Abstract
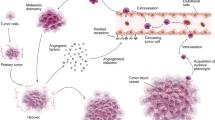
Angiogenesis is a term that describes the formation of new capillaries from a pre-existing vasculature. This process is very important in physiologic conditions because it helps healing injured tissues, and in female populations it helps forming the placenta after fertilization and reconstructs the inside layer of the uterus after menstruation. Angiogenesis is the result of an intricate balance between proangiogenic and antiangiogenic factors and is now very well recognized as a powerful control point in tumor development. In this particular environment, the fine modulation among proangiogenic and antiangiogenic factors is disrupted, leading to inappropriate vessels growth. In this review, we discuss the molecular basis of angiogenesis during tumor growth and we also illustrate some of the molecules that are involved in this angiogenic switch.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 50 print issues and online access
$259.00 per year
only $5.18 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
References
Adams RH, Wilkinson GA, Weiss C, Diella F, Gale NW, Deutsch U, Risau W and Klein R . (1999). Genes Dev., 13, 295–306.
Arbiser JL, Moses MA, Fernandez CA, Ghiso N, Cao Y, Klauber N, Frank D, Brownlee M, Flynn E, Parangi S, Byers HR and Folkman J . (1997). Proc. Natl. Acad. Sci. USA, 94, 861–866.
Baish JW and Jain RK . (2000). Cancer Res., 60, 3683–3688.
Bhushan M, Young HS, Brenchley PE and Griffiths CE . (2002). Br. J. Dermatol., 147, 418–425.
Breit S, Ashman K, Wilting J, Rossler J, Hatzi E, Fotsis T and Schweigerer L . (2000). Cancer Res., 60, 4596–4601.
Brooks PC, Montgomery AM, Rosenfeld M, Reisfeld RA, Hu T, Klier G and Cheresh DA . (1994). Cell, 79, 1157–1164.
Buschmann IS and W . (2000). J. Pathol., 190, 338–342.
Carmeliet P . (1999). Nature, 401, 657–658.
Carmeliet P . (2000). Nat. Med., 6, 389–395.
Carmeliet P, Ferreira V, Breier G, Pollefeyt S, Kieckens L, Gertsenstein M, Fahrig M, Vandenhoeck A, Harpal K, Eberhardt C, Declercq C, Pawling J, Moons L, Collen D, Risau W and Nagy A . (1996). Nature, 380, 435–439.
Casanova ML, Larcher F, Casanova B, Murillas R, Fernandez-Acenero MJ, Villanueva C, Martinez-Palacio J, Ullrich A, Conti CJ and Jorcano JL . (2002). Cancer Res., 62, 3402–3407.
Charvat S, Duchesne M, Parvaz P, Chignol MC, Schmitt D and Serres M . (1999). Anticancer Res., 19, 557–561.
Chavakis E and Dimmeler S . (2002). Arterioscler. Thromb. Vasc. Biol., 22, 887–893.
Cheng SY, Nagane M, Huang HS and Cavenee WK . (1997). Proc. Natl. Acad. Sci. USA, 94, 12081–12087.
D'Angelo G, Struman I, Martial J and Weiner RI . (1995). Proc. Natl. Acad. Sci. USA, 92, 6374–6378.
Davis S, Aldrich TH, Jones PF, Acheson A, Compton DL, Jain V, Ryan TE, Bruno J, Radziejewski C, Maisonpierre PC and Yancopoulos GD . (1996). Cell, 87, 1161–1169.
Denekamp J . (1993). Br. J. Radial., 66, 181–196.
Dulak J and Jozkowicz A . (2003). Antioxid. Redox Signal., 5, 123–132.
Dvorak HF, Nagy JA, Dvorak JT and Dvorak AM . (1988). Am. J. Pathol., 133, 95–109.
Dvorak HF, Nagy JA, Feng D, Brown LF and Dvorak AM . (1999). Curr. Top. Microbiol. Immunol., 237, 97–132.
Eberhard A, Kahlert S, Goede V, Hemmerlein B, Plate KH and Augustin HG . (2000). Cancer Res., 60, 1388–1393.
Ehrmann RL and Knoth M . (1968). J. Natl. Cancer Inst., 41, 1329–1341.
Eriksson U and Alitalo K . (1999). Curr. Top. Microbiol. Immunol., 237, 41–57.
Ferrara N . (1999). Curr. Top. Microbiol. Immunol., 237, 1–30.
Ferrara N, Carver-Moore K, Chen H, Dowd M, Lu L, O'Shea KS, Powell-Braxton L, Hillan KJ and Moore MW . (1996). Nature, 380, 439–442.
Ferrara N and Davis-Smyth T . (1997). Endocr. Rev., 18, 4–25.
Folkman J . (1971). N. Engl. J. Med., 285, 1182–1186.
Folkman J . (1985). Adv. Cancer. Res., 43, 175–203.
Folkman J . (1992). Semin. Cancer Biol., 3, 65–71.
Folkman J . (2002). Semin. Oncol., 29, 15–18.
Folkman J, Merler E, Abernathy C and Williams G . (1971). J. Exp. Med., 133, 275–288.
Forsythe JA, Jiang BH, Iyer NV, Agani F, Leung SW, Koos RD and Semenza GL . (1996). Mol. Cell. Biol., 16, 4604–4613.
Fotsis T, Breit S, Lutz W, Rossler J, Hatzi E, Schwab M and Schweigerer L . (1999). Eur. J. Biochem., 263, 757–764.
Gamble J, Meyer G, Noack L, Furze J, Matthias L, Kovach N, Harlant J and Vadas M . (1999). Endothelium, 7, 23–34.
Gastl G, Hermann T, Steurer M, Zmija J, Gunsilius E, Unger C and Kraft A . (1997). Oncology, 54, 177–184.
Gerety SS, Wang HU, Chen ZF and Anderson DJ . (1999). Mol. Cell, 4, 403–414.
Greenblatt M and Shubik P . (1968). J. Natl. Canc. Inst., 41, 111–124.
Hanai J, Dhanabal M, Karumanchi SA, Albanese C, Waterman M, Chan B, Ramchandran R, Pestell R and Sukhatme VP . (2002). J. Biol. Chem., 277, 16464–16469.
Hashizume H, Baluk P, Morikawa S, McLean JW, Thurston G, Roberge S, Jain RK and McDonald DM . (2000). Am. J. Pathol., 156, 1363–1380.
Helmlinger G, Yuan F, Dellian M and Jain RK . (1997). Nat. Med., 3, 177–182.
Hobbs SK, Monsky WL, Yuan F, Roberts WG, Griffith L, Torchilin VP and Jain RK . (1998). Proc. Natl. Acad. Sci. USA, 95, 4607–4612.
Hogg PJ, Owensby DA and Chesterman CN . (1993a). J. Biol. Chem., 268, 21811–21818.
Hogg PJ, Owensby DA, Mosher DF, Misenheimer TM and Chesterman CN . (1993b). J. Biol. Chem., 268, 7139–7146.
Hong YK, Chung DS, Joe YA, Yang YJ, Kim KM, Park YS, Yung WK and Kang JK . (2000). Clin. Cancer Res., 6, 3354–3360.
Hori A, Sasada R, Matsutani E, Naito K, Sakura Y, Fujita T and Kozai Y . (1991). Cancer Res., 51, 6180–6184.
Ikeda E, Achen MG, Breier G and Risau W . (1995). J. Biol. Chem., 270, 19761–19766.
Jain RK, Koenig GC, Dellian M, Fukumura D, Munn LL and Melder RJ . (1996). Cancer Metastasis Rev., 15, 195–204.
Jiang BH, Agani F, Passaniti A and Semenza GL . (1997). Cancer Res., 57, 5328–5335.
Jimenez B, Volpert OV, Crawford SE, Febbraio M, Silverstein RL and Bouck N . (2000). Nat. Med., 6, 41–48.
Juczewska M and Chyczewski L . (1997). Rocz. Akad. Med. Bialymst., 42 (Suppl 1), 86–100.
Kageyama K, Ihara Y, Goto S, Urata Y, Toda G, Yano K and Kondo T . (2002). J. Biol. Chem., 277, 19255–19264.
Kerbel RS . (2000). Carcinogenesis, 21, 505–515.
Kim YM, Jang JW, Lee OK, Yeon J, Choi EY, Kim KW, Lee ST and Kwon YG . (2000a). Cancer Res., 60, 5410–5413.
Kim I, Kim HG, So JN, Kim JH, Kwak HJ and Koh GY . (2000b). Circ. Res., 86, 24–29.
Klagsbrun M and Moses MA . (1999). Chem. Biol., 6, R217–R224.
Lahm H, Amstad P, Yilmaz A, Fischer JR, Givel JC, Odartchenko N and Sordat B . (1996). Biochem. Biophys. Res. Commun., 220, 334–340.
Landgren E, Schiller P, Cao Y and Claesson-Welsh L . (1998). Oncogene, 16, 359–367.
Liekens S, De Clercq E and Neyts J . (2001). Biochem. Pharmacol., 61, 253–270.
Lingen MW, Polverini PJ and Bouck NP . (1998). Cancer Res., 58, 5551–5558.
Liotta LA and Stetler-Stevenson WG . (1991). Cancer Res., 51, 5054s–5059 s.
MacDonald NJ, Shivers WY, Narum DL, Plum SM, Wingard JN, Fuhrmann SR, Liang H, Holland-Linn J, Chen DH and Sim BK . (2001). J. Biol. Chem., 276, 25190–25196.
Majewski S, Marczak M, Szmurlo A, Jablonska S and Bollag W . (1996). J. Invest. Dermatol., 106, 1114–1118.
Malonne H, Langer I, Kiss R and Atassi G . (1999). Clin. Exp. Metastasis, 17, 1–14.
McDonald DM and Foss AJ . (2000). Cancer Metastasis Rev., 19, 109–120.
Meyer M, Clauss M, Lepple-Wienhues A, Waltenberger J, Augustin HG, Ziche M, Lanz C, Buttner M, Rziha HJ and Dehio C . (1999). EMBO J., 18, 363–374.
Minchenko A, Bauer T, Salceda S and Caro J . (1994). Lab. Invest., 71, 374–379.
Nangia-Makker P, Honjo Y, Sarvis R, Akahani S, Hogan V, Pienta KJ and Raz A . (2000). Am. J. Pathol., 156, 899–909.
Neufeld G, Cohen T, Gengrinovitch S and Poltorak Z . (1999). FASEB J., 13, 9–22.
Nor JE, Mitra RS, Sutorik MM, Mooney DJ, Castle VP and Polverini PJ . (2000). J. Vasc. Res., 37, 209–218.
Ogawa S, Oku A, Sawano A, Yamaguchi S, Yazaki Y and Shibuya M . (1998). J. Biol. Chem., 273, 31273–31282.
Pluda JM . (1997). Semin. Oncol., 24, 203–218.
Potgens AJ, Lubsen NH, van Altena MC, Vermeulen R, Bakker A, Schoenmakers JG, Ruiter DJ and de Waal RM . (1994). J. Biol. Chem., 269, 32879–32885.
Rak J, Filmus J, Finkenzeller G, Grugel S, Marme D and Kerbel RS . (1995a). Cancer Metastasis Rev., 14, 263–277.
Rak J, Mitsuhashi Y, Bayko L, Filmus J, Shirasawa S, Sasazuki T and Kerbel RS . (1995b). Cancer Res., 55, 4575–4580.
Ruiter DJ, Schlingemann RO, Westphal JR, Denijn M, Rietveld FJ and De Waal RM . (1993). Behring Inst. Mitt., 92, 258–272.
Ryan CJ and Wilding G . (2000). Drugs Aging, 17, 249–255.
Sargiannidou I, Zhou J and Tuszynski GP . (2001). Exp. Biol. Med. (Maywood), 226, 726–733.
Scappaticci FA, Smith R, Pathak A, Schloss D, Lum B, Cao Y, Johnson F, Engleman EG and Nolan GP . (2001). Mol. Ther., 3, 186–196.
Shweiki D, Itin A, Soffer D and Keshet E . (1992). Nature, 359, 843–845.
Sierra-Honigmann MR, Nath AK, Murakami C, Garcia-Cardena G, Papapetropoulos A, Sessa WC, Madge LA, Schechner JS, Schwabb MB, Polverini PJ and Flores-Riveros JR . (1998). Science, 281, 1683–1686.
Silverman KJ, Lund DP, Zetter BR, Lainey LL, Shahood JA, Freiman DG, Folkman J and Barger AC . (1988). Biochem. Biophys. Res. Commun., 153, 347–352.
Soff GA . (2000). Cancer Metastasis Rev., 19, 97–107.
Soker S, Takashima S, Miao HQ, Neufeld G and Klagsbrun M . (1998). Cell, 92, 735–745.
Sonobe MH, Bravo R and Armelin MS . (1991). Oncogene, 6, 1531–1537.
Stack MS, Gately S, Bafetti LM, Enghild JJ and Soff GA . (1999). Biochem. J., 340 (Part 1), 77–84.
Suri C, Jones PF, Patan S, Bartunkova S, Maisonpierre PC, Davis S, Sato TN and Yancopoulos GD . (1996). Cell, 87, 1171–1180.
Taraboletti G, Belotti D, Borsotti P, Vergani V, Rusnati M, Presta M and Giavazzi R . (1997). Cell Growth Differ., 8, 471–479.
Taraboletti G, Morbidelli L, Donnini S, Parenti A, Granger HJ, Giavazzi R and Ziche M . (2000). FASEB J., 14, 1674–1676.
Tischer E, Gospodarowicz D, Mitchell R, Silva M, Schilling J, Lau K, Crisp T, Fiddes JC and Abraham JA . (1989). Biochem. Biophys. Res. Commun., 165, 1198–1206.
Tolsma SS, Volpert OV, Good DJ, Frazier WA, Polverini PJ and Bouck N . (1993). J. Cell Biol., 122, 497–511.
Valentinis B, Morrione A, Taylor SJ and Baserga R . (1997). Mol. Cell. Biol., 17, 3744–3754.
Volpert OV, Zaichuk T, Zhou W, Reiher F, Ferguson TA, Stuart PM, Amin M and Bouck NP . (2002). Nat. Med., 8, 349–357.
von Marschall Z, Scholz A, Cramer T, Schafer G, Schirner M, Oberg K, Wiedenmann B, Hocker M and Rosewicz S . (2003). J. Natl. Cancer Inst., 95, 437–448.
Waltenberger J, Claesson-Welsh L, Siegbahn A, Shibuya M and Heldin CH . (1994). J. Biol. Chem., 269, 26988–26995.
Wang HU, Chen ZF and Anderson DJ . (1998). Cell, 93, 741–753.
Werner H, Shalita-Chesner M, Abramovitch S, Idelman G, Shaharabani-Gargir L and Glaser T . (2000). Mol. Genet. Metab., 71, 315–320.
Wheeler DG, Horsford J, Michalak M, White JH and Hendy GN . (1995). Nucleic Acids Res., 23, 3268–3274.
White FC, Benehacene A, Scheele JS and Kamps M . (1997). Growth Factors, 14, 199–212.
Wouters BG, Koritzinsky M, Chiu RK, Theys J, Buijsen J and Lambin P . (2003). Semin. Radiat. Oncol., 13, 31–41.
Yang S, Graham J, Kahn JW, Schwartz EA and Gerritsen ME . (1999). Am. J. Pathol., 155, 887–895.
Yao L, Pike SE and Tosato G . (2002). J. Leukoc. Biol., 71, 47–53.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Tonini, T., Rossi, F. & Claudio, P. Molecular basis of angiogenesis and cancer. Oncogene 22, 6549–6556 (2003). https://doi.org/10.1038/sj.onc.1206816
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.onc.1206816
Keywords
This article is cited by
-
The various role of microRNAs in breast cancer angiogenesis, with a special focus on novel miRNA-based delivery strategies
Cancer Cell International (2023)
-
Newly synthesized methionine aminopeptidase 2 inhibitor hinders tumor growth
Drug Delivery and Translational Research (2023)
-
Understanding the process of angiogenesis in regenerating earthworm
In Vitro Cellular & Developmental Biology - Animal (2023)
-
Preclinical evaluation of a dual-receptor targeted tracer [68Ga]Ga-HX01 in 10 different subcutaneous and orthotopic tumor models
European Journal of Nuclear Medicine and Molecular Imaging (2023)
-
Nanoengineered drug delivery in cancer immunotherapy for overcoming immunosuppressive tumor microenvironment
Drug Delivery and Translational Research (2023)