Summary:
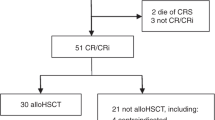
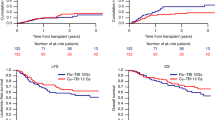
Allogeneic bone marrow transplant (BMT) with an MRD in complete remission (CR)1 is the preferred treatment for children with Philadelphia-positive (Ph+) ALL. The role of MUD BMT in CR1 is still controversial. We compared the outcomes of two treatment strategies: BMT using an MRD or MUD vs chemotherapy in children with Ph+ ALL in CR1. In total, 21 children were treated from 1985 to 2001. In all, 10 received chemotherapy and 11 received allogeneic BMT: four MRD, seven MUD. In the MRD group, one relapsed 12 months after BMT and died; the remaining three are long-term event-free survivors (median follow-up, 6.1 years). In the MUD group four died; the remaining three are long-term event-free survivors (median follow-up, 7.2 years). The 4-year event-free survival (EFS) for the BMT group was 53±15%. In the chemotherapy group, seven relapsed after a median period of 12.5 months and three remain in continuous CR (median follow-up, 2.4 years). Four chemotherapy patients received CR2 transplants; all died. The 4-year EFS for the chemotherapy and MUD groups was 33±17 and 35.7±20%, respectively. This difference was not statistically significant. We continue to support treating children with Ph+ ALL with MRD BMT in CR1. The effectiveness of MUD BMT vs chemotherapy merits further study.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Crist W, Carroll A, Shuster J et al. Philadelphia chromosome positive childhood acute lymphoblastic leukemia: clinical and cytogenetic characteristics and treatment outcome. A Pediatric Oncology Group study. Blood 1990; 76: 489–494.
Fletcher JA, Lynch EA, Kimball VM et al. Translocation (9;22) is associated with extremely poor prognosis in intensively treated children with acute lymphoblastic leukemia. Blood 1991; 77: 435–439.
Uckun FM, Nachman JB, Sather HN et al. Clinical significance of Philadelphia chromosome positive pediatric acute lymphoblastic leukemia in the context of contemporary intensive therapies. A report from the Children's Cancer Group. Cancer 1998; 83: 2030–2039.
Linker CA, Levitt LJ, O'Donnell M et al. Treatment of adult acute lymphoblastic leukemia with intensive cyclical chemotherapy: a follow-up report. Blood 1991; 78: 2814–2822.
Gotz G, Weh HJ, Walter TA et al. Clinical and prognostic significance of the Philadelphia chromosome in adult patients with acute lymphoblastic leukemia. Ann Hematol 1992; 64: 97–100.
Carella AM, Frassoni F, Pollicardo N et al. Philadelphia-chromosome-negative peripheral blood stem cells can be mobilized in the early phase of recovery after a myelosuppressive chemotherapy in Philadelphia-chromosome-positive acute lymphoblastic leukaemia. Br J Haematol 1995; 89: 535–538.
Reece DE, Buskard NA, Hill RS et al. Allogeneic bone marrow transplantation for Philadelphia-chromosome positive acute lymphoblastic leukemia. Leuk Res 1986; 10: 457–459.
Forman SJ, O'Donnell MR, Nademanee AP et al. Bone marrow transplantation for patients with Philadelphia chromosome-positive acute lymphoblastic leukemia. Blood 1987; 70: 587–588.
Barrett AJ, Horowitz MM, Ash RC et al. Bone marrow transplantation for Philadelphia chromosome-positive acute lymphoblastic leukemia. Blood 1992; 79: 3067–3070.
Chao NJ, Blume KG, Forman SJ, Snyder DS . Long-term follow-up of allogeneic bone marrow recipients for Philadelphia chromosome-positive acute lymphoblastic leukemia. Blood 1995; 85: 3353–3354, (letter).
Dunlop LC, Powles R, Singhal S et al. Bone marrow transplantation for Philadelphia chromosome-positive acute lymphoblastic leukemia. Bone Marrow Transplant 1996; 17: 365–369.
Snyder DS, Nademanee AP, O'Donnell MR et al. Long-term follow-up of 23 patients with Philadelphia chromosome-positive acute lymphoblastic leukemia treated with allogeneic bone marrow transplant in first complete remission. Leukemia 1999; 13: 2053–2058.
Stockschläder M, Hegewisch-Becker S, Krüger W et al. Bone marrow transplantation for Philadelphia-chromosome-positive acute lymphoblastic leukemia. Bone Marrow Transplant 1995; 16: 663–667.
Kroger N, Kniger W, Walker-Backhans G et al. Intensified conditioning regimen for in bone marrow transplantation for Philadelphia chromosome-positive acute lymphoblastic leukemia. Bone Marrow Transplant 1998; 22: 1029–1033.
Marks DI, Bird JM, Cornish JM et al. Unrelated donor bone marrow transplantation for children and adolescents with Philadelphia-positive acute lymphoblastic leukemia. J Clin Oncol 1998; 16: 931–936.
Sierra J, Radich J, Hansen JA et al. Marrow transplants from unrelated donors for treatment of Philadelphia chromosome-positive acute lymphoblastic leukemia. Blood 1997; 90: 1410–1414.
Casper J, Camitta B, Ash R et al. Bone marrow transplantation for Philadelphia chromosome positive (Ph+) acute lymphocytic leukemia (ALL) using alternative donors. Blood 1992; 80 (Suppl. 1): 65a (abstract #249).
Mori T, Manabe A, Tsuchida M et al. Allogeneic bone marrow transplantation in first remission rescues children with Philadelphia chromosome-positive acute lymphoblastic leukemia: Tokyo Children's Cancer Study Group (TCCSG) studies L89-12 and L92-13. Med Pediatr Oncol 2001; 37: 426–431.
Ribeiro RC, Broniscer A, Rivera GK et al. Philadelphia chromosome-positive acute lymphoblastic leukemia in children: durable responses to chemotherapy associated with low initial white blood cell counts. Leukemia 1997; 11: 1493–1496.
Aricò M, Valsecchi MG, Camitta B et al. Outcome of treatment in children with Philadelphia chromosome positive acute lymphoblastic leukemia. N Engl J Med 2000; 342: 998–1006.
Schrappe M, Aricò M, Harbott J et al. Philadelphia chromosome-positive (Ph+) childhood acute lymphoblastic leukemia: good initial steroid response allows early prediction of a favorable treatment outcome. Blood 1998; 92: 2730–2741.
Bennett JM, Catovsky D, Daniel M-T et al. Proposals for the classification of the acute leukemias. Brit J Haematol 1976; 33: 451–458.
Chan LC, Pegram SM, Greaves MF . Contribution of immunophenotype to the classification and differential diagnosis of acute leukaemia. Lancet 1985; I: 475–479.
Mitelman F (ed) ISCN (1995). An International System for Human Cytogenetic Nomenclature. Karger: Basel, 1995.
Rivera G, Dahl GV, Bowman WP et al. VM-26 and cytosine arabinoside combination chemotherapy for initial induction failures in childhood lymphocytic leukemia. Cancer 1980; 46: 1727–1730.
Henze G, Fengler R, Hartmann R et al. Six-year experience with a comprehensive approach to the treatment of recurrent childhood acute lymphoblastic leukemia (ALL-REZ BFM 85). A relapse study of the BFM group. Blood 1991; 78: 1166–1172.
Glucksberg H, Storb R, Fefer A et al. Clinical manifestations of graft-versus-host disease in human recipients of marrow from HL-A-matched sibling donors. Transplantation 1974; 18: 295–304.
Lansky SB, List MA, Lansky LL et al. The measurement of performance in childhood cancer patients. Cancer 1987; 60: 1651–1656.
Kaplan G, Meier P . Non-parametric estimations from incomplete observations. J Am Stat Assoc 1958; 53: 457–481.
Cornelissen JJ, Carston M, Kollman C et al. Unrelated marrow transplantation for adult patients with poor-risk acute lymphoblastic leukemia: strong graft-versus-leukemia effect and risk factors determining outcome. Blood 2001; 97: 1572–1577.
Al-Kasim FA, Thornley I, Rolland M et al. Single-center experience with allogeneic bone marrow transplantation for acute lymphoblastic leukemia in childhood: comparable survival after matched-related and matched-unrelated donor transplants. Br J Haematol 2002; 116: 483–490.
Machin D, Campbell M, Fayers P, Pinol A . Sample Size Tables for Clinical Studies, 2nd edn. Balckwell Science: Malden, MA, 1997.
Wheeler KA, Richards SM, Bailey CC et al. Bone marrow transplantation versus chemotherapy in the treatment of very high-risk childhood acute lymphoblastic leukemia in first remission: results from Medical Research Council UKALL X and XI. Blood 2000; 96: 2412–2418.
Acknowledgements
We thank Chris Armstrong RN NP, Kim Yuille RN, Martha Rolland, the staff of the BMT unit, patients and their families, as well as physicians and staff at other Canadian centers who participated in the care of these children – Dr J Hand, Janeway Child Health Centre, St John's, Newfoundland; Dr C Fernandez, IWK Grace Health Centre, Halifax, Nova Scotia; Dr R Klaassen, Children's Hospital of Eastern Ontario, Ottawa, Ontario; Dr M Silva, Kingston General Hospital, Kingston, Ontario; Dr E Cairney, Children's Hospital of Western Ontario, London, Ontario; Dr R Barr, Dr M Pai, McMaster University Medical Centre, Hamilton, Ontario. We also acknowledge Dr Lillian Sung for helpful discussions and advice, Mr Derek Stephens for statistical assistance and the Editorial Services of The Hospital for Sick Children, Toronto, Canada for the technical assistance.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Sharathkumar, A., Saunders, E., Dror, Y. et al. Allogeneic bone marrow transplantation vs chemotherapy for children with Philadelphia chromosome-positive acute lymphoblastic leukemia. Bone Marrow Transplant 33, 39–45 (2004). https://doi.org/10.1038/sj.bmt.1704319
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.bmt.1704319
Keywords
This article is cited by
-
BCR/ABL analysis in myelodysplastic syndromes
Comparative Clinical Pathology (2018)
-
Impact of age, leukocyte count and day 21-bone marrow response to chemotherapy on the long-term outcome of children with philadelphia chromosome-positive acute lymphoblastic leukemia in the pre-imatinib era: results of the FRALLE 93 study
BMC Cancer (2009)
-
Allo-hematopoietic cell transplantation for Ph chromosome-positive ALL: impact of imatinib on relapse and survival
Bone Marrow Transplantation (2009)
-
Transplantation for children with acute lymphoblastic leukemia
Bone Marrow Transplantation (2008)