Abstract
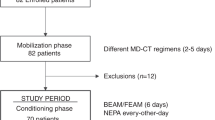
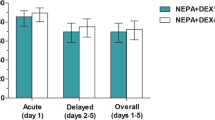
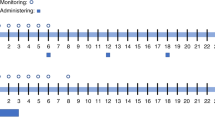
We evaluated the combination of diphenhydramine, lorazepam, and dexamethasone delivered as a continuous i.v. infusion via an ambulatory infusion pump with patient-activated intermittent dosing (BAD pump) for prevention of acute and delayed nausea/vomiting in patients receiving high-dose chemotherapy (HDC) for peripheral blood progenitor cell (PBPC) mobilization (MOB) or prior to autologous PBPC rescue. The BAD pump was titrated to patient response and tolerance, and continued until the patient could tolerate oral anti-emetics. Forty-four patients utilized the BAD pump during 66 chemotherapy courses, 34 (52%) for MOB and 32 (48%) for HDC with autologous PBPC rescue. The median number of days on the BAD pump during MOB and HDC was 3 (1–6) and 9 (2–19) days, respectively. Complete overall or complete emesis control occurred on 94% of MOB and 89% of HDC treatment days during chemotherapy administration and 72% and 43%, respectively, following chemotherapy administration. Eighty-three percent of MOB and 55% of HDC treatment days were associated with no nausea. While on the BAD pump, no patient experienced severe toxicity or required hospitalization for management of nausea/vomiting. The BAD pump was safe and effective in minimizing nausea and vomiting associated with HDC, and thus, eliminated the need for hospitalization for management of chemotherapy-induced nausea and vomiting.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Dix, S., Cord, M., Howard, S. et al. Safety and efficacy of a continuous infusion, patient controlled anti-emetic pump to facilitate outpatient administration of high-dose chemotherapy. Bone Marrow Transplant 24, 561–566 (1999). https://doi.org/10.1038/sj.bmt.1701909
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.bmt.1701909
Keywords
This article is cited by
-
Pharmacological treatment options for mast cell activation disease
Naunyn-Schmiedeberg's Archives of Pharmacology (2016)
-
Chemotherapy-induced nausea and vomiting: contemporary approaches to optimal management
Supportive Care in Cancer (2010)