Abstract
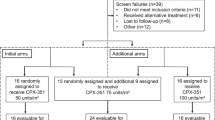
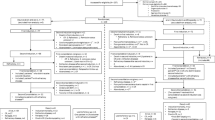
We report the first randomized study assessing the efficacy and safety of daunorubicin (DNR) continuous infusion (CI) compared to the more conventional 30-min infusion (i.v.) in newly diagnosed adult acute lymphoblastic leukemia (ALL). Seventy-seven patients were initially randomized to receive either a 24-h CI DNR (60 mg/m2 days 2–4) (40 patients) or bolus DNR at the same dosage (37 patients) with vincristine (2 mg i.v. days 1, 8, 15) and oral prednisone (60 mg/m2 days 1–15), without hematopoietic growth factor support, as an induction regimen. The distribution of adverse prognostic factors was comparable in the two-induction arm. Acute toxicity was more important in the CI arm. Gram negative infection (9 vs 1 gram negative septicemia, P = 0.01) and infection-related deaths (6 vs 1 deaths, P = NS) occurred more frequently in the CI arm during the induction treatment than in the i.v. arm, leading to the study interruption. Neutropenia but not thrombopenia duration was significantly longer in the CI arm than in the i.v. arm (18 days vs 14 days, P > 0.05 and 16 days vs 12 days, P > 0.05, respectively). Despite a similar CR rate according to the method of DNR administration (68% in the CI DNR arm vs 76% in the i.v. arm after the first course), there was a trend toward higher freedom from relapse (FFR) after DNR CI (48% vs 28% in the i.v. arm at 5 years, P = NS), suggesting that despite this high toxicity, DNR CI may improve the CR quality and decrease further the residual disease.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Hoelzer DF . Therapy of the newly diagnosed adult with acute lymphoblastic leukemia Hematol Oncol Clin North Am 1993 7: 139–160
Copelan EA, McGuire EA . The biology and treatment of acute lymphoblastic leukemia in adults Blood 1995 85: 1151–1168
Pui CH, Evans WE . Acute lymphoblastic leukemia N Engl J Med 1998 339: 605–615
Carlson R, Sikic B . Continuous infusion or bolus injection in cancer chemotherapy Ann Int Med 1983 99: 823–833
Speth P, Linssen P, De Pauw B, De Witte T . Cellular pharmacokinetics of daunomycin administered as continuous intravenous infusion in the treatment of acute non-lymphocytic leukaemia Br J Haematol 1986 63: 603–605
Garnick M, Weiss G, Steele G, Isreael M, Schade D, Sack M, Frei E . Clinical evaluation of long-term, continuous infusion doxorubicin Cancer Treat Rep 1983 67: 133–142
Gottlieb AJ, Weinberg V, Ellison RR, Henderson ES, Terebelo H, Rafla S, Cuttner J, Silver RT, Carey RW, Levy RN, Hutchinson J, Raich P, Cooper M, Wiernik P, Anderson J, Holland J . Efficacy of daunorubicin in the therapy of adult acute lymphocytic leukemia: a prospective randomized trial by cancer and leukemia group B Blood 1984 64: 267–274
Bassan R, Chiodini B, Zucchetti M, Lerede T, Cornelli PE, Cortelazzo S, Barbui T . Short course infusional idarubicin plus intermittent cytarabine and etoposide for refractory hematologic malignancies: clinical and preliminary pharmacological results Haematologica 1998 83: 27–33
Steinherz PG, Redner A, Steinherz L, Meyers P, Tan C, Heller G . Development of a new intensive therapy for acute lymphoblastic leukemia in children at increased risk of early relapse. The Memorial Sloan- Kettering-New York-II protocol Cancer 1993 72: 3120–3130
DeGregorio MW, Carrera CJ, Klock JC, Pegelow CH, Wilbur JR . Cellular and plasma kinetics of daunorubicin given by two methods of administration in a patient with acute leukemia Cancer Treat Rep 1982 66: 2085–2088
Koskela K, Pelliniemi TT, Remes K . VAD regimen in the treatment of resistant multiple myeloma: slow or fast infusion? Leuk Lymphoma 1993 10: 347–351
Lewis J, Meyers F, Tanaka L . Daunomycin administered by continuous intravenous infusion is effective in the treatment of acute nonlymphocytic leukemia Br J Haematol 1985 61: 261–265
Archimbaud E, Anglaret B, Thomas X, Devaux Y, Ffrench M, Sebban C, Troncy J, Fiere D . Continuous-infusion daunorubicin and carboplatin for high-risk acute myeloid leukemia in the elderly Leukemia 1992 6: 776–779
Liso V, Specchia G, Pavone V, Capalbo S, Dione R . Continuous infusion chemotherapy with epirubicin and vincristine in relapsed and refractory acute leukemia Acta Haematol 1990 83: 116–119
Neuendank A, Hartmann R, Buhrer C, Winterhalter B, Klumper E, Veerman AJ, Henze G . Acute toxicity and effectiveness of idarubicin in childhood acute lymphoblastic leukemia Eur J Haematol 1997 58: 326–332
Koc Y, Akpek G, Kansu E, Kars A, Tekuzman G, Baltali E, Guler N, Barista I, Gullu I, Ozisik Y, Firat D . Bolus and continuous infusion mitoxantrone in newly diagnosed adult acute lymphoblastic leukemia: results of two consecutive phase II clinical studies Cancer Invest 1998 16: 355–365
Kantarjian HM, Walters RS, Keating MJ, Smith TL, O'Brien S, Estey EH, Huh YO, Spinolo J, Dicke K, Barlogie B, McCredie K, Freireich E . Results of the vincristine, doxorubicin, and dexamethasone regimen in adults with standard- and high-risk acute lymphocytic leukemia J Clin Oncol 1990 8: 994–1004
Kantarjian HM, O'Brien S, Smith T, Estey EH, Beran M, Preti A, Pierce S, Keating MJ . Acute lymphocytic leukaemia in the elderly: characteristics and outcome with the vincristine-adriamycin-dexamethasone (VAD) regimen Br J Haematol 1994 88: 94–100
Morland BJ, Shaw PJ . Induction toxicity of a modified Memorial Sloan-Kettering-New York II protocol in children with relapsed acute lymphoblastic leukemia: a single institution study Med Pediatr Oncol 1996 27: 139–144
Ottmann OG, Hoelzer D . Growth factors in the treatment of acute lymphoblastic leukemia Leuk Res 1998 22: 1171–1178
Engels EA, Lau J, Barza M . Efficacy of quinolone prophylaxis in neutropenic cancer patients: a meta-analysis J Clin Oncol 1998 16: 1179–1187
Hortobagyi GN . Anthracyclines in the treatment of cancer. An overview Drugs 1997 54: 1–7
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Hunault-Berger, M., Milpied, N., Bernard, M. et al. Daunorubicin continuous infusion induces more toxicity than bolus infusion in acute lymphoblastic leukemia induction regimen: a randomized study. Leukemia 15, 898–902 (2001). https://doi.org/10.1038/sj.leu.2402130
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.leu.2402130
Keywords
This article is cited by
-
Uptake of anthracyclines in vitro and in vivo in acute myeloid leukemia cells in relation to apoptosis and clinical response
European Journal of Clinical Pharmacology (2009)