Summary:
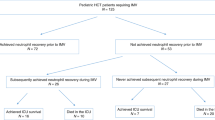
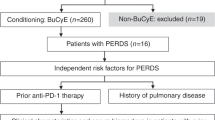
Exacerbation of prior pulmonary involvement may occur during neutropenia recovery. Granulocyte colony-stimulating factor (G-CSF)-related pulmonary toxicity has been documented in cancer patients, and experimental models suggest a role for G-CSF in acute lung injury during neutropenia recovery. We reviewed 20 cases of noncardiac acute respiratory failure during G-CSF-induced neutropenia recovery. Half the patients had received hematopoietic stem cell transplants. All patients experienced pulmonary infiltrates during neutropenia followed by respiratory status deterioration coinciding with neutropenia recovery. Neutropenia duration was 10 (4–22) days, and time between respiratory symptoms and the first day with more than 1000 leukocytes/mm3 was 1 (−0.5 to 2) day. Of the 20 patients, 16 received invasive or noninvasive mechanical ventilation, including 14 patients with acute respiratory distress syndrome (ARDS). Five patients died, with refractory ARDS. In patients with pulmonary infiltrates during neutropenia, G-CSF-induced neutropenia recovery carries a risk of respiratory status deterioration with acute lung injury or ARDS. Clinicians must maintain a high index of suspicion for this diagnosis, which requires eliminating another cause of acute respiratory failure, G-CSF discontinuation and ICU transfer for early supportive management including diagnostic confirmation and noninvasive mechanical ventilation.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Kress JP, Christenson J, Pohlman AS et al. Outcomes of critically ill cancer patients in a University Hospital Setting. Am J Respir Crit Care Med 1999; 160: 1957–1961.
Ewig S, Torres A, Riquelme R et al. Pulmonary complications in patients with hematological malignancies treated at a respiratory ICU. Eur Respir J 1998; 12: 116–122.
Blot F, Guiguet M, Nitenberg G et al. Prognostic factors for neutropenic patients in an intensive care unit: respective roles of underlying malignancies and acute organ failures. Eur J Cancer 1997; 33: 1031–1037.
Azoulay E, Recher C, Alberti C et al. B. Changing use of intensive care for hematological patients: the example of multiple myeloma. Intensive Care Med 199; 25: 1395–1401.
Azoulay E, Thiéry G, Chevret S et al. The prognosis of acute respiratory failure in critically ill cancer patients. Medicine 2004; 83: 1–11.
Hilbert G, Gruson D, Vargas F et al. Noninvasive ventilation in immunosuppressed patients with pulmonary infiltrates, fever, and acute respiratory failure. N Engl J Med 2001; 344: 481–487.
Azoulay E, Alberti C, Bornstain C et al. Improved survival in cancer patients requiring mechanical ventilatory support: Impact of noninvasive mechanical ventilatory support. Crit Care Med 2001; 29: 519–525.
Cordonnier C, Fleury-Feith J, Escudier E et al. Secondary alveolar proteinosis is a reversible cause of respiratory failure in leukemic patients. Am J Respir Crit Care Med 1994; 149: 788–794.
Azoulay E, Fieux F, Moreau D et al. Acute monocytic leukemia presenting as acute respiratory failure. Am J Respir Crit Care Med 2003; 167: 1329–1333.
Rinaldo JE, Borovetz H . Deterioration of oxygenation and abnormal lung microvascular permeability during resolution of leukopenia in patients with diffuse lung injury. Am Rev Respir Dis 1985; 131: 579–583.
Azoulay E, Darmon M, Delclaux C et al. Deterioration of previous acute lung injury during neutropenia recovery. Crit Care Med 2002; 30: 781–786.
Lieschke GJ, Burgess AW . Granulocyte colony-stimulating factor and granulocyte-macrophage colony-stimulating factor (1). N Engl J Med 1992; 327: 28–35.
Lieschke GJ, Burgess AW . Granulocyte colony-stimulating factor and granulocyte-macrophage colony-stimulating factor (2). N Engl J Med 1992; 327: 99–106.
Pfreundschuh M, Trümper L, Kloess M et al. Two-weekly or 3-weekly CHOP chemotherapy with or without etoposide for the treatment of young patients with good prognosis (normal LDH) aggressive lymphomas: results of the NHL-B1 trial of the DSHNHL. Blood 2004; 104: 626–633.
Pfreundschuh M, Trümper L, Kloess M et al. Two-weekly or 3-weekly CHOP chemotherapy with or without etoposide for the treatment of elderly patients with aggressive lymphomas: results of the NHL-B2 trial of the DSHNHL. Blood 2004; 104: 634–641.
Azoulay E, Attalah H, Harf A et al. Granulocyte colony-stimulating factor or neutrophil-induced pulmonary toxicity: myth or reality? Chest 2001; 120: 1695–1701.
Takatsuka H, Takemoto Y, Mori A et al. Common features in the onset of ARDS after administration of granulocyte colony-stimulating factor. Chest 2002; 121: 1716–1720.
Azoulay E, Attalah H, Yang K et al. Exacerbation with granulocyte colony-stimulating factor of prior acute lung injury during neutropenia recovery in rats. Crit Care Med 2003; 31: 157–165.
Le Gall JR, Lemeshow S, Saulnier F . A new Simplified Acute Physiology Score (SAPS II) based on a European/North American multicenter study [published erratum appears in JAMA 1994 May 4; 271(17): 1321]. JAMA 1993; 270: 2957–2963.
Le Gall JR, Klar J, Lemeshow S et al. The logistic organ dysfunction system, a new way to assess organ dysfunction in the intensive care unit. JAMA 1996; 276: 802–810.
Bernard GR, Artigas A, Brigham KL et al. The American–European Consensus Conference on ARDS: définitions, mechanisms, relevant outcomes, and clinical trial coordination. Am J Respir Crit Care Med. 1994; 149: 818–824.
Wilczynski SW, Erasmus JJ, Petros WP et al. Delayed pulmonary toxicity syndrome following high-dose chemotherapy and bone marrow transplantation for breast cancer. Am J Respir Crit Care Med 1998; 157: 565–573.
Glauser FL, Fairman RP . The uncertain role of the neutrophil increased permeability pulmonary edema. Chest 1985; 88: 601–607.
Tate RM, Repine JE . Neutrophils and the adult respiratory distress syndrome. Am Rev Respir Dis 1983; 128: 552–559.
Maunder RJ, Hackman RC, Riff E et al. Occurence of the adult respiratory distress syndrome in neutropenic patients. Am Rev Respir Dis 1986; 133: 313–316.
Ognibene FP, Martin SE, Parker MM et al. Adult respiratory distress syndrome in patients with severe neutropenia. N Engl J Med 1986; 315: 547–551.
King J, Deboisblanc BP, Mason CM et al. Effect of granulocyte colony-stimulating factor on acute lung injury in the rat. Am J Respir Crit Care Med 151; 302: 1995.
Azoulay E, Herigault S, Levame M et al. Effect of granulocyte colony-stimulating factor on bleomycin-induced acute lung injury and pulmonary fibrosis. Crit Care Med 2003; 31: 1442–1448.
Aggarwal A, Baker CS, Evans TW, Haslam PL . G-CSF and IL-8 but not GM-CSF correlate with severity of pulmonary neutrophilia in acute respiratory distress syndrome. Eur Respir J 2000; 15: 895–901.
Wiedermann FJ, Mayr AJ, Hobisch-Hagen P et al. Association of endogenous G-CSF with anti-inflammatory mediators in patients with acute respiratory distress syndrome. J Interferon Cytokine Res 2003; 23: 729–736.
Acknowledgements
We thank A Wolfe MD for helping with this manuscript.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Karlin, L., Darmon, M., Thiéry, G. et al. Respiratory status deterioration during G-CSF-induced neutropenia recovery. Bone Marrow Transplant 36, 245–250 (2005). https://doi.org/10.1038/sj.bmt.1705037
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.bmt.1705037
Keywords
This article is cited by
-
The Care of the Leukemic Patients in Times of SARS-CoV-2
Current Oncology Reports (2021)
-
Influence of neutropenia on mortality of critically ill cancer patients: results of a meta-analysis on individual data
Critical Care (2018)
-
Consensus statement for cancer patients requiring intensive care support
Annals of Hematology (2018)
-
Prise en charge du patient neutropénique en réanimation (nouveau-nés exclus). Recommandations d’un panel d’experts de la Société de réanimation de langue française (SRLF) avec le Groupe francophone de réanimation et urgences pédiatriques (GFRUP), la Société française d’anesthésie et de réanimation (Sfar), la Société française d’hématologie (SFH), la Société française d’hygiène hospitalière (SF2H) et la Société de pathologies infectieuses de langue française (SPILF)
Médecine Intensive Réanimation (2017)
-
Neutropenic sepsis is associated with distinct clinical and biological characteristics: a cohort study of severe sepsis
Critical Care (2016)