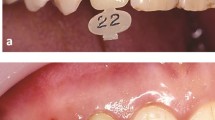
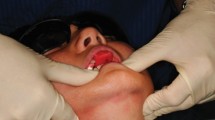
Key Points
In this part, we will discuss
-
Rest seats
-
Guide surfaces
-
Correction of unfavourable survey lines
-
Creating retentive areas
Abstract
This final article in the series describes the modification of teeth to improve their shape for the support and retention of RPDs.
Similar content being viewed by others
Main
New publications: All the parts which comprise this series (which will be published in the BDJ) have been included (together with a number of unpublished parts) in the book A Clinical Guide to Removable Partial Dentures (ISBN 0-904588-599) and A Clinical Guide to Removable Partial Denture Design (ISBN 0-904588-637). Available from Macmillan on 01256 302699
Preparation may be undertaken for a number of reasons.
-
Provide rest seats.
-
Establish guide surfaces.
-
Modify unfavourable survey lines.
-
Create retentive areas.

In addition, occlusal adjustment may also form an important part of tooth preparation (see Figs 7.14, 7.15 and 7.17 of A Clinical Guide to Removable Partial Dentures).
Where a clasp is to extend buccally from an occlusal rest and there is no space occlusally for it to do so, the preparation must be extended as a channel on to the buccal surface of the tooth. In some circumstances it may also be necessary to reduce and recontour the cusp of the tooth in the opposing arch.
Tooth preparation for RPDs should be planned on articulated study casts after they have been surveyed and a denture design produced.
Shaping of enamel surfaces for any of the reasons listed is usually undertaken with rotary diamond instruments of appropriate size and shape. The resulting roughened enamel surface must always be smoothed and polished. Special burs, stones and abrasive-impregnated rubber wheels and points are available for this purpose. Subsequent application of a topical fluoride varnish, to reduce the chance of carious attack of the modified enamel surfaces, should be carried out routinely.
Rest seats
Rest seats may need to be prepared to:
-
produce a favourable tooth surface for support (Fig. 1);
Figure 1: Rest seats A rest placed on an inclined surface will tend to slide down the tooth under the influence of occlusal loads (1). The resulting horizontal force may cause a limited labial migration of the tooth with further loss of support for the denture.
The provision of a rest seat (2) will result in a vertical loading of the tooth, more efficient support and absence of tooth movement.
-
prevent interference with the occlusion (Fig. 2);
Figure 2: Rest seats An occlusal rest placed at the arrow in (1) would create a premature occlusal contact (2), unless a rest seat was prepared to make room for it (3).
Space for the rest should not usually be created by grinding the mandibular buccal cusp as this is a supporting cusp contributing to the stability of the intercuspal position.
-
reduce the prominence of a rest (Fig. 3).Fig. 4, Fig. 5, Fig. 6, Fig. 7, Fig. 8
Figure 3: Rest seats In addition, a rest placed on an unprepared tooth surface (1) will stand proud of that surface and may tend to collect food particles and possibly create difficulties in tolerating the denture.
The preparation of a rest seat (2) will allow the rest to be shaped so that it blends into the contour of the tooth, is less apparent to the patient and also harmonises with the occlusal relationship.
Figure 4 Rest seats on posterior teeth
The design of rest seats on posterior teeth is shown in:
1. occlusal view;
2. mesiodistal view;
3. proximal view.
It will be seen that preparation involves a reduction in the height of the marginal ridge in order to ensure an adequate bulk of material linking the occlusal rest to the minor connector.
Rest seats on posterior teeth should normally be saucer-shaped so that a certain amount of horizontal movement of the rest within the seat is possible. Dissipation of some of the energy developed by occlusal forces acting on the denture can then occur.
Figure 5: Rest seats on posterior teeth Figure 6: Rest seats on posterior teeth The rest should be at least 1 mm thick for adequate strength. To check that sufficient enamel has been removed during rest seat preparation to accommodate this thickness of metal, the patient should be asked to occlude on a strip of softened pink wax. The thickness of wax in the region of the rest seat will indicate if adequate clearance has been achieved.
Figure 8: Rest seats on posterior teeth Where a clasp is to extend buccally from an occlusal rest and there is no space occlusally for it to do so, the preparation must be extended as a channel on to the buccal surface of the tooth. In some circumstances it may also be necessary to reduce and recontour the cusp of the tooth in the opposing arch.
Rest seats on anterior teeth
The design of rest seats on anterior teeth is shown in Figs 9, 10, 11 to 12.
The lingual surface of a mandibular anterior tooth is usually too vertical and the cingulum too poorly developed to allow preparation of a cingulum rest seat without penetration of the enamel. Incisal rest seats therefore have a wider application in this situation, in spite of their inferior appearance. The preparation is shown from the labial (1), lingual (2) and proximal (3) viewpoints.
The advantages of guide surfaces
It is widely accepted on the basis of clinical observation that the use of guide surfaces confers a number of benefits in RPD construction. The benefits include the following:
-
Increased stability.
-
Reciprocation.
-
Prevention of clasp deformation.
-
Improved appearance.
Guide surfaces
Fig. 13, Fig. 14, Fig. 15, Fig. 16, Fig. 17
A guide surface* allows a reciprocating component to maintain continuous contact with a tooth as the denture is displaced occlusally. The retentive arm of the clasp is thus forced to flex as it moves up the tooth. It is this elastic deformation of the clasp that creates the retentive force (Chapter 7, A Clinical Guide to Removable Partial Denture Design).
The preparation of guide surfaces
Guide surfaces are usually prepared, somewhat imprecisely, by eye. The position in which the handpiece must be held to prepare the required guide surfaces, so that they are all parallel to each other and to the path of insertion, should be established on the study cast.
As a check on the accuracy of the prepared guide surface, an alginate impression may be taken to produce a second study cast. This cast can then be placed on a surveyor and the parallelism of the guide surfaces checked using the analysing rod. If correction is found to be needed, further intra-oral adjustment can be undertaken.
A more precise approach to the preparation of guide surfaces can be achieved by the use of jigs constructed on a prepared study cast and then transferred to the mouth, either to control the positioning of the handpiece or to check on the location and amount of enamel reduction.Fig. 18, Fig. 19, Fig. 20
A guide surface should be produced by removing a minimal and fairly uniform thickness of enamel, usually not more than 0.5 mm, from around the appropriate part of the circumference of the tooth (green area).
The surfaces should not be prepared as a flat plane, as would tend to occur if an abrasive disc were used (red area). This is unnecessarily destructive and may even lead to penetration into dentine, thus making a restoration obligatory.
The required location of a guide surface will be dependent on its function. The red guide surfaces on the proximal surfaces of the abutment teeth facing the edentulous space will be needed to control the path of insertion of the saddle. The green guide surfaces on the tooth surfaces diametrically opposite the retentive portion of the clasp will be needed for the latter's reciprocation.
Unfavourable survey lines
Fig. 20, Fig. 21, Fig. 22, Fig. 23
A high survey line on a tooth that is to be clasped is unfavourable because it requires the clasp to be placed too close to the occlusal surface and may create an occlusal interference (arrows).Even if an occlusal interference is not present, a high clasp arm is more noticeable to the patient and may interfere with mastication.
A high survey line on a tooth that is to be clasped is unfavourable because it requires the clasp to be placed too close to the occlusal surface and may create an occlusal interference (arrows).Even if an occlusal interference is not present, a high clasp arm is more noticeable to the patient and may interfere with mastication.
(1) A high survey line may also result in deformation of the clasp because, on insertion, the clasp is prevented from moving down the tooth by contact with the occlusal surface. If the patient persists in trying to seat the denture, the clasp is bent upwards rather than flexed outwards.
(2) Shaping the enamel to lower the survey line will allow the clasp to be positioned further gingivally and it also provides a 'lead-in' during insertion, causing the clasp to flex outwards over the survey line as planned.
Retentive areas
Retentive areas can be created by grinding enamel. However, the enamel is relatively thin in the gingival third of the crown where the retentive tip of the clasp would normally be placed, so the amount of undercut that can be achieved by these means without penetrating the enamel is strictly limited. It is usually better to establish improved contours for retention by restorative methods as outlined in Chapter 14 of A Clinical Guide to Removable Partial Dentures.
Undercut areas can also be created by the use of acid-etch composite restorations.
A broad area of attachment of the restoration to the enamel is desirable as this will reduce the chance of the restoration being displaced and will produce a contour more suitable for clasping.
The early composites were not suitable for this purpose as they contained coarse filler particles that caused marked abrasion of the clasp arm with consequent weakening of the clasp and loss of retention. However, the use of modern ultrafine and hybrid composites results in minimal mutual abrasion of composite and clasp so that the technique is a durable, effective and conservative method of enhancing RPD retention.
Author information
Authors and Affiliations
Corresponding author
Additional information
Refereed paper
Rights and permissions
About this article
Cite this article
Davenport, J., Basker, R., Heath, J. et al. Tooth preparation. Br Dent J 190, 288–294 (2001). https://doi.org/10.1038/sj.bdj.4800954
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.bdj.4800954
This article is cited by
-
Unilateral removable partial dentures
British Dental Journal (2017)
-
Analysis of the compressive strain below the removable and fixed prosthesis in the posterior mandible using a digital image correlation method
Biomechanics and Modeling in Mechanobiology (2012)