Abstract
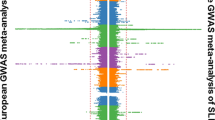
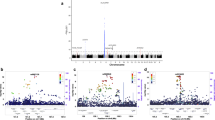
Anti-double-stranded DNA (anti-dsDNA) is arguably one of the most specific autoantibodies in systemic lupus erythematosus (SLE). This antibody is associated with more severe SLE and with glomerulonephritis. From 196 pedigrees multiplex for SLE, we selected those that had any SLE affected positive for anti-dsDNA by the Crithidia luciliae kinetoplast imunofluorescence assay. This stratification strategy tested the hypothesis that anti-dsDNA would identify a more genetically homogeneous group of pedigrees, in which previously undetected linkage effects could be established. A genome screen data for linkage to SLE was available at 307 microsatellite markers for this selected group of 71 pedigrees: 37 European-American, 29 African-American, and five others. The most significant results were obtained at 19p13.2 (LODmax = 4.93), named SLED1, in the 37 European-American pedigrees using a dominant model with mixed penetrances (92% for females and 49% for males) at 100% homogeneity (θ = 0). A second linkage effect, SLED2, was established in the 29 African-American pedigrees at 18q21.1 (LODmax = 3.40) using a recessive model with 100% penetrance (θ = 0.1). Parametric and non-parametric multipoint analyses were performed, which provided further evidence and support of susceptibility genes residing in these regions. In conclusion, two powerful linkages have been detected with SLE based on the presence of anti-dsDNA. These findings show SLE to be a richly complicated disease phenotype that is now ripe for important new discovery through a genetic approach.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 6 digital issues and online access to articles
$119.00 per year
only $19.83 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout





Similar content being viewed by others
References
Harley JB, Moser KL, Gaffney PM, Behrens TW . The genetics of human systemic lupus erythematosus Curr Opin Immunol 1998 10: 690–696
Deapen D, Escalante A, Weinrib L et al. A revised estimate of twin concordance in systemic lupus erythematosus Arthritis Rheum 1992 35: 311–318
Arnett FC . The genetics of human lupus In: Wallace DJ, Hahn BH (eds) Dubois’ Lupus Erythematosus. 5th edn Williams and Wilkins: Baltimore 1997 pp 77–117
Salmon JE, Millard S, Schachter LA et al. FcgammaRIIA alleles are heritable risk factors for lupus nephritis in African-Americans J Clin Invest 1996 97: 1348–1354
Tsao BP, Cantor RM, Kalunian KC et al. Evidence for linkage of a candidate chromosome 1 region to human systemic lupus erythematosus J Clin Invest 1997 99: 725–731
Moser KL, Neas BR, Salmon JE et al. Genome scan of human systemic lupus erythematosus: evidence for linkage on chromosome 1q in African-American pedigrees Proc Natl Acad Sci USA 1998 95: 14869–14874
Gaffney PM, Kearns GM, Shark KB et al. A genome-wide search for susceptibility genes in human systemic lupus erythematosus sib-pair families Proc Nat Acad Sci USA 1998 95: 14875–14879
Ho A, Magder LS, Barr SG, Petri M . Decreases in anti-double-stranded DNA levels are associated with concurrent flares in patients with systemic lupus erythematosus Arthritis Rheum 2001 44: 2342–2349
Arbuckle MR, James JA, Kohlhase KF, Rubertone MV, Dennis GJ, Harley JB . Development of anti-dsDNA autoantibodies prior to clinical diagnosis of systemic lupus erythematosus Scand J Immunol 2001 54: 211–219
Witte T, Hartung K, Matthias T et al. Association of IgA anti-dsDNA antibodies with vasculitis and disease activity in systemic lupus erythematosus SLE Study Group, Rheumatol Int 1998 18: 63–69
Witte T, Hartung K, Sachse C et al. IgM anti-dsDNA antibodies in systemic lupus erythematosus: negative association with nephritis. SLE Study Group Rheumatol Int 1998 18: 85–91
Nossent H, Berden J, Swaak T . Renal immunofluorescence and the prediction of renal outcome in patients with proliferative lupus nephritis Lupus 2000 9: 504–510
Amoura Z, Koutouzov S, Chabre H et al. Presence of antinucleosome autoantibodies in a restricted set of connective tissuediseases: antinucleosome antibodies of the IgG3 subclass are markers of renal pathogenicity in systemic lupus erythematosus Arthritis Rheum 2000 43: 76–84
Wigand R, Gottschalk R, Falkenbach A, Matthias T, Kaltwasser JP, Hoelzer D . Detection of dsDNA antibodies in diagnosis of systemic lupus erythematosus, comparative studies of diagnostic effectiveness of 3 ELISA methods with different antigens and a Crithidia luciliaeimmunofluorescence test Z Rheumatol 1997 56: 53–62
Tan EM, Cohen AS, Fries JF et al. The 1982 revised criteria for the classification of systemic lupus erythematosus Arthritis Rheum 1982 25: 1271–1277
Hochberg MC . Updating the American College of Rheumatology Criteria for systemic lupus erythematosus Arthritis Rheum 1998 41: 751
Arnett FC, Hamilton RG, Roebker M, Harley JB, Reichlin M . Increased frequencies of Sm and nRNP autoantibodies in American blacks compared to whites with systemic lupus erythematosus J Rheumatol 1988 15: 1773–1776
Lander E, Kruglyak L . Genetic dissection of complex traits: guidelines for interpreting and reporting linkage results Nat Genet 1995 11: 241–247
Hahn H, Tsao P . Antibodies to DNA In: Wallace DJ, Hahn BH (eds) Dubois’ Lupus Erythematosus. 5th edn Williams and Wilkins: Baltimore 1997 pp 410–411
Yasutomo K, Horiuchi T, Kagami S et al. Mutation of DNASE1 in people with systemic lupus erythematosus Nat Genet 2001 28: 313–314
Yasuda T, Nadano D, Sawazaki K, Kishi K . Genetic polymorphism of human deoxyribonuclease II (DNase II): low activity levels in urine and leukocytes are due to an autosomal recessive allele Ann Hum Genet 1992 56: 1–10
Krieser RJ, Eastman A . Deoxyribonuclease II: structure and chromosomal localization of the murine gene, and comparison with the genomic structure of the human and three C. eleganshomologs Gene 2000 252: 155–162
Yung RL, Richardson BC . Role of T cell DNA methylation in lupus syndromes Lupus 1994 3: 487–491
Deng C, Kaplan MJ, Yang J et al. Decreased Ras-mitogen-activated protein kinase signaling may cause DNA hypomethylation in T lymphocytes from lupus patients Arthritis Rheum 2001 44: 397–407
Quddus J, Johnson KJ, Gavalchin J et al. Treating activated CD4+ T cells with either of two distinct DNA methyltransferase inhibitors, 5-azacytidine or procainamide, is sufficient to cause a lupus-like disease in syngeneic mice J Clin Invest 1993 92: 38–53
Boehm J, Orth T, Van Nguyen P, Soling HD . Systemic lupus erythematosus is associated with increased autoantibody titers against calreticulin and grp94, but calreticulin is not the Ro/SS-A antigen Eur J Clin Invest 1994 24: 248–257
Seddiki N, Nato F, Lafaye P, Amoura Z, Piette JC, Mazie JC . Calreticulin, a potential cell surface receptor involved in cell penetration of anti-DNA antibodies J Immunol 2001 166: 6423–6429
McDonald JP, Rapic-Otrin V, Epstein JA et al. Novel human and mouse homologs of Saccharomyces cerevisiae DNA polymerase eta Genomics 1999 60: 20–30
Kelly JA, Moser KL, Harley JB . The genetics of systemic lupus erythematosus: putting the pieces together Genes Immun 2002 (in press)
Nath SK, Kelly JA, Namjou B et al. Evidence for a susceptibility gene, SLEV1, on chromosome 17p13 in families with vitiligo-related systemic lupus erythematosus Am J Hum Genet 2001 69: 1401–1406
Kaufman KM, Rankin J, Kelly JA, Harley JB, Scofield RH . A genetic marker within the CD44 gene confirms linkage at 11p13 in African-American families with lupus stratified by thrombocytopenia, but genetic association with CD44 is not present Genes Immun 2002 (in press)
Sawalha AH, Namjou B, Nath SK et al. Genetic linkage of systemic lupus erythematosus with chromosome 11q14 (SLEH1) in African-American families stratified by a nucleolar antinuclear antibody pattern Genes Immun 2002 (revisions submitted)
Quintero-Del-Rio AI, Kelly JA, Kilpatrick J, James JA, Harley JB . The genetics of systemic lupus erythematosus stratified by renal disease: linkage at 10q22.3 (SLEN1), 2q34-35 (SLEN2) and 11p15.6 (SLEN3) Genes Immun 2002 3 (Suppl 1): S57–S62
Fritzler MJ . Immunofluorescent antinuclear antibody tests In: Rose NR, Friedman H, Fahey JL (eds) Manual of Clinical Laboratory Immunology, 3rd edn American Society for Microbiology: Washington, D.C. 1986 pp 733–739
Ballon SP, Kushner I . Crithidia luciliae immunofluorescence test for antibodies to DNA In: Rose NR, Friedman H, Fahey JL (eds) Manual of Clinical Laboratory Immunology, 3rd edn American Society for Microbiology: Washington, D.C. 1986 pp 740–743
Clark GM, Reichlin M, Tomasi TB . Characterization of a soluble cytoplasmic antigen reactive with sera from patients with systemic lupus erythematosus J Immunol 1968 102: 117–122
Harris EN, Gharavi AE, Patel SP, Hughes GR . Evaluation of the anti-cardiolipin antibody test: report of an international workshop held 4 April 1986 Clin Exp Immunol 1987 68: 215–222
Olson JM . Relationship estimation by Markov-process models in a sib-pair linkage study Am J Hum Genet 1999 64: 1464–1472
S.A.G.E. Statistical Analysis for Genetic Epidemiology, release 4.0, Beta 3 Computer package, Cleveland (OH): Department of Epidemiology and Biostatistics, Case Western Reserve University 1999
Cottingham RW Jr, Idury RM, SchΩaffer AA . Faster sequential genetic linkage computations Am J Hum Genet 1993 53: 252–263
Terwilliger JD . A powerful likelihood method for the analysis of linkage disequilibrium between trait loci and one or more polymorphic marker loci Am J Hum Genet 1995 56: 777–787
Morton NE . Sequential tests for the detection of linkage Am J Hum Genet 1955 7: 277–318
Kruglyak L, Daly MJ, Reeve-Daly MP, Lander ES . Parametric and nonparametric linkage analysis: a unified multipoint approach Am J Hum Genet 1996 58: 1347–1363
Acknowledgements
The authors would like to thank the patients and family members who participated in this study and those who referred them to us. Ninety pedigrees (Cohorts A, B and C) were obtained from the Lupus Multiplex Registry and Repository (AR-1-2253) (see http://omrf.ouhsc.edu/lupus).
Author information
Authors and Affiliations
Corresponding author
Additional information
Supported by the NIH (AR12253, AI24717, AR42460, AR45231, AI31584, RR15577) and the US Department of Veterans Affairs.
Rights and permissions
About this article
Cite this article
Namjou, B., Nath, S., Kilpatrick, J. et al. Genome scan stratified by the presence of anti-double-stranded DNA (dsDNA) autoantibody in pedigrees multiplex for systemic lupus erythematosus (SLE) establishes linkages at 19p13.2 (SLED1) and 18q21.1 (SLED2). Genes Immun 3 (Suppl 1), S35–S41 (2002). https://doi.org/10.1038/sj.gene.6363905
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.gene.6363905
Keywords
This article is cited by
-
Sex differences in the genetic architecture of depression
Scientific Reports (2020)
-
Familial aggregation and linkage analysis of autoantibody traits in pedigrees multiplex for systemic lupus erythematosus
Genes & Immunity (2006)
-
Unraveling the genetics of systemic lupus erythematosus
Springer Seminars in Immunopathology (2006)
-
Current advances in the human lupus genetics
Current Rheumatology Reports (2004)
-
Looking back and looking forward
Genes & Immunity (2003)