Abstract
Background:
Epidemiologic studies of body mass index (BMI) in relation to mortality commonly exclude persons with health conditions and/or a history of smoking to prevent bias resulting from illness-related weight loss (‘reverse causation’). Analysis of BMI from an earlier time period may minimize reverse causation without requiring exclusion of participants based on disease or smoking history.
Methods:
We prospectively examined BMI based on technician measurements of weight and height from 10 years prior to start of follow-up in relation to subsequent mortality in a cohort of 50 186 women who were 40–93 years old at baseline in 1987–1989. Deaths were ascertained through the US National Death Index. Proportional hazards regression was used to estimate hazard ratios (HRs) of mortality, adjusted for age, education, race/ethnicity, income, menopausal hormone use, smoking and physical activity.
Results:
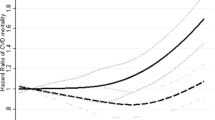
During 10 years of follow-up through 1997, 5201 women died. Overall, we observed a J-shaped association between BMI and mortality, with increased risk for women who were underweight, overweight or obese. The HRs and 95% confidence intervals of mortality for BMI categories of <18.5, 18.5–20.9, 21.0–23.4 (reference), 23.5–24.9, 25.0–27.4, 27.5–29.9, 30.0–34.9 and 35.0+ kg m−2 were 1.43 (1.19, 1.72), 1.07 (0.98, 1.17), 1.00 (reference), 1.10 (1.00, 1.20), 1.20 (1.11, 1.31), 1.23 (1.11, 1.37), 1.60 (1.44, 1.77) and 1.92 (1.64, 2.24). There was little evidence that pre-existing conditions (heart disease, diabetes and/or cancer) or smoking history modified the past BMI and mortality relation (P=0.54 and 0.76).
Conclusions:
In this large cohort of women, BMI based on technician measurements of weight and height from 10 years prior to baseline showed increased risk for mortality across the range of overweight and obesity, regardless of disease and smoking history. Observed associations between overweight, obesity and mortality in healthy individuals may also apply to persons with a history of disease or smoking.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Manson JE, Willett WC, Stampfer MJ, Colditz GA, Hunter DJ, Hankinson SE et al. Body weight and mortality among women. N Engl J Med 1995; 333: 677–685.
Calle EE, Thun MJ, Petrelli JM, Rodriguez C, Heath Jr CW . Body-mass index and mortality in a prospective cohort of U.S. adults. N Engl J Med 1999; 341: 1097–1105.
Flegal KM, Graubard BI, Williamson DF, Gail MH . Excess deaths associated with underweight, overweight, and obesity. JAMA 2005; 293: 1861–1867.
Gu D, He J, Duan X, Reynolds K, Wu X, Chen J et al. Body weight and mortality among men and women in China. JAMA 2006; 295: 776–783.
Dey DK, Rothenberg E, Sundh V, Bosaeus I, Steen B . Body mass index, weight change and mortality in the elderly. A 15 y longitudinal population study of 70 y olds. Eur J Clin Nutr 2001; 55: 482–492.
Breeze E, Clarke R, Shipley MJ, Marmot MG, Fletcher AE . Cause-specific mortality in old age in relation to body mass index in middle age and in old age: follow-up of the Whitehall cohort of male civil servants. Int J Epidemiol 2006; 35: 169–178.
Ogden CL, Carroll MD, Curtin LR, McDowell MA, Tabak CJ, Flegal KM . Prevalence of overweight and obesity in the United States, 1999–2004. JAMA 2006; 295: 1549–1555.
Prentice AM . The emerging epidemic of obesity in developing countries. Int J Epidemiol 2006; 35: 93–99.
Willett WC, Dietz WH, Colditz GA . Guidelines for healthy weight. N Engl J Med 1999; 341: 427–434.
Stevens J, Juhaeri, Cai J . Changes in body mass index prior to baseline among participants who are ill or who die during the early years of follow-up. Am J Epidemiol 2001; 153: 946–953.
Stevens J . Impact of age on associations between weight and mortality. Nutr Rev 2000; 58: 129–137.
Centers for Disease Control and Prevention (CDC). Cigarette smoking-attributable morbidity—United States, 2000. MMWR Morb Mortal Wkly Rep 2003; 52: 842–844.
Flegal KM, Graubard BI, Gail MH, Williamson DF . Underweight, overweight, obesity, and excess deaths—reply. JAMA 2005; 294: 552b.
Society of Actuaries and the Association of Life Insurance Medical Directors of America. Build Study 1979, 1st edn. Society of Actuaries and the Association of Life Insurance Medical Directors of America: Chicago, 1999.
Blair BF, Haines LW . Mortality experience according to build at the higher durations. Trans Soc Actuaries 1966; 18: 35–45.
Calle EE, Teras LR, Thun MJ . Obesity and mortality. N Engl J Med 2005; 353: 2197–2199.
Losonczy KG, Harris TB, Cornoni-Huntley J, Simonsick EM, Wallace RB, Cook NR et al. Does weight loss from middle age to old age explain the inverse weight mortality relation in old age? Am J Epidemiol 1995; 141: 312–321.
van Dam RM, Willett WC, Manson JE, Hu FB . The relationship between overweight in adolescence and premature death in women. Ann Intern Med 2006; 145: 91–97.
Adams KF, Schatzkin A, Harris TB, Kipnis V, Mouw T, Ballard-Barbash R et al. Overweight, obesity, and mortality in a large prospective cohort of persons 50 to 71 years old. N Engl J Med 2006; 355: 763–778.
Beahrs OH, Shapiro S, Smart CR . Report of the working group to review the National Cancer Institute–American Cancer Society Breast Cancer Detection Demonstration Projects. J Natl Cancer Inst 1979; 62: 639–709.
Schairer C, Byrne C, Keyl PM, Brinton LA, Sturgeon SR, Hoover RN . Menopausal estrogen and estrogen–progestin replacement therapy and risk of breast cancer (United States). Cancer Causes Control 1994; 5: 491–500.
Munoz KA, Ballard-Barbash R, Graubard B, Swanson CA, Schairer C, Kahle LL . Recall of body weight and body size estimation in women enrolled in the breast cancer detection and demonstration project (BCDDP). Int J Obes Relat Metab Disord 1996; 20: 854–859.
Colbert LH, Lacey Jr JV, Schairer C, Albert P, Schatzkin A, Albanes D . Physical activity and risk of endometrial cancer in a prospective cohort study (United States). Cancer Causes Control 2003; 14: 559–567.
Albanes D, Conway JM, Taylor PR, Moe PW, Judd J . Validation and comparison of eight physical activity questionnaires. Epidemiology 1990; 1: 65–71.
Rich-Edwards JW, Corsano KA, Stampfer MJ . Test of the national death index and Equifax nationwide death search. Am J Epidemiol 1994; 140: 1016–1019.
World Health Organization. Physical status: the use and interpretation of anthropometry. Report of a WHO expert committee. World Health Organ Tech Rep Ser 1995; 1995: 1–452.
Kant AK, Schatzkin A, Graubard BI, Schairer C . A prospective study of diet quality and mortality in women. JAMA 2000; 283: 2109–2115.
Durrleman S, Simon R . Flexible regression models with cubic splines. Stat Med 1989; 8: 551–561.
Ghali WA, Quan H, Brant R, van Melle G, Norris CM, Faris PD et al. Comparison of 2 methods for calculating adjusted survival curves from proportional hazards models. JAMA 2001; 286: 1494–1497.
Korn EL, Graubard BI . Analysis of Health Surveys, 1st edn. Wiley: New York, 1999.
Efron B, Tibshirani RJ . An Introduction to the Bootstrap, 1st edn. Chapman & Hall: New York, 1993.
Fontaine KR, Redden DT, Wang C, Westfall AO, Allison DB . Years of life lost due to obesity. JAMA 2003; 289: 187–193.
Peeters A, Barendregt JJ, Willekens F, Mackenbach JP, Al Mamun A, Bonneux L . Obesity in adulthood and its consequences for life expectancy: a life-table analysis. Ann Intern Med 2003; 138: 24–32.
Perry GS, Byers TE, Mokdad AH, Serdula MK, Williamson DF . The validity of self-reports of past body weights by U.S. adults. Epidemiology 1995; 6: 61–66.
Romero-Corral A, Montori VM, Somers VK, Korinek J, Thomas RJ, Allison TG et al. Association of bodyweight with total mortality and with cardiovascular events in coronary artery disease: a systematic review of cohort studies. Lancet 2006; 368: 666–678.
The BMI in Diverse Populations Collaborative Group. Effect of smoking on the body mass index–mortality relation: empirical evidence from 15 studies. Am J Epidemiol 1999; 150: 1297–1308.
Folsom AR, Kaye SA, Sellers TA, Hong CP, Cerhan JR, Potter JD et al. Body fat distribution and 5-year risk of death in older women. JAMA 1993; 269: 483–487.
Corrada MM, Kawas CH, Mozaffar F, Paganini-Hill A . Association of body mass index and weight change with all-cause mortality in the elderly. Am J Epidemiol 2006; 163: 938–949.
Allison DB, Faith MS, Heo M, Townsend-Butterworth D, Williamson DF . Meta-analysis of the effect of excluding early deaths on the estimated relationship between body mass index and mortality. Obes Res 1999; 7: 342–354.
Lange P, Vestbo J, Nyboe J . Risk factors for death and hospitalization from pneumonia. A prospective study of a general population. Eur Respir J 1995; 8: 1694–1698.
Sacks LV, Pendle S . Factors related to in-hospital deaths in patients with tuberculosis. Arch Intern Med 1998; 158: 1916–1922.
Acknowledgements
This study was supported by the Intramural Research Program and TU2CA105666 from the National Cancer Institute, National Institutes of Health. We have no conflict of interest relevant to this study. The views expressed are those of the authors. We thank Leslie Carroll and Matthew Butcher at Information Management Services and Tawanda Roy at the Nutritional Epidemiology Branch for research assistance.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Moore, S., Mayne, S., Graubard, B. et al. Past body mass index and risk of mortality among women. Int J Obes 32, 730–739 (2008). https://doi.org/10.1038/sj.ijo.0803801
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.ijo.0803801
Keywords
This article is cited by
-
Relationship between body mass index and mortality among Europeans
European Journal of Clinical Nutrition (2012)
-
Body mass index and mortality in an ethnically diverse population: the Multiethnic Cohort Study
European Journal of Epidemiology (2012)
-
Individual and Aggregate Years‐of‐life‐lost Associated With Overweight and Obesity
Obesity (2010)
-
Relationships of dietary patterns with body composition in older adults differ by gender and PPAR-γ Pro12Ala genotype
European Journal of Nutrition (2010)
-
BMI and mortality: sorting through the data to find the public health message
International Journal of Obesity (2008)