Abstract
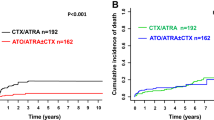
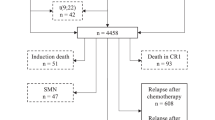
We analyzed the incidence, presenting features, risk factors of extramedullary (EM) relapse occurring in acute promyelocytic leukemia (APL) treated with all-trans retinoic acid (ATRA) and chemotherapy by using a competing-risk method. In total, 740/806 (92%) patients included in three multicenter trials (APL91, APL93 trials and PETHEMA 96) achieved CR, of whom 169 (23%) relapsed, including 10 EM relapses. Nine relapses involved the central nervous system (CNS) and one the skin, of which two were isolated EM relapse. In patients with EM disease, median WBC count was 26 950/mm3 (7700–162 000). The 3-year cumulative incidence of EM disease at first relapse was 5.0%. Univariate analysis identified age <45 years (P=0.05), bcr3 PML-RARα isoform (P=0.0003) and high WBC counts (⩾10 000/mm3) (P<0.0001) as risk factors for EM relapse. In multivariate analysis, only high WBC count remained significant (P=0.001). Patients with EM relapse had a poorer outcome since median survival from EM relapse was 6.7 months as compared to 26.3 months for isolated BM relapse (P=0.04). In conclusion, EM relapse in APL occurs more frequently in patients with increased WBC counts (⩾10 000/mm3) and carries a poor prognosis. Whether CNS prophylaxis should be systematically performed in patients with WBC ⩾10 000/mm3 at diagnosis remains to be established.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Fenaux P, Chevret S, Guerci A, Fegueux N, Dombret H, Thomas X et al. Long-term follow-up confirms the benefit of all-trans retinoic acid in acute promyelocytic leukemia. European APL group. Leukemia 2000; 14: 1371–1377.
Tallman MS, Andersen JW, Schiffer CA, Appelbaum FR, Feusner JH, Woods WG et al. All-trans retinoic acid in acute promyelocytic leukemia: long-term outcome and prognostic factor analysis from the North American Intergroup protocol. Blood 2002; 100: 4298–4302.
Mandelli F, Diverio D, Avvisati G, Luciano A, Barbui T, Bernasconi C et al. Molecular remission inPML/RAR-positive acute promyelocytic leukemia by combined all-trans retinoic acid, idarubicin (AIDA) therapy. Blood 1997; 90: 1014–1021.
Sanz MA, Martin G, Rayon C, Esteve J, Gonzalez M, Diaz-Mediavilla J et al. A modified AIDA protocol with anthracycline-based consolidation results in high antileukemic efficacy and reduced toxicity in newly diagnosed PML/RARalpha-positive acute promyelocytic leukemia. PETHEMA group. Blood 1999; 94: 3015–3021.
Fenaux P, Chastang C, Chevret S, Sanz M, Dombret H, Archimbaud E et al. A randomized comparison of all transretinoic acid (ATRA) followed by chemotherapy and ATRA plus chemotherapy and the role of maintenance therapy in newly diagnosed acute promyelocytic leukemia. The European APL Group. Blood 1999; 94: 1192–2000.
Sanz MA, Martin G, Gonzalez M, Leon A, Rayon C, Rivas C et al. Risk-adapted treatment of acute promyelocytic leukemia with all-trans retinoic acid and anthracycline monochemotherapy: a multicenter study by the PETHEMA Group. Blood 2004; 103: 1237–1243.
Tallman MS, Nabhan C, Feusner JH, Rowe JM . Acute promyelocytic leukemia: evolving therapeutic strategies. Blood 2002; 99: 759–767.
Ohno R, Asou N, Ohnishi K . Treatment of acute promyelocytic leukemia: strategy toward further increase of cure rate. Leukemia 2003; 17: 1454–1463.
Wiernik PH, De Bellis R, Muxi P, Dutcher JP . Extramedullary acute promyelocytic leukemia. Cancer 1996; 78: 2510–2514.
Byrd JC, Edenfield WJ, Shields DJ, Dawson NA . Extramedullary myeloid cell tumors in acute non lymphocytic leukemia: a clinical review. J Clin Oncol 1995; 13: 1800–1816.
Marra R, Storti S, Pagano L . Central nervous system acute promyelocytic leukemia: a report of three cases. Haematologica 1989; 3: 195–199.
Evans GD, Grimwade DJ . Extramedullary disease in acute promyelocytic leukemia. Leuk Lymphoma 1999; 33: 219–229.
Liso V, Specchia G, Pogliani EM, Palumbo G, Mininni D, Rossi V et al. Extramedullary involvement in patients with acute promyelocytic leukemia: a report of seven cases. Cancer 1998; 83: 1522–1528.
Ko B-S, Tang G-L, Chen Y-C, Yao M, Wang CH, Shen MC et al. Extramedullary relapse after all-trans retinoic acid treatment in acute promyelocytic leukemia. The occurrence of retinoic acid syndrome is a risk factor. Leukemia 1999; 13: 1406–1408.
Sanz MA, Larrea L, Sanz G, Martin G, Sempere A, Gomis F et al. Cutaneous promyelocytic sarcoma at sites of vascular access, marrow aspiration. A characteristic localization of chloromas in acute promyelocytic leukemia? Haematologica 2000; 85: 758–762.
Specchia G, Lo Coco F, Vignetti M, Avvisati G, Albano V, Fazi P et al. Extramedullary involvement at relapse in acute promyelocytic leukemia patients treated or not with ATRA. A report by the Gimema group. J Clin Oncol 2001; 19: 4023–4028.
Breccia M, Carmosino I, Diverio D, De Santis S, De Propris MS, Romano A et al. Early detection of meningeal localization in acute promyelocytic leukaemia patients with high presenting leucocyte count. Br J Haematol 2003; 120: 266–270.
Breccia M, Petti MC, Testi AM, Specchia G, Ferrara F, Diverio D et al. Ear involvement in acute promyelocytic leukemia at relapse: a disease-associated ‘sanctuary’? Leukemia 2002; 16: 1127–1130.
Eclache V, Benzacken B, Le Roux G, Casassus P, Chomienne C . PML/RAR alpha rearrangement in acute promyelocytic leukaemia with t(1;17) elucidated using fluorescence in situ hybridization. Br J Haematol 1997; 98: 440–443.
Bolufer P, Barragán E, Sanz MA, Martín G, Bornstein R, Colomer D et al. Preliminary experience in external quality control of RT-PCR PML/RARα detection in promyelocytic leukemia. Leukemia 1998; 12: 2024–2028.
Prentice RL, Kalbfleish JD, Peterson AV, Flournoy N, farewell N, Breslow NE . The analysis of failure times in the presence of competing risks. Biometrics 1978; 34: 541–554.
Gray RJ . A class of k-sample tests for comparing the cumulative incidence of a competing risk. Ann Statist 1988; 16: 1115–1141.
Fine JP, Gray RJ . A proportional hazards model for the subdistribution of a competing risk. JASA 1999; 94: 496–509.
Peto R, Peto J . Asymptotically efficient rank invariant test procedures. J Roy Stat Soc 1972; 135: 185–206.
Kaplan E, Meier P . Nonparametric estimation from incomplete observations. J Am Stat Assoc 1958; 53: 457–472.
Guglielmi C, Martelli MP, Diviero D, Fenu S, Vegna ML, Cantu-Rajnoldi A et al. Immunophenotype of adult and childhood acute promyelocytic leukaemia: correlation with morphology, type of PML gene breakpoint and clinical outcome. A cooperative Italian study on 196 cases. Br J Haematol 1998; 102: 1035–1041.
Gonzalez M, Barragan E, Bolufer P, Chillon C, Colomer D, Borstein R et al. Pretreatment characteristics and clinical outcome of acute promyelocytic leukaemia patients according to the PML-RAR alpha isoforms: a study of the PETHEMA group. Br J Haematol 2001; 114: 99–103.
Sanz MA, Lo Coco F, Martin G, Avvisati G, Rayon C, Barbui T et al. Definition of relapse risk and role of ninanthracycline drugs for consolidation in patients with acute promyelocytic leukemia: a joint study of the PETHEMA and GIMEMA Cooperative Groups. Blood 2000; 96: 1247–1253.
de Botton S, Coiteux V, Chevret S, Rayon C, Vilmer E, Sanz M et al. Outcome of childhood acute promyelocytic leukemia with all-trans-retinoic acid and chemotherapy. J Clin Oncol 2004; 22: 1404–1412.
Ferrara F, Morabito F, Martino B, Specchia G, Liso V, Nobile F et al. CD56 expression is an indicator of poor clinical outcome in patients with acute promyelocytic leukemia treated with simultaneous all-trans-retinoic acid and chemotherapy. J Clin Oncol 2000; 18: 1295–1300.
Ravandi F, Cortes J, Estrov Z, Thomas D, Giles FJ, Huh YO et al. CD56 expression predicts occurrence of CNS disease in acute lymphoblastic leukemia. Leuk Res 2002; 26: 643–649.
Acknowledgements
This work was supported by the Programme Hospitalier de Recherche Clinique (CHU Lille), the Association de Recherche contre le Cancer and the Ligue Nationale contre le Cancer (Comité du Nord).
Author information
Authors and Affiliations
Corresponding author
Additional information
Complete list of participants and addresses are given in appendix A.
Appendix A
Appendix A
The following clinical departments and personnel participated in the PETHEMA 96 trial:
Hospital Universitario La Fe, Valencia, Sanz MA, Martín G; Hospital Central de Asturias, Oviedo, Rayón C; Hospital Clínico San Carlos, Madrid, Díaz-Mediavilla J; Hospital Clínico Universitario, Valencia, Terol MJ; Hospital Insular de Las Palmas, Las Palmas, González JD; Hospital Clinic, Barcelona, Esteve J; Hospital General, Alicante, Rivas C; Hospital U. Germans Trias i Pujol, Badalona, Ribera JM; Complexo Hospitalario Xeral-Calde, Lugo, Arias J; Hospital Universitario, Salamanca, González M; Hospital de Cruces, Baracaldo, Alvarez MC; Complejo Hospitalario, León, Ramos F; Hospital Juan Canalejo, La Coruña, Debén G; Hospitales Ntra Sra del Pino/Sabinal, Las Palmas, Mataix R; Hospital Reina Sofia, Córdoba, Tabares S; Hospital Clínico Universitario, Valladolid, Fernández F; Hospital Universitario Vall D'Hebron, Barcelona, Bueno J; Hospital Son Dureta, Palma de Mallorca, Novo A; Hospital Xeral de Galicia, Santiago de Compostela, Pérez M; Hospital Ramón y Cajal, Madrid, Odriozola J; Hospital do Meixoeiro, Vigo, Loureiro C; Hospital Severo Ochoa, Leganés, Sánchez P; Hospital Dr Peset, Valencia, Sayas MJ; Hospital 12 de Octubre, Madrid, De la Serna J; Hospital General de Murcia, Murcia, Moraleda JM; H Universitario Virgen de la Victoria, Málaga, Pérez I; HU Puerta del Mar, Cádiz, Capote FJ Hospital San Pedro de Alcántara, Cáceres, Bergua JM; Hospital Materno-Infantil de Las Palmas, Las Palmas, Lodos JC Basurtuko Ospitalea, Basurto, Beltrán de Heredia JM; Hospital Rio Hortega, Valladolid, Peñarrubia MJ; Hospital Clínico Universitario Lozano Blesa, Zaragoza, Palomera L; Hospital General Jerez de la Frontera, Jerez de la Frontera, León A; Hospital General, Albacete, Romero JR; Hospital Xeral Cíes, Vitoria, Poderós C; Hospital Txagorritxu, Vitoria, Guinea JM; Hospital San Pau, Barcelona, Brunet S; Hospital General (Oncología Pediátrica), Alicante, Esquembre C; Hospital Rio Carrión, Palencia, Ortega F; Hospital U Marqués de Valdecilla, Santander, Conde E; H Universitario La Fe (Hospital Infantil), Valencia, Castell V
The following laboratories and personnel participated in the PETHEMA 96 trial:
Hospital Universitario La Fe, Valencia, Bolufer P, Barragán E; Hospital Universitario, Salamanca, González M, Chillón C; Hospital Clinic, Barcelona, Colomer D; Hospitales Ntra Sra del Pino/Sabinal, Las Palmas, Gómez T; Hospital Reina Sofia, Córdoba, Román J; Universidad de Navarra, Pamplona, Calasanz MJ; Hospital 12 de Octubre, Madrid, Bornstein R; Hospital Clínico San Carlos, Madrid, Villegas A; Hospital Clínico Universitario, Valencia, Marugán I; Hospital Ramón y Cajal, Madrid, Ferro C; Hospital do Meixoeiro, Vigo, Loureiro C; Hospital U Marqués de Valdecilla, Santander, Richard C.
Dr P Fenaux and Dr L Degos served as cochairmen, and Dr C Chastang and S Chevret-Chastang (Department of Biostatistics, Hopital St Louis, Paris), as biostatiscians. The following clinical departments participated in APL91 and APL93 trials:
French APL Group: S Castaigne, H Dombret (Paris), R Zittoun (Paris), E Archimbaud (Lyon), P Travade (Clermont Ferrand), C Gardin (Clichy), A Guerci (Nancy), S de Botton (Lille), AM Stoppa (Marseille), F Dreyfus (Paris), F Stamatoulas (Rouen), F Rigal-Huguet (Toulouse), H Guy (Dijon), JJ Sotto (Grenoble), F Maloisel (Strasbourg), J Reiffers (Pessac), A Gardembas (Angers), D Bordessoule (Limoges), N Fegueux (Montpellier), A Veil (Paris), T Lamy (Rennes), M Hayat (Villejuif), E Deconinck (Besancon), E Guyotat (St Etienne), M Martin (Annecy), E Cony-Makhoul (Bordeaux), JP Abgrall (Brest), O Reman (Caen), B Desablens (Amiens), JL Harousseau (Nantes), Y Bastion (Lyon), JP Pollet (Valenciennes), J Pulik (Argenteuil), M Lepeu (Avignon), M Renoux (Bayonne), P Morel (Lens), P Henon (Mulhouse), N Gratecos (Nice), P Colombat (Tours), D Machover (Villejuif), A Dor (Antibes), P Casassus (Bobigny), J Donadio (Castelnou), B Salles (Chalon), B Legros (Clermont Ferrand), P Audhuy (Colmar), A Dutel (Compiègne), N Philippe (Lyon), B Benothman (Meaux), C Christian (Metz), C Margueritte (Montpellier), F Witz (Nancy), A Pesce (Nice), A Baruchel (Paris), L Sutton (Paris), C Quetin (Pointe à Pitre), B Pignon (Reims), E Vilmer (Paris), E Bourquard (St Brieuc), JP Marolleau (Paris), P Robert (Toulouse), B Despax (Toulouse), G Nedellec, P Auzanneau (Paris), M Janvier (St Cloud).
Spanish AML Group: O Rayon (Oviedo), M Sanz (Valencia), J San Miguel (Salamanca), J Montagud (Valencia), E Condé (Santander), P Javier de la Serna (Madrid), G Martin (Valencia), M Perez Encinas (Santiago), JP Torres Carrete (Juan Canalejo), J Zuazu (Barcelone), J Odriozola (Madrid), E Gomez-Sanz (Madrid), L Palomera (Zaragoza), L Villegas (Almeria), A Deben (Juan Canalejo), P Besalduch (Palma de Mallorca).
Cooperative AML Study Group, Germany: H Link (Hannover), A Ganser (Frankfurt), E Wandt (Nurnberg), A Breitenbach (Stuttgart), B Brennscheidt (Freiburg), D Herrmann (Ulm), H Soucek (Dresden), H Strobel (Erlangen).
Swiss Group for Clinical Cancer Research AML group: K Geiser (Berne), M Fey (Berne), T Egger (Berne), E Jacky.
Belgian Group: JL Michaux (Bruxelles), A Bosly (Yvoir), E Meeus (Anvers), A Boulet (Mons).
Dutch group: P Daenen (Groningen), P Muus (Nijmegen).
Rights and permissions
About this article
Cite this article
de Botton, S., Sanz, M., Chevret, S. et al. Extramedullary relapse in acute promyelocytic leukemia treated with all-trans retinoic acid and chemotherapy. Leukemia 20, 35–41 (2006). https://doi.org/10.1038/sj.leu.2404006
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.leu.2404006
Keywords
This article is cited by
-
An overview of arsenic trioxide-involved combined treatment algorithms for leukemia: basic concepts and clinical implications
Cell Death Discovery (2023)
-
A case of acute promyelocytic leukemia variant with derivative chromosome 3 der(3)t(3;8) associated with 8q partial gain
Molecular Cytogenetics (2019)
-
Management of patients with acute promyelocytic leukemia
Leukemia (2018)