Summary:
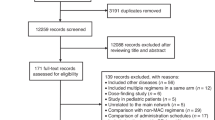
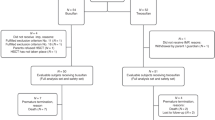
We evaluated the 100-day mortality rates associated with busulfan-based myeloablative conditioning regimens based on data from 1812 chronic myelogenous leukemia patients who underwent allogeneic blood or marrow transplantation (allotx). In all, 47 patients received intravenous (i.v.) busulfan and cyclophosphamide (i.v.BuCy2) with allotx at MD Anderson Cancer Center (MDACC) during 1995–1999. The remaining 1765 patients, whose data were supplied by the International Bone Marrow Transplant Registry (IBMTR), received alternative preparative regimens, primarily Cy-total body irradiation (∼45%) or oral BuCy (∼35%) during 1997–1998. As patients were not randomized between conditioning regimens, the i.v.BuCy2-versus-alternative treatment effect is confounded with a possible center effect due to nontreatment differences associated with factors differing between MDACC and the IBMTR centers. Additional complications are that the i.v.BuCy2-MDACC patients all survived 100 days, and three prognostic subgroups were included. Bayesian sensitivity analyses were performed to assess treatment effect on the probability of 100-day mortality, over a range of possible MDACC-versus-IBMTR center effects. For these patients, the posterior probability that i.v.BuCy2 was superior to alternative conditioning regimens ranges from 0.54 to 0.99, depending on prognosis and the magnitude of the assumed center effect.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Horowitz MM . Results of allogeneic stem cell transplantation for malignant disorders. In: Hoffman R, Benz Jr EJ, Shattil SJ, Fine B, Cohen H, Silberstein LE, McGlave P (eds). Hematology, Basic Principles and Practice, 3rd edn. Churchill Livingston, New York, NY, 2000; pp 1573–1587.
International Bone Marrow Transplant Registry. September 2000.
Bushhouse S, Ramsay NK, Pescovitz OH et al. Growth in children following irradiation for bone marrow transplantation. Am J Ped Hematol/Oncol 1989; 11: 134–140.
Sanders JE . Bone marrow transplantation for pediatric leukemia. Pediat Ann 1991; 20: 671–676.
Liesner RJ, Leiper AD, Hann IM et al. Late effects of intensive treatment for acute myeloid leukemia and myelodysplasia in childhood. J Clin Oncol 1994; 12: 916–924.
Cohen A, van-Lint MT, Uderzo C et al. Growth in patients after allogeneic bone marrow transplant for hematological diseases in childhood. Bone Marrow Transplant 1995; 15: 343–348.
Bhatia S, Ramsay NK, Steinbuch M et al. Malignant neoplasms following bone marrow transplantation. Blood 1996; 87: 3633–3639.
Chou RH, Wong GB, Kramer JH et al. Toxicities of total-body irradiation for pediatric bone marrow transplantation. Int J Radiat Oncol Biol Phys 1996; 34: 843–851.
Deeg HJ, Socié G, Schoch G et al. Malignancies after marrow transplantation for aplastic anemia and Fanconi anemia: a joint Seattle and Paris analysis of results in 700 patients. Blood 1996; 87: 386–392.
Kony SJ, de Vathaire F, Chompret A et al. Radiation and genetic factors in the risk of second malignant neoplasms after a first cancer in childhood. Lancet 1997; 350: 91–95.
Deeg HJ, Socié G . Malignancies after hematopoietic stem cell transplantation: many questions, some answers. Blood 1998; 91: 1833–1844.
Socié G, Curtis RE, Deeg HJ et al. New malignant diseases after allogeneic marrow transplantation for childhood acute leukemia. J Clin Oncol 2000; 18: 348–357.
Santos GW, Tutschka PJ, Brookmeyer R et al. Marrow transplantation for acute nonlymphocytic leukemia after treatment with busulfan and cyclophosphamide. N Engl J Med 1983; 309: 1347–1353.
Lu C, Braine HG, Kaizer H et al. Preliminary results of high-dose busulfan and cyclophosphamide with syngeneic or autologous bone marrow rescue. Cancer Treat Rep 1984; 68: 711–717.
Tutschka PJ, Copelan EA, Klein JP . Bone marrow transplantation for leukemia following a new busulfan and cyclophosphamide regimen. Blood 1987; 70: 1382–1388.
Clift RA, Buckner CD, Thomas ED et al. Marrow transplantation for chronic myeloid leukemia: a randomized study comparing cyclophosphamide and total body irradiation with busulfan and cyclophosphamide. Blood 1994; 84: 2036–2043.
Clift RA, Radich J, Appelbaum FR et al. Long-term follow-up of a randomized study comparing cyclophosphamide and total body irradiation with busulfan and cyclophosphamide for patients receiving allogeneic marrow transplants during chronic phase of chronic myeloid leukemia. Blood 1999; 94: 3960–3962.
Grochow LB, Jones RJ, Brundrett RB et al. Pharmacokinetics of busulfan: correlation with veno-occlusive disease in patients undergoing bone marrow transplantation. Cancer Chemother Pharmacol 1989; 25: 55–61.
Grochow LB . Busulfan disposition: the role of therapeutic monitoring in bone marrow transplantation induction regimens. Semin Oncology 1993; 20 (Suppl. 4): 18–25.
Hassan M, Öberg G, Ehrsson H et al. Pharmacokinetic and metabolic studies of high-dose busulphan in adults. Eur J Clin Pharmacol 1989; 36: 525–530.
Hassan M, Ljungman P, Bolme P et al. Busulfan bioavailability. Blood 1994; 84: 2144–2150.
Dix SP, Wingard JR, Mullins RE et al. Association of busulfan area under the curve with veno-occlusive disease following BMT. Bone Marrow Transplant 1996; 17: 225–230.
Styler MJ, Crilley P, Biggs J et al. Hepatic dysfunction following busulfan and cyclophosphamide myeloablation: a retrospective, multicenter analysis. Bone Marrow Transplant 1996; 18: 171–176.
Vassal G, Deroussent A, Hartmann O et al. Dose-dependent neurotoxicity of high-dose busulfan in children: a clinical and pharmacological study. Cancer Res 1990; 50: 6203–6207.
Peters WP, Henner WD, Grochow LB et al. Clinical and pharmacologic effects of high dose single agent busulfan with autologous bone marrow support in the treatment of solid tumors. Cancer Res 1987; 47: 6402–6406.
Vassal G . Pharmacologically-guided dose adjustment of busulfan in high-dose chemotherapy regimens: rationale and pitfalls (review). Anticancer Res 1994; 14: 2363–2370.
Andersson BS, Madden T, Tran H et al. Acute safety and pharmacokinetics of intravenous busulfan when used with oral busulfan and cyclophosphamide as pretransplantation conditioning therapy: A phase I Study. Biol Blood and Marrow Transplant 2000; 6: 548–554.
Hassan M . Busulphan. In: Grochow LB, Ames MM (eds). A Clinical Guide to Chemotherapy Pharmacokinetics and Pharmacodynamics. Williams and Wilkins: New York, NY, 1997; pp 189–210.
Benet LZ, Sheiner LB . Pharmacokinetics: The dynamics of drug absorption, distribution, and elimination. In: Goodman Gilman A, Goodman LS, Rall TW, Murad F (eds). Goodman and Gilman's The Pharmacological Basis of Therapeutics, 7th edn. MacMillan Publishing Co.: New York, NY, 1985; p 8.
Bhagwatwar HP, Phadungpojna S, Chow DS et al. Formulation and stability of busulfan for intravenous administration in high-dose chemotherapy. Cancer Chemother Pharmacol 1996; 37: 401–408.
Andersson BS, Kashyap A, Gian V et al. Conditioning therapy with intravenous busulfan and cyclophosphamide (IV BuCy2) for hematologic malignancies prior to allogeneic stem cell transplantation: a phase II study. Biol Blood Marrow Transplant 2002; 8: 145–154.
Andersson BS, Thall PF, Madden T et al. Busulfan systemic exposure relative to regimen-related toxicity and acute graft vs. host disease: defining a therapeutic window for IV BuCy2 in chronic myelogenous leukemia. Biol Blood Marrow Transplant 2002; 8: 477–485.
Gelman A, Carlin JB, Stern HS, Rubin DB . Bayesian Data Analysis. Chapman & Hall: New York, NY, 1995.
Robert CP . The Bayesian Choice, 2nd edn. Springer Verlag: New York, NY, 2001.
Estey E, Thall P, Giles F et al. Gemtuzumab ozogamycin with or without interleukin 11 in patients 65 years of age or older with untreated acute myeloid leukemia and high-risk myelodysplastic syndrome: comparison with idarubicin+continuous-infusion high-dose cytosine arabinoside. Blood 2002; 99: 4343–4349.
Van Besien KW, Mehra RC, Giralt SA et al. Allogeneic bone marrow transplantation for poor-prognosis lymphoma: response, toxicity and survival depend on disease histology. Am J Medicine 1996; 100: 299–307.
Van Besien K, Thall P, Korbling M et al. Allogeneic transplantation for recurrent or refractory non-Hodgkin's lymphoma with poor prognostic features after conditioning with thiotepa, busulfan, and cyclophosphamide: experience in 44 consecutive patients. Biol Blood Marrow Transplant 1997; 3: 150–156.
Przepiorka D, Anderlini P, Ippoliti C et al. Allogeneic blood stem cell transplantation in advanced hematologic cancers. Bone Marrow Transplant 1997; 19: 455–460.
Przepiorka D, Khouri I, Thall PF et al. Thiotepa, busulfan and cyclophosphamide as a preparative regimen for allogeneic transplantation for advanced chronic myelogenous leukemia. Bone Marrow Transplant 1999; 23: 977–981.
Przepiorka D, Smith TL, Folloder J et al. Risk factors for actue graft-versus-host disease after allogeneic blood stem cell transplantation. Blood 1999; 94: 1465–1470.
Przepiorka D, van Besien K, Khouri I et al. Carmustine, etoposide, cytarabine and melphalan as a preparative regimen for allogeneic transplantation for high-risk malignant lymphoma. Ann Oncol 1999; 10: 527–532.
Bibawi S, Abi-Said D, Fayad L et al. Thiotepa, busulfan, and cyclophosphamide as a preparative regimen for allogeneic transplantation for advanced myelodysplastic syndrome and acute myelogenous leukemia. Am J Hematol 2001; 67: 227–233.
Giralt S, Thall PF, Khouri I et al. Melphalan and purine analog-containing preparative regimens: reduced-intensity conditioning for patients with hematologic malignancies undergoing allogeneic progenitor cell transplantation. Blood 2001; 97: 631–637.
Radich JP, Gooley T, Bensinger W et al. HLA-matched related hematopoetic cell transplantation for CML chronic phase using a targeted busulfan and cyclophosphamide preparative regimen. Blood 2003; 102: 31–35.
Acknowledgements
The i.v.BuCy2 studies at the MDACC were sponsored by Grants FD-R-001650-02 from the Food and Drug Administration and by CA49639 and CA16672-27 from the National Cancer Institute. Peter Thall's research was partially supported by NIH Grant R01 CA 83932. We thank two referees for their thoughtful and constructive comments on an earlier version of the manuscript.
Author information
Authors and Affiliations
Corresponding author
Appendix
Appendix
The Bayesian paradigm for statistical analysis is concerned with two objects, the model parameters, which we denote by θ and the observed data. Parameters may be such factors as probabilities, median survival times, or the effects of treatments or patient characteristics on a given outcome. Thus, while parameters are not observed, they characterize important aspects of the observed phenomenon. In the Bayesian framework, parameters are considered random quantities to reflect the fact that one has uncertainty about them. Consequently, a key component of the Bayesian model is a prior probability distribution on θ. The likelihood of observing the data for a given parameter θ also is a probability distribution. Bayes’ Theorem formally combines one's prior with the likelihood to obtain the posterior, f(θ|data), which characterizes one's uncertainty about θ, and hence about the phenomenon, after observing the data. Thus, f(θ|data) is the basis for inference and decision-making in Bayesian analysis.
The methodology used here relies on two closely related probability distributions, the binomial and the beta. Consider the general setting where one observes the number of times, X, that a particular event occurs out of N independent trials, and the probability of the event in each trial is π. Then X follows a binomial probability distribution characterized by N and the parameter π and X has mean Nπ and variance Nπ(1−π). In most settings N is known, since it is simply the number of trials, but π is generally unknown. The most commonly used prior for π in such settings is the beta distribution. If π follows a beta distribution with parameters a and b, denoted π∼beta[a,b], then π has mean μ=a/(a+b) and variance μ(1−μ)/(a+b+1). The sum n=a+b may be interpreted as the prior sample size, so that larger n corresponds to more prior information. An equivalent, often useful way to express the beta[a,b] distribution is in terms of its mean and effective sample size, μ and n, so that π∼beta[μn, (1−μ)n]. Let Y=N−X denote the number of times that the event does not occur in the N trials. Once X and N have been observed, the posterior distribution of π is also beta, but with updated parameters a+X and b+Y, denoted π|X, N∼beta[a+X, b+Y]. The posterior mean of π|X,N is (a+X)/(n+N) and the posterior variance is (a+X)(b+Y)/{(n+N)2(n+N+1)}. The posterior mean (a+X)/(n+N) may be considered a Bayesian estimator of π, and it may be contrasted with the usual, non-Bayesian empirical mean, X/N. Some simple algebra shows that the posterior mean equals the weighted average μ{n/(n+N)}+(X/N)/{N/(n+N)} of the prior mean, μ=a/(a+b), and the empirical mean, X/N, and that the weights are proportional to the prior and actual sample sizes, n and N.
In comparing two binomial samples with probabilities π1 and π2 following beta distributions, we computed posterior probabilities of the form Pr(π2>π1|Data) using the following Splus program. 
Rights and permissions
About this article
Cite this article
Thall, P., Champlin, R. & Andersson, B. Comparison of 100-day mortality rates associated with i.v. busulfan and cyclophosphamide vs other preparative regimens in allogeneic bone marrow transplantation for chronic myelogenous leukemia: Bayesian sensitivity analyses of confounded treatment and center effects. Bone Marrow Transplant 33, 1191–1199 (2004). https://doi.org/10.1038/sj.bmt.1704461
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.bmt.1704461
Keywords
This article is cited by
-
Once-daily i.v. BU-based conditioning regimen before allogeneic hematopoietic SCT: a study of influence of GST gene polymorphisms on BU pharmacokinetics and clinical outcomes in Chinese patients
Bone Marrow Transplantation (2015)
-
Regional differences in performance of bone marrow transplantation, care-resource use and outcome for adult T-cell leukaemia in Japan
BMC Health Services Research (2014)
-
Allogeneic hematopoietic SCT for adults AML using i.v. BU in the conditioning regimen: outcomes and risk factors for the occurrence of hepatic sinusoidal obstructive syndrome
Bone Marrow Transplantation (2014)
-
Prospective validation of a novel IV busulfan fixed dosing for paediatric patients to improve therapeutic AUC targeting without drug monitoring
Cancer Chemotherapy and Pharmacology (2007)