Summary:
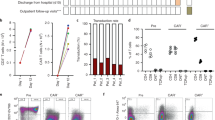
We report graft product stem cell yields and donor safety results of a randomized multicenter study comparing allogeneic peripheral blood stem cell (PBSC) PBSC transplantation with BM transplantation. Matched HLA-identical sibling donors (n=329) were randomized to filgrastim-mobilized PBSC or bone marrow (BM) donation groups. Median yields per kg recipient weight of CD34+ cells, T cells, and natural killer (NK) cells, respectively, were approximately two-fold, eight-fold, and greater than eight-fold in the PBSC group than in the BM group (CD34+ cells, 5.8 × 106/kg vs 2.7 × 106/kg; T cells, 300.1 × 106/kg vs 35.7 × 106/kg; NK cells, 28.2 × 106/kg vs 3.6 × 106/kg; P<0.001 for each). In connection with the cell collection procedures, PBSC donors spent a shorter median time in hospital than BM donors (0 vs 2 days; median difference −2 days, 95% CI −2 to 2) and had fewer median days of restricted activity (2 vs 6 days; median difference −3 days, 95% CI −4 to 2). Overall, 65% of PBSC donors and 57% of BM donors reported at least one adverse event (AE), most of which were transient, mild–moderate in severity, and without clinical sequelae. PBSC donors experienced predominantly filgrastim-related AEs, while BM donors experienced predominantly harvest-related AEs.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Gratwohl A, Baldomero H, Horisberger B et al. Current trends in hematopoietic stem cell transplantation in Europe. Blood 2002; 100: 2374–2386.
To LB, Roberts MM, Haylock DN et al. Comparison of haematological recovery times and supportive care requirements of autologous recovery phase peripheral blood stem cell transplants, autologous bone marrow transplants and allogeneic bone marrow transplants. Bone Marrow Transplant 1992; 9: 277–284.
Schmitz N, Linch DC, Dreger P et al. Randomised trial of filgrastim-mobilised peripheral blood progenitor cell transplantation vs autologous bone-marrow transplantation in lymphoma patients. Lancet 1996; 347: 353–357.
Bensinger WI, Martin PJ, Storer B et al. Transplantation of bone marrow as compared with peripheral-blood cells from HLA-identical relatives in patients with hematologic cancers. N Engl J Med 2001; 344: 175–181.
Powles R, Mehta J, Kulkarni S et al. Allogeneic blood and bone-marrow stem cell transplantation in haematological malignant diseases: a randomised trial. Lancet 2000; 355: 1231–1237.
Schmitz N, Beksaç M, Hasenclever D et al. Transplantation of mobilized peripheral blood cells to HLA-identical siblings with standard-risk leukemia. Blood 2002; 100: 761–767.
Aversa F, Terenzi A, Felicini R et al. Haploidentical stem cell transplantation for acute leukemia. Int J Hematol 2002; 76 (Suppl. 1): 165–168.
Blaise D, Kuentz M, Fortanier C et al. Randomized trial of bone marrow vs lenograstim-primed blood cell allogeneic transplantation in patients with early stage leukemia: a report from the Société Française de Greffe de Moelle. J Clin Oncol 2000; 18: 537–546.
Heldal D, Tjønnfjord G, Brinch L et al. A randomised study of allogeneic transplantation with stem cells from blood or bone marrow. Bone Marrow Transplant 2000; 25: 1129–1136.
Stroncek DF, Holland PV, Bartch G et al. Experiences of the first 493 unrelated marrow donors in the National Marrow Donor Program. Blood 1993; 81: 1940–1946.
Hosoya N, Miyagawa K, Mimura T et al. Malignant hyperthermia induced by general anesthesia for bone marrow harvesting. Bone Marrow Transplant 1997; 19: 509–511.
Murata M, Harada M, Kato S et al. Peripheral blood stem cell mobilization and apheresis: analysis of adverse events in 94 normal donors. Bone Marrow Transplant 1999; 24: 1065–1071.
Anderlini P, Rizzo JD, Nugent ML et al. Peripheral blood stem cell donation: an analysis from the International Bone Marrow Transplant Registry (IBMTR) and European Group for Blood and Marrow Transplant (EBMT) databases. Bone Marrow Transplant 2001; 27: 689–692.
Becker PS, Wagle M, Matous S et al. Spontaneous splenic rupture following administration of granulocyte colony-stimulating factor (G-CSF): occurrence in an allogeneic donor of peripheral blood stem cells. Biol Blood Marrow Transplant 1997; 3: 45–49.
Falzetti F, Aversa F, Minelli O, Tabilio A . Spontaneous rupture of spleen during peripheral blood stem-cell mobilisation in a healthy donor. Lancet 1999; 353: 555.
Vij R, Adkins DR, Brown RA et al. Unstable angina in a peripheral blood stem and progenitor cell donor given granulocyte-colony-stimulating factor. Transfusion 1999; 39: 542–543.
Anderlini P, Przepiorka D, Körbling M, Champlin R . Blood stem cell procurement: donor safety issues. Bone Marrow Transplant 1998; 21 (Suppl. 3): S35–S39.
Schmitz N, Bacigalupo A, Hasenclever D et al. Allogeneic bone marrow transplantation vs filgrastim-mobilised peripheral blood progenitor cell transplantation in patients with early leukaemia: first results of a randomised multicentre trial of the European Group for Blood and Marrow Transplantation. Bone Marrow Transplant 1998; 21: 995–1003.
Couban S, Simpson DR, Barnett MJ et al. A randomized multicenter comparison of bone marrow and peripheral blood in recipients of matched sibling allogeneic transplants for myeloid malignancies. Blood 2002; 100: 1525–1531.
Majolino I, Cavallaro AM, Bacigalupo A et al. Mobilization and collection of PBSC in healthy donors: a retrospective analysis of the Italian Bone Marrow Transplantation Group (GITMO). Haematologica 1997; 82: 47–52.
Anderlini P, Donato M, Chan K-W et al. Allogeneic blood progenitor cell collection in normal donors after mobilization with filgrastim: The M.D. Anderson Cancer Center experience. Transfusion 1999; 39: 555–560.
Bolan CD, Cecco SA, Wesley RA et al. Controlled study of citrate effects and response to IV calcium administration during allogeneic peripheral blood progenitor cell donation. Transfusion 2002; 42: 935–946.
Miflin G, Charley C, Stainer C et al. Stem cell mobilization in normal donors for allogeneic transplantation: analysis of safety and factors affecting efficacy. Br J Haematol 1996; 95: 345–348.
Buckner CD, Clift RA, Sanders JE et al. Marrow harvesting from normal donors. Blood 1984; 64: 630–634.
Anderlini P, Körbling M, Dale D et al. Allogeneic blood stem cell transplantation: considerations for donors. Blood 1997; 90: 903–908.
Cavallaro AM, Lilleby K, Majolino I et al. Three to six year follow-up of normal donors who received recombinant human granulocyte colony-stimulating factor. Bone Marrow Transplant 2000; 25: 85–89.
Hasenclever D, Sextro M . Safety of alloPBSCT donors: Biometrical considerations on monitoring long term risks. Bone Marrow Transplant 1996; 17 (Suppl. 2): S26–S30.
Couban S, Dranitsaris G, Andreou P et al. Clinical and economic analysis of allogeneic peripheral blood progenitor cell transplants: a Canadian perspective. Bone Marrow Transplant 1998; 22: 1199–1205.
Bennett CL, Waters TM, Stinson TJ et al. Valuing clinical strategies early in development: a cost analysis of allogeneic peripheral blood stem cell transplantation. Bone Marrow Transplant 1999; 24: 555–560.
Madero L, Vicent MG, Ramirez M et al. Clinical and economic comparison of allogeneic peripheral blood progenitor cell and bone marrow transplantation for acute lymphoblastic leukemia in children. Bone Marrow Transplant 2000; 26: 269–273.
Switzer GE, Goycoolea JM, Dew MA et al. Donating stimulated peripheral blood stem cells vs bone marrow: do donors experience the procedures differently? Bone Marrow Transplant 2001; 27: 917–923.
Rowley SD, Donaldson G, Lilleby K et al. Experiences of donors enrolled in a randomized study of allogeneic bone marrow or peripheral blood stem cell transplantation. Blood 2001; 97: 2541–2548.
Munzenberger N, Fortanier C, Macquart-Moulin G et al. Psychosocial aspects of haematopoietic stem cell donation for allogeneic transplantation: how family donors cope with this experience. Psychooncology 1999; 8: 55–63.
Acknowledgements
This study was sponsored by Amgen Ltd., Cambridge, UK, and F Hoffmann – La Roche AG, Basel, Switzerland, and partially supported by grants from the Swiss National Research Foundation (32-52756.97) and the Horton Foundation to Dr G Favre.
Author information
Authors and Affiliations
Consortia
Corresponding author
Appendix
Appendix
This study was conducted at the following institutions under the auspices of the named principal investigators: Allgemeines Krankenhaus, Vienna, Austria (H Greinix); University Hospital, Innsbruck, Austria (D Niederwieser, D Nachbauer); University Hospital, Leuven, Belgium (M Boogaerts); Cliniques Universitaires St Luc, Brussels, Belgium (A Ferrant); Charité der Humboldt Universität, Berlin, Germany (R Arnold); Hôpital St Louis, Paris, France (E Gluckman); Hôpital St. Antoine, Paris, France (NC Gorin); Universität Ulm, Ulm, Germany (N Frickhofen); Christian-Albrechts Universität, Kiel, Germany (N Schmitz); Universitätsklinikum Eppendorf, Hamburg, Germany (A Zander); St James Hospital, Dublin, Ireland (S McCann); Hadassah University Hospital, Jerusalem, Israel (A Nagler); Ospedale San Martino, Genova, Italy (A Bacigalupo); Kantonsspital Basel, Basel, Switzerland (A Gratwohl); Hammersmith Hospital, London, UK (J Apperley); Nottingham City Hospital, Nottingham, UK (NH Russell); Huddinge Hospital, Huddinge, Sweden (O Ringdén); Ospedale V Cervello-USL, Palermo, Italy(I Majolino); Hôpital Claude Huriez, Lille, France (JP Jouet); Hôpital Necker, Paris, France (B Varet); Klinikum der Albert-Ludwigs Universität, Freiburg, Germany (J Finke); Leeds General Infirmary, Leeds, UK (G Smith); Azienda Ospedaliera Careggi, Firenze, Italy (A Bosi); Padiglione G Marcora, Ospedale Maggiore di Milano, Milano, Italy (G Lambertenghi-Deliliers); Universitätsklinikum, Mainz, Germany (K Kolbe); Helsinki University Central Hospital, Helsinki, Finland (T Ruutu); Westmead Hospital, Westmead, Australia (KA Bradstock); LCHRU de Hautepierre, Strasbourg, France (B Lioure); Hanson Centre for Cancer Research, Royal Adelaide Hospital, Adelaide, Australia (T Hughes); Royal Melbourne Hospital, Parkville, Australia (J Szer); Royal Perth Hospital, Perth, Australia (R Herrmann); Universitätsklinik, Hamburg, Germany (L Trümper); Centro Dipartimentale Trapianti di Midollo, Ospedale Molinette, Torino, Italy (M Falda); Ankara University Medical Facility, Ankara, Turkey (M Beksaç); Evangelismos General Hospital, Athens, Greece (E Nikiforakis); Instituto Portugues de Oncologia Francisco Gentil, Lisbon, Portugal (M Abecasis); Rambam Medical Center, Haifa, Israel (J Rowe); Royal Free Hospital, Hampstead, London, UK (M Potter); Medizinische Klinik Nürnberg, Nürnberg, Germany (H Wandt); Stiftung Deutsche Klinik f. Diagnostik, Wiesbaden, Germany (R Schwerdtfeger); Universität Rostock, Rostock, Germany (J Casper); King's College Hospital, London, UK (A Pagliuca).
Rights and permissions
About this article
Cite this article
Favre, G., Beksaç, M., Bacigalupo, A. et al. Differences between graft product and donor side effects following bone marrow or stem cell donation. Bone Marrow Transplant 32, 873–880 (2003). https://doi.org/10.1038/sj.bmt.1704245
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.bmt.1704245
Keywords
This article is cited by
-
Detection of CRISPR/Cas9-Mediated Fetal Hemoglobin Reactivation in Erythroblasts Derived from Cord Blood-Hematopoietic Stem Cells
Molecular Biotechnology (2024)
-
Allogeneic transplantation of bone marrow versus peripheral blood stem cells from HLA-identical relatives in patients with myelodysplastic syndromes and oligoblastic acute myeloid leukemia: a propensity score analysis of a nationwide database
Annals of Hematology (2023)
-
Basic characteristics and safety of donation in related and unrelated haematopoietic progenitor cell donors – first 10 years of prospective donor follow-up of Swiss donors
Bone Marrow Transplantation (2022)
-
IgA nephropathy diagnosed as a result of acute exacerbation due to G-CSF administration
CEN Case Reports (2022)
-
Peripheral hematopoietic stem cell mobilization utilizing growth factors in donors with sickle cell trait is safe and effective
Bone Marrow Transplantation (2018)