATC-3′; reverse 5′- ATCCAGACGCCAACATAGACCACCTTTTCA-3′; CCR7 forward 5′-GTGC CCGCGTCCTTCTCATCAG- 3′; reverse 5′-GGCCAGGACCACCCCATTGTAG -3′; and β-actin as internal control: forward 5′-GAGCGGGAAATCGTGCGTGACATT-3′; reverse 5′-GAAGGTAGTTTCGTGGATGCC-3′. Changes in target gene mRNA were calculated using the ΔΔCT method as follows: target gene mRNA (folder increase)=2−ΔΔCT, ΔCT(sample)=CT (target gene)-CT (β-actin), ΔCT(calibrator)=CT (target gene)-CT (β-actin), ΔΔCT=ΔCT(sample)−ΔCT(calibrator).
Gel electrophoresis and immunoblotting
Immunoblotting analysis was performed as described previously19. Briefly, adherent cells were washed twice with PBS and then lysed in RIPA buffer. Cell lysates were incubated at 4 °C for 15 min, and cellular debris was pelleted by centrifugation at 15 000×g for 15 min at 4 °C. Total protein was quantified with a BCA Protein Assay Reagent Kit (Pierce, Rockford, IL), using bovine serum albumin (Pierce) as a standard. Equal amounts (40 μg) of protein were loaded in each lane of a 12% SDS-PAGE gel, followed by transfer to a PVDF membrane (Bio-Rad, Hercules, CA) on a semidry transfer apparatus (Bio-Rad). After being blocked with 5% nonfat milk for 1 h at room temperature, the membrane was incubated with antibodies specific for CXCR4 (Santa Cruz) and CCR7 (Santa Cruz) with proper dilutions for 1 h. After washing, horseradish peroxidase-linked anti-mouse IgG (Sigma) was used as a secondary antibody and then incubated with the membrane for 45 min at room temperature. The signal was detected using ECL Western blotting detection reagents (Amersham Biosciences).
Plasmids construction and transient transfection
Full-length cDNA for CCR7 was amplified and cloned into T easy vector. Cloned fragments were recovered and ligated into pcDNA3.1+(Invitrogen, Carlsbad, CA). Transfections were done using Lipofectamine 2000 transfection reagents (Invitrogen) according to manufacturer instructions. Briefly, MDA-MB-435 cells were seeded in 6-multiwell plates and were transfected at 70%−80% of confluence with 2.5 μg of pcDNA3.1+-CCR7. After 6 h, reagents were removed and cells were allowed to recover for 18 h. Cells transfected with empty vectors (pcDNA3.1+) were used as a control. PCR primers for CCR7 were as follows: forward, 5′-TTTGGATCCCGCCCAGAGAGCGTCATG-3′; reverse: 5′-GGGAAGCTTGTCGCCTATGGGGAGAAG-3′.
RNA interference
Validated siRNA molecules targeted against human CCR7 (NM_001838) and a negative control siRNA were purchased from Ambion. Cells were plated the day before the transfection procedure was started. siRNA was transfected at a final concentration of 1, 10, and 50 nmol/L, respectively, according to the manufacture's protocol. Twenty-four hours after transfection, reagents were removed and cells were harvested. CCR7 knockdown was confirmed by quantitative PCR and Western blotting.
ELISA
Cells were incubated with serum-deprived medium for 24 h and the supernatants were harvested. Each supernatant was centrifuged at 2000×g and stored at −70 °C. Enzyme-linked immunosorbent assays were performed with human MMP-2 and MMP-9 kits (R&D Systems) according to the manufacturer's instructions.
Gelatin zymography
Cells were incubated with serum-free medium for 24 h, and then conditioned medium was collected and stored at −70 °C until analysis. MMP activity was assessed using 10% zymogram gels (Bio-Rad, Richmond, CA). Gels were renatured in buffer containing 2.5% Triton X-100 for 30 min at room temperature. After being washed in developing buffer (100 mmol/L Tris, 5 mmol/L CaCl2 and 0.04% NaN3) for 30 min, gels were incubated with developing buffer overnight at 37°C. Gels were stained with Coomassie brilliant blue R-250, and enzymatic activity was characterized by the presence of clear zones in a background of blue staining.
Statistical analysis
Statistical analysis of the data was performed using the unpaired Student's t test, Mann-Whitney U test and Spearman correlation coefficient analysis. P values were two-sided and a value of 0.05 was considered statistically significant.
Results
TPT inhibits the proliferation and migration of cancer cells
TPT has been reported to induce cell death in human breast cancer cells17. To evaluate the effect of TPT on the viability of MDA-MB-231 and MDA-MB-435 cells, cell proliferation was investigated using the MTT assay performed with logarithmically growing cells. As shown in Figure 1A, TPT significantly inhibited the growth of MDA-MB-435 cells and MDA-MB-231 cells. The proliferation of MDA-MB-435 cells challenged with 0.1 μmol/L TPT for 24 h was reduced to 71.9% compared with non-treated cells, whereas the ratio was 78.3% in MDA-MB-231 cells challenged with 1 μmol/L TPT.
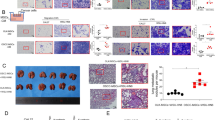
Effect of TPT on cancer cell migration. The data shown are representatives of three independent experiments. (A) Evaluation of cell viability of MDA-MB-435 cells and MDA-MB-231 cells treated with different concentrations of TPT for 24 h. Cell survival was determined by MTT assay. (B) TPT decreased cancer cell migration in MDA-MB-435 cells and MDA-MB-231 cells. Cells were cultured with different doses of TPT for 24 h, and representative pictures of cancer cell migration are shown. Microscopic images of cells that migrated into the lower chamber. (C) Cell migration was quantified by counting migrated cells in five randomly selected fields 24 h after seeding. Control cells remained untreated. Data are presented as means±SD. bP<0.05, cP<0.01 vs control.
We next explored the effect of TPT on cancer cell migration. To address this issue, we performed invasion studies using the classic transwell in vitro assay. Cells in serum-free medium were seeded in the upper chamber and different concentrations of TPT were loaded in both the upper and the lower chambers. As such, 2% FCS was used as the chemoattractant in the lower chamber. As shown in Figure 1B and 1C, TPT significantly inhibited cancer cell migration in both MDA-MB-231 and MDA-MB-435 cells.
TPT reduces the expression of chemokine receptors
CXC chemokine receptor 4 (CXCR4) and CC chemokine receptor 7 (CCR7) are membrane proteins that are highly expressed in malignant cancer cells. Cells expressing CXCR4 and CCR7 usually metastasize to organs and tissues and secrete respective chemokines, such as SDF-1 and CCL2110, 11. Subsequently, we examined the effect of TPT on CXCR4 and CCR7 expression. We found that TPT significantly decreased CCR7 gene expression and modestly reduced CXCR4 gene expression in MDA-MB-435 cells (Figure 2A and 2B). MDA-MB-231 cells treated with TPT showed down-regulation of CCR7 expression; however, CXCR4 expression was unaffected. Similar to the results of gene expression, a significant down-regulation of CCR7 protein was observed in both cell lines, but CXCR4 protein levels were decreased only in MDA-MB-435 cells (Figure 2C). These data probably ruled out a critical role of CXCR4 in TPT-induced inhibition on cancer cell migration and indicated that CCR7 might be associated with the inhibitory effect of TPT.
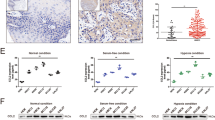
Effect of TPT on the expression of chemokine receptors in MDA-MB-435 and MDA-MB-231 cells. Cells were incubated with different concentrations of TPT for 24 h or cultured with 0.01 μmol/L TPT (MDA-MB-435) or 0.1 μmol/L TPT (MDA-MB-231) for different times. The Effect of TPT on the expression of chemokine receptors was analyzed by quantitative PCR, semi-quantitative PCR and Western blotting. Experiments were performed in triplicate and representative data are presented. (A) Gene expression of CXCR4 and CCR7 in MDA-MB-435 and MDA-MB-231 cells challenged with TPT. Total cellular RNA was extracted and subjected to RT-PCR using specific primers. (B) Relative gene expression of CXCR4 and CCR7 in MDA-MB-231 and MDA-MB-435 cells. Total RNA was tested for CXCR4 and CCR7 mRNA levels by qPCR. (C) CXCR4 and CCR7 proteins were detected by Western blotting. Protein samples were collected and separated by 12% SDS–PAGE and immunoblotted with the anti-CXCR4 and anti-CCR7 antibodies. bP<0.05, cP<0.01 vs control group.
Effect of TPT on MMP secretion
Tumor cells are known to secrete MMPs, which are thought to degrade the extracellular matrix (ECM) and facilitate tumor cell invasion in tissues. Here, we examined the effect of TPT on the secretion of MMP-2 and MMP-9 in MDA-MB-435 and MDA-MB-231 cells. Cells were incubated with different concentrations of TPT for 24 h, after which supernatants were collected for analysis by enzyme-linked immunosorbent assay (ELISA) and gelatin zymography. As shown in Figure 3A, treatment with increasing concentrations of TPT resulted in a decrease in active MMP-9 (86 kDa band) and MMP-2 secretion (72 kDa band) in MDA-MB-435 cells. A significant reduction of active MMP-2 secretion was also observed when MDA-MB-231 cells were treated with 1 μmol/L TPT for 24 h (Figure 3B). However, in contrast to MDA-MB-435 cells, no significant changes of active MMP-9 secretion were detected in MDA-MB-231 cells, as measured by gelatin zymography (Figure 3B). Only a slight decrease in optical density values (about 15%) was found when active MMP-9 secretion was analyzed by ELISA, reflecting a weak effect of 1 μmol/L TPT. Our data showed a more potent inhibition by TPT on active MMP-2 secretion. As such, these experiments indicated that TPT inhibited MMPs secretion (especially MMP-2) and therefore impaired ECM degradation.
Effect of TPT on the secretion of MMPs in MDA-MB-435 (A) and MDA-MB-231 cells (B). Cells were treated with increasing concentrations of TPT for 24 h, after which supernatants were collected and active MMP-2/9 secretion was analyzed by ELISA and gelatin zymography. Results are representatives of three independent experiments. Asterisks indicate significant difference (bP<0.05, cP<0.01). Upper panel, ELISA; lower panel, gelatin zymography.
Effect of CCR7 on MMPs and cancer cell migration
Recent studies have demonstrated that the CXCR4/SDF-1 axis induces MMP activity in cancer cells and then promotes cancer cell migration and metastatic potential15, 16. However, studies on the relationship between CCR7 and MMPs are limited. To investigate the possible contributions of CCR7 to MMP secretion, we transfected MDA-MB-435 cells with the CCR7 gene. As shown in Figure 4A and 4B, gelatin zymography and ELISAs for MMP-2 and MMP-9 showed strong up-regulation of active MMP-2 and MMP-9 secretion in transfected MDA-MB-435 cells (435/CCR7), but not in cells transfected with empty vector (435/EV). To further explore the role of CCR7 in MMP production, MDA-MB-435 cells were transfected with siRNA specifically designed against CCR7 (siCCR7). Both 10 and 50 nmol/L of the double-strand oligonucleotides significantly inhibited (>80%) CCR7 expression (Figure S1). Silencing of CCR7 with 50 nmol/L siRNA significantly reduced MMP-2 and MMP-9 secretion, as measured by ELISA (Figure 4A) and gelatin zymography (Figure 4B). Overexpression of CCR7 also increased MDA-MB-435 cell migration, and knockdown of CCR7 attenuated cell migration (Figure 4C and 4D). These data demonstrated a critical role of CCR7 in regulating cancer cell migration as well as MMP-2/9 secretion, and indicated that the inhibitory effect of TPT was likely caused, at least in part, by changes in CCR7.
Role of CCR7 in mediating MMP secretion and cancer cell migration. The secretion of MMP-2 and MMP-9 was increased after plasmid pcDNA3.1+-CCR7 was transiently transfected into MDA-MB-435 cells (435/CCR7); 50 nmol/L CCR7 siRNA (siCCR7) reduced the production of both MMPs. Cells transfected with empty vector pcDNA3.1+ (435/EV) and untreated cells were used as controls. MMP production was measured by ELISA (A) and gelatin zymography (B). Overexpression of CCR7 promoted cell migration, whereas knockdown of CCR7 decreased cell migration in MDA-MB-435 cells. (C) Representative photos of cancer cell migration are shown. (D) Cell migration was quantified by counting migrated cells in five randomly selected fields 24 h after seeding. Data are presented as means±SD. bP<0.05, cP<0.01 vs control.
Knockdown of CCR7 by RNA interference. (A) Expression of CCR7 mRNA in MDA-MB-435 cells transfected with different concentrations of CCR7 siRNA. Relative gene expression was measured by quantitative PCR; (B) CCR7 protein was detected by Western blotting in MDA-MB-435 cells transfected with different concentrations of CCR7 siRNA. Data shown were representatives of three independent experiments. bP<0.05, cP<0.01 vs control.
Discussion
TPT has been established as a second line anti-cancer agent for solid tumors (eg, SCLC). Previous clinical reports have highlighted the potential activity of TPT against tumor metastasis20, 21. In this study, we showed that TPT decreased cancer cell migration via down-regulation of CCR7 and MMPs (MMP-2 and MMP-9).
The chemokine and chemokine receptor family have important roles in cancer metastasis23, 24, 25. One of the predominant chemokines that associates with the migration, adhesion, and invasion of cancer cells is SDF-1/CXCR4. CXCR4 is one of the few genes that are up-regulated in bone-metastasized breast cancer cells. Cells that metastasize to lung also highly express CXCR4. CCR7, which mediates the survival and migration of immune cells to lymph nodes, has recently been associated with nodal metastasis of squamous cell carcinomas of the head and neck (SCCHN)26. These findings suggest that inhibition of CXCR4 and CCR7 may be a strategy for the prevention of cancer metastasis. We examined the effect of TPT on CXCR4 and CCR7 expression. We found that TPT strongly inhibited CCR7 expression and modestly decreased CXCR4 expression in MDA-MB-435 cells, whereas only CCR7 expression was reduced in MDA-MB-231 cells. We next showed that TPT significantly reduced active MMP secretion. Compared with MMP-2, MMP-9 was less efficiently inhibited. Finally, we demonstrated that overexpression of CCR7 elevated MMP-2/9 secretion and cancer cell migration, whereas knockdown of CCR7 substantially reduced active MMP-2/9 production and migration of MDA-MB-435 cells. These results suggested that CCR7 played a crucial role in TPT-induced inhibition in cancer cell migration.
Cancer cells may express various functional chemokine receptors, and different chemokine receptors play different roles in cancer metastasis. Although TPT decreased the expression of CXCR4 and CCR7 in MDA-MB-435 cells, the inhibition of CXCR4 was less efficient. In MDA-MB-231 cells, TPT reduced CCR7 expression, whereas the expression of CXCR4 was unaffected. These results probably reflected significant differences between CXCR4 and CCR7. Clinical studies27 indicate that both CXCR4 and CCR7 are predictors of cancer metastasis, patient outcome and overall survival, but multivariate analysis demonstrates that CXCR4 and CCR7 are independent factors, and there are no associations between the two. Furthermore, MDA-MB-435 cells express low levels of CXCR4 and do not invade through Matrigel in the presence of SDF-128. MDA-MB-231 but not MDA-MB-435 cell migration is stimulated by SDF-1alpha29. These observations probably indicate that CXCR4/SDF-1 do not substantially contribute to MDA-MB-435 cell migration. Our study also confirmed that CCR7, but not CXCR4, played a critical role in the effect of TPT on cancer cell migration. However, because our experiments showed that 0.1 μmol/L TPT resulted in a moderate decrease in CXCR4 expression in MDA-MB-435 cells, we could not completely rule out the involvement of CXCR4 in TPT-induced inhibition on MDA-MB-435 cells.
Using MDA-MB-435 cells as a model, our results also demonstrated that CCR7 mediated active MMP-2/9 secretion. CXCR4 induces MMP activity. Singh et al showed that the CXCR4/SDF-1 axis induced high levels of MMPs in prostate cancer cells, including MMP-2, MMP-3, MMP-9, MMP-11, and MMP-1430. Chinni et al demonstrated that SDF-1 elevated MMP-9 expression and then facilitated prostate cancer cell bone metastasis. The PI3/AKT pathway contributed significantly to the process with which SDF-1 increased MMP-9 expression31. However, compared with CXCR4, less is known about the role of CCR7 in regulating the secretion of MMPs. The first research on the relationship between CCR7 and MMPs was performed by Redondo and colleagues32. Redondo showed that MMP-9 was regulated by CCL21, the ligand of CCR7, and MMP-9 was involved in B-cell chronic lymphocytic leukemia nodal infiltration. In this study, we showed that overexpression of CCR7 promoted the secretion of MMP-2/9 as well as migration of MDA-MB-435 cells and that silencing of CCR7 resulted in decreased MMP-2/9 secretion and attenuated cancer cell migration. These results suggested a possible role of CCR7 in mediating MMP-2/9 secretion. Interestingly, TPT induced down-regulation of CCR7 expression, but did not dramatically alter the secretion of MMP-9 in MDA-MB-231 cells. Only a less significant reduction (about 15%) of active MMP-9 secretion was observed by ELISA, probably caused by the incomplete inhibition of CCR7 expression. As such, 1 μmol/L TPT resulted in an approximate 50% decrease in the expression of CCR7 in MDA-MB-231 cells, whereas 0.1 μmol/L TPT achieved a 90% decrease in MDA-MB-435 cells. The apparent inability of TPT to eliminate CCR7 expression in MDA-MB-231 cells could reflect an inability to significantly decrease active MMP-9 secretion.
Physiologically, CCR7 is expressed in immune cells, eg, naive T cells, memory T cells, B cells, and mature dendritic cells. The expression of CCR7 is associated with lymph node metastases, stromal invasion and overall survival27. In breast cancer patients, lymph nodes are the first site of regional nodal metastasis and the presence of metastasis in lymph nodes is important for staging and prognosis. CCL21, the ligand of CCR7, is highly expressed in lymph nodes. Therefore, functional CCR7 may facilitate cancer cells to metastasize to lymph nodes in response to CXCL21. Increasing emphasis has been placed on developing CXCR4 antagonists in cancer therapy. Given this, our data also show the possibility of making anti-CCR7 treatment a new strategy for the treatment of cancer metastasis.
Author contribution
Sen-sen LIN, Sheng-tao YUAN and Lu-yong ZHANG designed the research; Sen-sen LIN, Ren-ping ZHAO and Wen-lu LIANG performed the research; Li SUN and Yan-kai ZHANG contributed new reagents or analytical tools; Sen-sen LIN, Sheng-tao YUAN and Lu-yong ZHANG analyzed the data; and Sen-sen LIN prepared the manuscript.
References
Thiery JP, Sleeman JP . Complex networks orchestrate epithelial mesenchymal transitions. Nat Rev Mol Cell Biol 2006; 7: 131–42.
Chambers AF, Groom AC, MacDonald IC . Dissemination and growth of cancer cells in metastatic sites. Nat Rev Cancer 2002; 2: 563–72.
Pienta KJ, Loberg R . The “emigration, migration, and immigration” of prostate cancer. Clin Prostate Cancer 2005; 4: 24–30.
Leong SP, Cady B, Jablons DM, Garcia-Aguilar J, Reintgen D, Jakub J, et al. Clinical patterns of metastasis. Cancer Metastasis Rev 2006; 25: 221–32.
Gupta SK, Lysko PG, Pillarisetti K, Ohlstein E, Stadel JM . Chemokine receptors in human endothelial cells: functional expression of CXCR4 and its transcriptional regulation by inflammatory cytokines. J Biol Chem 1998; 273: 4282–7.
Liotta LA . An attractive force in metastasis. Nature 2001; 410: 24–5.
Kang H, Watkins G, Parr C, Douglas-Jones A, Mansel RE, Jiang WG . Stromal cell derived factor-1: its influence on invasiveness and migration of breast cancer cells in vitro, and its association with prognosis and survival in human breast cancer. Breast Cancer Res 2005; 7: 402–10.
Andre F, Cabioglu N, Assi H, Sabourin JC, Delaloge S, Sahin A, et al. Expression of chemokine receptors predicts the site of metastatic relapse in patients with axillary node positive primary breast cancer. Ann Oncol 2006; 17: 945–51.
Cabioglu N, Yazici MS, Arun B, Broglio KR, Hortobagyi GN, Price JE, et al. CCR7 and CXCR4 as novel biomarkers predicting axillary lymph node metastasis in T1 breast cancer. Clin Cancer Res 2005; 11: 5686–93.
Cabioglu N, Sahin A, Doucet M, Yavuz E, Igci A, Yildirim EO, et al. Chemokine receptor CXCR4 expression in breast cancer as a potential predictive marker of isolated tumor cells in bone marrow. Clin Exp Metastasis 2005; 22: 39–46.
Wilson JL, Burchell J, Grimshaw MJ . Endothelins induce CCR7 expression by breast tumor cells via endothelin receptor A and hypoxia-inducible factor-1. Cancer Res 2007; 67: 854–5.
Takeuchi H, Fujimoto A, Tanaka M, Yamano T, Hsueh E, Hoon DS . CCL21 chemokine regulates chemokine receptor ccr7 bearing malignant melanoma cells. Clin Cancer Res 2004; 10: 2351–8.
Iurlaro M, Loverro G, Vacca A, Cormio G, Ribatti D, Minischetti M, et al. Angiogenesis extent and expression of matrix metalloproteinase-2 and -9 correlate with upgrading and myometrial invasion in endometrial carcinoma. Eur J Clin Invest 1999; 29: 793–801.
Sillem M, Prifti S, Koumouridis A, Runnebaum B . Invasiveness corresponds to differentiation rather than to proteinase secretion in endometrial cancer cell lines. Eur J Gynaecol Oncol 1999; 20: 367–70.
Hu W, Zhen X, Xiong B, Wang B, Zhang W, Zhou W . CXCR6 is expressed in human prostate cancer in vivo and is involved in the in vitro invasion of PC3 and LNCap cells. Cancer Sci 2008; 99: 1362–9.
Tang CH, Tan TW, Fu WM, Yang RS . Involvement of matrix metalloproteinase 9 in stromal cell-derived factor-1/CXCR4 pathway of lung cancer metastasis. Carcinogenesis 2008; 29: 35–43.
Kaufmann SH, Peereboom D, Buckwalter CA, Grochow LB, Donehower RC, et al. Cytotoxic effects of topotecan combined with various anticancer agents in human cancer cell lines. J Nat Cancer Inst 1996; 88: 734–41.
von Pawel J, Gatzemeier U, Pujol JL, Moreau L, Bildat S, Ranson M, et al. Phase II comparator study of oral versus intravenous topotecan in patients with chemosensitive small-cell lung cancer. J Clin Oncol 2001; 19: 1743–9.
Rodriguez M, Rose PG . Improved therapeutic index of lower dose topotecan chemocherapy in recurrent ovarian cancer. Gynecol Oncol 2001; 83: 257–62.
Oberhoff C, Kieback DG, Wurstlein R, Deertz H, Sehouli J, van Soest C, et al. Topotecan chemotherapy in patients with breast cancer and brain metastases: results of a pilot study. Onkologie 2001; 24: 256–60.
Korfel A, Oehm C, von Pawel J, Keppler U, Deppermann M, Kaubitsch S, et al. Response to topotecan of symptomatic brain metastases of small-cell lung cancer also after whole-brain irradiation: a multicentre phase II study. Eur J Cancer 2002; 38: 1724–9.
Hou YF, Yuan ST, Li HC, Wu J, Lu JS, Liu G, et al. ER beta exerts multiple stimulative effects on human breast carcinoma cells. Oncogene 2004; 23: 5799–806.
Vicari AP, Caux C . Chemokines in cancer. Cytokine Growth Factor Rev 2002; 13: 143–54.
Murakami T, Cardones AR, Hwang ST . Chemokine receptors and melanoma metastasis. J Dermatol Sci 2004; 36: 71–8.
Tanaka T, Bai Z, Srinoulprasert Y, Yang BG, Hayasaka H, Miyasaka M . Chemokines in tumor progression and metastasis. Cancer Sci 2005; 96: 317–22.
Wang J, Xi L, Gooding W, Godfrey TE, Ferris RL . Chemokine receptors 6 and 7 identify a metastatic expression pattern in squamous cell carcinoma of the head and neck. Adv Otorhinolaryngol 2005; 62: 121–33.
Kodama J, Hasengaowa, Kusumoto T, Seki N, Matsuo T, Ojima Y, et al. Association of CXCR4 and CCR7 chemokine receptor expression and lymph node metastasis in human cervical cancer. Ann Oncol 2007; 18: 70–6.
Liang Z, Wu T, Lou H, Yu X, Taichman RS, Lau SK, et al. Inhibition of breast cancer metastasis by selective synthetic polypeptide against CXCR4. Cancer Res 2004; 64: 4302–8.
Lechertier T, Berard M, Vassy R, Herve MA, Crepin M . Transendothelial migration of two metastatic breast carcinoma cells depend on the SDF-lalpha-CXCR4 complexes. Anticancer Res 2004; 24: 4011–7.
Singh S, Singh UP, Grizzle WE, Lillard JW Jr . CXCL12-CXCR4 interactions modulate prostate cancer cell migration, metalloproteinase expression and invasion. Lab Invest 2004; 84: 1666–76.
Chinni SR, Sivalogan S, Dong Z, Filho JC, Deng X, Bonfil RD, et al. CXCL12/CXCR4 signaling activates Akt-1 and MMP-9 expression in prostate cancer cells: the role of bone microenvironment-associated CXCL12. Prostate 2006; 66: 32–48.
Redondo-Muñoz J, José Terol M, García-Marco JA, García-Pardo A . Matrix metalloproteinase-9 is up-regulated by CCL21/CCR7 interaction via extracellular signal-regulated kinase-1/2 signaling and is involved in CCL21-driven B-cell chronic lymphocytic leukemia cell invasion and migration. Blood 2008; 111: 383–6.
Acknowledgements
This project was financially supported by the National High Technology Research and Development Program of China (863 Program, No 2004AA2Z3785) and by a grant from the Natural Science Foundation of Jiangsu province (No BK2006150).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Lin, Ss., Sun, L., Zhang, Yk. et al. Topotecan inhibits cancer cell migration by down-regulation of chemokine CC motif receptor 7 and matrix metalloproteinases. Acta Pharmacol Sin 30, 628–636 (2009). https://doi.org/10.1038/aps.2009.32
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/aps.2009.32