Abstract
Objective: Maternal weight gain has been consistently linked to birth weight but, beyond maternal energy intake, no macronutrient has been associated with either of them. We have examined whether maternal energy-adjusted intake of macronutrients is associated with either maternal weight gain or birth-size parameters.
Design: Cohort study.
Setting: University hospital in Boston, USA.
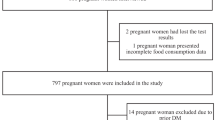
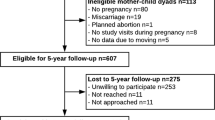
Subjects: A total of 224 pregnant women coming for their first routine prenatal visit. The women were followed through delivery.
Interventions: None. Pregnant women's dietary intake during the second trimester was ascertained at the 27th week of pregnancy through a food frequency questionnaire.
Results: Intake of neither energy nor any of the energy-generating nutrients was significantly associated with birth size. In contrast, maternal weight gain by the end of the second trimester of pregnancy was significantly associated with energy intake (+0.9 kg/s.d. of intake; P∼0.006) as well as energy-adjusted intake of protein (+3.1 kg/s.d. of intake; P<10-4), lipids of animal origin (+2.6 kg/s.d. of intake; P<10−4) and carbohydrates (−5.2 kg/s.d. of intake; P<10−4).
Conclusions: Although maternal weight gain is strongly associated with birth size, the indicated nutritional associations with weight gain are not reflected in similar associations with birth-size parameters. The pattern is reminiscent of the sequence linking diet to coronary heart disease (CHD) through cholesterol: diet has been conclusively linked to blood cholesterol levels and cholesterol levels are conclusively linked to this disease, even though the association of diet with CHD has been inconclusive and controversial.
Sponsorship: This study was supported in part by Grant No. CA54220 from the National Institutes of Health
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
References
Abrams B & Selvin S (1995): Maternal weight gain pattern and birth weight. Obstet. Gynecol. 86,163–169.
Alexy B, Nichols B, Heverly MA & Garzon L (1997): Prenatal factors and birth outcomes in the public health service: a rural/urban comparison. Res. Nurs. Health 20, 61–70.
Bergmann MM, Flagg EW, Miracle-McMahill HL & Boeing H (1997): Energy intake and net weight gain in pregnant women according to body mass index (BMI) status. Int. J. Obes. Relat. Metab. Disord. 21,1010–1017.
Brown JE, Murtaugh MA, Jacobs Jr DR & Margellos HC . (2002): Variation in newborn size according to pregnancy weight change by trimester. Am. J. Clin. Nutr. 76, 205–209.
England LJ, Kendrick JS, Wilson HG, Merritt RK, Gargiullo PM & Zahniser SC (2001): Effects of smoking reduction during pregnancy on the birth weight of term infants. Am. J. Epidemiol. 154, 694–701.
Eskenazi B, Stapleton AL, Kharrazi M & Chee WY (1999): Associations between maternal decaffeinated and caffeinated coffee consumption and fetal growth and gestational duration. Epidemiology 10, 242–249.
Godfrey KM, Barker DJ, Robinson S & Osmond C (1997): Maternal birthweight and diet in pregnancy in relation to the infant's thinness at birth. Br. J. Obstet. Gynaecol. 104, 663–667.
Guihard-Costa AM, Papiernik E, Grange G & Richard A (2002): Gender differences in neonatal subcutaneous fat store in late gestation in relation to maternal weight gain. Ann. Hum. Biol. 29, 26–36.
Kramer MS (2000a): High Protein Supplementation in Pregnancy. Cochrane Database Syst Rev, Vol. 2, CD000105.
Kramer MS (2000b): Balanced Protein/Energy Supplementation in Pregnancy. Cochrane Database Syst Rev, Vol. 2, CD000032.
Lagiou P, Hsieh CC, Trichopoulos D, Xu B, Wuu J, Mucci L, Tamimi R, Adami HO & Cnattingius S (2003): Birth weight differences between USA and China and their relevance to breast cancer etiology. Int. J. Epidemiol. 32, 193–198.
Lee KS, Ferguson RM, Corpuz M & Gartner LM (1988): Maternal age and incidence of low birth weight at term: a population study. Am. J. Obstet. Gynecol. 158, 84–89.
Levy L & Jackson AA (1993): Modest restriction of dietary protein during pregnancy in the rat: fetal and placental growth. J. Dev. Physiol. 19, 113–118.
Lipworth L, Hsieh Cc, Wide L, Ekbom A, Yu SZ, Yu GP, Xu B, Hellerstein S, Carlstrom K, Trichopoulos D & Adami HO (1999): Maternal pregnancy hormone levels in an area with a high incidence (Boston, USA) and in an area with a low incidence (Shanghai, China) of breast cancer. Br. J. Cancer. 79, 7–12.
Magnus P, Berg K & Bjerkedal T (1985): The association of parity and birth weight: testing the sensitization hypothesis. Early Hum. Dev. 12, 49–54.
Mathews F, Yudkin P & Neil A (1999): Influence of maternal nutrition on outcome of pregnancy: prospective cohort study. BMJ 319, 339–343.
Olsen SF (1993): Consumption of marine n-3 fatty acids during pregnancy as a possible determinant of birth weight. A review of the current epidemiologic evidence. Epidemiol. Rev. 15, 399–413.
Petridou E, Stoikidou M, Diamantopoulou M, Mera E, Dessypris N & Trichopoulos D (1998): Diet during pregnancy in relation to birthweight in healthy singletons. Child Care Health Dev. 24, 229–242.
Potischman N & Troisi R (1999): In-utero and early life exposures in relation to risk of breast cancer. Cancer Causes Control 10, 561–573.
Rich-Edwards JW, Stampfer MJ, Manson JE, Rosner B, Hankinson SE, Colditz GA, Willett WC & Hennekens CH (1997): Birth weight and risk of cardiovascular disease in a cohort of women followed up since 1976. BMJ 315, 396–400.
Rich-Edwards JW, Colditz GA, Stampfer MJ, Willett WC, Gillman MW, Hennekens CH, Speizer FE & Manson JE (1999): Birthweight and the risk for type 2 diabetes mellitus in adult women. Ann. Intern. Med. 130, 278–284.
Romieu I, Stampfer MJ, Stryker WS, Hernandez M, Kaplan L, Sober A, Rosner B & Willett WC (1990): Food predictors of plasma beta-carotene and alpha-tocopherol: validation of a food frequency questionnaire. Am. J. Epidemiol. 131, 864–876.
Rondo PH & Tomkins AM (1999): Maternal and neonatal anthropometry. Ann. Trop. Paediatr. 19,349–356.
Rush D (2001): Maternal nutrition and perinatal survival. Nutr. Rev. 59, 315–326.
Scholl TO, Hediger ML, Khoo CS, Healey MF & Rawson NL (1991): Maternal weight gain, diet and infant birth weight: correlations during adolescent pregnancy. J. Clin. Epidemiol. 44, 423–428.
Shapiro C, Sutija VG & Bush J (2000): Effect of maternal weight gain on infant birth weight. J. Perinat. Med. 28, 428–431.
Spencer N, Bambang S, Logan S & Gill L (1999): Socioeconomic status and birth weight: comparison of an area-based measure with the Registrar General's social class. J. Epidemiol. Commun. Health 53, 495–498.
Susser M (1991): Maternal weight gain, infant birth weight, and diet: causal sequences. Am. J. Clin. Nutr. 53, 1384–1396.
Thorsdottir I & Birgisdottir BE (1998): Different weight gain in women of normal weight before pregnancy: postpartum weight and birth weight. Obstet. Gynecol. 92, 377–383.
Weigel MM, Narvaez WM, Lopez A, Felix C & Lopez P (1991): Prenatal diet, nutrient intake and pregnancy outcome in urban Ecuadorian primiparas. Arch. Latinoam. Nutr. 41, 21–37.
Willett WC, Sampson L, Stampfer MJ, Rosner B, Bain C, Witschi J, Hennekens CH & Speizer FE (1985): Reproducibility and validity of a semiquantitative food frequency questionnaire. Am. J. Epidemiol. 122, 51–65.
Willett W . (1998): Diet and coronary heart disease. In Nutritional Epidemiology, W Willett (ed). 2nd Edition, pp 414–466. New York: Oxford University Press, 1998.
Yu SM & Nagey DA . (1992): Validity of self-reported pregravid weight. Ann. Epidemiol. 2: 715–721.
Zhou W & Olsen J (1997): Gestational weight gain as a predictor of birth and placenta weight according to pre-pregnancy body mass index. Acta. Obstet. Gynecol. Scand. 76, 300–307.
Author information
Authors and Affiliations
Contributions
Guarantor: D Trichopoulos.
Contributors: The study was executed by PL, RMT and LAM. The original international study was conceived by H-OA, DT and CcH, who also provided input in the analysis. All authors contributed to the interpretation of the results and the preparation of the manuscript.
Corresponding author
Rights and permissions
About this article
Cite this article
Lagiou, P., Tamimi, R., Mucci, L. et al. Diet during pregnancy in relation to maternal weight gain and birth size. Eur J Clin Nutr 58, 231–237 (2004). https://doi.org/10.1038/sj.ejcn.1601771
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.ejcn.1601771
Keywords
This article is cited by
-
Association of plant-based dietary patterns in first trimester of pregnancy with gestational weight gain: results from a prospective birth cohort
European Journal of Clinical Nutrition (2023)
-
Maternal protein intake in early pregnancy and child development at age 3 years
Pediatric Research (2023)
-
Dietary protein intake during pregnancy and birth weight among Chinese pregnant women with low intake of protein
Nutrition & Metabolism (2022)
-
Ernährung in der Schwangerschaft: Makronährstoffe
Journal für Gynäkologische Endokrinologie/Österreich (2022)
-
Gestational weight gain mediates the effects of energy intake on birth weight among singleton pregnancies in the Japan Environment and Children’s Study
BMC Pregnancy and Childbirth (2022)