Abstract
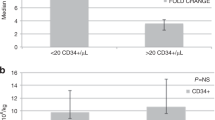
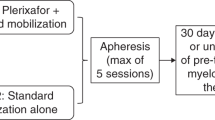
The use of a combination of G-CSF and GM-CSF versus G-CSF alone, after cyclophosphamide (4 g/m2) was compared in two randomized phase III studies, including 120 patients. In study A, 60 patients received 5 × 2 μg/kg/day of G-CSF and GM-CSF compared to 5 μg/kg/day of G-CSF. In study B, 60 patients received 2.5 × 2 μg/kg/day G-CSF and GM-CSF compared to G-CSF alone (5 μg/kg/day). With the aim to collect at least 5 × 106/kg CD34 cells in a maximum of three large volume leukapherises (LK), 123 LK were performed in study A, showing a significantly higher number of patients reaching 10 × 106/kg CD34 cells (21/29 in G+GM-CSF arm vs 11/27 in G-CSF arm, P=0.00006). In study B, 109 LK were performed, with similar results (10/27 vs 15/26, P=0.003). In both the study, the total harvest of CD34 cells/kg was twofold higher in G-CSF plus GM-CSF group (18.3 × 106 in study A and 15.85 × 106 in study B) than in G-CSF group (9 × 106 in study A and 8.1 × 106 in study B), a significant difference only seen in multiple myeloma, with no significant difference in terms of mobilized myeloma cells between G-CSF and GM-CSF groups.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout





Similar content being viewed by others
References
Attal M, Harousseau JL, Stoppa AM, Sotto JJ, Fuzibet JG, Rossi JF et al. A prospective, randomized trial of autologous bone marrow transplantation and chemotherapy in multiple myeloma. N Engl J Med 1996; 335: 91–97.
Harousseau JL . Stem cell transplantation in multiple myeloma (0, 1, or 2). Curr Opin Oncol 2005; 17: 93–98.
Gorin NC . Autologous stem cell transplantation in hematological malignancies. Springer Semin Immunopathol 2004; 26: 3–30.
Philip T, Guglielmi C, Hagenbeek A, Somers R, Van der Lelie H, Bron D et al. Autologous bone marrow transplantation as compared with salvage chemotherapy in relapses of chemotherapy-sensitive non-Hodgkin's lymphoma. N Engl J Med 1995; 333: 1540–1545.
Gratwohl A, Schmid O, Baldomero H, Horisberger B, Urbano-Ispizua A . Accreditation Committee of the European Group for Blood and Marrow Transplantation. Haematopoietic stem cell transplantation (HSCT) in Europe 2002. Changes in indication and impact of team density. A report of the EBMT activity survey. Bone Marrow Transplant 2004; 34: 855–875.
Demirer T, Buckner CD, Bensinger WI . Optimization of stem cell mobilization. Stem Cells 1996; 14: 106–116.
Lane TA, Law P, Maruyama M, Young D, Burgess J, Mullen M et al. Harvesting and enrichment of HPC mobilized into the peripheral blood of normal donors by GM-CSF or G-CSF: potential role in allogenic transplantation. Blood 1995; 85: 275–282.
Peters WP, Rosner G, Ross M, Vredenburgh J, Meisenberg B, Gilbert C et al. Comparative effect of GM-CSF and G-CSF on priming of peripheral blood progenitor cells for use with autologous bone marrow after high dose chemotherapy. Blood 1993; 81: 1709–1719.
Gazitt Y . Comparison between granulocyte colony-stimulating factor and granulocyte-macrophage colony-stimulating factor in the mobilization of peripheral blood stem cells. Curr Opin Hematol 2002; 9: 190–198.
Lyman SD . Biologic effects and potential clinical applications of Flt3 ligand. Curr Opin Hematol 1998; 5: 192–196.
Haas R, Ehrhardt R, Witt B, Goldschmidt H, Hohaus S, Pforsich M et al. Autografting with peripheral blood stem cells mobilized by sequential interleukin-3/granulocyte-macrophage colony-stimulating factor following high-dose chemotherapy in non-Hodgkin's lymphoma. Bone Marrow Transplant 1993; 12: 643–649.
Stiff P, Gingrich R, Luger SA, Wyres MR, Brown RA, LeMaistre CF et al. Randomized phase 2 study of PBPC mobilization by stem cell factor and filgrastim in heavily pretreated patients with Hodgkin's disease or non-Hodgkin's lymphoma. Bone Marrow Transplant 2000; 26: 471–481.
Prosper F, Sola C, Hornedo J, Arbona C, Menendez P, Orfao A et al. Mobilization of peripheral blood progenitor cells with a combination of cyclophosphamide, r-metHuSCF and filgrastim in patients with breast cancer previously treated with chemotherapy. Leukemia 2003; 17: 437–441.
Waller CF, von Lintig F, Daskalakis A, Musahl V, Lange W . Mobilization of peripheral blood progenitor cells in patients with breast cancer: a prospective randomized trial comparing rhG-CSF with the combination of rhG-CSF plus rhEpo after VIP-E chemotherapy. Bone Marrow Transplant 1999; 24: 19–24.
Liles WC, Rodger E, Broxmeyer HE, Dehner C, Badel K, Calandra G et al. Augmented mobilization and collection of CD34+ hematopoietic cells from normal human volunteers stimulated with granulocyte-colony-stimulating factor by single-dose administration of AMD3100, a CXCR4 antagonist. Transfusion 2005; 45: 295–300.
Ozer H, Armitage JO, Bennett CL, Crawford J, Demetri GD, Pizzo PA et al. 2000 update of recommendations for the use of hematopoietic colony-stimulating factors: evidence-based, clinical practice guidelines. J Clin Oncol 2000; 18: 3558–3585.
Andre M, Baudoux E, Bron D, Canon JL, D'Hondt V, Fassotte MF et al. Phase III randomized study comparing 5 or 10 microg per kg per day of filgrastim for mobilization of peripheral blood progenitor cells with chemotherapy, followed by intensification and autologous transplantation in patients with nonmyeloid malignancies. Transfusion 2003; 43: 50–57.
Jones HM, Jones SA, Watts MJ . The effects of variation of the dose and schedule of G-CSF administration after low dose cyclophosphamide (1.5 g/m2) on both neutrophil and peripheral blood haemopoietic progenitor cell levels. Blood 1993; 82 (Suppl 1): 233a.
Carrion R, Serrano D, Gomez-Pineda A, Diez-Martin JL . A randomised study of 10 microg/kg/day (single dose) vs 2 × 5 microg/kg/day (split dose) G-CSF as stem cell mobilisation regimen in high-risk breast cancer patients. Bone Marrow Transplant 2003; 32: 563–567.
Green MD, Koelbl H, Baselga J, Galid A, Guillem V, Gascon P et al. A randomized double-blind multicenter phase III study of fixed-dose single-administration pegfilgrastim versus daily filgrastim in patients receiving myelosuppressive chemotherapy. Ann Oncol 2003; 14: 29–35.
Siena S, Schiavo R, Pedrazzoli P, Carlo-Stella C . Therapeutic relevance of CD34+ cell dose in blood cell transplantation for cancer therapy. J Clin Oncol 2000; 18: 1360–1377.
Weaver CH, Hazelton B, Birch R, Palmer P, Allen C, Schwartzberg L et al. An analysis of engraftment kinetics as a function of the CD34 content of peripheral blood progenitor cell collections in 692 patients after the administration of myeloablative chemotherapy. Blood 1995; 86: 3961–3969.
Schulman KA, Birch R, Zhen B, Pania N, Weaver CH . Effect of CD34+ cell dose on resource utilization in patients after high-dose chemotherapy with peripheral-blood stem-cell support. J Clin Oncol 1999; 17: 1227.
Winter JN, Lazarus HM, Rademaker A, Villa M, Mangan C, Tallman M et al. Phase I/II study of combined granulocyte colony-stimulating factor and granulocyte-macrophage colony-stimulating factor administration for the mobilization of hematopoietic progenitor cells. J Clin Oncol 1996; 14: 277–286.
Charrier S, Chollet P, Bay JO, Cure H, Kwiatkowski F, Portefaix G et al. Hematological recovery and peripheral blood progenitor cell mobilization after induction chemotherapy and GM-CSF plus G-CSF in breast cancer. Bone Marrow Transplant 2000; 252: 705–710.
Bolwell B, Goormastic M, Yanssens T, Dannley R, Baucco P, Fishleder A et al. Comparison of G-CSF with GM-CSF for mobilizing peripheral blood progenitor cells and for enhancing marrow recovery after autologous bone marrow transplant. Bone Marrow Transplant 1994; 14: 913–918.
Spitzer G, Adkins D, Mathews M, Velasquez W, Bowers C, Dunphy F et al. Randomized comparison of G-CSF + GM-CSF vs G-CSF alone for mobilization of peripheral blood stem cells: effects on hematopoietic recovery after high-dose chemotherapy. Bone Marrow Transplant 1997; 20: 921–930.
Weisdorf D, Miller J, Verfaillie C, Burns L, Wagner J, Blazar B et al. Cytokine-primed bone marrow stem cells vs peripheral blood stem cells for autologous transplantation: a randomized comparison of GM-CSF vs G-CSF. Biol Blood Marrow Transplant 1997; 3: 217–223.
Hohaus S, Martin H, Wassmann B, Egerer G, Haus U, Farber L et al. Recombinant human granulocyte and granulocyte-macrophage colony-stimulating factor (G-CSF and GM-CSF) administered following cytotoxic chemotherapy have a similar ability to mobilize peripheral blood stem cells. Bone Marrow Transplant 1998; 22: 625–630.
Comenzo RL, Sanchorawala V, Fisher C, Akpek G, Farhat M, Cerda S et al. Intermediate-dose intravenous melphalan and blood stem cells mobilized with sequential GM+G-CSF or G-CSF alone to treat AL (amyloid light chain) amyloidosis. Br J Haematol 1999; 104: 539–553.
Siena S, Bregni M, Gianni AM . Mobilization of peripheral blood progenitor cells for autografting: chemotherapy and G-CSF or GM-CSF. Baillieres Best Pract Res Clin Haematol 1999; 12: 27–39.
Madero L, Gonzalez-Vicent M, Molina J, Madero R, Quintero V, Diaz MA . Use of concurrent G-CSF + GM-CSF vs G-CSF alone for mobilization of peripheral blood stem cells in children with malignant disease. Bone Marrow Transplant 2000; 26: 365–369.
Weaver CH, Schulman KA, Wilson-Relyea B, Birch R, West W, Buckner CD . Randomized trial of filgrastim, sargramostim, or sequential sargramostim and filgrastim after myelosuppressive chemotherapy for the harvesting of peripheral-blood stem cells. J Clin Oncol 2000; 18: 43–53.
Koc ON, Gerson SL, Cooper BW, Laughlin M, Meyerson H, Kutteh L et al. Randomized cross-over trial of progenitor-cell mobilization: high-dose cyclophosphamide plus granulocyte colony-stimulating factor (G-CSF) versus granulocyte-macrophage colony-stimulating factor plus G-CSF. J Clin Oncol 2000; 18: 1824–1830.
Gazitt Y, Callander N, Freytes CO, Shaughnessy P, Liu Q, Tsai TW et al. Peripheral blood stem cell mobilization with cyclophosphamide in combination with G-CSF, GM-CSF, or sequential GM-CSF/G-CSF in non-Hodgkin's lymphoma patients: a randomized prospective study. J Hematother Stem Cell Res 2000; 9: 737–748.
Gazitt Y, Shaughnessy P, Liu Q . Differential mobilization of CD34+ cells and lymphoma cells in non-Hodgkin's lymphoma patients mobilized with different growth factors. J Hematother Stem Cell Res 2001; 10: 167–176.
Armitage JO . Emerging applications of recombinant human granulocyte-macrophage colony-stimulating factor. Blood 1998; 92: 4491–4508.
Sutherland DR, Anderson L, Keeney M, Nayar R, Chin-Yee I . The ISHAGE guidelines for CD34+ cell determination by flow cytometry. International Society of Hematotherapy and Graft Engineering. J Hematother 1996; 5: 213–226.
Costes V, Magen V, Legouffe E, Durand L, Baldet P, Rossi JF et al. The Mi15 monoclonal antibody (anti-syndecan-1) is a reliable marker for quantifying plasma cells in paraffin-embedded bone marrow biopsy specimens. Hum Pathol 1999; 30: 1405–1411.
Duggan PR, Guo D, Luider J, Auer I, Klassen J, Chaudhry A et al. Predictive factors for long-term engraftment of autologous blood stem cells. Bone Marrow Transplant 2000; 26: 1299–1304.
Uyl-de Groot CA, Huijgens PC, Rutten FF . Colony-stimulating factors and peripheral blood progenitor cell transplantation, benefits and costs. Pharmaco Economics 1996; 10: 23–35.
Bensinger W, Appelbaum F, Rowley S, Storb R, Sanders J, Lilleby K et al. Factors that influence collection and engraftment of autologous peripheral-blood stem cells. J Clin Oncol 1995; 13: 2547–2555.
Ketterer N, Salles G, Raba M, Espinousse D, Sonet A, Tremisi P et al. High CD34 (+) cell counts decrease hematologic toxicity of autologous peripheral blood progenitor cell transplantation. Blood 1998; 91: 3148–3155.
Dercksen MW, Rodenhuis S, Dirkson MK, Schaasberg WP, Baars JW, van der Waal E et al. Subsets of CD34+ cells and rapid hematopoietic recovery after peripheral-blood stem-cell transplantation. J Clin Oncol 1995; 13: 1922–1932.
Wahlin A, Eriksson M, Hultdin M . Relation between harvest success and outcome after autologous peripheral blood stem cell transplantation in multiple myeloma. Eur J Haematol 2004; 73: 263–268.
Porrata LF, Gertz MA, Geyer SM, Litzow MR, Gastineau DA, Moore SB et al. The dose of infused lymphocytes in the autograft directly correlates with clinical outcome after autologous peripheral blood hematopoietic stem cell transplantation in multiple myeloma. Leukemia 2004; 18: 1085–1092.
O'Neil DW, Adams S, Bhardwaj N . Manipulating dendritic cell biology for the active immunotherapy cancer. Blood 2004; 104: 2235–2246.
Dranoff G . GM-CSF-based cancer vaccines. Immunol Rev 2002; 188: 147–154.
Gazitt Y . Immunologic profiles of effector cells and peripheral blood stem cells mobilized with different hematopoietic growth factors. Stem Cells 2000; 18: 390–398.
Koumakis G, Vassilomanolakis M, Hatzichristou H, Barbounis V, Filis J, Papanastasiou K et al. Predictive factors affecting mobilization and peripheral blood stem cell (PBSC) collection using single apheresis (SA) for rescuing patients after high-dose chemotherapy (HD.CHE) in various malignancies. Bone Marrow Transplant 1996; 18: 1065–1072.
Haas R, Möhle R, Frühauf S, Goldschmidt H, Goldschmidt H, Witt B et al. Patient characteristics associated with successful mobilizing and autografting of peripheral blood progenitor cells in malignant lymphoma. Blood 1994; 83: 3787–3794.
von Lindern M, Zauner W, Mellitzer G, Steinlein P, Fritsch G, Huber K et al. The glucocorticoid receptor cooperates with the erythropoietinreceptor and c-Kit to enhance and sustain proliferation of erythroid progenitors in vitro. Blood 1999; 94: 550–559.
Dror Y, Ward AC, Touw IP, Freedman MH . Combined corticosteroid/granulocyte colony-stimulating factor (G-CSF) therapy in the treatment of severe congenital neutropenia unresponsive to G-CSF: Activated glucocorticoid receptors synergize with G-CSF signals. Exp Hematol 2000; 28: 1381–1389.
Armitage S, Hargreaves R, Samson D, Brennan M, Kanfer E, Navarrete C . CD34 counts to predict the adequate collection of peripheral blood progenitor cells. Bone Marrow Transplant 1997; 20: 587–591.
Möhle R, Murea S, Pförsich M, Witt B, Haas R . Estimation of the progenitor cell yield in a leukapheresis product by previous measurement of CD34+ cells in the peripheral blood. Vox Sang 1996; 71: 90–96.
Rill DR, Moen RC, Buschle M, Bartholomew C, Foreman NK, Mirro Jr J et al. An approach for the analysis of relapse and marrow reconstitution after autologous marrow transplantation using retrovirus-mediated gene transfer. Blood 1992; 79: 2694–2700.
Vora AJ, Toh CH, Peel J, Greaves M . Use of granulocyte colony-stimulating factor (G-CSF) for mobilizing peripheral blood stem cells:risk of mobilizing clonal myeloma cells in patients with bone marrow infiltration. Br J Haematol 1994; 86: 180–182.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Quittet, P., Ceballos, P., Lopez, E. et al. Low doses of GM-CSF (molgramostim) and G-CSF (filgrastim) after cyclophosphamide (4 g/m2) enhance the peripheral blood progenitor cell harvest: results of two randomized studies including 120 patients. Bone Marrow Transplant 38, 275–284 (2006). https://doi.org/10.1038/sj.bmt.1705441
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.bmt.1705441
Keywords
This article is cited by
-
Intermediate-dose Ara-C plus G-CSF for stem cell mobilization in patients with lymphoid malignancies, including predicted poor mobilizers
Bone Marrow Transplantation (2013)
-
Improving stem cell mobilization strategies: future directions
Bone Marrow Transplantation (2009)