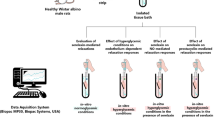
Abstract
Nitric oxide (NO) is formed from the conversion of L-arginine by nitric oxide synthase (NOS), which exists in three isoforms: neuronal (nNOS), endothelial (eNOS), and inducible (iNOS). nNOS is expressed in penile neurons innervating the corpus cavernosum, and eNOS protein expression has been identified primarily in both cavernosal smooth muscle and endothelium. NO is released from nerve endings and endothelial cells and stimulates the activity of soluble guanylate cyclase (sGC), leading to an increase in cyclic guanosine-3′,5′-monophosphate (cGMP) and, finally, to calcium depletion from the cytosolic space and cavernous smooth muscle relaxation. The effects of cGMP are mediated by cGMP dependent protein kinases, cGMP-gated ion channels, and cGMP-regulated phosphodiesterases (PDE). Thus, cGMP effect depends on the expression of a cell-specific cGMP-receptor protein in a given cell type. Numerous systemic vasculature diseases that cause erectile dysfunction (ED) are highly associated with endothelial dysfunction, which has been shown to contribute to decreased erectile function in men and a number of animal models of penile erection. Based on the increasing knowledge of intracellular signal propagation in cavernous smooth muscle tone regulation, selective PDE inhibitors have recently been introduced in the treatment of ED. Phosphodiesterase 5 (PDE5) inactivates cGMP, which terminates NO-cGMP-mediated smooth muscle relaxation. Inhibition of PDE5 is expected to enhance penile erection by preventing cGMP degradation. Development of pharmacologic agents with this effect has closely paralleled the emerging science.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 8 print issues and online access
$259.00 per year
only $32.38 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
References
Stuehr DJ, Marletta MA . Mammalian nitrate biosynthesis. Mouse macrophages produce nitrite and nitrate in response to Escherichia coli lipopolysaccharide. Proc Natl Acad Sci USA 1985; 82: 7738–7742.
Furchgott RF, Zawadzki JV . The obligatory role of endothelial cells in the relaxation of arterial smooth muscle by acetylcholine. Nature 1980; 228: 373–376.
Ignarro LJ et al. Endothelium-derived relaxing factor produced and released from artery and vein is nitric oxide. Proc Natl Acad Sci USA 1987; 84: 9265–9269.
Hobbs AJ . Soluble guanylate cyclase: the forgotten sibling. Trends Pharmacol Sci 1997; 18: 484–491.
McDonald LJ, Murad F . Nitric oxide and cyclic GMP signaling. Proc Soc Exp Biol Med USA 1996; 211: 1–6.
Johannes CB et al. Incidence of erectile dysfunction in men 40 to 69 years old: longitudinal results from the Massachusetts male aging study. J Urol 2000; 163: 460–463.
NIH Consensus Conference. Impotence. NIH Consensus Development Panel on Impotence. JAMA 1993; 270: 83–90.
Hurt KJ et al. Akt-dependent phosphorylation of endothelial nitric-oxide synthase mediates penile erection. PNAS 2002; 99: 4061–4066.
Hosogai N, Takakura S, Manda T, Mutoh S . Enzyme activities of the nitric oxide–cGMP pathway in corpus cavernosum isolated from middle-aged rats. Eur J Pharmacol 2003; 473: 65–70.
Burnett Al et al. Nitric oxide: a physiological mediator of penile erection. Science 1992; 257: 401–403.
Cartledge J, Minhas S, Eardley I . The role of nitric oxide in penile erection. Expert Opin Pharmacother 2001; 2: 95–107.
Ignarro LJ, Bush PS, Buga GM, Rajfer J . Neurotrasmitter identity in doubt. Nature 1990; 347: 131–132.
Kim YC et al. Modulation of vascoactive intestinal polypeptide (VIP)-mediated relaxation by nitric oxide and prostanoids in the rabbit corpus cavernosum. J Urol 1995; 153: 807–810.
Guiliano F, Rampin O, Benoit G, Jardin A . The peripheral pharmacology of erection. Prog Urol 1997; 7: 24–33.
Bivalacqua TJ et al. Gene transfer of prepro-calcitonin gene-related peptide restores erectile function in the aged rat. Biol Reprod 2001; 65: 1371–1377.
Champion HC et al. Comparison of responses to adrenomedullin and calcitonin gene-related peptide in the feline erection model. J Androl 1997; 18: 513–521.
Djamilian M, Stief CG, Kuczyk M, Jonas U . Followup results of a combination of calcitonin gene-related peptide and prostaglandin E1 in the treatment of erectile dysfunction. J Urol 1993; 149: 1296–1298.
Thomas G, Ramwell PW . Nitric oxide, donors, & inhibitors. In: Katzung BG (ed). Basic & Clinical Pharmacology, 7th edn. Appleton & Lange: Stamford, Connecticut, 1998, pp 319–324.
Chen J et al. Effect of oral administration of high-dose nitric oxide donor L-arginine in men with organic erectile dysfunction: results of double-blind, randomized, placebo-controlled study. BJU 1999; 83: 269–273.
Lowenstein CJ, Synder SH . Nitric oxide, a novel biologial messenger. Cell 1992; 70: 705–707.
Lamas S et al. Endothelial nitric oxide synthase: molecular cloning and characterization of a distinct constitutive enzyme isoform. Proc Natl Acad Sci USA 1992; 89: 6348–6352.
Forstermann U et al. Isoforms of nitric oxide synthase. Properties, cellular distribution and expressional control. Biochem Pharmacol 1995; 50: 1321–1332.
Lyons CR, Orloff GJ, Cunningham JM . Molecular cloning and functional expression of an inducible nitric oxide synthase from a murine macrophage cell line. J Biol Chem 1992; 267: 6370–6374.
Bredt DS et al. Cloned and expressed nitric oxide synthase structurally resemble cytochrome P-450 reductase. Nature 1991; 315: 714–718.
Okita RT, Masters BSS . Biotransformations: The cytochromes P45. In: Devlin TM (ed). Textbook of Biochemistry with Clinical Correlations, 4th edn. Wiley-Liss: New York, 1997, pp 981–999.
Magee TR et al. Gene therapy of erectile dysfunction in the rat with penile neuronal nitric oxide synthase cDNA. Biol Reprod 2002a; 67: 20–28.
Magee TR et al. Protein inhibitor of nitric oxide synthase (NOS) and the N-methyl-D-aspartate receptor are expressed in the rat and mouse penile nerves and colocalize with penile neuronal NOS. Biol Reprod 2003; 68: 478–488.
Pereira EC, Neto HS, Marques MJ . Immunolocalisation of neuronal nitric oxide synthase at the neuromuscular junction of MDX mice: a confocal microscopy study. J Anat 2001; 198: 663–671.
Tang Y, Rampin O, Giuliano F, Ugolini G . Spinal and brain circuits to motoneurons of the bulbospongiosus muscle: retrograde transneuronal tracing with rabies virus. J Comp Neurol 1999; 414: 167–192.
González-Cadavid NF, Ignarro LJ, Rajfer J . Nitric oxide and the cyclic GMP system in the penis. Mol Urol 1999; 3: 51–59.
Roczniak A, Levine DZ, Burns KD . Localization of protein inhibitor of neuronal nitric oxide synthase in rat kidney. Am J Physiol Renal Physiol 2000; 278: F702–F707.
Che YH et al. Changes in mRNA of protein inhibitor of neuronal nitric oxide synthase following facial nerve transection. J Chem Neuroanat 2000; 17: 199–206.
Hemmens B et al. The protein inhibitor of neuronal nitric oxide synthase (PIN): characterization of its action on pure nitric oxide synthases. FEBS Lett 1998; 430: 397–400.
Jaffrey SR et al. CAPON: a protein associated with neuronal nitric oxide synthase that regulates its interactions with PSD95. Neuron 1998; 20: 115–124.
Marson L, Carson CC . Central nervous system innervation of the penis, prostate, and perineal muscles: a transneuronal tracing study. Mol Urol 1999; 3: 43–50.
Giuliano F, Rampin O . Central neural regulation of penile erection. Neurosci Behav Rev 2000; 24: 517–533.
Chen KK, Chan JY, Chang LS . Dopaminergic neurotransmission at the paraventricular nucleus of hypothalamus in central regulation of penile erection in the rat. J Urol 1999; 162: 237–242.
Giuliano F et al. Erectile response to hypothalamic stimulation in rats: role of peripheral nerves. Am J Physiol 1997; 273: R1990–R1997.
Melis MR, Argiolas A . Role of central nitric oxide in the control of penile erection and yawning. Prog Neuropsychopharmacol Biol Psychiatry 1997; 21: 899–922.
Rampin O, Bernabe J, Giuliano F . Spinal control of penile erection. World J Urol 1997; 15: 2–13.
Ferrini MG et al. Penile neuronal nitric oxide synthase and its regulatory proteins are present in hypothalamic and spinal cord regions involved in the control of penile erection. J Comp Neurol 2003; 24: 46–61.
Rajfer J et al. Nitric oxide as a mediator of relaxation of the corpus cavernosum in response to nonadrenergic, noncholinergic neurotransmission. N Engl J Med 1992; 326: 90–94.
Fukuto JM, Wood KS, Byrns RE, Ignarro LJ . NG-amino-L-arginine: a new poten antagonist of L-arginine-mediated endothelium-dependent relaxation. Biochem Biophys Res Commun 1990; 168: 458–465.
Babu BR, Griffith OW . N5-(1-Imino-3-butenyl)-L-ornithine. A neuronal isoform selective mechanism-based inactivator of nitric oxide synthase. J Biol Chem 1998; 273: 8882–8889.
Gomez-Vidal JA, Martasek P, Roman LJ, Silverman RB . Potent and selective conformationally restricted neuronal nitric oxide synthase inhibitors. J Med Chem 2004; 47: 703–710.
Spiess PE et al. 7-Nitroindazole: a selective inhibitor of penile erection: an in vivo study in a rat animal model. Urology 1996; 47: 93–96.
Du XL et al. Hyperglycemia inhibits endothelial nitric oxide synthase activity by posttranslational modification at the Akt site. J Clin Invest 2001; 108: 1341–1348.
Akingba AG, Burnett AL . Endothelial nitric oxide synthase protein expression, localization, and activity in the penis of the alloxan-induced diabetic rat. Mol Urol 2001; 5: 189–197.
Seftel AD et al. Advanced glycation end products in human penis: elevation in diabetic tissue, site of deposition, and possible effect through iNOS or eNOS. Urology 1997; 50: 1016–1026.
Lincoln TM, Cornwell TL . Intracellular cyclic GMP receptor proteins. FASEB J 1993; 7: 328–339.
Czapski G, Goldstein S . The role of the reactions of NO with superoxide and oxygen in biological systems. A kinetic approach. Free Radical Biol Med 1995; 19: 785–794.
Khan MA et al. The effect of superoxide dismutase on nitric oxide-mediated and electrical field-stimulated diabetic rabbit cavernosal smooth muscle relaxation. BJU Int 2001; 87: 98–103.
Kim SC et al. Involvement of superoxide radical in the impaired endothelium-dependent relaxation of cavernous smooth muscle in hypercholesterolemic rabbits. Urol Res 1997; 25: 341–346.
Bivalacqua TJ et al. Gene transfer of extracellular SOD to the penis reduces O2− and improves erectile function in aged rats. Am J Physiol Heart Circ Physiol 2003; 284: 1408–1421.
Yu F, Warburton D, Wellington S, Danziger RS . Assignment of GUCIA2, the gene coding for the alpha 2 subunit of soluble guanylyl cyclase, to position 11q21–q22 on human chromosome 11. Genomics 1996; 33: 334–336.
Giuili G, Scholl U, Bulle F, Guellaen G . Molecular cloning of the cDNAs coding for the two subunits of soluble guanylyl cyclase from human brain. FEBS Lett 1992; 304: 83–88.
Papapetropoulos A et al. cGMP accumulation and gene expression of soluble guanylate cyclase in human vascular tissue. J Cell Physiol 1996; 167: 213–221.
Ignarro LJ et al. Activation of purified guanylate cyclase by nitric oxide requires heme. Comparison of heme-deficient-reconstituted and heme-containing forms of soluble enzyme from bovine lung. Biochim Biophys Acta 1982; 718: 49–59.
Stone JR, Marletta MA . Heme stoichiometry of heterodimeric soluble guanylate cyclase. Biochemistry 1995; 34: 14668–14674.
Ignarro LJ et al. A mechanism of vascular smooth muscle relaxation by organic nitrates, nitrites, nitroprusside and nitric oxide: evidence for the involvement of S-nitrosothiols as active intermediates. J Pharmacol Exp Ther 1981; 218: 739–749.
Wedel B et al. Mutation of His-105 in the beta 1 subunit yields a nitric oxide-insensitive form of soluble guanylyl cyclase. Proc Natl Acad Sci USA 1994; 91: 2592–2596.
Thorpe DS, Garbers DL . The membrane form of guanylate cyclase. Homology with a subunit of the cytoplasmic form of the enzyme. J Biol Chem 1989; 264: 6545–6549.
Wolin MS et al. Oxidant—nitric oxide signalling mechanisms in vascular tissue. Biochemistry (Moscow) 1998; 63: 810–816.
Stone JR, Marletta MA . Spectral and kinetic studies on the activation of soluble guanylate cyclase by nitric oxide. Biochemistry 1996; 35: 1093–1099.
Wolin MS, Wood KS, Ignarro LJ . Guanylate cyclase from bovine lung. A kinetic analysis of the regulation of the purified soluble enzyme by protoporphyrin IX, heme, and nitrosyl-heme. J Biol Chem 1982; 257: 13312–13320.
Schrammel A et al. Inhibition of purified soluble guanylyl cyclase by copper ions. Biochem Pharmaco 1996; 52: 1041–1045.
Luo D, Das S, Vincent SR . Effects of methylene blue and LY83583 on neuronal nitric oxide synthase and NADPH-diaphorase. Eur J Pharmacol 1995; 290: 247–251.
Deguchi T, Saito M, Kono M . Blockade by N-methylhydroxylamine of activation of guanylate cyclase and elevations of guanosine 3′,5′-monophosphate levels in nervous tissues. Biochim Biophys Acta 1978; 544: 8–19.
Cellek S, Kasakov L, Moncada S . Inhibition of nitrergic relaxations by a selective inhibitor of the soluble guanylate cyclase. Br J Pharmacol 1996; 118: 137–140.
Moro MA et al. cGMP mediates the vascular and platelet actions of nitric oxide: confirmation using an inhibitor of the soluble guanylyl cyclase. Proc Natl Acad Sci USA 1996; 93: 1480–1485.
Ko FN et al. YC-1, a novel activator of platelet guanylate cyclase. Blood 1994; 12: 4226–4233.
Mulsch A et al. Effect of YC-1, an NO-independent, superoxide-sensitive stimulator of soluble guanylyl cyclase, on smooth muscle responsiveness to nitrovasodilators. Br J Pharmacol 1997; 120: 681–689.
Mizusawa H et al. Nitric oxide independent activation of guanylate cyclase by YC-1 causes erectile responses in the rat. J Urol 2002; 167: 2276–2281.
Nakane M et al. Activation of soluble guanylate cyclase causes relaxation of corpus cavernosum tissue: synergism of nitric oxide and YC-1. Int J Impot Res (England) 2002; 14: 121–127.
Wolf L, Corbin JD, Francis SH . Characterization of a novel isozyme of cGMP-dependent protein kinase from bovine aorta. J Biol Chem 1989; 263: 17632–17637.
Lincoln TM . cGMP-dependent protein kinase. Methods Enzymol 1983; 99: 62–71.
Vrolix M et al. Cyclic GMP-dependent protein kinase stimulates the plasmalemmal Ca2+ pump of smooth muscle via phosphorylation of phosphatidyinositol. Biochem J 1988; 255: 855–863.
Yoshida Y, Sun HT, Cai JQ, Imai S . Cyclic GMP dependent protein kinase stimulates the plasma membrane Ca2+ pump ATPase of vascular smooth muscle via phosphorylation of a 240 kDa protein. J Biol Chem 1991; 266: 19819–19825.
Joyce NC, De Camilli P, Lomhmann SM, Walter U . cGMP-dependent protein kinase is present in high concentrations in contractile cells of the kidney vasculature. J Cyclic Nucleotide Protein Phosphor Res 1986; 11: 191–198.
Katzung BG, Chatterjee K . Vasodilators and the treatment of Angina Pectoris. In: Katzung BG (ed). Basic & Clinical Pharmacology, 7th edn. Appleton & Lange: Stamford. Connecticut, 1998, pp 179–196.
Ogut O, Brozovich FV . Regulation of force in vascular smooth muscle. J Mol Cell Cardiol 2003; 35: 347–355.
Chitaley K et al. Antagonism of Rho-kinase stimulates rat penile erection via a nitric oxide-independent pathway. Nat Med 2001; 7: 119–122.
Mills TM, Chitaley K, Lewis RW, Webb RC . Nitric oxide inhibits RhoA/Rho-kinase signaling to cause penile erection. Eur J Pharmacol 2002; 439: 173–174.
Chitaley K, Webb RC, Mills TM . Rho-kinase as a potential target for the treatment of erectile dysfunction. Drug News Perspect 2001; 14: 601–606.
Lincoln TM . Cyclic GMP and mechanisms of vasodilation. Pharmacol Ther 1989; 41: 479–502.
Twort CHC, Van Breemen C . Cyclic guanosine monophosphate-enhanced sequestration of Ca2+ by sarcoplasmic reticulum in vascular smooth muscle. Circ Res 1988; 62: 961–964.
Lucas KA et al. Guanylyl cyclases and signaling by cyclic GMP. Pharmacol Rev 2000; 52: 375–414.
Bredt DS, Snyder SH . Isolation of nitric oxide synthetase, a calmodulin-requiring enzyme. Proc Natl Acad Sci USA 1990; 87: 682–685.
Fulton D et al. Regulation of endothelium-derived nitric oxide production by the protein kinase Akt. Nature 1999; 10: 597–601.
Michell BJ et al. Coordinated control of endothelial nitric-oxide synthase phosphorylation by protein kinase C and the cAMP-dependent protein kinase. J Biol Chem 2001; 276: 17625–17628.
Murphy RA, Walker JS . Inhibitory mechanisms for cross–bridge cycling: the nitric oxide-cGMP signal transduction pathway in smooth muscle relaxation. Acta Physiol Scand 1998; 164: 373–380.
Archer SL . Potassium channels and erectile dysfunction. Vasc Pharmacol 2002; 38: 61–71.
Rosen RC, Kostis JB . Overview of phosphodiesterase 5 inhibition in erectile dysfunction. Am J Cardiol 2003; 92: 9–18.
Ückert S, küthe A, Stief CG, Jonas U . Phosphodiesterase isoenzymes as pharmacological targets in the treatment of male erectile dysfunction. World J Urol 2001; 19: 14–22.
Taher A et al. Cyclic nucleotide phosphodiesterase in human cavernous smooth muscle. World J Urol 1997; 15: 32–35.
Ballard SA et al. Effects of sildenafil on the relaxation of human corpus cavernosum tissue in vitro and on the activities of cyclic nucleotide phosphodiesterase isozymes. J Urol 1998; 159: 2164–2171.
Stief CG et al. Effects of specific phosphodiesterase (PDE) inhibitorson human and rabbit cavernous tissue in vitro and in vivo. J Urol 1998; 159: 1390–1393.
Francis SH, Turko IV, Corbin JD . Cyclic nucleotide phosphodiesterases: relating structure and function. Prog Nucleic Acid Res Mol Biol 2001; 65: 1–52.
Zusman RM, Morales A, Glasser DB, Osterloh IH . Overall cardiovascular profile of sildenafil citrate. Am J Cardiol 1999; 83: 35–44.
Brock GE et al. Efficacy and safety of tadalafil in the treatment of erectile dysfunction: results of integrated analyses. J Urol 2002; 168: 1332–1336.
Angulo J et al. IC351 enhances NO-mediated relaxation of human arterial and trabecular penile smooth muscle. Eur Urol 2001; 39 (Suppl 5): 106, Abstract 415.
Sáenz de Tejada I et al. The phosphodiesterase inhibitory selectivity and the in vitro and in vivo potency of the new PDE5 inhibitor vardenafil. Int J Impot Res 2001; 13: 282–290.
Ishikura F et al. Effects of sildenafil citrate (Viagra) combined with nitrate on the heart. Circulation 2000; 102: 2516–2521.
Piccirillo G et al. Effects of sildenafil citrate (viagra) on cardiac repolarization and on autonomic control in subjects with chronic heart failure. Am Heart J 2002; 143: 703–710.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Ghalayini, I. Nitric oxide–cyclic GMP pathway with some emphasis on cavernosal contractility. Int J Impot Res 16, 459–469 (2004). https://doi.org/10.1038/sj.ijir.3901256
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.ijir.3901256
Keywords
This article is cited by
-
Enhanced pericyte-endothelial interactions through NO-boosted extracellular vesicles drive revascularization in a mouse model of ischemic injury
Nature Communications (2023)
-
Topically delivered nitric oxide acts synergistically with an orally administered PDE5 inhibitor in eliciting an erectile response in a rat model of radical prostatectomy
International Journal of Impotence Research (2022)
-
Stimulators and activators of soluble guanylate cyclase for urogenital disorders
Nature Reviews Urology (2018)
-
Erectile properties of the Rho-kinase inhibitor SAR407899 in diabetic animals and human isolated corpora cavernosa
Journal of Translational Medicine (2012)
-
Chuanxiongzine relaxes isolated corpus cavernosum strips and raises intracavernous pressure in rabbits
International Journal of Impotence Research (2010)