Abstract
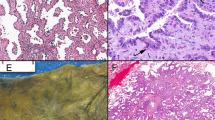
We have previously described a group of non-small cell lung carcinomas without morphological evidence of neo-angiogenesis. In these tumours neoplastic cells fill up the alveoli and the only vessels present appear to belong to the trapped alveolar septa. In the present study we have characterised the phenotype of the vessels present in these non-angiogenic tumours, in normal lung and in angiogenic non-small cell lung carcinomas. The vessels, identified by the expression of CD31, were scored as mature when expressing the epitope LH39 in the basal membrane and as newly formed when expressing αVβ3 on the endothelial cells and/or lacking LH39 expression. In the nine putative non-angiogenic cases examined, the vascular phenotype of all the vessels was the same as that of alveolar vessels in normal lung: LH39 positive and αVβ3 variable or negative. Instead in 104 angiogenic tumours examined, only a minority of vessels (mean 13.1%; range 0–60%) expressed LH39, while αVβ3 (in 45 cases) was strongly expressed on many vessels (mean 55.5%; range 5–90%). We conclude that in putative non-angiogenic tumours the vascular phenotype is that of normal vessels and there is no neo-angiogenesis. This type of cancer may be resistant to some anti-angiogenic therapy and different strategies need to be developed.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 24 print issues and online access
$259.00 per year
only $10.79 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout






Similar content being viewed by others
References
Almeida BM, Challacombe SJ, Eveson JW, Smith CG, Leigh IM (1992a) A novel lamina lucida component of epithelial and endothelial basement membranes detected by LH39 monoclonal antibody. J Pathol 166: 243–253
Almeida BM, Challacombe SJ, Eveson JW, Morgan PR, Purkis PE, Leigh IM (1992b) The distribution of LH39 basement membrane epitope in the tumour stroma of oral squamous cell carcinomas. J Pathol 166: 369–374
Brooks PC, Clark RAF, Cheresh DA (1994) Requirement of vascular integrin aVb3 for angiogenesis. Science 264: 569–571
Coman DR, Sheldon WF (1946) The significance of hyperemia around tumour implants. Am J Pathol 22: 821
Folkman J (1971) Tumour angiogenesis: therapeutic implication. N Engl J Med 285: 1182–1186
Folkman J (1990) What is the evidence that tumours are angiogenesis dependent. JNCI 82: 4–6
Folkman J (1995) Tumour angiogenesis. In The molecular basis of cancer Mendelshon J, Howley PM, Israel MA, Liotta LA (eds). pp 206–232, Philadelphia, PA: W.B. Saunders
Friedlander M, Brooks PC, Shaffer RW, Kincaid CM, Varner JA, Cheres DA (1995) Definition of two angiogenic pathways by distinct alpha v integrins. Science 270: 1500–1502
Gasparini G, Brooks PC, Biganzoli E, Vermeulen PB, Bonoldi E, Dirix LY, Ranieri G, Miceli R, Cheresh DA (1998) Vascular integrin avb3: a new prognostic indicator in breast cancer. Clin Cancer Res 4: 2652–2634
Gutheil JC, Campbell TN, Pierce PR, Watkins JD, Huse WD, Bodkin DJ, Cheresh DA (2000) Targeted antiangiogenic therapy for cancer using vitaxin: A humanized monoclonal antibody to the integrin alpha(nu)beta(3). Clin Cancer Res 6: 3056–3061
Hanahan D, Folkman J (1996) Patterns and emerging mechanisms of the angiogenic switch during tumorigenesis. Cell 86: 353–364
Holash J, Maisonpierre PC, Compton D, Boland P, Alexander CR, Zagzag D, Yancopoulos GD, Wiegand SJ (1999a) Vessel cooption, regression, and growth in tumours mediated by angiopoietin and VEGF. Science 284: 1994–1998
Holash J, Wiegand SJ, Yancopoulos GD (1999b) New model of tumor angiogenesis: dynamic balance between vessel regression and growth mediated by angiopoietins and VEGF. Oncogene 18: 5356–5362
Hyjek E, Chadburn A, Dias S, Zhu Z, Witte L, Hicklin D, Ceserman E, Knowels D, Rafii S (1999) High grade Non-Hodgkin's lymphomas and Hodgkin's disease are associated with increase density of KDR+SMA(-) immature microvessels. Blood 94: Suppl 1 2659
Kakolyris S, Giatromanalaki, Koukourakis M, Leigh IM, Georgoulias V, Kanavaros P, Sivridis E, Gatter KC, Harris AL (1999) Assesment of vascular maturation in non small cell using a novel basement membrane component, LH39: correlation with p53 and angiogenic factor expression. Cancer Res 59: 5602–5607
Kakolyris S, Fox SB, Koukourakis M, Giatromanolaki A, Brown N, Leek RD, Taylor M, Leigh IM, Gatter KC, Harris AL (2000) Relationship of vascular maturation in breast cancer blood vessels to vascular density and metastasis, assessed by expression of a novel basement membrane component, LH39. Br J Cancer 82: 844–851
Kolin A, Koutoulakis T (1988) Role of arterial occlusion in pulmonary scar cancers. Hum Pathol 19: 1161–1167
Kolin A (1995) Tumor angiogenesis in human lung adenocarcinoma. Cancer 76: 151
Maniotis AJ, Folberg R, Hess A, Seftor EA, Gardner LMG, Pe'er J, Trent JM, Meltzer PS, Hendrix MJC (1999) Vascular channel formation by human melanoma cells in Vivo and in Vitro: vasculogenic mimicry. Am J Pathol 155: 739–752
Nagano N, Sasaki H, Aoyagi M, Hirakawa K (1993) Invasion of experimental rat brain tumor: early morphological changes following microinjection of C6 glioma cells. Acta Neuropathol Berl 86: 117–125
Navratil E, Couvelard A, Rey A, Henin D, Scoazec JY (1997) Expression of cell adhesion molecules by microvascular endothelial cells in the cortical and subcortical regions of normal human brain: an immunohistochemical analysis. Neuropathol Appl Neurobiol 23: 68–80
Offersen BV, Pfeiffer P, Hamilton-Dutoit S, Overgaard J (2001) Patterns of angiogenesis in nonsmall-cell hung carcinoma. Cancer 91: 1500–1509
Parums DV, Cordell JL, Micklem K, Heryet AR, Gatter KC, Mason DY (1990) JC70: a new monoclonal antibody that detects vascular endothelium associated antigen on routinely processed tissue sections. J Clin Pathol 43: 752–757
Pastorino U, Andreola S, Tagliabue E, Pezzella F, Incarbone M, Sozzi G, Buyse M, Menard S, Pierotti M, Rilke F (1997) Immunocytochemical markers in stage I lung cancer (NSCLC): relevance to prognosis. J Clin Oncol 15: 2858–2865
Pazouki S, Chisolm DM, Adi MM, Carmichael G, Farquharson M, Ogden GR, Schor SL, Schor AM (1997) The association between tumour progression and vascularity in the oral mucosa. J Pathol 183: 39–43
Pezzella F, Di Bacco A, Andreola S, Nicholson AG, Pastorino U, Harris AL (1996) Angiogenesis in primary lung cancer and lung secondaries. Eur J Cancer 32A: 2494–2500
Pezzella F, Pastorino U, Tagliabue E, Andreola S, Sozzi G, Gasparini G, Menard S, Gatter KC, Harris AL, Fox S, Buyse M, Pilotti S, Pierotti M, Rilke F (1997) Non-small cell lung carcinoma tumour growth without neo angiogenesis. Am J Path 5: 1417–1423
Pezzella F, Manzotti M, Di Bacco A, Viale G, Nicholson AG, Price R, Ratcliffe C, Pastorino U, Gatter KC, Altman DG, Harris AL, Pilotti S, Veronesi U (2000) Evidence for a novel non-angiogenic pathway in breast cancer metastasis. Lancet 355: 1787–1788
Rabb H, Barroso-Vicens E, Adams R, Pow-Sang J, Ramirez G (1996) Alpha-V/beta-3 and alpha-V/beta-5 integrin distribution in neoplastic kidney. Am J Nephrol 16: 402–408
Tang DG, Diglio CA, Honn KV (1994) Activation of microvascular epithelium by ecosanoid 12(S)-hydroxyeicosatetraeonic acid leads to enhanced tumor cell adhesion via up-regulation of surface expression of alpha v beta 3 integrin: a postranscriptional, protein kinase C- and cytoskeleton-dependent process. Cancer Res 54: 1119–1129
Warren BA (1979) The vascular morphology of tumors. In Tumor blood circulation: Angiogenesis, vascular morphology and blood flow of experimental human tumors Peterson H-I (ed) pp 1–47, FL: CRC Press
Wesseling P, van der Laak JA, de Leeuw H, Ruiter DJ, Burger PC (1994) Quantitative immunohistological analysis of the microvasculature in untreated human glioblastoma multiforme. Computer-assisted image analysis of whole tumor sections. J Neurosurg 81: 902–909
Acknowledgements
The authors would like to thank Professor Doug Altman for his suggestions and the many helpful discussions. Supported by the Imperial Cancer Research Fund and by a grant from ‘The Special Trustees of the Middlesex Hospital, University College Hospital and University College London Medical School’. E Passalidou was supported by a Research Fellowship from the European Respiratory Society.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Passalidou, E., Trivella, M., Singh, N. et al. Vascular phenotype in angiogenic and non-angiogenic lung non-small cell carcinomas. Br J Cancer 86, 244–249 (2002). https://doi.org/10.1038/sj.bjc.6600015
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.bjc.6600015
Keywords
This article is cited by
-
Vessel co-option and resistance to anti-angiogenic therapy
Angiogenesis (2020)
-
Pathological features of vessel co-option versus sprouting angiogenesis
Angiogenesis (2020)
-
Non-angiogenic tumours and their influence on cancer biology
Nature Reviews Cancer (2018)
-
Consensus guidelines for the use and interpretation of angiogenesis assays
Angiogenesis (2018)
-
Why some tumours trigger neovascularisation and others don’t: the story thus far
Chinese Journal of Cancer (2016)