Abstract
The 3243A>G mutation is one of the most frequently observed mutations of mitochondrial DNA (mtDNA), and is associated with numerous clinical presentations including mitochondrial myopathy, encephalopathy, lactic acidosis and stroke-like episodes (MELAS), progressive external ophthalmoplegia (PEO) and diabetes and deafness. The routine diagnosis of the 3243A>G mutation in blood is difficult as mutation levels are known to decrease in this tissue over time, while in some patients it may be absent. We have directly compared the levels of the 3243A>G mutation in skeletal muscle, blood and urinary epithelial cells in 18 patients and observed a striking correlation between the mutation load in postmitotic muscle and urinary epithelium, a mitotic tissue. These data strongly support the use of urinary epithelial cells as the tissue of choice in the noninvasive diagnosis of the 3243A>G mutation.
Similar content being viewed by others
Introduction
The 3243A>G mutation in the tRNALeu(UUR) gene of mitochondrial DNA (mtDNA) is associated with a number of different clinical phenotypes. It was first described in patients with the syndrome of mitochondrial myopathy, encephalopathy, lactic acidosis and stroke-like episodes (MELAS), characterised by seizures, episodes of vomiting, migraine and recurrent stroke-like episodes and is reported in more than 80% MELAS cases.1 It is also found in families with progressive external ophthalmoplegia (PEO) or maternally inherited diabetes mellitus, with or without deafness,2 and is arguably the most common heteroplasmic mtDNA point mutation, with a prevalence of ∼1:15 000 in certain populations.3 The diversity of clinical phenotype is not fully understood, but is thought to be related to the level and tissue distribution of mutation load since a clear correlation exists between certain clinical features and the level of 3243A>G mutation in skeletal muscle.4
Screening for the 3243A>G mutation is not only part of the routine diagnostic workup for patients with suspected mtDNA disease,2 but it also enters the differential diagnosis of patients with diabetes and deafness, young stroke and unexplained cardiomyopathy. Determining the mutation load in asymptomatic and presymptomatic relatives of affected individuals contributes informative data on those at risk of developing symptoms and is a useful guide for genetic counselling. Although the noninvasive genetic testing of blood samples is common for some mtDNA disorders,5 patients with the 3243A>G mutation have consistently higher mutation levels in postmitotic muscle than blood,6 introducing the potential for reporting false-negative results.7 With longitudinal studies showing the level of 3243A>G mutation to decrease in patient's blood over time,8, 9 the analysis of 3243A>G mutation load in blood is probably a poor indicator of the overall mutation load in affected tissues and therefore not a good choice for noninvasive diagnostic testing.10
This has prompted investigators to explore other tissues as a source of DNA for routine screening of the 3243A>G mutation, including epithelial cells and hair shafts, with many investigators reporting higher mutation levels in these various tissues than those expressed in circulating lymphocytes.11, 12, 13 Interestingly, Dubeau et al commented that mutation levels in urinary epithelial cells were consistently higher than those observed in blood and buccal cells from four individuals with this mutation.14 Here, we present data that show the level of 3243A>G mutation in urinary epithelium to be a useful indicator of the level observed in skeletal muscle, a finding which we believe has important implications for both clinical practice and diagnosis.
Patients and methods
Patients
We studied 18 patients with the 3243A>G mutation, all of whom had been referred for investigation at the Department of Neurology, University of Newcastle upon Tyne, UK. Every individual had previously consented to these investigations, and in each case, the initial molecular diagnosis of the 3243A>G mutation had been confirmed in skeletal muscle DNA following needle muscle biopsy.
Molecular genetic analyses
Total DNA was extracted from skeletal muscle and 4 ml EDTA-blood using standard Proteinase-K/SDS digestion protocols followed by phenol/chloroform extraction. Urinary epithelial cells were pelleted from 20 ml urine by centrifugation, and total DNA extracted as described above. Typical DNA yields from this volume of urine were between 0.4–1.0 μg total DNA.
The level of the 3243A>G mutation was determined in each sample by last hot cycle PCR-RFLP analysis, a technique previously shown to be sensitive down to a level of 0.5% mutant mtDNA.15 Briefly, a 154-bp fragment of mtDNA encompassing the mutation site within the tRNALeu(UUR) gene was amplified (30 cycles) using the forward primer L3200 (nucleotides 3200–3218) and the reverse primer H3353 (nucleotides 3353–3334). Following the addition of 30 pmol of each primer, 5 μCi [α-32P]dCTP (3000Ci/mmol) and 1U of Taq polymerase, PCR reactions were subjected to an additional cycle of amplification. Labelled products were precipitated and digested at 37°C with 7.5 U Hae III (Roche Biochemicals). Restriction fragments were separated through a 12% nondenaturing polyacrylamide gel, dried onto a support and exposed to a PhosphorImager cassette. The level of mtDNA heteroplasmy was quantified using ImageQuant software (Molecular Dynamics). A single Hae III recognition site in the wild-type product generates fragments of 117, and 37 bp, while the 3243A>G transition generates an additional recognition site cleaving the 117 bp fragment into two smaller products of 72 and 45 bp.
Results
We determined the level of the 3243A>G mutation in skeletal muscle, blood and urinary epithelial cells from 18 patients, permitting a direct comparison of mutation load between these three tissues. Our findings are shown in Table 1. In all patients, the level of 3243A>G mutation in muscle was higher than that observed in blood, and with the exception of one individual (patient 7), the mutation load in urinary epithelial cells was always higher than the level in blood (Table 1). Strikingly, we observed a close correlation between the levels of 3243A>G mutation in muscle and urinary epithelial cells for many of the patients (Table1 and Figure 1; Pearson's correlation coefficient, r=0.40, P=0.045). Only three individuals (patients 5, 7 and 17) showed poor correlation between the observed mutation loads in these two tissues (Table 1), although their clinical manifestations reflect the 3243A>G mutation load in muscle as has been previously reported.4 Patients 5 and 7 presented with ataxia and encephalopathy, respectively, while patient 17 has diabetes and deafness.
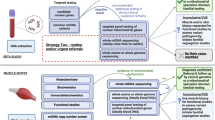
Molecular analysis of the 3243A>G mutation. (a) Quantitation of the relative amounts of mutant and wild-type mtDNA in different tissues from patient 12, highlighting the observed variation in intertissue distribution of the 3243A>G mutation. U, uncut sample; C, control; M, skeletal muscle; B, blood; Ur, urinary epithelial cells; (b) Plot of % 3243A>G mutation level in muscle versus urinary epithelial cells for the 18 patients.
Discussion
With a reported frequency of 10.2 index cases per 100 000 in some populations,3 methodologies that can accurately diagnose the 3243A>G mutation are an important component of any laboratory undertaking genetic testing of patients suspected of having a mitochondrial DNA disorder. Although the noninvasive genetic testing of blood samples is advocated and continues to be practiced,5 a greater understanding of basic mitochondrial genetics through the study of patients has shown us that there are inherent problems in studying pathogenic mtDNA point mutations in this tissue. Many mtDNA mutations are restricted to skeletal muscle, which is commonly the clinically affected tissue. Furthermore, in addition to 3243A>G mutation loads decreasing in blood over time,8, 9 previous investigations have shown that analysis of this tissue is not as helpful in predicting the prognosis of a patient's disease, with no obvious correlation between mutant load and patient's clinical features.4 The finding of lower mutation levels in blood is thought to be due to the rapidly dividing nature of these cells. High levels of the 3243A>G mutation cause a severe respiratory chain defect, and presumably, preferential selection of lymphocytes with more wild-type genomes. This results in lower levels of the point mutation with age and thus difficulties with diagnosis.
It has been previously shown in some patients with the 3243A>G mutation that the proportion of mutant mtDNA is higher in urinary epithelial cells, another mitotically active tissue, than blood.14 This prompted us to explore the relevance of these cells in the laboratory diagnosis of 3243A>G more fully by directly comparing 3243A>G mutation levels in three tissues (skeletal muscle, blood and urinary epithelial cells) from 18 of our patients. In keeping with other laboratories, we find that the 3243A>G mutation level in urine is consistently higher than that seen in blood, and typically reflects the mutation load present in skeletal muscle (Sara Shanske, personal communication). As this measure is a proven means of predicting clinical outcome, we would advocate that urinary epithelial cells should be the tissue of choice in the noninvasive diagnosis of the 3243A>G mutation.
The reason for these apparent high mutant loads in these cells is more difficult to explain. Embryologically, the ectodermal germ layer gives rise to the CNS, and the mesodermal layer to muscle and the vascular system. Muscle and the CNS, both postmitotic, are common affected tissues in patients with the 3243A>G mutation. The mesodermal layer also gives rise to the urogenital system with the exception of the bladder, and therefore the urinary epithelia, which are derived from the endodermal germ layer. Given that each layer gives rise to a tissue that can demonstrate high levels of this mutation (CNS, muscle, urinary epithelia), it would indicate that the initial mutation level throughout the embryo is equal in all layers, at odds with this segregation occurring during differentiation of the germ layers.16 The demonstration of little variation in heteroplasmy in different foetal tissues with the 3243A>G mutation further supports this.17 There is therefore no evidence that the origin of the tissues causes the similarity in the mutation levels that we observed. Moreover, unlike the scenario in blood, it appears that selection against cells harbouring the mutation is not occurring as seen in other mitotic tissues. This may be due to differences in respiratory demand, permitting the mutation to accumulate, or at the level of selection. We have recently shown that human colonic crypt cells, another epithelial cell, can accumulate pathogenic mtDNA mutations to very high levels,18 a phenomenon that we believe can be explained by virtue of these cells being short lived, and without significant selection against harmful mutations, they accumulate. Interestingly, a similar observation has also been made in hair follicles from patients with the 3243A>G mutation.12
In conclusion, the correlation we observe between the levels of 3243A>G mutation in urinary epithelia and skeletal muscle is fascinating, and while further studies are required to determine whether this is true of other pathogenic mtDNA mutations, we would recommend using urinary epithelial cells in routine screening for the 3243A>G mutation. Although the molecular genetic analysis of skeletal muscle is widely acknowledged to be the ‘gold standard’ in the investigation of patients with suspected mtDNA disease, the screening of 3243A>G in urine has distinct advantages over this tissue and is unlikely to yield the false negative results that are occasionally seen in blood.7 Muscle biopsy is an expensive, inconvenient procedure, while a 20 ml urine sample will contain enough cells to extract an adequate amount of DNA for testing, be obtained in the clinic and forwarded to the specialist diagnostic centre without the need for freezing, making it the most convenient sample to analyse. With mtDNA mutations being increasingly recognised in the paediatric population,19, 20 the noninvasive nature of genetic testing in urine offers a most attractive alternative to muscle biopsy.
References
Goto Y, Nonaka I, Horai S : A mutation in the tRNALeu(UUR) gene associated with the MELAS subgroup of mitochondrial encephalomyopathies. Nature 1990; 348: 651–653.
McFarland R, Taylor RW, Turnbull DM : The neurology of mitochondrial DNA disease. Lancet Neurol 2002; 1: 345–351.
Majamaa K, Moilanen JS, Uimonen S et al: Epidemiology of A3243G, the mutation for mitochondrial encephalomyopathy, lactic acidosis, and strokelike episodes: prevalence of the mutation in an adult population. Am J Hum Genet 1998; 63: 447–454.
Chinnery PF, Howell N, Lightowlers RN, Turnbull DM : Molecular pathology of MELAS and MERRF. The relationship between mutation load and clinical phenotypes. Brain 1997; 120: 1713–1721.
Hammans SR, Sweeney MG, Brockington M, Morgan-Hughes JA, Harding AE : Mitochondrial encephalopathies: molecular genetic diagnosis from blood samples. Lancet 1991; 337: 1311–1313.
Ciafaloni E, Ricci E, Shanske S et al: MELAS: clinical features, biochemistry, and molecular genetics. Ann Neurol 1992; 31: 391–398.
Chinnery PF, Turnbull DM, Walls TJ, Reading PJ : Recurrent strokes in a 34-year-old man. Lancet 1997; 350: 560.
t'Hart LM, Jansen JJ, Lemkes HH, de Knijff P, Maassen JA : Heteroplasmy levels of a mitochondrial gene mutation associated with diabetes mellitus decrease in leucocyte DNA upon aging. Hum Mutat 1996; 7: 193–197.
Rahman S, Poulton J, Marchington D, Suomalainen A : Decrease of 3243 A>G mtDNA mutation from blood in MELAS syndrome: a longitudinal study. Am J Hum Genet 2001; 68: 238–240.
Chinnery PF, Howell N, Lightowlers RN, Turnbull DM : MELAS and MERRF. The relationship between maternal mutation load and the frequency of clinically affected offspring. Brain 1998; 121: 1889–1894.
Kotsimbos N, Jean-Francois MJ, Huizing M et al: Rapid and noninvasive screening of patients with mitochondrial myopathy. Hum Mutat 1994; 4: 132–135.
Sue CM, Quigley A, Katsabanis S et al: Detection of MELAS A3243G point mutation in muscle, blood and hair follicles. J Neurol Sci 1998; 161: 36–39.
Chinnery PF, Zwijnenburg PJ, Walker M et al: Nonrandom tissue distribution of mutant mtDNA. Am J Med Genet 1999; 85: 498–501.
Dubeau F, De Stefano N, Zifkin BG, Arnold DL, Shoubridge EA : Oxidative phosphorylation defect in the brains of carriers of the tRNAleu(UUR) A3243G mutation in a MELAS pedigree. Ann Neurol 2000; 47: 179–185.
McFarland R, Schaefer AM, Gardner JL et al: Familial mitochondrial myopathy: new insights into the T14709C mitochondrial tRNA mutation. Ann Neurol 2004; 55: 478–484.
Macmillan C, Lach B, Shoubridge EA : Variable distribution of mutant mitochondrial DNAs (tRNA(Leu[3243])) in tissues of symptomatic relatives with MELAS: the role of mitotic segregation. Neurology 1993; 43: 1586–1590.
Matthews PM, Hopkin J, Brown RM, Stephenson JB, Hilton-Jones D, Brown GK : Comparison of the relative levels of the 3243 (A → G) mtDNA mutation in heteroplasmic adult and fetal tissues. J Med Genet 1994; 31: 41–44.
Taylor RW, Barron MJ, Borthwick GM et al: Mitochondrial DNA mutations in human colonic crypt stem cells. J Clin Invest 2003; 112: 1351–1360.
Chol M, Lebon S, Benit P et al: The mitochondrial DNA G13513A MELAS mutation in the NADH dehydrogenase 5 gene is a frequent cause of Leigh-like syndrome with isolated complex I deficiency. J Med Genet 2003; 40: 188–191.
McFarland R, Kirby DM, Fowler KJ et al: De novo mutations in the mitochondrial ND3 gene as a cause of infantile mitochondrial encephalopathy and complex I deficiency. Ann Neurol 2004; 55: 58–64.
Acknowledgements
MTM was funded by the William Leech Foundation, University of Newcastle upon Tyne. This study was supported by grants from the Wellcome Trust, the Muscular Dystrophy Campaign and the Newcastle upon Tyne NHS Hospitals Trust.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
McDonnell, M., Schaefer, A., Blakely, E. et al. Noninvasive diagnosis of the 3243A>G mitochondrial DNA mutation using urinary epithelial cells. Eur J Hum Genet 12, 778–781 (2004). https://doi.org/10.1038/sj.ejhg.5201216
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.ejhg.5201216
Keywords
This article is cited by
-
Genetic testing for mitochondrial disease: the United Kingdom best practice guidelines
European Journal of Human Genetics (2023)
-
Mutations in mitochondrially encoded complex I enzyme as the second common cause in a cohort of Chinese patients with mitochondrial myopathy, encephalopathy, lactic acidosis and stroke-like episodes
Journal of Human Genetics (2011)
-
Maternally inherited mitochondrial DNA disease in consanguineous families
European Journal of Human Genetics (2011)
-
A Diagnostic Algorithm for Metabolic Myopathies
Current Neurology and Neuroscience Reports (2010)