Abstract
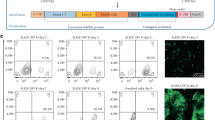
Electroporation of mRNA has become an established method for gene transfer into dendritic cells for immunotherapeutic purposes. However, many more cell types and applications might benefit from an efficient mRNA-based gene transfer method. In this study, we investigated the potential of mRNA-based gene transfer to induce short-term transgene expression in adult stem cells and activated T cells, based on electroporation with mRNA encoding the enhanced green fluorescent protein. The results show efficient transgene expression in CD34-positive hematopoietic progenitor cells (35%), in in vitro cultured mesenchymal cells (90%) and in PHA-stimulated T cells (50%). Next to presentation of gene transfer results, potential applications of mRNA-based gene transfer in stem cells and T cells are discussed.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Sullenger BA, Gilboa E . Emerging clinical applications of RNA. Nature 2002; 418: 252–258.
Hacein-Bey-Abina S, von Kalle C, Schmidt M, Le Deist F, Wulffraat N, McIntyre E et al. A serious adverse event after successful gene therapy for X-linked severe combined immunodeficiency. N Engl J Med 2003; 348: 255–256.
Marshall E . Gene therapy death prompts review of adenovirus vector. Science 1999; 286: 2244–2245.
Van Tendeloo VF, Ponsaerts P, Lardon F, Nijs G, Lenjou M, Van Broeckhoven C et al. Highly efficient gene delivery by mRNA electroporation in human hematopoietic cells: superiority to lipofection and passive pulsing of mRNA and to electroporation of plasmid cDNA for tumor antigen loading of dendritic cells. Blood 2001; 98: 49–56.
Ponsaerts P, Van Tendeloo VF, Berneman ZN . Cancer immunotherapy using RNA-loaded dendritic cells. Clin Exp Immunol 2003; 134: 378–384.
Saeboe-Larssen S, Fossberg E, Gaudernack G . mRNA-based electrotransfection of human dendritic cells and induction of cytotoxic T lymphocyte responses against the telomerase catalytic subunit (hTERT). J Immunol Methods 2002; 259: 191–203.
Chen ZZ, Van Bockstaele DR, Buyssens N, Hendrics D, De MI, Vanhoof G et al. Stromal populations and fibrosis in human long-term bone marrow cultures. Leukemia 1991; 5: 772–781.
Miller G, Lipman M . Release of infectious Epstein–Barr virus by transformed marmoset leukocytes. Proc Natl Acad Sci USA 1973; 70: 190–194.
Savoldo B, Huls MH, Liu Z, Okamura T, Volk HD, Reinke P et al. Autologous Epstein–Barr virus (EBV)-specific cytotoxic T cells for the treatment of persistent active EBV infection. Blood 2002; 100: 4059–4066.
Nair SK, Boczkowski D, Morse M, Cumming RI, Lyerly HK, Gilboa E . Induction of primary carcinoembryonic antigen (CEA)-specific cytotoxic T lymphocytes in vitro using human dendritic cells transfected with RNA. Nat Biotechnol 1998; 16: 364–369.
Ponsaerts P, Van Tendeloo VF, Cools N, Van Driessche A, Lardon F, Nijs G et al. mRNA-electroporated mature dendritic cells retain transgene expression, phenotypical properties and stimulatory capacity after cryopreservation. Leukemia 2002; 16: 1324–1330.
Van Tendeloo VF, Willems R, Ponsaerts P, Lenjou M, Nijs G, Vanhove M et al. High-level transgene expression in primary human T lymphocytes and adult bone marrow CD34+ cells via electroporation-mediated gene delivery. Gene Therapy 2000; 7: 1431–1437.
Van Tendeloo VF, Van Broeckhoven C, Berneman ZN . Gene therapy: principles and applications to hematopoietic cells. Leukemia 2001; 15: 523–544.
Pfeifer A, Verma IM . Gene therapy: promises and problems. Annu Rev Genomics Hum Genet 2001; 2: 177–211.
Van Tendeloo VF, Van Broeckhoven C, Berneman ZN . Gene-based cancer vaccines: an ex vivo approach. Leukemia 2001; 15: 545–558.
Muller MR, Tsakou G, Grunebach F, Schmidt SM, Brossart P . Induction of chronic lymphocytic leukemia (CLL)-specific CD4- and CD8-mediated T-cell responses using RNA-transfected dendritic cells. Blood 2004; 103: 1763–1769.
Srour EF, Jetmore A, Wolber FM, Plett PA, Abonour R, Yoder MC et al. Homing, cell cycle kinetics and fate of transplanted hematopoietic stem cells. Leukemia 2001; 15: 1681–1684.
Tocci A, Forte L . Mesenchymal stem cell: use and perspectives. Hematol J 2003; 4: 92–96.
Brun AC, Fan X, Bjornsson JM, Humphries RK, Karlsson S . Enforced adenoviral vector-mediated expression of HOXB4 in human umbilical cord blood CD34+ cells promotes myeloid differentiation but not proliferation. Mol Ther 2003; 8: 618–628.
Svedberg H, Richter J, Gullberg U . Forced expression of the Wilms tumor 1 (WT1) gene inhibits proliferation of human hematopoietic CD34(+) progenitor cells. Leukemia 2001; 15: 1914–1922.
Lou J, Xu F, Merkel K, Manske P . Gene therapy: adenovirus-mediated human bone morphogenetic protein-2 gene transfer induces mesenchymal progenitor cell proliferation and differentiation in vitro and bone formation in vivo. J Orthop Res 1999; 17: 43–50.
Tsuda H, Wada T, Ito Y, Uchida H, Dehari H, Nakamura K et al. Efficient BMP2 gene transfer and bone formation of mesenchymal stem cells by a fiber-mutant adenoviral vector. Mol Ther 2003; 7: 354–365.
Herndon TM, Juang YT, Solomou EE, Rothwell SW, Gourley MF, Tsokos GC . Direct transfer of p65 into T lymphocytes from systemic lupus erythematosus patients leads to increased levels of interleukin-2 promoter activity. Clin Immunol 2002; 103: 145–153.
Lai W, Chang CH, Farber DL . Gene transfection and expression in resting and activated murine CD4 T cell subsets. J Immunol Methods 2003; 282: 93–102.
Rufer N, Migliaccio M, Antonchuk J, Humphries RK, Roosnek E, Lansdorp PM . Transfer of the human telomerase reverse transcriptase (TERT) gene into T lymphocytes results in extension of replicative potential. Blood 2001; 98: 597–603.
Schreurs MW, Scholten KB, Kueter EW, Ruizendaal JJ, Meijer CJ, Hooijberg E . In vitro generation and life span extension of human papillomavirus type 16-specific, healthy donor-derived CTL clones. J Immunol 2003; 171: 2912–2921.
Zheng WP, Zhao Q, Zhao X, Li B, Hubank M, Schatz DG et al. Up-regulation of Hlx in immature Th cells induces IFN-gamma expression. J Immunol 2004; 172: 114–122.
Acknowledgements
This work was supported by Grant No. G.0313.01 of the Fund for Scientific Research – Flanders, Belgium (FWO-Vlaanderen), by a grant of the Scientific Committee of the Fortis Bank (FB) Verzekeringen-financed Cancer Research and by a grant of the Belgian Federation against Cancer (BFK). We also acknowledge support from Grant No. 7.0004.03 (Levenslijn) of the FWO-Vlaanderen. VFIVT is a postdoctoral fellow of the FWO-Vlaanderen.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Smits, E., Ponsaerts, P., Lenjou, M. et al. RNA-based gene transfer for adult stem cells and T cells. Leukemia 18, 1898–1902 (2004). https://doi.org/10.1038/sj.leu.2403463
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.leu.2403463
Keywords
This article is cited by
-
CAR T cell therapy for patients with solid tumours: key lessons to learn and unlearn
Nature Reviews Clinical Oncology (2024)
-
Tools for translation: non-viral materials for therapeutic mRNA delivery
Nature Reviews Materials (2017)
-
pEVL: A Linear Plasmid for Generating mRNA IVT Templates With Extended Encoded Poly(A) Sequences
Molecular Therapy - Nucleic Acids (2016)
-
RNA-based, transient modulation of gene expression in human haematopoietic stem and progenitor cells
Scientific Reports (2015)
-
Reporter gene-expressing bone marrow-derived stromal cells are immune-tolerated following implantation in the central nervous system of syngeneic immunocompetent mice
BMC Biotechnology (2009)