Abstract
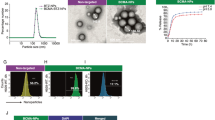
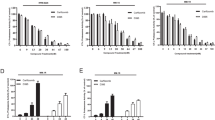
Multiple myeloma (MM) is an incurable B-cell cancer characterised by the monoclonal proliferation of tumour cells in the bone marrow (BM). It has been described that matrix metalloproteinases (MMPs) and especially MMP-9 is secreted by MM cells. In this study, we investigated the possibility to exploit MMP-9 activity to activate prodrugs and to target MM cells as a new tumour-specific therapy. Cleavage of the prodrug EV1-FITC by MMP-9 resulted in release of fluorescence which can be used as a measure of prodrug activation. The 5T33MM mouse model was used in this proof-of-principle study. The prodrug was activated in a higher amount by addition to MMP-9-producing 5T33MMvv cells, homogenates from tumour-bearing organs (BM, spleen) and isolated 5T33MM-diseased BM and spleen cells compared to non-MMP-9-producing 5T33MMvt cells and homogenates/cells from nontumour-bearing organs/mice, as measured by fluorescence release. This fluorescence release could be inhibited by the MMP-2/MMP-9-specific inhibitor, CTT. Activation of the prodrug in the 5T33MM spleen and BM homogenates was confirmed by chromatography. EV1-fluorescein isothiocyanate injection into 5T33MM-diseased animals resulted in a higher fluorescence release by the isolated BM and spleen cells compared to injection into healthy animals. In conclusion, MMP-9 activity can be used to activate prodrugs that target MM.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout









Similar content being viewed by others
References
Denny WA . Prodrug strategies in cancer therapy. Eur J Med Chem 2001; 36: 577–595.
DeFeo-Jones D, Brady SF, Feng DM, Wong BK, Bolyar T, Haskell K et al. A prostate-specific antigen (PSA)-activated vinblastine prodrug selectively kills PSA-secreting cells in vivo. Mol Cancer Ther 2002; 1: 451–459.
Liu C, Sun C, Huang H, Janda K, Edgington T . Overexpression of legumain in tumors is significant for invasion/metastasis and a candidate enzymatic target for prodrug therapy. Cancer Res 2003; 63: 2957–2964.
Devy L, de Groot FM, Blacher S, Hajitou A, Beusker PH, Scheeren HW et al. Plasmin-activated doxorubicin prodrugs containing a spacer reduce tumor growth and angiogenesis without systemic toxicity. FASEB J 2004; 18: 565–567.
Trouet A, Passioukov A, Van derpoorten K, Fernandez AM, Abarca-Quinones J, Baurain R et al. Extracellularly tumor-activated prodrugs for the selective chemotherapy of cancer: application to doxorubicin and preliminary in vitro and in vivo studies. Cancer Res 2001; 61: 2843–2846.
Mincher DJ, Turnbull A, Bibby MC, Loadman PM . (Inventors) Tumour targeting prodrugs activated by matrix metalloproteinases. US Patent Application, (2004) US 2004/0248765 (Publ 09-12-2004) corresponding to: WO02072620; PCT/GB/02/01069, EP1366064; GB0105929.4 (priority date 09-03-2001).
Barillé S, Akhoundi C, Collette M, Mellerin MP, Rapp MJ, Harousseau JL et al. Metalloproteinases in multiple myeloma: production of matrix metalloproteinase-9 (MMP-9), activation of proMMP-2, and induction of MMP-1 by myeloma cells. Blood 1997; 90: 1649–1655.
Van Valckenborgh E, Bakkus M, Munaut C, Noël A, St Pierre Y, Asosingh K et al. Upregulation of matrix metalloproteinase-9 in murine 5T33 multiple myeloma cells by interaction with bone marrow endothelial cells. Int J Cancer 2002; 101: 512–518.
Van Valckenborgh E, Croucher PI, De Raeve H, Carron C, De Leenheer E, Blacher S et al. Multifunctional role of matrix metalloproteinases in multiple myeloma: a study in the 5T2MM mouse model. Am J Pathol 2004; 165: 869–878.
Radl J, De Glopper ED, Schuit HR, Zurcher C . Idiopathic paraproteinemia. II. Transplantation of the paraprotein-producing clone from old to young C57BL/KaLwRij mice. J Immunol 1979; 122: 609–613.
Vanderkerken K, De Raeve H, Goes E, Van Meirvenne S, Radl J, Van Riet I et al. Organ involvement and phenotypic adhesion profile of 5T2 and 5T33 myeloma cells in the C57BL/KaLwRij mouse. Br J Cancer 1997; 76: 451–460.
Barillé S, Bataille R, Rapp M, Harousseau J, Amiot M . Production of metalloproteinase-7 (matrilysin) by human myeloma cells and its potential involvement in metalloproteinase-2 activation. J Immunol 1999; 163: 5723–5728.
Vacca A, Ribatti D, Iurlaro M, Albini A, Minischetti M, Bussolino F et al. Human lymphoblastoid cells produce extracellular matrix-degrading enzymes and induce endothelial cell proliferation, migration, morphogenesis, and angiogenesis. Int J Clin Lab Res 1998; 28: 55–68.
Vacca A, Ribatti D, Presta M, Minischetti M, Iurlaro M, Ria R et al. Bone marrow neovascularization, plasma cell angiogenic potential, and matrix metalloproteinase-2 secretion parallel progression of human multiple myeloma. Blood 1999; 93: 3064–3073.
Wahlgren J, Maisi P, Sorsa T, Sutinen M, Tervahartiala T, Pirilä E et al. Expression and induction of collagenases (MMP-8 and -13) in plasma cells associated with bone-destructive lesions. J Pathol 2001; 194: 217–224.
Vacca A, Ria R, Semeraro F, Merchionne F, Coluccia M, Boccarelli A et al. Endothelial cells in the bone marrow of patients with multiple myeloma. Blood 2003; 102: 3340–3348.
Vande Broek I, Asosingh K, Allegaert V, Leleu X, Facon T, Vanderkerken K et al. Bone marrow endothelial cells increase the invasiveness of human multiple myeloma cells through upregulation of MMP-9: evidence for a role of hepatocyte growth factor. Leukemia 2004; 18: 976–982.
Hoekstra R, Eskens FALM, Verweij J . Matrix metalloproteinase inhibitors: current developments and future perspectives. Oncologist 2001; 6: 415–427.
Bonomi P . Matrix metalloproteinases and matrix metalloproteinase inhibitors in lung cancer. Semin Oncol 2002; 29: 78–86.
Turnbull A, Mincher DJ . (Inventors). Anticancer Agents. US Patent, 2003: US2003203975, corresponding to PCT/GB99/01901, WO99/65866 (Publ. 30-10-2003).
Gershkovich AA, Kholodovych VV . Fluorogenic substrates for proteases based on intramolecular fluorescence energy transfer (IFETS). J Biochem Biophys Methods 1996; 33: 135–162.
McGeehan G, Bickett D, Green M, Kassel D, Wiseman JS, Berman J . Characterization of the peptide substrate specificities of interstitial collagenase and 92-kDa gelatinase. Implications for substrate optimization. J Biol Chem 1994; 269: 32814–32820.
Schechter I, Berger A . On the size of the active site in proteases. I. Papain. Biochem Biophys Res Commun 1967; 27: 157–162.
Kridel SJ, Chen EI, Kotra LP, Howard EW, Mobashery S, Smith JW . Substrate hydrolysis by matrix metalloproteinase-9. J Biol Chem 2001; 276: 20572–20578.
Chen EI, Kridel SJ, Howard EW, Li W, Godzik A, Smith JW . A unique substrate recognition profile for matrix metalloproteinase-2. J Biol Chem 2002; 277: 4485–4491.
Gehring MR, Condon B, Margosiak SA, Kan C-C . Characterization of the phe-81 and val-82 human fibroblast collagenase catalytic domain purified from Escherichia coli. J Biol Chem 1995; 270: 22507–22513.
Acknowledgements
This work was financially supported by the Stichting Emmanuel Vander Scheuren, Onderzoeksraad-Vrije Universiteit Brussel (OZR-VUB), Fonds voor Wetenschappelijk Onderzoek-Vlaanderen, Kom op tegen Kanker, Belgische Federatie tegen Kanker, Fortis, VIVA and VIS. Karin Vanderkerken is a postdoctoral fellow of the ‘Fonds voor Wetenschappelijk Onderzoek-Vlaanderen’ (FWO-Vl). The financial support of BTG International plc (ADS and DM) and assistance of the EPSRC Mass Spectrometry Service Centre, Swansea, UK, are gratefully acknowledged.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Van Valckenborgh, E., Mincher, D., Di Salvo, A. et al. Targeting an MMP-9-activated prodrug to multiple myeloma-diseased bone marrow: a proof of principle in the 5T33MM mouse model. Leukemia 19, 1628–1633 (2005). https://doi.org/10.1038/sj.leu.2403866
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.leu.2403866
Keywords
This article is cited by
-
Principles in the design of ligand-targeted cancer therapeutics and imaging agents
Nature Reviews Drug Discovery (2015)
-
New approaches to selectively target cancer-associated matrix metalloproteinase activity
Cancer and Metastasis Reviews (2014)
-
Tumour endoproteases: the cutting edge of cancer drug delivery?
British Journal of Pharmacology (2008)
-
Importance of the bone marrow microenvironment in inducing the angiogenic response in multiple myeloma
Oncogene (2006)