Abstract
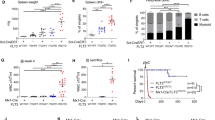
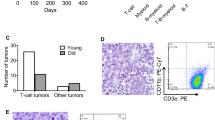
Activating FMS-like tyrosine kinase 3 (FLT3) mutations have been identified in ∼30% of patients with acute myelogenous leukemia (AML), and recently in a smaller subset of patients with acute lymphoblastic leukemia (ALL). To explore the in vivo consequences of an activating FLT3 internal tandem duplication mutation (FLT3-ITD), we created a transgenic mouse model in which FLT3-ITD was expressed under the control of the vav hematopoietic promoter. Five independent lines of vav-FLT3-ITD transgenic mice developed a myeloproliferative disease with high penetrance and a disease latency of 6–12 months. The phenotype was characterized by splenomegaly, megakaryocytic hyperplasia, and marked thrombocythemia, but without leukocytosis, polycythemia, or marrow fibrosis, displaying features reminiscent of the human disease essential thrombocythemia (ET). Clonal immature B- or T-lymphoid disease was observed in two additional founder mice, respectively, that could be secondarily transplanted to recipient mice that rapidly developed lymphoid disease. Treatment of these mice with the FLT3 tyrosine kinase inhibitor, PKC412, resulted in suppression of disease and a statistically significant prolongation of survival. These results demonstrate that FLT3-ITD is capable of inducing myeloproliferative as well as lymphoid disease, and indicate that small-molecule tyrosine kinase inhibitors may be an effective treatment for lymphoid malignancies in humans that are associated with activating mutations in FLT3.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 50 print issues and online access
$259.00 per year
only $5.18 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout





Similar content being viewed by others
References
Abu-Duhier FM, Goodeve AC, Wilson GA, Care RS, Peake IR and Reilly JT . (2001). Br. J. Haematol., 113, 1076–1077.
Armstrong SA, Kung AL, Mabon ME, Silverman LB, Stam RW, Den Boer ML, Pieters R, Kersey JH, Sallan SE, Fletcher JA, Golub TR, Griffin JD and Korsmeyer SJ . (2003). Cancer Cell, 3, 173–183.
Armstrong SA, Staunton JE, Silverman LB, Pieters R, den Boer ML, Minden MD, Sallan SE, Lander ES, Golub TR and Korsmeyer SJ . (2002). Nat. Genet., 30, 41–47.
Brasel K, Escobar S, Anderberg R, de Vries P, Gruss HJ and Lyman SD . (1995). Leukemia, 9, 1212–1218.
Chen J, Deangelo DJ, Kutok JL, Williams IR, Lee BH, Wadleigh M, Duclos N, Cohen S, Adelsperger J, Okabe R, Coburn A, Galinsky I, Huntly B, Cohen PS, Meyer T, Fabbro D, Roesel J, Banerji L, Griffin JD, Xiao S, Fletcher JA, Stone RM and Gilliland DG . (2004). Proc. Natl. Acad. Sci. USA, 101, 14479–14484.
Cools J, Stover EH, Boulton CL, Gotlib J, Legare RD, Amaral SM, Curley DP, Duclos N, Rowan R, Kutok JL, Lee BH, Williams IR, Coutre SE, Stone RM, DeAngelo DJ, Marynen P, Manley PW, Meyer T, Fabbro D, Neuberg D, Weisberg E, Griffin JD and Gilliland DG . (2003). Cancer Cell, 3, 459–469.
DaSilva N, Hu ZB, Ma W, Rosnet O, Birnbaum D and Drexler HG . (1994). Leukemia, 8, 885–888.
deLapeyriere O, Naquet P, Planche J, Marchetto S, Rottapel R, Gambarelli D, Rosnet O and Birnbaum D . (1995). Differentiation, 58, 351–359.
Drexler HG . (1996). Leukemia, 10, 588–599.
Ferrando AA, Neuberg DS, Staunton J, Loh ML, Huard C, Raimondi SC, Behm FG, Pui CH, Downing JR, Gilliland DG, Lander ES, Golub TR and Look AT . (2002). Cancer Cell, 1, 75–87.
Gilliland DG and Griffin JD . (2002). Blood, 100, 1532–1542.
Griffin JD . (2001). Blood, 97, 2193.
Hayakawa F, Towatari M, Kiyoi H, Tanimoto M, Kitamura T, Saito H and Naoe T . (2000). Oncogene, 19, 624–631.
Horiike S, Yokota S, Nakao M, Iwai T, Sasai Y, Kaneko H, Taniwaki M, Kashima K, Fujii H, Abe T and Misawa S . (1997). Leukemia, 11, 1442–1446.
Ishii E, Zaitsu M, Ihara K, Hara T and Miyazaki S . (1999). Pediatr. Hematol. Oncol., 16, 437–441.
Kelly LM, Liu Q, Kutok JL, Williams IR, Boulton CL and Gilliland DG . (2002). Blood, 99, 310–318.
Kiyoi H, Naoe T, Nakano Y, Yokota S, Minami S, Miyawaki S, Asou N, Kuriyama K, Jinnai I, Shimazaki C, Akiyama H, Saito K, Oh H, Motoji T, Omoto E, Saito H, Ohno R and Ueda R . (1999). Blood, 93, 3074–3080.
Kiyoi H, Towatari M, Yokota S, Hamaguchi M, Ohno R, Saito H and Naoe T . (1998). Leukemia, 12, 1333–1337.
Mackarehtschian K, Hardin JD, Moore KA, Boast S, Goff SP and Lemischka IR . (1995). Immunity, 3, 147–161.
Maroc N, Rottapel R, Rosnet O, Marchetto S, Lavezzi C, Mannoni P, Birnbaum D and Dubreuil P . (1993). Oncogene, 8, 909–918.
Meierhoff G, Dehmel U, Gruss HJ, Rosnet O, Birnbaum D, Quentmeier H, Dirks W and Drexler HG . (1995). Leukemia, 9, 1368–1372.
Mizuki M, Fenski R, Halfter H, Matsumura I, Schmidt R, Muller C, Gruning W, Kratz-Albers K, Serve S, Steur C, Buchner T, Kienast J, Kanakura Y, Berdel WE and Serve H . (2000). Blood, 96, 3907–3914.
Nakao M, Yokota S, Iwai T, Kaneko H, Horiike S, Kashima K, Sonoda Y, Fujimoto T and Misawa S . (1996). Leukemia, 10, 1911–1918.
Ogilvy S, Elefanty AG, Visvader J, Bath ML, Harris AW and Adams JM . (1998). Blood, 91, 419–430.
Ogilvy S, Metcalf D, Gibson L, Bath ML, Harris AW and Adams JM . (1999a). Blood, 94, 1855–1863.
Ogilvy S, Metcalf D, Print CG, Bath ML, Harris AW and Adams JM . (1999b). Proc. Natl. Acad. Sci. USA, 96, 14943–14948.
Rasko JE, Metcalf D, Rossner MT, Begley CG and Nicola NA . (1995). Leukemia, 9, 2058–2066.
Rosnet O and Birnbaum D . (1993). Crit. Rev. Oncogenet., 4, 595–613.
Rosnet O, Buhring HJ, Marchetto S, Rappold I, Lavagna C, Sainty D, Arnoulet C, Chabannon C, Kanz L, Hannum C and Birnbaum D . (1996). Leukemia, 10, 238–248.
Tse KF, Mukherjee G and Small D . (2000). Leukemia, 14, 1766–1776.
Turner AM, Lin NL, Issarachai S, Lyman SD and Broudy VC . (1996). Blood, 88, 3383–3390.
Weisberg E, Boulton C, Kelly LM, Manley P, Fabbro D, Meyer T, Gilliland DG and Griffin JD . (2002). Cancer Cell, 1, 433–443.
Yamamoto Y, Kiyoi H, Nakano Y, Suzuki R, Kodera Y, Miyawaki S, Asou N, Kuriyama K, Yagasaki F, Shimazaki C, Akiyama H, Saito K, Nishimura M, Motoji T, Shinagawa K, Takeshita A, Saito H, Ueda R, Ohno R and Naoe T . (2001). Blood, 97, 2434–2439.
Acknowledgements
We thank members of the Gilliland laboratory for valuable advice and discussions. This work was supported in part by NIH grants CA66996 and DK50654, and by a Leukemia and Lymphoma Society SCOR grant. BHL is a recipient of a Physician-Scientist Fellowship from the Leukemia Research Foundation and was previously supported by NIH departmental training grant 5T32HL 07627-16, and DGG is an Investigator in the Howard Hughes Medical Institute.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Lee, B., Williams, I., Anastasiadou, E. et al. FLT3 internal tandem duplication mutations induce myeloproliferative or lymphoid disease in a transgenic mouse model. Oncogene 24, 7882–7892 (2005). https://doi.org/10.1038/sj.onc.1208933
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.onc.1208933
Keywords
This article is cited by
-
Microenvironmental CXCL12 deletion enhances Flt3-ITD acute myeloid leukemia stem cell response to therapy by reducing p38 MAPK signaling
Leukemia (2023)
-
Update on Small Molecule Targeted Therapies for Acute Myeloid Leukemia
Current Treatment Options in Oncology (2023)
-
Gab2 deficiency prevents Flt3-ITD driven acute myeloid leukemia in vivo
Leukemia (2022)
-
Imipramine blue sensitively and selectively targets FLT3-ITD positive acute myeloid leukemia cells
Scientific Reports (2017)
-
The protein tyrosine phosphatase, Shp2, positively contributes to FLT3-ITD-induced hematopoietic progenitor hyperproliferation and malignant disease in vivo
Leukemia (2013)