Abstract
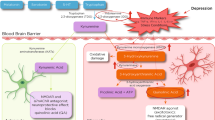
Studies show that administration of interferon (IFN)-α causes a significant increase in depressive symptoms. The enzyme indoleamine 2,3-dioxygenase (IDO), which converts tryptophan (TRP) into kynurenine (KYN) and which is stimulated by proinflammatory cytokines, may be implicated in the development of IFN-α-induced depressive symptoms, first by decreasing the TRP availability to the brain and second by the induction of the KYN pathway resulting in the production of neurotoxic metabolites. Sixteen patients with chronic hepatitis C, free of psychiatric disorders and eligible for IFN-α treatment, were recruited. Depressive symptoms were measured using the Montgomery Asberg Depression Rating Scale (MADRS). Measurements of TRP, amino acids competing with TRP for entrance through the blood–brain barrier, KYN and kynurenic acid (KA), a neuroprotective metabolite, were performed using high-performance liquid chromatography. All assessments were carried out at baseline and 1, 2, 4, 8, 12 and 24 weeks after treatment was initiated. The MADRS score significantly increased during IFN-α treatment as did the KYN/TRP ratio, reflecting IDO activity, and the KYN/KA ratio, reflecting the neurotoxic challenge. The TRP/CAA (competing amino acids) ratio, reflecting TRP availability to the brain, did not significantly change during treatment. Total MADRS score was significantly associated over time with the KYN/KA ratio, but not with the TRP/CAA ratio. Although no support was found that IDO decreases TRP availability to the brain, this study does support a role for IDO activity in the pathophysiology of IFN-α-induced depressive symptoms, through its induction of neurotoxic KYN metabolites.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Dieperink E, Ho SB, Thuras P, Willenbring ML . A prospective study of neuropsychiatric symptoms associated with interferon-alpha-2b and ribavirin therapy for patients with chronic hepatitis C. Psychosomatics 2003; 44: 104–112.
Hauser P, Khosla J, Aurora H, Laurin J, Kling MA, Hill J et al. A prospective study of the incidence and open-label treatment of interferon-induced major depressive disorder in patients with hepatitis C. Mol Psychiatry 2002; 7: 942–947.
Musselman DL, Lawson DH, Gumnick JF, Manatunga AK, Penna S, Goodkin RS et al. Paroxetine for the prevention of depression induced by high-dose interferon alfa. N Engl J Med 2001; 344: 961–966.
Bonaccorso S, Marino V, Puzella A, Pasquini M, Biondi M, Artini M et al. Increased depressive ratings in patients with hepatitis C receiving interferon-alpha-based immunotherapy are related to interferon-alpha- induced changes in the serotonergic system. J Clin Psychopharmacol 2002; 22: 86–90.
Staley JK, Malison RT, Innis RB . Imaging of the serotonergic system: interactions of neuroanatomical and functional abnormalities of depression. Biol Psychiatry 1998; 44: 534–549.
Graeff FG, Guimaraes FS, De Andrade TG, Deakin JF . Role of 5-HT in stress, anxiety, and depression. Pharmacol Biochem Behav 1996; 54: 129–141.
Maes M, Meltzer H . The serotonin hypothesis of major depression. In: Bloom F, Kupfer D, (eds) Psychopharmacology. Raven Press: New York, 1995 pp 933–944.
Salomon RM, Kennedy JS, Johnson BW, Schmidt DE, Kwentus J, Gwirtsman HE et al. Association of a critical CSF tryptophan threshold level with depressive relapse. Neuropsychopharmacology 2003; 28: 956–960.
Young SN, Leyton M . The role of serotonin in human mood and social interaction. Insight from altered tryptophan levels. Pharmacol Biochem Behav 2002; 71: 857–865.
Booij L, Van der Does W, Benkelfat C, Bremner JD, Cowen PJ, Fava M et al. Predictors of mood response to acute tryptophan depletion. A reanalysis. Neuropsychopharmacology 2002; 27: 852–861.
Maes M . Evidence for an immune response in major depression: a review and hypothesis. Prog Neuropsychopharmacol Biol Psychiatry 1995; 19: 11–38.
Sluzewska A, Rybakowski J, Bosmans E, Sobieska M, Berghmans R, Maes M et al. Indicators of immune activation in major depression. Psychiatry Res 1996; 64: 161–167.
Mikova O, Yakimova R, Bosmans E, Kenis G, Maes M . Increased serum tumor necrosis factor alpha concentrations in major depression and multiple sclerosis. Eur Neuropsychopharmacol 2001; 11: 203–208.
Zorrilla EP, Luborsky L, McKay JR, Rosenthal R, Houldin A, Tax A et al. The relationship of depression and stressors to immunological assays: a meta-analytic review. Brain Behav Immun 2001; 15: 199–226.
Wirleitner B, Neurauter G, Schrocksnadel K, Frick B, Fuchs D . Interferon-gamma-induced conversion of tryptophan: immunologic and neuropsychiatric aspects. Curr Med Chem 2003; 10: 1581–1591.
Dale WE, Dang Y, Brown OR . Tryptophan metabolism through the kynurenine pathway in rat brain and liver slices. Free Radic Biol Med 2000; 29: 191–198.
Russo S, Kema IP, Fokkema MR, Boon JC, Willemse PH, de Vries EG et al. Tryptophan as a link between psychopathology and somatic states. Psychosom Med 2003; 65: 665–671.
Stone TW . Endogenous neurotoxins from tryptophan. Toxicon 2001; 39: 61–73.
Okuda S, Nishiyama N, Saito H, Katsuki H . 3-Hydroxykynurenine, an endogenous oxidative stress generator, causes neuronal cell death with apoptotic features and region selectivity. J Neurochem 1998; 70: 299–307.
Santamaria A, Galvan-Arzate S, Lisy V, Ali SF, Duhart HM, Osorio-Rico L et al. Quinolinic acid induces oxidative stress in rat brain synaptosomes. Neuroreport 2001; 12: 871–874.
Behan WM, McDonald M, Darlington LG, Stone TW . Oxidative stress as a mechanism for quinolinic acid-induced hippocampal damage: protection by melatonin and deprenyl. Br J Pharmacol 1999; 128: 1754–1760.
Wu HQ, Guidetti P, Goodman JH, Varasi M, Ceresoli-Borroni G, Speciale C et al. Kynurenergic manipulations influence excitatory synaptic function and excitotoxic vulnerability in the rat hippocampus in vivo. Neuroscience 2000; 97: 243–251.
Stone TW, Addae JI . The pharmacological manipulation of glutamate receptors and neuroprotection. Eur J Pharmacol 2002; 447: 285–296.
Schwarcz R, Whetsell Jr WO, Mangano RM . Quinolinic acid: an endogenous metabolite that produces axon-sparing lesions in rat brain. Science 1983; 219: 316–318.
Kerr SJ, Armati PJ, Guillemin GJ, Brew BJ . Chronic exposure of human neurons to quinolinic acid results in neuronal changes consistent with AIDS dementia complex. Aids 1998; 12: 355–363.
Jeong JH, Kim HJ, Lee TJ, Kim MK, Park ES, Choi BS . Epigallocatechin 3-gallate attenuates neuronal damage induced by 3-hydroxykynurenine. Toxicology 2004; 195: 53–60.
Fukui S, Schwarcz R, Rapoport SI, Takada Y, Smith QR . Blood–brain barrier transport of kynurenines: implications for brain synthesis and metabolism. J Neurochem 1991; 56: 2007–2017.
Heyes MP, Achim CL, Wiley CA, Major EO, Saito K, Markey SP . Human microglia convert l-tryptophan into the neurotoxin quinolinic acid. Biochem J 1996; 320 (Part 2): 595–597.
Saito K, Crowley JS, Markey SP, Heyes MP . A mechanism for increased quinolinic acid formation following acute systemic immune stimulation. J Biol Chem 1993; 268: 15496–15503.
Reynolds GP, Pearson SJ, Halket J, Sandler M . Brain quinolinic acid in Huntington's disease. J Neurochem 1988; 50: 1959–1960.
Reynolds GP, Pearson SJ . Increased brain 3-hydroxykynurenine in Huntington's disease. Lancet 1989; 2: 979–980.
Mangoni A . The ‘kynurenine shunt’ and depression. Adv Biochem Psychopharmacol 1974; 11: 293–298.
Sheline YI, Sanghavi M, Mintun MA, Gado MH . Depression duration but not age predicts hippocampal volume loss in medically healthy women with recurrent major depression. J Neurosci 1999; 19: 5034–5043.
Bremner JD, Narayan M, Anderson ER, Staib LH, Miller HL, Charney DS . Hippocampal volume reduction in major depression. Am J Psychiatry 2000; 157: 115–118.
Krishnan KR, McDonald WM, Escalona PR, Doraiswamy PM, Na C, Husain MM et al. Magnetic resonance imaging of the caudate nuclei in depression. Preliminary observations. Arch Gen Psychiatry 1992; 49: 553–557.
Husain MM, McDonald WM, Doraiswamy PM, Figiel GS, Na C, Escalona PR et al. A magnetic resonance imaging study of putamen nuclei in major depression. Psychiatry Res 1991; 40: 95–99.
Ongur D, Drevets WC, Price JL . Glial reduction in the subgenual prefrontal cortex in mood disorders. Proc Natl Acad Sci USA 1998; 95: 13290–13295.
Rajkowska G, Miguel-Hidalgo JJ, Wei J, Dilley G, Pittman SD, Meltzer HY et al. Morphometric evidence for neuronal and glial prefrontal cell pathology in major depression. Biol Psychiatry 1999; 45: 1085–1098.
Stone TW, Darlington LG . Endogenous kynurenines as targets for drug discovery and development. Nat Rev Drug Discov 2002; 1: 609–620.
Heyes MP, Mefford IN, Quearry BJ, Dedhia M, Lackner A . Increased ratio of quinolinic acid to kynurenic acid in cerebrospinal fluid of D retrovirus-infected Rhesus macaques: relationship to clinical and viral status. Ann Neurol 1990; 27: 666–675.
Herve C, Beyne P, Jamault H, Delacoux E . Determination of tryptophan and its kynurenine pathway metabolites in human serum by high-performance liquid chromatography with simultaneous ultraviolet and fluorimetric detection. J Chromatogr B Biomed Appl 1996; 675: 157–161.
Widner B, Ledochowski M, Fuchs D . Interferon-gamma-induced tryptophan degradation: neuropsychiatric and immunological consequences. Curr Drug Metab 2000; 1: 193–204.
Hamilton M . Development of a rating scale for primary depressive illness. Br J Soc Clin Psychol 1967; 6: 278–296.
Montgomery SA, Asberg M . A new depression scale designed to be sensitive to change. Br J Psychiatry 1979; 134: 382–389.
Maes M, Verkerk R, Bonaccorso S, Ombelet W, Bosmans E, Scharpe S . Depressive and anxiety symptoms in the early puerperium are related to increased degradation of tryptophan into kynurenine, a phenomenon which is related to immune activation. Life Sci 2002; 71: 1837.
Myint AM, Kim YK . Cytokine–serotonin interaction through IDO: a neurodegeneration hypothesis of depression. Med Hypotheses 2003; 61: 519–525.
Sheline YI, Gado MH, Kraemer HC . Untreated depression and hippocampal volume loss. Am J Psychiatry 2003; 160: 1516–1518.
Shah PJ, Ebmeier KP, Glabus MF, Goodwin GM . Cortical grey matter reductions associated with treatment-resistant chronic unipolar depression. Controlled magnetic resonance imaging study. Br J Psychiatry 1998; 172: 527–532.
Stockmeier CA, Mahajan G, Konick LC, Overholser JC, Jurjus GJ, Meltzer HY et al. Neuronal and glial density is increased and neuronal soma size is decreased in the hippocampus in major depressive disorder (MDD). Biol Psychiatry 2003; 53S: 198.
Sapolsky RM . Glucocorticoids and hippocampal atrophy in neuropsychiatric disorders. Arch Gen Psychiatry 2000; 57: 925–935.
Capuron L, Ravaud A, Neveu PJ, Miller AH, Maes M, Dantzer R . Association between decreased serum tryptophan concentrations and depressive symptoms in cancer patients undergoing cytokine therapy. Mol Psychiatry 2002; 7: 468–473.
Capuron L, Neurauter G, Musselman DL, Lawson DH, Nemeroff CB, Fuchs D et al. Interferon-alpha-induced changes in tryptophan metabolism. Relationship to depression and paroxetine treatment. Biol Psychiatry 2003; 54: 906–914.
Pardridge WM . Tryptophan transport through the blood–brain barrier: in vivo measurement of free and albumin-bound amino acid. Life Sci 1979; 25: 1519–1528.
Curzon G, Sarna GS . Tryptophan transport to the brain: newer findings and older ones reconsidered. In: Schlossberger HG, Kochen W, Linzen B, Steinhart H (eds) Progress in Tryptophan and Serotonin Research. Walter De Gruyter: Berlin, 1984 pp 145–157.
Acknowledgements
We thank Jim van Os for his critical remarks on this paper.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Wichers, M., Koek, G., Robaeys, G. et al. IDO and interferon-α-induced depressive symptoms: a shift in hypothesis from tryptophan depletion to neurotoxicity. Mol Psychiatry 10, 538–544 (2005). https://doi.org/10.1038/sj.mp.4001600
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.mp.4001600
Keywords
This article is cited by
-
Although serotonin is not a major player in depression, its precursor is
Molecular Psychiatry (2023)
-
Haut und Psyche - ein Teufelskreis?
Deutsche Dermatologie (2023)
-
Rapid improvement of psychiatric stigmata after IFN-free treatment in HCV patients with and without cryoglobulinemic vasculitis
Clinical Rheumatology (2022)
-
Acute administration of ibuprofen increases serum concentration of the neuroprotective kynurenine pathway metabolite, kynurenic acid: a pilot randomized, placebo-controlled, crossover study
Psychopharmacology (2022)
-
The prognosis and prevention measures for mental health in COVID-19 patients: through the experience of SARS
BioPsychoSocial Medicine (2020)