Abstract
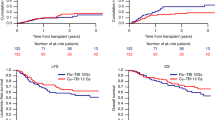
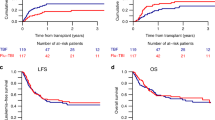
To compare the outcome of hematopoietic stem cell transplantation (HSCT) in pediatric acute lymphoblastic leukemia (ALL) conditioned with two different regimens: (1) single dose of VP16 (60 mg/kg over 4 h) and total body irradiation (TBI; 1200 cGy, in six fractions) or (2) Cyclophosphamide 50 mg/kg over 1 h daily for 4 days followed by the same dose of TBI. One hundred and seven children with ALL received fully matched HSCT from 1990 to 2003 in the Hospital for Sick Children, Toronto. All received cyclosporin A and a short course of methotrexate for graft-versus-host disease (GVHD) prophylaxis. The VP16 group, there were 36 matched related donor transplants (MRD) and 26 matched unrelated donor transplants (MUD), and in the cyclophosphamide group there were 23 MRD and 22 MUD transplants. Neutrophil engraftment occurred at a median of 18 and 17 days for the VP16/TBI and the CY/TBI groups, respectively. The 3 year event-free survival and overall survival were 47±7 and 55±7% for those receiving VP16/TBI, and 51±8 and 53±8% for the CY/TBI group. There were no significant differences in the prevalence of acute or chronic GVHD and transplant-related mortality between the two groups. Both VP16/FTBI and CY/FTBI regimen are equally effective regimens.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Davies SM, Ramsay NK, Klein JP, Weisdorf DJ, Bolwell B, Cahn JY et al. Comparison of preparative regimens in transplants for children with acute lymphoblastic leukemia. J Clin Oncol 2000; 18: 340–347.
Ringden O, Labopin M, Tura S, Arcese W, Iriondo A, Zittoun R et al. A comparison of busulphan versus total body irradiation combined with cyclophosphamide as conditioning for autograft or allograft bone marrow transplantation in patients with acute leukaemia. Acute Leukaemia Working Party of the European Group for Blood and Marrow Transplantation (EBMT). Br J Haematol 1996; 93: 637–645.
Ringden O, Ruutu T, Remberger M, Nikoskelainen J, Volin L, Vindelov L et al. A randomized trial comparing busulfan with total body irradiation as conditioning in allogeneic marrow transplant recipients with leukemia: a report from the Nordic Bone Marrow Transplantation Group. Blood 1994; 83: 2723–2730.
Wachowiak J, Bettoni C, Lange A, Malicki J, Kaczmarek-Kanold M, Gluszak B et al. Can busulfan replace fractionated total body irradiation as conditioning regimen for allogeneic bone marrow transplantation in children with acute lymphoblastic leukemia. Acta Haematol Pol 1995; 26: 377–384.
Shah AJ, Lenarsky C, Kapoor N, Crooks GM, Kohn DB, Parkman R et al. Busulfan and cyclophosphamide as a conditioning regimen for pediatric acute lymphoblastic leukemia patients undergoing bone marrow transplantation. J Pediatr Hematol Oncol 2004; 26: 91–97.
Dai QY, Souillet G, Bertrand Y, Galambrun C, Bleyzac N, Manel AM et al. Antileukemic and long-term effects of two regimens with or without TBI in allogeneic bone marrow transplantation for childhood acute lymphoblastic leukemia. Bone Marrow Transplant 2004; 34: 667–673.
Blume KG, Long GD, Negrin RS, Chao NJ, Kusnierz-Glaz C, Amylon MD . Role of etoposide (VP-16) in preparatory regimens for patients with leukemia or lymphoma undergoing allogeneic bone marrow transplantation. Bone Marrow Transplant 1994; 14 (Suppl 4): S9–S10.
Amylon MD, Co JP, Snyder DS, Donaldson SS, Blume KG, Forman SJ . Allogeneic bone marrow transplant in pediatric patients with high-risk hematopoietic malignancies early in the course of their disease. J Pediatr Hematol Oncol 1997; 19: 54–61.
Suttorp M, Schmitz N, Leuschner S, Appelt M, Rister M, Schaub J . Fractionated total body irradiation plus high-dose VP-16 prior to allogeneic bone marrow transplantation in children with poor risk acute leukaemias. Bone Marrow Transplant 1989; 4 (Suppl 4): 144–148.
Long GD, Amylon MD, Stockerl-Goldstein KE, Negrin RS, Chao NJ, Hu WW et al. Fractionated total-body irradiation, etoposide, and cyclophosphamide followed by allogeneic bone marrow transplantation for patients with high-risk or advanced-stage hematological malignancies. Biol Blood Marrow Transplant 1997; 3: 324–330.
Duerst RE, Horan JT, Liesveld JL, Abboud CN, Zwetsch LM, Senf ES et al. Allogeneic bone marrow transplantation for children with acute leukemia: cytoreduction with fractionated total body irradiation, high-dose etoposide and cyclophosphamide. Bone Marrow Transplant 2000; 25: 489–494.
Toubai T, Tanaka J, Mori A, Hashino S, Kobayashi S, Ota S et al. Efficacy of etoposide, cyclophosphamide, and total body irradiation in allogeneic bone marrow transplantation for adult patients with hematological malignancies. Clin Transplant 2004; 18: 552–557.
Thomas ED, Storb R, Clift RA, Fefer A, Johnson L, Neiman PE et al. Bone-marrow transplantation. N Engl J Med 1975; 292: 832–843, 895–902.
Goodman JL, Winston DJ, Greenfield RA, Chandrasekar PH, Fox B, Kaizer H et al. A controlled trial of fluconazole to prevent infections in patients undergoing bone marrow transplantation. N Engl J Med 1992; 326: 845–851.
Goodrich JM, Bowden RA, Fisher L, Keller C, Schoch G, Meyers JD . Ganciclovir prophylaxis to prevent cytomegalovirus disease after allogeneic marrow transplant. Ann Intern Med 1993; 18: 173–178.
Boeckh M, Gooley TA, Myerson D, Cunningham T, Schoch G, Bowden RA . Cytomegalovirus pp65 antigenemia-guided early treatment with ganciclovir versus ganciclovir at engraftment after allogeneic marrow transplantation: a randomized-blind study. Blood 1996; 88: 4063–4071.
Glucksberg H, Storb R, Fefer A, Buckner CD, Neiman PE, Clift RA et al. Clinical manifestation of graft-versus-host disease in human recipients of marrow from HLA-matched sibling donors. Transplantation 1974; 18: 295–304.
Atkinson K, Horowitz MM, Gale RP, Lee MB, Rimm AA, Bortin MM . Consensus among bone marrow transplanters for diagnosis, grading and treatment of chronic graft-versus-host disease. Committee of the International Bone Marrow Transplant Registry. Bone Marrow Transplant 1989; 4: 247–254.
Schwerdtfeger R, Schmid H, Baurmann H, Kleiner S, Zeiler T, Henze G et al. VP16 and TBI as conditioning regimen for allogeneic BMT in patients with high risk and relapsed ALL and NHL. Bone Marrow Transplant 1991; 7 (Suppl 2): 131.
Kosaka Y, Koh K, Kinukawa N, Wakazono Y, Isoyama K, Oda T et al. Infant acute lymphoblastic leukemia with MLL gene rearrangements: outcome following intensive chemotherapy and hematopoietic stem cell transplantation. Blood 2004; 104: 3527–3534.
Sanders JE, Im HJ, Hoffmeister PA, Gooley TA, Woolfrey AE, Carpenter PA et al. Allogeneic hematopoietic cell transplantation for infants with acute lymphoblastic leukemia. Blood 2005; 105: 3749–3756.
Jamieson CH, Amylon MD, Wong RM, Blume KG . Allogeneic hematopoietic cell transplantation for patients with high-risk acute lymphoblastic leukemia in first or second complete remission using fractionated total-body irradiation and high-dose etoposide: a 15-year experience. Exp Hematol 2003; 31: 981–986.
Dopfer R, Henze G, Bender-Gotze C, Ebell W, Ehninger G, Friedrich W et al. Allogeneic bone marrow transplantation for childhood acute lymphoblastic leukemia in second remission after intensive primary and relapse therapy according to the BFM- and CoALL-protocols: results of the German Cooperative Study. Blood 1991; 78: 2780–2784.
Locatelli F, Zecca M, Messina C, Rondelli R, Lanino E, Sacchi N et al. Improvement over time in outcome for children with acute lymphoblastic leukemia in second remission given hematopoietic stem cell transplantation from unrelated donors. Leukemia 2002; 16: 2228–2237.
Zikos P, Van Lint MT, Lamparelli T, Gualandi F, Occhini D, Bregante S et al. Allogeneic hemopoietic stem cell transplantation for patients with high risk acute lymphoblastic leukemia: favorable impact of chronic graft-versus-host disease on survival and relapse. Haematologica 1998; 83: 896–903.
Gustafsson Jernberg A, Remberger M, Ringden O, Winiarski J . Graft-versus-leukaemia effect in children: chronic GVHD has a significant impact on relapse and survival. Bone Marrow Transplant 2003; 31: 175–181.
Locatelli F, Zecca M, Rondelli R, Bonetti F, Dini G, Prete A et al. Graft versus host disease prophylaxis with low-dose cyclosporine-A reduces the risk of relapse in children with acute leukemia given HLA-identical sibling bone marrow transplantation: results of a randomized trial. Blood 2000; 95: 1572–1579.
Zecca M, Prete A, Rondelli R, Lanino E, Balduzzi A, Messina C et al. Chronic graft-versus-host disease in children: incidence, risk factors, and impact on outcome. Blood 2002; 100: 1192–1200.
Nordlander A, Mattsson J, Ringden O, Leblanc K, Gustafsson B, Ljungman P et al. Graft-versus-host disease is associated with a lower relapse incidence after hematopoietic stem cell transplantation in patients with acute lymphoblastic leukemia. Biol Blood Marrow Transplant 2004; 10: 195–203.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Gassas, A., Sung, L., Saunders, E. et al. Comparative outcome of hematopoietic stem cell transplantation for pediatric acute lymphoblastic leukemia following cyclophosphamide and total body irradiation or VP16 and total body irradiation conditioning regimens. Bone Marrow Transplant 38, 739–743 (2006). https://doi.org/10.1038/sj.bmt.1705515
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.bmt.1705515
Keywords
This article is cited by
-
How to Treat Relapsed Acute Lymphoblastic Leukemia: Transplant vs. Conventional Chemotherapy
The Indian Journal of Pediatrics (2013)
-
Longitudinal health-related quality of life outcomes and related factors after pediatric SCT
Bone Marrow Transplantation (2009)
-
Hematopoietic stem cell transplantation for pediatric autoimmune disease: where we stand and where we need to go
Bone Marrow Transplantation (2009)
-
Early lymphocyte recovery post-allogeneic hematopoietic stem cell transplantation is associated with significant graft-versus-leukemia effect without increase in graft-versus-host disease in pediatric acute lymphoblastic leukemia
Bone Marrow Transplantation (2008)
-
Allogeneic haematopoietic stem cell transplant in Philadelphia-positive acute lymphoblastic leukaemia
Bone Marrow Transplantation (2008)