Abstract
Potocki–Shaffer syndrome (PSS) is a contiguous gene deletion syndrome that results from haploinsufficiency of at least two genes within the short arm of chromosome 11[del(11)(p11.2p12)]. The clinical features of PSS can include developmental delay, mental retardation, multiple exostoses, parietal foramina, enlarged anterior fontanel, minor craniofacial anomalies, ophthalmologic anomalies, and genital abnormalities in males. We constructed a natural panel of 11p11.2–p13 deletions using cell lines from 10 affected individuals, fluorescence in situ hybridization (FISH), microsatellite analyses, and array-based comparative genomic hybridization (array CGH). We then compared the deletion sizes and clinical features between affected individuals. The full spectrum of PSS manifests when deletions are at least 2.1 Mb in size, spanning from D11S1393 to D11S1385/D11S1319 (44.6–46.7 Mb from the 11p terminus) and encompassing EXT2, responsible for multiple exostoses, and ALX4, causing parietal foramina. Yet one subject with parietal foramina whose deletion does not include ALX4 indicates that ALX4 in this subject may be rendered functionally haploinsufficient by a position effect. Based on comparative deletion mapping of eight individuals with the full PSS syndrome including mental retardation and two PSS families with no mental retardation, at least one gene related to mental retardation is likely located between D11S554 and D11S1385/D11S1319, 45.6–46.7 Mb from the 11p terminus.
Similar content being viewed by others
Introduction
Potocki–Shaffer syndrome (PSS) (MIM#601224) is a multiple congenital anomalies and mental retardation syndrome associated with a heterozygous deletion of 11p11.2p12. The full clinical spectrum of PSS includes developmental delay, mental retardation, multiple exostoses, parietal foramina, enlarged anterior fontanel, minor craniofacial anomalies, ophthalmologic anomalies, and genital abnormalities in males.1, 2 Major malformations of the cardiovascular, urinary, and central nervous systems are not often reported in individuals with this syndrome. To date, 23 individuals from 14 families with 11p11.2p12 deletions have been reported.1, 2, 3, 4, 5, 6, 7, 8, 9, 10, 11 One additional case was reported with del(11)(p11p12), but it is unclear if this child had the features of PSS.12
PSS is a contiguous gene syndrome (CGS) with two genes implicated in specific clinical features of this disorder. Exostosin 2 (EXT2 [MIM*60821) maps within 11p11.213, 14 and mutations in this gene result in the autosomal dominant condition of isolated hereditary multiple exostoses [MIM#133701].13, 14, 15 The Aristaless-like homeobox 4 gene (ALX4 [MIM*605420]) maps proximal to EXT2 and when haploinsufficient is involved in defects of skull ossification that manifest as parietal foramina.16, 17 As mutations in EXT2 or ALX4 do not cause mental retardation or craniofacial abnormalities, other genes are presumed to cause these features in PSS and are currently unknown. Large deletions of proximal 11p (eg del (11)(p11.2p14)) may result in features of PSS and WAGR syndrome (Wilms tumor, aniridia, genitourinary anomalies, mental retardation [MIM#194072]).7, 18 The 11p proximal deletions vary in size, and ongoing genotype–phenotype correlation will likely elucidate the genes causing the craniofacial anomalies and mental retardation in PSS.
We constructed a natural panel of 11p deletions using cell lines derived from 10 subjects, six of whom were newly identified (Table 1). The extent of the deletion region for each family or subject was determined using multiple fluorescence in situ hybridization (FISH) markers, microsatellite markers, and array-based comparative genomic hybridization (array CGH). Combined with the clinical features of the subjects, this deletion panel allows for genotype–phenotype correlation in this contiguous gene deletion syndrome.
Materials and methods
Study subjects
In all, 10 individuals with confirmed or suspected proximal deletions of 11p were studied (Table 1). Lymphoblastoid cell lines were received or established for all subjects and available parents and used for FISH, microsatellite, and microarray analysis after informed consent using either a Baylor College of Medicine or a Washington State University Institutional Review Board-approved protocol and consent form. Individual subjects were assigned a progressive number according to the order of their ascertainment in the PSS study. Four study subjects were previously reported (Table 1): PSS01, PSS02, PSS05, and PSS07. The clinical features of all subjects are shown in Table 2. The clinical descriptions of study subjects PSS01, PSS02, PSS05, and PSS07 can be found in Shaffer et al,8 Potocki and Shaffer,2 Hall et al,5 and Chien et al,3 respectively. The clinical descriptions of the newly ascertained subjects are as follows.
PSS03 is a female who was evaluated at 4 years of age. She was ascertained because of multiple exostoses and parietal foramina and is also affected with macrocephaly, short stature, and bowing of the lower extremities. The subject's height, weight, and head circumference were <3rd, <3rd, and 50th percentiles, respectively. She is developmentally normal. An initial karyotype was reportedly normal. A deletion was identified after FISH analysis using two probes, cSRL-102d9 and cSRL-42c6, which contain the EXT2 locus.19
PSS04 is a 3-year, 10-month-old male. He was diagnosed with 11p11.2p12 deletion by chromosome analysis performed at age 13 months because of abnormal clinical findings including developmental delay, hypotonia, microcephaly, parietal foramina, umbilical hernia, bilateral inguinal hernias, micropenis, and hypospadius. Exostoses were first noted at 18 months of age. Other medical problems include multiple upper respiratory tract infections, multiple episodes of otitis media, and hypogammaglobulinemia. An MRI of the brain showed no intracranial abnormalities at 3 years, 10 months. On examination, his height, weight, and FOC were at the 10th, 60th, and <5th percentiles, respectively. Dysmorphic craniofacial features are noted in Figure 1. Pulmonary, cardiac, and abdominal examinations were normal, and the phallus was of normal stretched length, contrary to earlier records. Radiographs revealed multiple exostoses and parietal foramina. A renal ultrasound showed a kidney length in the low normal range, and an ophthalmological exam revealed myopia.
Subject PSS04 at age 3 years, 10 months. Brachycephaly, broad forehead, frontal bossing, sparse lateral eyebrows, and prominent nose and nasal bridge are evident (a, d). A skull radiograph delineates the parietal foramina (b, e). Radiographs of the left humerus and right tibia show expansile lesions consistent with sessile osteochondromas, or exostosis (c, f). Consent has not been granted to show photographs of subject PSS04 on any websites. Please see print version for photographs.
PSS08 was ascertained after prenatal diagnosis and chromosome analysis revealed an 11p11.2p14 deletion. After her birth, the deletion was confirmed by cytogenetic analysis of peripheral blood. Multiple congenital anomalies were present, including large parietal foramina, aniridia, and dysmorphic facial features. Developmental delay was also present, although no further information regarding growth parameters was available. At 2 years of age she required lengthening of her Achilles tendon due to walking with inverted feet. At 29 months of age, following a routine screening protocol for Wilms tumor by renal ultrasound at 3-month intervals, a 4 cm mass was found on the left kidney. The mass was removed surgically, and a pathological exam confirmed a Wilms tumor.
PSS10 was ascertained at 11 years of age because of dysmorphic features and a hypoplastic corpus callosum. Physical examination revealed brachycephaly, short palpebral fissures, epicanthus, strabismus, deep-set eyes, short hands and feet, and micropenis. Additionally, the subject had severe speech delay and episodes of hyperactivity. Radiographs revealed multiple exostoses and small biparietal foramina. The subject's height, weight, and FOC were at the 75th, 75th, and 90th percentiles, respectively. A chromosomal analysis revealed an 11p11.2p12 deletion. At 11 years of age the subject developed uncontrolled episodes of aggression. The subject died at 12 years of age due to multiorgan failure resulting from pneumonia.
PSS12 was delivered at term and was appropriate for gestational age. The maternal serum triple screen showed an increased risk for trisomy 18. Chromosome analysis of amniotic fluid revealed a normal 46,XY complement. FISH performed at age 3.5 months because of developmental delay, parietal foramina, agenesis of the corpus callosum, and bilateral choroid plexus cysts revealed a deletion of EXT2. On examination at 13 months, his weight, length, and head circumference were at the 90th, 90th, and 40th percentiles, respectively. His head was brachycephalic with parietal foramina and fingertip anterior fontanel. There were two posterior hair whorls. The forehead was broad, and the face was full with prominent cheeks. There were sparse lateral eyebrows, a small nose, and hypoplasia of the nares. The pulmonary, cardiac, and abdominal examinations were normal. The testes were small, and the stretched penis length was 2.5 cm. Developmental assessment revealed that the subject's overall composite score was 64 (1st percentile). However, the subject exhibited a relative strength in socialization skills, which appeared to cluster at the 14-month level. Diagnostic evaluations revealed mild to moderate bilateral sensorineural hearing loss. No exostoses were detected by skeletal survey. A diagnosis of PSS was made after chromosome analysis revealed a visible deletion of 11p11.2.
In subject PSS13, a deletion 11p11.2p12 was detected by chromosome analysis performed at birth because of intrauterine growth retardation, microcephaly, oligohydramnios, and biparietal foramina. Hypotonia, cryptorchism, and congenital cardiovascular disease (ventricular septal defect) were also noted in the newborn period. Other medical problems included hearing impairment, history of multiple otitis media, visual impairment with esotropia, and history of respiratory illnesses requiring hospitalization. Upon evaluation at age 35 months the patient was below the 5th percentile for head circumference, weight, and length, and was severely hypotonic and globally developmentally delayed. Craniofacial features showed marked brachy/plagiocephaly, biparietal foramina, a broad forehead, sparse eyebrows, a prominent nasal bridge and hypoplastic alae nase. Developmental assessment showed significant global delay with performance ranging between the 4 and 12-month level. Diagnostic evaluation showed a sensorineural hearing impairment. An MRI showed mildly widened CSF spaces but normal myelination and a normally developed corpus callosum. No exostoses were detected on skeletal survey.
Contig construction
To refine the deletion regions and identify variability in deletion sizes, we constructed a physical map using information found in three public electronic-databases: the UCSC genome browser (http://genome.ucsc.edu), the NCBI genome browser (http://www.ncbi.nlm.org/), and Ensembl (http://www.ensembl.org/). In addition, we used information from published articles,9, 11, 13, 19, 20, 21 our own FISH-mapping efforts, and through assembly of our natural deletion panel after molecular analyses of the cell lines derived from the study participants. To determine the physical distance between the clones, we used the NCBI genome database (www.ncbi.nlm.org) and found that the majority of the previously reported bacterial artificial chromosomes (BACs) were only end-sequenced. To correlate them to a physical position on chromosome 11, we compared the two ends (SP6 and T7) with the BLAST database (http://www.ncbi.nlm.nih.gov/BLAST/) and found overlapping sequence with finished clones that physically linked our original clones. MapViewer (http://www.ncbi.nlm.nih.gov/mapview/map_search.cgi) was then used to estimate the clone position in Mb from the telomere. The mRNA sequences of PAX6, EXT2 and ALX4 were checked with BLAST to identify the overlap with the genomic clones. The UCSC genome database (http://genome.ucsc.edu) was used to localize one clone, RP11-85A19, within our contig. Selected FISH and microsatellite markers were used on each subject to identify the extent and parental origin of each deletion. Not all clones and markers were used on all subjects, but the extent of each deletion was delineated (Figure 2). The BAC clones were used to construct a microarray of the region.
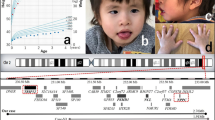
Physical map of proximal 11p (right side) and results of a natural deletion panel (left side) (not to scale). On the physical map, the solid vertical line represents the chromosome 11p11.2 region. The numbers to the left of this line show the distance from the short-arm telomere in Mb. Designations to the right show the STS markers in the region. The rectangles to the far right represent the large-insert clones and cosmids with available clone name used to construct the contig, based on the UCSC Nov. 2002 freeze. PAX6, EXT2, and ALX4 are shown in their relative locations (boxes). R=RP11-BAC library. On the natural deletion panel, black bars indicate the deleted regions. White bars indicate regions in which the extent of deletion is not known because clones do not overlap.
FISH analysis
The large-insert clones that map to 11p were available for FISH analysis on subject cell lines (Figure 2). Not all clones were selected for FISH analysis on all subjects. A total of 40 BAC clones were selected using the electronic-databases UCSC, NCBI, and Ensembl. Three cosmid clones (P60, Dreschler et al;22 cSRL-102d9 and cSRL-42c6, Stickens et al13 and Ligon et al19) and one additional BAC clone (RP11-706A13, Wu et al17) were also used. FISH was performed according to a standard protocol.23
Molecular analysis
To determine the parental origin and identify the breakpoints of the deleted 11p regions, highly polymorphic microsatellite markers within and flanking proximal 11p were used (Figure 2). DNA from seven study subjects (PSS01, PSS02, PSS03, PSS04, PSS05, PSS07, PSS08) and available parent cell lines was amplified by PCR, and products were visualized by autoradiography following electrophoresis in 6% denaturing polyacrylamide gels.24 For three subjects, parental origins were determined using genotyping performed with an ABI PRISM 3100-Avant genetic analyzer (Applied Biosystems, Foster City, CA, USA). The DS-30(D) dye set was used according to the manufacturer's specifications. Primers were obtained labeled with 5′-HEX or 5′6-FAM (Integrated DNA Technologies, Coralville, IA, USA). The ABI PRISM GeneScan analysis software and ABI PRISM Genotyper software were used to analyze the results.
Microarray construction
A total of 69 clones were arrayed, including 38 clones from 11p11.2–p13, 15 clones from 1p3625 used for normalization of the data prior to analyzing the 11p clones, and 11 X- and 5 Y-specific clones.
After insert DNA extraction with a RPM SPIN Midi kit (Q-BIOgene, Carlsbad, CA, USA), we sonicated the probes to a final size between 500 bp and 20 kb. We then precipitated the DNA with NaAc 3 M pH 5.2 (1:8 of the total volume) and isopropanol (1:1 volume). DNA was hydrated with sterile water for a final concentration of 50 ng/μl. Before printing, we added 50% DMSO with nitrocellulose as previously described.26 To ensure that no particular area of the microarray would lead to misclassification as a deletion, each clone was randomized in a 384-well plate and printed eight times on the microarray. The printing was conducted with an Omnigrid Accent Machine (GeneMachine, San Carlos, CA, USA) at 50% humidity and a temperature of 24°C at Signature Genomic Laboratories (Spokane, WA, USA). We used low-autofluorescence slides (VWR International, West Chester, PA, USA) treated with aminosilane (Sigma-Aldrich, Sheboygan Falls, WI, USA). Printed slides were baked at 80°C from 4 h to overnight and then washed with 80°C millipore water for 2 min and cold 95% ethanol for 1 min. The blocking was achieved with 10% bovine serum albumin fraction V (Sigma, St Louis, MO, USA) and 20 μg salmon sperm DNA (Invitrogen, Carlsbad, CA, USA) in a humid chamber at 45°C for 4 h. Slides were denatured with boiling millipore water, dehydrated with 95% ethanol at −20°C and stored in a desiccator. Genomic DNA was extracted (Puregene DNA isolation Kit, Gentra Systems, Inc., Minneapolis, MN, USA) from lymphoblastoid cell lines or from peripheral blood of the subjects and phenotypically normal male and female references. For two subjects (PSS01 and PSS04), genomic DNA was extracted from fixed cell pellets. Genomic DNA was digested with DpnII (New England Biolabs, Inc., Beverly, MA, USA), and the digestion was checked on an agarose gel. The DNA was purified with phenol/chloroform and chloroform. After precipitation (1:10 vol of NaCl 5 M and 1:1 vol of isopropanol), we measured the DNA concentration with a fluorometer (Amersham, Piscataway, NJ, USA) to adjust for an equal concentration between the two samples. We used a dye-reversal strategy on two separate microarrays in which 500 ng of both subject and reference DNAs were labeled (Bio Prime DNA labeling System, Invitrogen) with cyanine3 (Cy3) and cyanine5 (Cy5), respectively, as previously described.25, 27 The subject and reference DNA were cohybridized to one microarray and then oppositely labeled and cohybridized to a second microarray as previously described.25, 28 Shortly after the labeling, probes were purified with Microcon (Millipore, Billerica, MA, USA), and ∼500 ng of subjects' DNA, combined with an equal amount of opposite-sex control DNA, was coprecipitated with 50 μg of Cot1-DNA (Invitrogen) and hydrated with 15.5 μl ULTRAhyb (Ambion, Austin, TX, USA). The labeled genomic DNAs were denatured at 72°C for 5 min, preannealed immediately after at 37°C for 1 h, placed onto a microarray, and covered with a 22 × 22 mm2 coverslip. Hybridization was performed in an incubation chamber (Corning Incorporated Life Sciences, Acton, MA, USA) at 37°C with shaking for 14–16 h. Following the hybridization, the coverslips were removed with 1 × PBS and the microarrays were washed with 50% formamide+0.1% SDS at 45°C for 20 min and 1 × PBS for 20 min at room temperature in the dark. The microarrays were then rinsed with 0.2 × SSC and distilled water and immediately dried. For one subject (PSS13), microarray analysis was performed at Signature Genomic Laboratories (Spokane, WA, USA) using the SignatureChip™, which contains BACs covering the 11p11.2p12 region.
Microarray analysis
Images were acquired using a GenePix 4000B (Axon Instruments, Union City, CA, USA) dual-laser scanner, and individual spots were analyzed with GenePix Pro 4.0 imaging software (Axon Instruments). Two simultaneous scans of each array were obtained at wavelengths of 635 and 532 nm. The data were normalized using 15 overlapping clones from a published 1p36 contig.25, 29 These reference spots always contained DNA that was of the same complexity as the target spots to be analyzed and were known to be balanced (normal) in the test DNA. After normalization, an intensity ratio of ∼1.0 was seen for all 1p clones. Both ratios were averaged to eliminate erroneous data that could be interpreted incorrectly as a consequence of poorly printed spots, anomalous hybridization, or reactions of Cy3 and Cy5 with certain DNA sequences. Eight spots were averaged for each clone using Acuity 3.0 software (Axon Instruments). We set our threshold for copy-number gain and loss at 1.5 and 0.5, respectively.
Gene identification
The gene content of the 11p11.2 region between D11S1393 and D11S1385/D11S1319 was identified by comparative analysis of the annotated electronic-databases of the July 2003 draft of the human genome available on the three public genome browsers: the NCBI genome browser (http://www.ncbi.nlm.org), the UCSC genome browser (http://www.genome.ucsc.edu), and Ensembl (http://www.ensembl.org). As the number of hypothetical/predicted genes varied between databases, only the known genes and novel genes with functional identifiers found in at least two of the three databases were included in Table 3.
Results
A physical map of 11p11–p12 was constructed using BAC and cosmid clones (Figure 2). The sizes of the deleted regions (Mb from p terminus) were determined using FISH and microsatellite analysis. The deletion sizes were further delineated using array CGH (Figure 3). Deletion sizes are shown in Figure 2.
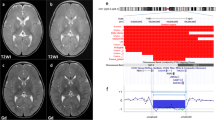
Plot of the hybridization results for (a) PSS07 and (b) mother of PSS07. In the plots of the hybridization results, the first 38 clones from the left are from 11p11.2–p13. To the right are 15 clones from 1p36 (Yu et al 25), 11 X-specific clones, and 5 Y-specific clones. The individual signal ratio (Cy3/Cy5) for each clone on the microarray is indicated (scale shown on the left). Two experiments were performed with dye reversal (shown as pink and blue dots, respectively). A comparison of the two experiments shows an excess of 11p material in the control as compared to the subject (a deviation with the ratio above 1.5, gray line) with a simultaneous loss of 11p material in the subject as compared to the control (a deviation with the ratio of less than 0.5, black line). A ratio of 1.0 indicates a normal DNA copy number as compared between subject and control. Note that in both (a) and (b), the subjects show loss of 11p material. (a) Subject PSS07 is a male, so he also shows a ‘loss’ of X material and a ‘gain’ of Y material as compared to the female control sample. (b) The mother of PSS07 also shows a loss of 11p material, although not as dramatic as her son because she is mosaic, and a ‘gain’ of the X chromosome material and a ‘loss’ of the Y chromosome material as compared to the normal male control sample.
Microsatellite analysis was performed on all subjects. Seven of the subjects (PSS02, PSS03, PSS04, PSS08, PSS10, PSS12, and PSS13) have paternally derived deletions, whereas three of the subjects (PSS01, PSS05, and PSS07) have deletions of maternal origin (data not shown).
Although molecular analysis of the deleted chromosome 11 in subject PSS01 was performed previously by Bartsch et al,1 we found two discrepancies between our analyses and those published. First, our analysis shows that the D11S1355 locus (43.6 Mb) is not deleted in this subject, and second, the D11S1344 locus (46.8 Mb), including clone RP11-58H7 (46.7–46.8 Mb), is deleted in this subject. These results are consistent with the other FISH results that showed a contiguous deletion in this subject.
All subjects with parietal foramina were deleted for ALX4, except PSS03. In this subject, the proximal breakpoint was located between markers D11S3805 (deleted) and D11S3975 (not deleted) – a 55 kb region, and more than 15 kb from the 3′ end of ALX4. Thus, no disruption of ALX4 could be identified. We have not excluded the possibility that this subject has both a deletion of 11p and mutation of some other gene causing the parietal foramina. However, it remains possible that ALX4 expression has been altered by a position effect (see Discussion).
PSS07 has a 6.9–7.9 Mb deletion of 11p – the largest deletion that does not extend into the WAGR syndrome region. This subject is hemizygous for a deletion of EXT2, but does not show exostoses at 14 months of age. Microsatellite analysis indicated that this subject had a maternally derived deletion of chromosome 11. The mother of PSS07, who does not have any features of PSS and was heterozygous for marker D11S554 in the deleted region,3 had three children with deletion. Thus, she was further evaluated for a chromosomal rearrangement involving this region. FISH analysis using the large-insert clones that were deleted in PSS07 revealed that the mother has a supernumerary marker chromosome, derived from 11p11.2, and deletion of this region on one chromosome 11.3, 30 About 76% of cells contained the marker chromosome and one deleted chromosome 11 (Figure 4), whereas 24% of cells demonstrated only a heterozygous deletion of chromosome 11. No normal cells were identified. Our microarray results show a difference in the ratio (1.4:0.6) between the mother's sample and a control for the clones that were deleted. FISH analysis revealed that the marker is analphoid because D11Z1 did not hybridize to the marker but did hybridize to both chromosomes 11. The marker contains RP11-937A2 and RP11-737O8, which were deleted in her child.30
Array CGH corroborated the deletion sizes delineated with FISH for most subjects. However, our analysis revealed a discrepancy in one subject. PSS03, who has the smallest deletion among our subjects, has a breakpoint that falls in a region covered by overlapping clones. The deletion, as determined by array CGH, differs by one adjacent clone from the FISH results. This discrepancy is likely a factor of the amount and type (unique or repetitive) of DNA retained near the deletion and less a factor of either FISH or array CGH being more accurate.25
The deletion sizes (Figure 2) were compared to the clinical features (Table 2) among the subjects. PSS08 has the largest deletion of 11p-14.2–17.6 Mb, which extends distal into the WAGR syndrome region and has features of both PSS and WAGR, including Wilms tumor. The full spectrum of PSS manifests in subjects with deletions spanning D11S1392 to D11S1385/D11S1319. Those subjects without mental retardation (PSS03, PSS05) were compared to the remaining subjects. This comparison revealed a minimal deletion region between D11S554 and D11S1385/ D11S1319 that is predicted to contain at least one gene for cognitive functioning, an aberration of which would lead to MR. A list of all 15 known genes in the full spectrum PSS critical region (D11S1393D11S1385/D11S1319) is given in Table 3.
Discussion
Construction of the 11p11.2 physical map
We constructed a physical map of 11p11–p12 that includes the EXT2 and ALX4 loci using large-insert clones identified through the Electronic-Database Information (UCSC Genome Browser on Human Nov. 2002 Freeze). We used this map to identify the breakpoint regions in 10 study subjects submitted to our study as having possible PSS. Physical mapping studies revealed that the interstitial deletions are of varying sizes (Figure 2). We determined the distal and proximal breakpoints to within ∼1 Mb in each subject. No clustering of breakpoints was observed, as the distal and proximal breakpoints were unique in the 10 subjects (Figure 2).
Parietal foramina in PSS03 may be caused by a position effect
Chromosome rearrangements can lead to alteration of the gene's genomic environment. This may be reflected in a change of expression, referred to as a position effect.31 Mutations 3′ from candidate genes are less likely to cause a position effect than mutations in the open reading frame or 5′ from the gene.31 However, sequences 3′ from many genes are important for the regulation of gene expression.31 Ideally, the absence of mutation in association with the chromosomal rearrangement should be demonstrated to strengthen the hypothesis that the rearrangement is solely responsible for the phenotype through a position effect.31 It is likely that the parietal foramina detected in PSS03 reflect a position effect from the deletion that occurs more than 15 kb from the 3′ end of ALX4. Combined with the previous report of a patient with parietal foramina and a 11p11.2–p14.2 deletion flanking but not including ALX4,7, 14 this suggests the presence of an enhancer either within the deleted region or in the 3′ region of the gene that is susceptible to position effect.
Phenotype/genotype correlation
Although developmental delay and mental retardation are found in most subjects with PSS, MR is not a feature in subjects PSS03 (de novo) or PSS05 (familial5). Based on the deletion sizes in these two families, the region 43.6–45.6 Mb from the short arm terminus, which spans from D11S1355 to D11S554, may be excluded as a region containing a dosage-sensitive gene(s) responsible for the mental retardation. Family 4, reported by Bartsch et al,1 and family I, reported by Wuyts et al,9 also did not have mental retardation. The deleted regions of these cases and the lack of mental retardation are consistent with our proposed exclusion region. Given this assumption, the complete overlapping region among the remaining study subjects with mental retardation is 44.6–46.7 Mb from the short arm terminus. We proposed that the 2.1 Mb region, which spans from D11S1393 to D11S1385/D11S1319, is the minimum critical region for the full PSS clinical spectrum, including mental retardation (Table 3). Given the overlapping and excluded regions, a gene necessary for cognitive development and/or cognitive function likely resides 45.6–46.7 Mb from the 11p terminus located between D11S554 and D11S1385/D11S1319. However, if subjects PSS03 and PSS05 are nonpenetrant for mental retardation, the region containing the gene is the minimal critical region between D11S1393 and D11S1385/D11S1319. This region partially overlaps with the two MR critical regions proposed by Wuyts et al.10 However, this group failed to include the family reported in Hall et al,5 included here as PSS05, who does not have MR. Taking into account all published data and the new cases presented here, we have proposed a single MR region.
There is no obvious parental origin effect for PSS because the phenotypes do not vary depending on whether the deletions have been derived from the maternal or paternal chromosomes 11. Further support that parental origin is not a factor comes from Hall et al,5 in which two children carry the same deletion as their father, which was likely derived from the paternal grandmother, and all three individuals have similar phenotypes.5
Parietal foramina and multiple exostoses are the primary characteristics of PSS. If present, parietal foramina can be identified at birth. However, the exostoses are usually not apparent until after 1 year of age, with the age for diagnosis usually by 3 years.32 The detection of exostoses is also dependent on the method of diagnosis and index of suspicion. A skeletal survey would detect an exostosis before it can be diagnosed by physical examination alone. Subject PSS04 did not have any exostoses at 1 year, 10 months of age, but upon re-examination at age 3 years, 10 months, three to four exostoses were found. A similar scenario was previously documented with exostoses not noted at 2 years, 3 months, but apparent at 4 years, 6 months.1, 6 Such age-of-onset variability complicates genotype/phenotype correlations.
The causative gene(s) for the craniofacial features of PSS has not been identified. Careful characterization of the craniofacial features of subjects with mutations in either ALX4 or EXT2 may help to clarify any causal relationship. It was proposed previously that the micropenis in males with PSS might be caused by haploinsufficiency of ALX4.17, 33 However, we suggest that other genes in the region could also be candidates for the urinary anomalies.
Major CNS malformations have been reported previously in PSS.10 Four of the 10 cases reported here showed thinning, hypoplasia or agenesis of the corpus callosum. Thus, this brain malformation should be added to the list of clinical features associated with this syndrome.
Summary
Including the current study, 29 subjects in 20 families with 11p11.2 proximal deletions have been reported. All cases that had the full PSS spectrum (subjects PSS01, PSS02, PSS04, PSS07, PSS08, PSS10, PSS12, and PSS13) had cytogenetically visible abnormalities of 11p. The only exceptions were that exostoses were not present in individuals PSS07, PSS08, and PSS13 by the age of 14 months, 22 months and 35 months respectively. The subjects without mental retardation – subjects PSS03 and PSS05 – had submicroscopic deletions detected by FISH analyses but not by routine chromosome analyses. Given this variation in deletion size, small interstitial deletions, especially those near the centromeres, can be particularly difficult to detect using routine chromosome banding methods. FISH analyses for EXT2 and ALX4 are helpful to diagnose individuals with some or all of the features of PSS suspected to have a deletion.
The present study also confirms the efficiency of array CGH. In this study, DNA from 10 subjects suspected of PSS was hybridized against our 11p11.2–p13 clones. In all but one of the subjects, array CGH was consistent with the FISH results. The one discrepancy was likely a consequence of hybridization to a small amount of retained DNA near the deletion and not a failure of the microarray to replicate the FISH analysis. Moreover, the array CGH required only two experiments for each patient (due to the dye-reversal experiment) compared to the numerous experiments needed for individual FISH experiments. For the present study, this translated into a few hours of experiments to delineate the deletion sizes with array CGH compared to many months to delineate the deletions using FISH.
In the last decade, PSS was added to the growing list of contiguous gene deletion syndromes.34 Many of these syndromes are characterized by consistent-sized deletions or duplications mediated through flanking low-copy repeat sequences.35, 36, 37 Although the deletion mechanism is not known in PSS, the highly variable breakpoints and range of deletion sizes suggest nonallelic homologous recombination through flanking repeats is likely not the mechanism through which these deletions occur.38 Delineation of the breakpoint sequences may elucidate sequences susceptible to chromosome rearrangements and the mechanism causing these interstitial deletions.
References
Bartsch O, Wuyts W, Van Hul W et al: Delineation of a contiguous gene syndrome with multiple exostoses, enlarged parietal foramina, craniofacial dysostosis, and mental retardation, caused by deletions in the short arm of chromosome 11. Am J Hum Genet 1996; 58: 734–742.
Potocki L, Shaffer LG : Interstitial deletion of 11(p11.2p12): a newly described contiguous gene deletion syndrome involving the gene for hereditary multiple exostoses (EXT2). Am J Med Genet 1996; 62: 319–325.
Chien WH, Sue WC, Kuo PL, Su MH, Lin CL : Potocki–Shaffer syndrome: report of one case. Acta Paediatr Taiwan 2003; 44: 242–245.
Gustavson KH, Anneren G, Wranne L : Two cases of 11p13 interstitial deletion and unusual clinical features. Clin Genet 1984; 26: 247–249.
Hall CR, Wu Y, Shaffer LG, Hecht JT : Familial case of Potocki–Shaffer syndrome associated with microdeletion of EXT2 and ALX4. Clin Genet 2001; 60: 356–359.
Lorenz P, Rupprecht E, Tellkamp H : An unusual type of acrocephalosyndactyly with bilateral parietooccipital ‘encephalocele,’ micropenis, and severe mental retardation. Am J Med Genet 1990; 36: 265–268.
McGaughran JM, Ward HB, Evans DG : WAGR syndrome and multiple exostoses in a patient with del(11)(p11.2p14.2). J Med Genet 1995; 32: 823–824.
Shaffer LG, Hecht JT, Ledbetter DH, Greenberg F : Familial interstitial deletion 11(p11.12p12) associated with parietal foramina, brachymicrocephaly, and mental retardation. Am J Med Genet 1993; 45: 581–583.
Wuyts W, Di Gennaro G, Bianco F et al: Molecular and clinical examination of an Italian DEFECT11 family. Eur J Hum Genet 1999; 7: 579–584.
Wuyts W, Waeber G, Meinecke P et al: Proximal 11p deletion syndrome (P11pDS): additional evaluation of the clinical and molecular aspects. Eur J Hum Genet 2004; 12: 400–406.
Yamamoto T, Akaboshi S, Ninomiya H, Nanba E : DEFECT 11 syndrome associated with agenesis of the corpus callosum. J Med Genet 2001; 38: E5.
Francke U, George DL, Brown MG, Riccardi VM : Gene dose effect: intraband mapping of the LDH A locus using cells from four individuals with different interstitial deletions of 11p. Cytogenet Cell Genet 1977; 19: 197–207.
Stickens D, Clines G, Burbee D et al: The EXT2 multiple exostoses gene defines a family of putative tumour suppressor genes. Nat Genet 1996; 14: 25–32.
Wuyts W, Van Hul W, Wauters J et al: Positional cloning of a gene involved in hereditary multiple exostoses. Hum Mol Genet 1996; 5: 1547–1557.
Wuyts W, Van Hul W : Molecular basis of multiple exostoses: mutations in the EXT1 and EXT2 genes. Hum Mutat 2000; 15: 220–227.
Mavrogiannis LA, Antonopoulou I, Baxova A et al: Haploinsufficiency of the human homeobox gene ALX4 causes skull ossification defects. Nat Genet 2001; 27: 17–18.
Wu YQ, Badano JL, McCaskill C, Vogel H, Potocki L, Shaffer LG : Haploinsufficiency of ALX4 as a potential cause of parietal foramina in the 11p11.2 contiguous gene-deletion syndrome. Am J Hum Genet 2000; 67: 1327–1332.
Riccardi VM, Sujansky E, Smith AC, Francke U : Chromosomal imbalance in the Aniridia–Wilms' tumor association: 11p interstitial deletion. Pediatrics 1978; 61: 604–610.
Ligon AH, Potocki L, Shaffer LG, Stickens D, Evans GA : Gene for multiple exostoses (EXT2) maps to 11(p11.2p12) and is deleted in patients with a contiguous gene syndrome. Am J Med Genet 1998; 75: 538–540.
Wu YQ, Heutink P, de Vries BB et al: Assignment of a second locus for multiple exostoses to the pericentromeric region of chromosome 11. Hum Mol Genet 1994; 3: 167–171.
Wuyts W, Ramlakhan S, Van Hul W et al: Refinement of the multiple exostoses locus (EXT2) to a 3-cM interval on chromosome 11. Am J Hum Genet 1995; 57: 382–387.
Drechsler M, Meijers-Heijboer EJ, Schneider S et al: Molecular analysis of aniridia patients for deletions involving the Wilms' tumor gene. Hum Genet 1994; 94: 331–338.
Ligon AH, Beaudet AL, Shaffer LG : Simultaneous, multilocus FISH analysis for detection of microdeletions in the diagnostic evaluation of developmental delay and mental retardation. Am J Hum Genet 1997; 61: 51–59.
Shaffer LG, Overhauser J, Jackson LG, Ledbetter DH : Genetic syndromes and uniparental disomy: a study of 16 cases of Brachmann-de Lange syndrome. Am J Med Genet 1993; 47: 383–386.
Yu W, Ballif BC, Kashork CD et al: Development of a comparative genomic hybridization microarray and demonstration of its utility with 25 well-characterized 1p36 deletions. Hum Mol Genet 2003; 12: 2145–2152.
Buckley PG, Mantripragada KK, Benetkiewicz M et al: A full-coverage, high-resolution human chromosome 22 genomic microarray for clinical and research applications. Hum Mol Genet 2002; 11: 3221–3229.
Hodgson G, Hager JH, Volik S et al: Genome scanning with array CGH delineates regional alterations in mouse islet carcinomas. Nat Genet 2001; 29: 459–464.
Wessendorf S, Fritz B, Wrobel G et al: Automated screening for genomic imbalances using matrix-based comparative genomic hybridization. Lab Invest 2002; 82: 47–60.
Heilstedt HA, Ballif BC, Howard LA et al: Physical map of 1p36, placement of breakpoints in monosomy 1p36, and clinical characterization of the syndrome. Am J Hum Genet 2003; 72: 1200–1212.
Chuang L, Wakui K, Sue WC, Su MH, Shaffer LG, Kuo PL : Interstitial deletion 11(p11.12p12) and neocentromere formation results in inherited Potocki–Shaffer syndrome. Am J Med Genet, in press.
Kleinjan DJ, van Heyningen V : Position effect in human genetic disease. Hum Mol Genet 1998; 7: 1611–1618.
Schmale GA, Conrad III EU, Raskind WH : The natural history of hereditary multiple exostoses. J Bone Joint Surg Am 1994; 76: 986–992.
Qu S, Tucker SC, Ehrlich JS et al: Mutations in mouse Aristaless-like4 cause Strong's luxoid polydactyly. Development 1998; 125: 2711–2721.
Gorlin RJ, Cohen MM, Levin LS : Syndromes of the Head and Neck. New York: Oxford University Press, 2001.
Shaffer LG, Lupski JR : Molecular mechanisms for constitutional chromosomal rearrangements in humans. Annu Rev Genet 2000; 34: 297–329.
Stankiewicz P, Lupski JR : Genome architecture, rearrangements and genomic disorders. Trends Genet 2002; 18: 74–82.
Stankiewicz P, Lupski JR : Molecular-evolutionary mechanisms for genomic disorders. Curr Opin Genet Dev 2002; 12: 312–319.
Inoue K, Osaka H, Thurston VC et al: Genomic rearrangements resulting in PLP1 deletion occur by nonhomologous end joining and cause different dysmyelinating phenotypes in males and females. Am J Hum Genet 2002; 71: 838–853.
Koch KA, Capitani G, Gruetter MG, Kirsch JF : The human cDNA for a homologue of the plant enzyme 1-aminocyclopropane-1-carboxylate synthase encodes a protein lacking that activity. Gene 2001; 272: 75–84.
McCormick C, Duncan G, Goutsos KT, Tufaro F : The putative tumor suppressors EXT1 and EXT2 form a stable complex that accumulates in the Golgi apparatus and catalyzes the synthesis of heparan sulfate. Proc Natl Acad Sci USA 2000; 97: 668–673.
Simmons AD, Musy MM, Lopes CS, Hwang LY, Yang YP, Lovett M : A direct interaction between EXT proteins and glycosyltransferases is defective in hereditary multiple exostoses. Hum Mol Genet 1999; 8: 2155–2164.
Raskind WH, Conrad EU, Chansky H, Matsushita M : Loss of heterozygosity in chondrosarcomas for markers linked to hereditary multiple exostoses loci on chromosomes 8 and 11. Am J Hum Genet 1995; 56: 1132–1139.
Dong JT, Lamb PW, Rinker-Schaeffer CW et al: KAI1, a metastasis suppressor gene for prostate cancer on human chromosome 11p11.2. Science 1995; 268: 884–886.
Mashimo T, Watabe M, Hirota S et al: The expression of the KAI1 gene, a tumor metastasis suppressor, is directly activated by p53. Proc Natl Acad Sci USA 1998; 95: 11307–11311.
Hemler ME : Specific tetraspanin functions. J Cell Biol 2001; 155: 1103–1107.
Liang XQ, Cao EH, Zhang Y, Qin JF : P53-induced gene 11 (PIG11) involved in arsenic trioxide-induced apoptosis in human gastric cancer MGC-803 cells. Oncol Rep 2003; 10: 1265–1269.
Ricketts SL, Carter JC, Coleman WB : Identification of three 11p11.2 candidate liver tumor suppressors through analysis of known human genes. Mol Carcinog 2003; 36: 90–99.
Jiang GL, Huang S : The yin-yang of PR-domain family genes in tumorigenesis. Histol Histopathol 2000; 15: 109–117.
Craxton M : Genomic analysis of synaptotagmin genes. Genomics 2001; 77: 43–49.
Fukuda M, Mikoshiba K : Characterization of KIAA1427 protein as an atypical synaptotagmin (Syt XIII). Biochem J 2001; 354: 249–257.
Jahn JE, Ricketts SL, Coleman WB : Identification of candidate liver tumor suppressor genes from human 11p11.2 by transcription mapping of microcell hybrid cell lines. Int J Oncol 2003; 22: 1303–1310.
Fukuta M, Inazawa J, Torii T, Tsuzuki K, Shimada E, Habuchi O : Molecular cloning and characterization of human keratan sulfate Gal-6-sulfotransferase. J Biol Chem 1997; 272: 32321–32328.
Hasegawa N, Torii T, Kato T et al: Decreased GlcNAc 6-O-sulfotransferase activity in the cornea with macular corneal dystrophy. Invest Ophthalmol Vis Sci 2000; 41: 3670–3677.
Ishida N, Kawakita M : Molecular physiology and pathology of the nucleotide sugar transporter family (SLC35). Pflugers Arch 2004; 447: 768–775.
Lubke T, Marquardt T, Etzioni A, Hartmann E, von Figura K, Korner C : Complementation cloning identifies CDG-IIc, a new type of congenital disorders of glycosylation, as a GDP-fucose transporter deficiency. Nat Genet 2001; 28: 73–76.
Luhn K, Wild MK, Eckhardt M, Gerardy-Schahn R, Vestweber D : The gene defective in leukocyte adhesion deficiency II encodes a putative GDP-fucose transporter. Nat Genet 2001; 28: 69–72.
Griffin Jr EA, Staknis D, Weitz CJ : Light-independent role of CRY1 and CRY2 in the mammalian circadian clock. Science 1999; 286: 768–771.
Kume K, Zylka MJ, Sriram S et al: mCRY1 and mCRY2 are essential components of the negative limb of the circadian clock feedback loop. Cell 1999; 98: 193–205.
Bonny C, Oberson A, Steinmann M, Schorderet DF, Nicod P, Waeber G : IB1 reduces cytokine-induced apoptosis of insulin-secreting cells. J Biol Chem 2000; 275: 16466–16472.
Waeber G, Delplanque J, Bonny C et al: The gene MAPK8IP1, encoding islet-brain-1, is a candidate for type 2 diabetes. Nat Genet 2000; 24: 291–295.
Thompson NA, Haefliger JA, Senn A et al: Islet-brain1/JNK-interacting protein-1 is required for early embryogenesis in mice. J Biol Chem 2001; 276: 27745–27748.
Honsho M, Hiroshige T, Fujiki Y : The membrane biogenesis peroxin Pex16p. Topogenesis and functional roles in peroxisomal membrane assembly. J Biol Chem 2002; 277: 44513–44524.
Shimozawa N, Nagase T, Takemoto Y et al: A novel aberrant splicing mutation of the PEX16 gene in two patients with Zellweger syndrome. Biochem Biophys Res Commun 2002; 292: 109–112.
South ST, Gould SJ : Peroxisome synthesis in the absence of preexisting peroxisomes. J Cell Biol 1999; 144: 255–266.
Freeze HH : Human disorders in N-glycosylation and animal models. Biochim Biophys Acta 2002; 1573: 388–393.
Miller BS, Freeze HH : New disorders in carbohydrate metabolism: congenital disorders of glycosylation and their impact on the endocrine system. Rev Endocr Metab Disord 2003; 4: 103–113.
Hakimi MA, Bochar DA, Chenoweth J, Lane WS, Mandel G, Shiekhattar R : A core-BRAF35 complex containing histone deacetylase mediates repression of neuronal-specific genes. Proc Natl Acad Sci USA 2002; 99: 7420–7425.
Acknowledgements
We thank the subjects and families for their participation in this study and Marianna Horz (Texas Children's Hospital), C McCaskill, C Knox-Du Bois, and CD Kashork (Baylor College of Medicine) for their technical assistance and A Theisen (Washington State University) for his critique and editing of this manuscript. This study was supported in part by grants from the National Institutes of Health and the Texas Children's Hospital General Clinical Research Center (M01-RR00188).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Wakui, K., Gregato, G., Ballif, B. et al. Construction of a natural panel of 11p11.2 deletions and further delineation of the critical region involved in Potocki–Shaffer syndrome. Eur J Hum Genet 13, 528–540 (2005). https://doi.org/10.1038/sj.ejhg.5201366
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.ejhg.5201366
Keywords
This article is cited by
-
11p11.12p12 duplication in a family with intellectual disability and craniofacial anomalies
BMC Medical Genomics (2021)
-
De novo truncating variants in PHF21A cause intellectual disability and craniofacial anomalies
European Journal of Human Genetics (2019)
-
Enlarged parietal foramina caused by mutations in the homeobox genes ALX4 and MSX2: from genotype to phenotype
European Journal of Human Genetics (2006)