Abstract
Objective:
To evaluate repeat surfactant therapy for the treatment of respiratory failure associated with postsurfactant slump in extremely low birth weight infants (ELBW) by characterizing the population of premature infants who develop postsurfactant slump and measuring their response to a secondary course of surfactant therapy.
Study Design:
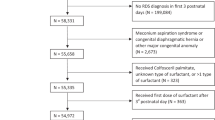
A retrospective analysis of a cohort of all patients admitted over a 3-year period with birth weights <1000?g (ELBW infants). Information was collected by chart review and the patients were categorized into three distinct groups for analysis. Initial surfactant only, patients who received surfactant replacement therapy only for respiratory distress syndrome (RDS); repeat surfactant, patients who received both initial surfactant replacement for RDS and repeat surfactant therapy for postsurfactant slump (defined as respiratory failure after 6 days of age), and no surfactant, patients in whom no surfactant was ever administered. A respiratory severity score (RSS) was used to measure the severity of lung disease and response to surfactant therapy.
Results:
Over 3 years, there were 165 ELBW infants who could develop postsurfactant slump and be eligible for repeat surfactant therapy. There were 39 infants who never received any surfactant therapy estimated gestational age (EGA) 27.7±1.7, birth weight 856±109?g) either at birth or after 6 days of life. There were 126 patients treated for RDS with initial surfactant replacement therapy (EGA 25.6±1.9 weeks, birth weight 713±179?g). Out of these RDS patients, 101 improved with an initial course of surfactant therapy (EGA 26±1.8, birth weight 751±143?g), but 25 (20% of the patients with RDS) developed postsurfactant slump and received a repeat course of surfactant therapy (EGA 24.7±1.2, birth weight 647±120?g). The repeat surfactant group (postsurfactant slump) was significantly more premature and had significantly lower birth weights compared to both the initial surfactant only group and the no surfactant ever group. Logistic regression analysis revealed that lack of antenatal steroids, earlier gestational age, and the receiving of 2 or more doses of surfactant to treat the initial RDS were significantly associated with receiving repeat surfactant therapy for postsurfactant slump. Of the 25 patients treated with a repeat course of surfactant therapy more than 70% of patients (n=18) had an improvement in their lung disease with a 15% reduction in their RSS. This improvement was significant at all time points evaluated (12, 24, and 48?h).
Conclusion:
We found that a repeat course of surfactant therapy, after day of life 6, led to a significant improvement in hypoxemic respiratory failure in premature infants with postsurfactant slump. Infants who received repeat surfactant therapy were born at a significantly earlier gestational age, had significantly smaller birth weight and had significantly worse lung disease. They were significantly less likely to have received antenatal steroids and were significantly more likely to have received multiple doses of surfactant to treat their initial RDS. A repeat course of surfactant therapy for patients with postsurfactant slump appeared beneficial in the short-term. These initial findings would support performing randomized control trials of repeat surfactant therapy for postsurfactant slump.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
Abbreviations
- RSS:
-
respiratory severity score
- RDS, respiratory distress syndrome, BPD:
-
bronchopulmonary dysplasia
- ELBW:
-
extremely low birth weight
- ROP:
-
retinopathy of prematurity
- IVH:
-
intraventricular hemorrhage
References
Enhorning G, Shennan A, Possmayer F, Dunn M, Chen CP, Milligan J . Prevention of neonatal respiratory distress syndrome by tracheal instillation of surfactant: a randomized clinical trial. Pediatrics 1985; 76: 145–153.
Hoekstra RE, Jackson JC, Myers TF, Frantz III ID, Stern ME, Powers WF et al. Improved neonatal survival following multiple doses of bovine surfactant in very premature neonates at risk for respiratory distress syndrome. Pediatics 1991; 88: 10–16.
Smyth JA, Metcalfe IL, Duffty P, Possmayer F, Bryan MH, Enhorning G . Hyaline membrane disease treated with bovine surfactant. Pediatics 1983; 71: 913–917.
Sobel DB, Carroll A . Postsurfactant slump: early prediction of neonatal chronic lung disease. J Perinatol 1994; 14: 268–274.
Clark RH, Gerstmann DR, Jobe AH, Moffitt ST, Slutsky AS, Yoder BA . Lung injury in neonates: causes, strategies for prevention, and long-term consequences. J Pediatr 2001; 139: 478–486.
Curley AE, Sweet DG, Thornton CM, O'Hara MD, Chesshyre E, Pizzotti J et al. Chorioamnionitis and increased neonatal lung lavage fluid matrix metalloproteinase-9 levels: implications for antenatal origins of chronic lung disease. Am J Obstet Gynecol 2003; 188: 871–875.
Van Marter LJ, Dammann O, Allred EN, Leviton A, Pagano M, Moore M et al. Chorioamnionitis, mechanical ventilation, and postnatal sepsis as modulators of chronic lung disease in preterm infants. J Pediatr 2002; 140: 171–176.
Merrill JD, Ballard RA, Cnaan A, Hibbs AM, Godinez RI, Godinez MH et al. Dysfunction of pulmonary surfactant in chronically ventilated premature infants. Pediatr Res 2004; 56: 918–926.
Pandit PB, Dunn MS, Kelly EN, Perlman M . Surfactant replacement in neonates with early chronic lung disease. Pediatics 1995; 95: 851–854.
Bissinger R, Carlson C, Hulsey T, Eicher D . Secondary surfactant deficiency in neonates. J Perinatol 2004; 24: 663–666.
Bloom BT, Kattwinkel J, Hall RT, Delmore PM, Egan EA, Trout JR et al. Comparison of Infasurf (calf lung surfactant extract) to Survanta (beractant) in the treatment and prevention of respiratory distress syndrome. Pediatics 1997; 100: 31–38.
Hall SB, Venkitaraman AR, Whitsett JA, Holm BA, Notter RH . Importance of hydrophobic apoproteins as constituents of clinical exogenous surfactants. Am Rev Respir Dis 1992; 145: 24–30.
Seeger W, Grube C, Gunther A, Schmidt R . Surfactant inhibition by plasma proteins: differential sensitivity of various surfactant preparations. Eur Respir J 1993; 6: 971–977.
Beresford MW, Shaw NJ . Bronchoalveolar lavage surfactant protein A, B, and D concentrations in preterm infants ventilated for respiratory distress syndrome receiving natural and synthetic surfactants. Pediatr Res 2003; 53: 663–670.
Taeusch HW, Keough KMW . Inactivation of pulmonary surfactant and the treatment of acute lung injuries. Pediatr Pathol Molec Med 2001; 20: 519–536.
Poynter SE, LeVine AM . Surfactant biology and clinical application. Crit Care Clin 2003; 19: 459–472.
Muller B, Garn H, Hochscheid R . Impaired recycling of surfactant-like liposomes in type ii pneumocytes from injured lungs. Thorax 2003; 58: 127–134.
Herting E, Moller O, Schiffmann JH, Robertson B . Surfactant improves oxygenation in infants and children with pneumonia and acute respiratory distress syndrome. Acta Paediatr 2002; 91: 1174–1178.
Greenough A . Expanded use of surfactant replacement therapy. Eur J Pediatr 2000; 159: 635–640.
Acknowledgements
Supported by a grant from Dey Pharmaceuticals.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Katz, L., Klein, J. Repeat surfactant therapy for postsurfactant slump. J Perinatol 26, 414–422 (2006). https://doi.org/10.1038/sj.jp.7211533
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.jp.7211533
Keywords
This article is cited by
-
Patent ductus arteriosus (PDA) and response to late surfactant treatment in premature infants
Journal of Perinatology (2023)
-
Characteristics and outcomes of preterm neonates according to number of doses of surfactant received
Journal of Perinatology (2021)
-
Surfactant status and respiratory outcome in premature infants receiving late surfactant treatment
Pediatric Research (2019)
-
Genetic variation in CRHR1 is associated with short-term respiratory response to corticosteroids in preterm infants at risk for bronchopulmonary dysplasia
Pediatric Research (2019)
-
Surfactant replacement therapy beyond respiratory distress syndrome in neonates
Indian Pediatrics (2016)