Abstract
Socioeconomic differences in age-standardised crude survival for women diagnosed with breast cancer during 1991–1999 in England were influenced by the population of the geographic area used to assign the deprivation index, but not by the choice of index.
Similar content being viewed by others
Main
In the absence of individual data on personal circumstances, the socioeconomic status of cancer patients has often been determined using a census-derived or area-based score designed to reflect some aspect of material deprivation or socioeconomic status of the small geographic area in which a person resides. Using such an ecologic approach, large differences in cancer patient survival have been described in various countries (Boyd et al, 1999; Coleman et al, 2001, 2004; Bradley et al, 2001). However, it is not known to what extent the observed variability in the deprivation gradients is due to the nature of the small-area geographies in question, the years to which the deprivation data apply, or the particular deprivation index used. This analysis aims to clarify the impact of each of these factors with specific reference to breast cancer survival in England in the 1990s. It was originally conducted in order to determine the most suitable deprivation geography to use in a large-scale cancer survival study in which a single index of deprivation could not be consistently applied across the study period (Coleman et al, 2004).
Materials and methods
Table 1 summarises the deprivation measures applied. We used three deprivation indices for the period 1991–2001: the census-derived Townsend score (Townsend et al, 1988) and the Indices of Multiple Deprivation (IMD) 2000 (Department of the Environment, 2000) and 2004 (Neighbourhood Renewal Unit, 2004) comprising a number of indices of deprivation for different domains of life. Each IMD domain is based upon routinely available administrative data. Indices were calculated using several different definitions of small geographic area as the basis of analysis, consisting of census Enumeration District (ED) 1991, electoral ward 1991 and 1998, census-defined Standard Table wards 2001 and Lower-Level Super Output Area 2001 (SOA, a new census geography). Table 2 summarises the number of geographic units in England, and the mean, standard deviation (s.d.) and coefficient of variation (CV) of their population. The Townsend score was calculated for two geographic levels in 1991 and 2001. The IMD 2000 was available from data applying to 1998, for each electoral ward as defined in 1998, while the IMD 2004 used data from 2000 and 2001 for each SOA as defined in 2001. We used only the income, employment and education domains of the IMD 2000 and 2004, since these domains displayed the greatest temporal consistency of definition between 1998 and 2001. We excluded the health domain because it was likely to be autocorrelated with cancer survival. We also examined a crude measure of material deprivation: the proportion of adults registered as being in receipt of income support during 1995 for each of the electoral wards defined in 1998. In all, deprivation was categorised by 11 unique combinations of geographic unit, data time point and deprivation index. Each set of small areas in England was ranked on the relevant index and divided into five deprivation categories defined by quintiles of its national distribution, numbered from 1 (the most affluent areas) to 5 (the most deprived areas).
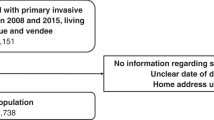
All women resident in England diagnosed aged 15 or over with malignant breast cancer during the period 1 January 1991 to 31 December 1999 were eligible for inclusion. Tumour records were excluded if they represented a bilateral, synchronous or second tumour (4.2%), if survival time or vital status was unknown (6.6%), if the woman was aged 100 years or over at diagnosis (0.1%) or if baseline data fields were inconsistent (<0.1%). Follow-up was complete on all women to 31 December 2001. A deprivation category for each of the 11 unique combinations was assigned to each individual patient on the basis of her postcode at diagnosis. One percent of records could not be linked to one or more of the 11 combinations due to missing geographic information, and these were excluded from all analyses. A total of 246 611 women (88% of those eligible) were included in the analyses.
Crude survival was estimated using individual survival times. Five-year survival rates were directly age standardised using a detailed set of 12 age groups (15–34, 35–39, …, 80–84 and 85–99) in order to adjust as fully as possible for any differences between deprivation categories in the age structure of women with breast cancer. The age structure of all the women included in the analyses was used as the standard.
The deprivation ‘gap’ in survival between the most affluent and the most deprived categories was estimated using least-squares linear regression. As indicated in Table 1, 11 different models were fitted, one for each unique combination of geographic unit, data time point and deprivation index. Each model was fitted upon the five quintile-specific age-standardised survival rates, each weighted by its standard error. A nonlinear relationship between deprivation and survival was also modelled using a quadratic term (y=a+bx+cx2). The statistical significance of differences in the survival gradient between any two models was assessed by fitting a single model to the 10 quintile-specific rates in question, with and without an interaction term, and applying the likelihood ratio test. All results were evaluated at the 95% significance level.
Results
A significant quadratic component was found in the association between crude survival and socioeconomic deprivation with all 11 combinations of geographic unit, data time point and deprivation index.
Impact of geography and time point
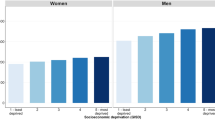
The deprivation gap in 5-year survival based on the 1991 Townsend score for electoral wards (−5.53%) was significantly smaller than that based on EDs (−7.28%), for which the average population is less than a tenth that of wards (Table 2, Figure 1A). Similarly, the deprivation gap in survival based on Townsend scores for the 2001 Standard Table wards (−5.25%) was significantly smaller than that estimated with SOA-based Townsend scores (−7.01%). SOAs are about one-third the size of wards (Table 2, Figure 1B). In contrast, there was no significant difference between the deprivation gaps in survival assessed with Townsend scores based on wards for 1991 and 2001, for which the average populations were very similar. In addition, no significant difference was observed between the deprivation survival gap based upon the Townsend score for EDs in 1991 and SOAs in 2001, despite the fact that SOAs are three times larger than EDs.
Crude age-standardised 5-year survival, with 95% confidence intervals, by Townsend deprivation category and associated fitted quadratic regression lines in (A) 1991 and (B) 2001: England, women (15–99 years) diagnosed with breast cancer 1991–1999 and followed up until 2001. P-values originate from a likelihood ratio test of the interaction between deprivation category and geographic unit of analysis (see text).
Impact of deprivation score
For a given geographic unit of analysis and the same data time point, the deprivation gap in survival was similar for all measures of deprivation (Table 2). The deprivation gaps for income support 1995 and the income domain of IMD 2000 were not significantly different, nor was there a significant difference between the gaps identified by the income and employment domains of the IMD 2000. The IMD 2000 education domain identified a slightly but significantly smaller gap (−5.28%) than both the employment and income domains, but the differences were all less than 1%. The deprivation gap in survival varied between −7.01 and −7.44% with the four deprivation indices measured at SOA level in 2001, but none of these small differences was significant.
Discussion
We have shown that when using an ecologic approach, the measurement of deprivation differentials in breast cancer survival in England during the late 20th century was primarily influenced by the population of the geographic area for which the deprivation index is derived, rather than by the definition of the index itself.
Although small in absolute terms, the influence of underlying geography is striking. For a given time point and deprivation score, the deprivation gap in crude survival was some 25% smaller when estimated with large geographic units than with small ones. These differences represent a dilution effect caused by the larger population of the larger area, and the associated increase in social heterogeneity. For example, the mean population of EDs in 1991 was about 10 times smaller than that of the 1991 electoral wards, and had a much smaller CV (see Table 2). The differences in population size and homogeneity between SOAs and Standard Table wards in 2001 were also marked.
The interpretation of these patterns as a dilution effect is supported by three other observations. First, the impact of geography is seen primarily in the most deprived quintiles. The mean population size of both 1991 electoral wards and 2001 Standard Table wards increases with increasing deprivation, while for EDs and SOAs, the population size of each quintile is fairly constant (data not shown). These patterns result in the mean population of deprived wards being much larger than that of deprived EDs or SOAs, while the population size of affluent wards is more similar to that of affluent EDs and SOAs. This leads to greater attenuation in survival for the more deprived categories. Second, the survival gap estimated with ward-based Townsend scores was similar for the 1991 and 2001 wards, which had a similar mean population size and CV (Table 2). Finally, the deprivation gaps in survival identified for SOAs in 2001 and EDs in 1991 were not significantly different. In this case, although SOAs have a population three times the size of EDs in 1991, they are much more homogeneous with respect to their size (CV 13 vs 37% Table 2) and their social characteristics (Martin, 2002). It appears that the joint effect of these two competing factors is to produce a very similar deprivation gap in survival for EDs and SOAs.
The definition of the deprivation index had little impact on the survival gap. Thus for electoral wards in 1998, the estimated deprivation gap in survival was very similar when deprivation was categorised either by the proportion of the population on income support or by the more complex income domain score, suggesting that the simpler index was just as useful for detecting socioeconomic differences in cancer survival. However, the use of two or more different scores may help in understanding the meaning and/or the mechanisms of such inequalities. Categorisation of deprivation using educational rather than employment or income variables led to a smaller deprivation gap in survival using IMD 2000 (based on wards), but not IMD 2004 (based on SOAs). Since the constituent variables for IMD 2000 and IMD 2004 are similar, this may again indicate attenuation of the effect of deprivation on survival with the larger geographic unit.
This analysis has only examined survival from breast cancer among women, but is probable that these observations apply similarly to incidence or mortality data and other diseases in both sexes. Our results are consistent with some of the literature on this topic, which has shown that the choice of deprivation score has little impact upon socioeconomic differences in morbidity (Hoare, 2003), and that underlying geography is influential in mortality and cancer incidence differentials (Krieger et al, 2002). Our results are less consistent with the conclusions of three other published studies, in which differences in the explanatory power of several deprivation indices were detected (Morris and Carstairs, 1991) and no impact of small-area geography was observed (Carr-Hill and Rice, 1995; Reijneveld et al, 2000). This may be due to the fact that these studies used outcomes other than cancer (Morris and Carstairs, 1991), or because the populations of the geographic areas examined were much more similar (Reijneveld et al, 2000), or a result of the analytic approach applied in which individual variables were correlated with area-derived data (Carr-Hill and Rice, 1995). Our study adds a cancer-specific component to this literature, and demonstrates the primary importance of deprivation geography when interpreting ecologic studies on socioeconomic differences in cancer survival.
Change history
16 November 2011
This paper was modified 12 months after initial publication to switch to Creative Commons licence terms, as noted at publication
References
Boyd C, Zhang-Salomons JY, Groome PA, Mackillop WJ (1999) Associations between community income and cancer survival in Ontario, Canada, and the United States. J Clin Oncol 17: 2244–2255
Bradley CJ, Given CW, Roberts C (2001) Disparities in cancer diagnosis and survival. Cancer 91: 178–188
Carr-Hill R, Rice N (1995) Is Enumeration District level an improvement on ward level analysis in studies of deprivation and health? J Epidemiol Commun Health 49(Suppl 2): S28–S29
Coleman MP, Babb P, Sloggett A, Quinn MJ, De Stavola BL (2001) Socioeconomic inequalities in cancer survival in England and Wales. Cancer 91: 208–216
Coleman MP, Rachet B, Woods LM, Mitry E, Riga M, Cooper N, Quinn MJ, Brenner H, Esteve J (2004) Trends and socioeconomic inequalities in cancer survival in England and Wales up to 2001. Br J Cancer 90: 1367–1373
Department of the Environment, Transport and the Regions (2000) Measuring Multiple Deprivation at the Small Area Level: The Indices of Deprivation 2000. London: Department of the Environment, Transport and the Regions
Hoare J (2003) Comparison of area-based inequality measures and disease morbidity in England, 1994–1998. Health Stat Q 18: 18–24
Krieger N, Chen JT, Waterman PD, Soobader MJ, Subramanian SV, Carson R (2002) Geocoding and monitoring of US socioeconomic inequalities in mortality and cancer incidence: does the choice of area-based measure and geographic level matter? The Public Health Disparities Geocoding Project. Am J Epidemiol 156: 471–482
Martin D (2002) Geography for the 2001 census in England and Wales. Popul Trend 108: 7–15
Morris R, Carstairs V (1991) Which deprivation? A comparison of selected deprivation indexes. J Public Health Med 13: 318–326
Neighbourhood Renewal Unit, Office for the Deputy Prime Minister (2004) The English Indices of Deprivation 2004 (Revised). London: Neighbourhood Renewal Unit, Office for the Deputy Prime Minister
Reijneveld SA, Verheij RA, de Bakker DH (2000) The impact of area deprivation on differences in health: does the choice of the geographical classification matter? J Epidemiol Commun Health 54: 306–313
Townsend P, Phillimore P, Beattie A (1988) Health and Deprivation: Inequality and The North. New York: Croom Helm
Acknowledgements
We would like to thank the staff of the National Cancer Intelligence Centre, Office for National Statistics, London, for linking the deprivation scores to the breast cancer records and Dr Catherine Lejeune, Dijon, for her insightful comments on the Townsend deprivation score.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
From twelve months after its original publication, this work is licensed under the Creative Commons Attribution-NonCommercial-Share Alike 3.0 Unported License. To view a copy of this license, visit http://creativecommons.org/licenses/by-nc-sa/3.0/
About this article
Cite this article
Woods, L., Rachet, B. & Coleman, M. Choice of geographic unit influences socioeconomic inequalities in breast cancer survival. Br J Cancer 92, 1279–1282 (2005). https://doi.org/10.1038/sj.bjc.6602506
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.bjc.6602506
Keywords
This article is cited by
-
What can hospital emergency admissions prior to cancer diagnosis tell us about socio-economic inequalities in cancer diagnosis? Evidence from population-based data in England
British Journal of Cancer (2024)
-
Socio-economic inequalities in lung cancer mortality in Spain: a nation-wide study using area-based deprivation
International Journal for Equity in Health (2023)
-
Cancer Mortality and Deprivation: Comparison Among the Performances of the European Deprivation Index, the Italian Deprivation Index and Local Socio-Health Deprivation Indices
Social Indicators Research (2020)
-
Cancer survival disparities worsening by socio-economic disadvantage over the last 3 decades in new South Wales, Australia
BMC Public Health (2017)
-
Assessment of the ecological bias of seven aggregate social deprivation indices
BMC Public Health (2017)