Abstract
Background:
Cross-sectional studies have shown that vegetarians and vegans are leaner than omnivores. Longitudinal data on weight gain in these groups are sparse.
Objective:
We investigated changes in weight and body mass index (BMI) over a 5-year period in meat-eating, fish-eating, vegetarian, and vegan men and women in the UK.
Design:
Self-reported anthropometric, dietary and lifestyle data were collected at baseline in 1994–1999 and at follow-up in 2000–2003; the median duration of follow-up was 5.3 years.
Subjects:
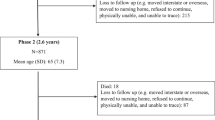
A total of 21 966 men and women participating in Oxford arm of the European Prospective Investigation into Cancer and Nutrition aged 20–69 years at baseline.
Results:
The mean annual weight gain was 389 (SD 884) g in men and 398 (SD 892) g in women. The differences between meat-eaters, fish-eaters, vegetarians and vegans in age-adjusted mean BMI at follow-up were similar to those seen at baseline. Multivariable-adjusted mean weight gain was somewhat smaller in vegans (284 g in men and 303 g in women, P<0.05 for both sexes) and fish-eaters (338 g, women only, P<0.001) compared with meat-eaters. Men and women who changed their diet in one or several steps in the direction meat-eater → fish-eater → vegetarian → vegan showed the smallest mean annual weight gain of 242 (95% CI 133–351) and 301 (95% CI 238–365) g, respectively.
Conclusion:
During 5 years follow-up, the mean annual weight gain in a health-conscious cohort in the UK was approximately 400 g. Small differences in weight gain were observed between meat-eaters, fish-eaters, vegetarians and vegans. Lowest weight gain was seen among those who, during follow-up, had changed to a diet containing fewer animal food.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others

References
Swinburn BA, Caterson I, Seidell JC, James WPT . Diet, nutrition and the prevention of excess weight gain and obesity. Public Health Nutr 2004; 7: 123–146.
Anderson JW, Konz EC, Frederich RC, Wood CL . Long-term weight-loss maintenance: a meta-analysis of US studies. Am J Clin Nutr 2001; 74: 579–584.
Appleby PN, Thorogood M, Mann J, Key TJ . Low body mass index in non-meat eaters: the possible roles of animal fat, dietary fibre and alcohol. Int J Obes Relat Metab Disord 1998; 22: 454–460.
Fraser GE . Associations between diet and cancer, ischemic heart disease, and all-cause mortality in non-Hispanic white California Seventh-day Adventists. Am J Clin Nutr 1999; 70 (Suppl): 532S–538S.
Spencer EA, Appleby PN, Davey GK, Key TJ . Diet and body mass index in 38 000 EPIC-Oxford meat-eaters, fish-eaters, vegetarians and vegans. Int J Obes Relat Metab Disord 2003; 27: 728–734.
Key TJ, Fraser GE, Thorogood M, Appleby PN, Beral V, Reeves G et al. Mortality in vegetarians and nonvegetarians: detailed findings from a collaborative analysis of 5 prospective studies. Am J Clin Nutr 1999; 70 (3 Suppl): 516S–524S.
Newby PK, Katherine LT, Wolk A . Risk of overweight and obesity among semivegetarian, lactovegetarian, and vegan women. Am J Clin Nutr 2005; 81: 1267–1274.
Key T, Davey G . Prevalence of obesity is low in people who do not eat meat. Br Med J 1996; 313: 816–817.
Fraser GE . Diet, Life Expectancy, and Chronic Disease. Studies of Seventh-day Adventists and Other Vegetarians. Oxford University Press: New York, 2003. pp 132–134.
Davey GK, Spencer EA, Appleby PN, Allen NE, Knox KH, Key TJ . EPIC-Oxford: lifestyle characteristics and nutrient intakes in a cohort of 33 883 meat-eaters and 31 546 non meat-eaters in the UK. Public Health Nutr 2003; 6: 259–269.
Spencer EA, Appleby PN, Davey GD, Key TJ . Validity of self-reported height and weight in 4808 EPIC-Oxford participants. Public Health Nutr 2001; 5: 561–565.
Wareham NJ, Jakes RW, Rennie KL, Shuit J, Mitchell J, Hennings S et al. Validity and repeatability of a simple index derived from the short physical activity questionnaire used in the European Prospective Investigation into Cancer and Nutrition (EPIC) study. Public Health Nutr 2003; 6: 407–413.
Cade JE, Burley VJ, Greenwood DC, and the UK Women's Cohort Study Steering Group. The UK Women's Cohort Study: comparison of vegetarians, fish-eaters and meat-eaters. Public Health Nutr 2004; 7: 871–878.
Haddad EH, Tanzman JS . What do vegetarians in the United States eat? Am J Clin Nutr 2003; 78 (Suppl): 626S–632S.
Koh-Banerjee P, Chu N-F, Spiegelman D, Rosner B, Colditz G, Willett W et al. Prospective study of the association of changes in dietary intake, physical activity, alcohol consumption, and smoking with 9-y gain in waist circumference among 16 587 US men. Am J Clin Nutr 2003; 78: 719–727.
Liu S, Willett WC, Manson JE, Hu FB, Rosner B, Colditz G . Relation between changes in intakes of dietary fiber and grain products and changes in weight and development of obesity among middle-aged women. Am J Clin Nutr 2003; 78: 920–927.
Ludwig DS, Pereira MA, Kroenke CH, Hilner JE, Slattery ML, Jacobs Jr DR . Dietary fiber, weight gain, and cardiovascular disease risk factors in young adults. JAMA 1999; 282: 1539–1546.
WHO. Diet nutrition and the prevention of chronic diseases: report of a joint WHO/FAO expert consultation. WHO Technical Report Series 916. Geneva, Switzerland, 2003.
Katz DL . Pandemic obesity and the contagion of nutritional nonsense. Public Health Rev 2003; 31: 33–44.
Bravata DM, Sanders L, Huang J, Krumholz HM, Olkin I, Gardner CD . Efficacy and safety of low-carbohydrate diets. A systematic review. JAMA 2003; 289: 1837–1850.
Astrup A, Larsen TM, Harper A . Atkins and other low-carbohydrate diets: hoax or an effective tool for weight loss? Lancet 2004; 364: 897–899.
Sternfeld B, Wang H, Quesenberry CP, Abrams B, Everson-Rose SA, Greendale GA et al. Physical activity and changes in weight and waist circumference in midlife women: findings from the Study of Women's Health Across the Nation. Am J Epidemiol 2004; 160: 912–922.
Schmitz KH, Jacobs Jr DR, Leon AS, Schreiner PJ, Sternfeld B . Physical activity and body weight: associations over ten years in the CARDIA study. Coronary Artery Risk Development in Young Adults. Int J Obes Relat Metab Disord 2000; 24: 1475–1487.
Williamson DF, Madans J, Anda RF, Kleinman JC, Kahn HS, Byers T . Recreational physical activity and ten-year weight change in a US national cohort. Int J Obes Relat Metab Disord 1993; 17: 279–286.
Owens JF, Matthews KA, Wing RR, Kuller LH . Can physical activity mitigate the effects of aging in middle-aged women? Circulation 1992; 85: 1265–1270.
Sherwood NE, Jeffery RW, French SA, Hannan PJ, Murray DM . Predictors of weight gain in the Pound of Prevention study. Int J Obes Relat Metab Disord 2000; 24: 395–403.
Taylor CB, Jatulis DE, Winkleby MA, Rockhill BJ, Kraemer HC . Effects of life-style on body mass index change. Epidemiology 1994; 5: 599–603.
Klesges RC, Klesges LM, Haddock CK, Eck LH . A longitudinal analysis of the impact of dietary intake and physical activity on weight change in adults. Am J Clin Nutr 1992; 55: 818–822.
Filozof C, Fernandes Pinilla MC, Fernandes-Cruz A . Smoking cessation and weight gain. Obes Rev 2004; 5: 95–103.
Jeffery RW, Rick AM . Cross-sectional and longitudinal associations between body mass index and marriage-related factors. Obes Res 2002; 10: 809–815.
Eng PM, Kawachi I, Fitzmaurice G, Rimm EB . Effects of marital status on changes in dietary and other health behaviours in US male health professionals. J Epidemiol Commun Health 2005; 59: 56–62.
Sobal J, Rauschenbach B, Frongillo EA . Marital status changes and body weight changes: a US longitudinal analysis. Soc Sci Med 2003; 56: 1543–1555.
Kahn HS, Williamson DF . The contributions of income, education and changing marital status to weight change among US men. Int J Obes Relat Metab Disord 1990; 14: 1057–1068.
Umberson D . Gender, marital status and the social control of health behaviour. Soc Sci Med 1992; 34: 907–917.
Lee S, Cho E, Grodstein F, Kawachi I, Hu FB, Colditz GA . Effects of marital transitions on changes in dietary and other health behaviours in US women. Int J Epidemiol 2005; 34: 69–78.
Lund R, Holstein BE, Osler M . Marital history from age 15–40 years and subsequent 10-year mortality: a longitudinal study of Danish males born in 1953. Int J Epidemiol 2004; 33: 389–397.
Ebrahim S, Wannamethee G, McCallum A, Walker M, Shaper AG . Marital status, change in marital status, and mortality in middle-aged British men. Am J Epidemiol 1995; 142: 834–842.
Johnson NJ, Backlund E, Sorlie PD, Loveless CA . Marital status and mortality: the national longitudinal mortality study. Ann Epidemiol 2000; 10: 224–238.
Lahmann PH, Lissner L, Gullberg B, Berglund G . Sociodemographic factors associated with long-term weight gain, current body fatness and central adiposity in Swedish women. Int J Obes Relat Metab Disord 2000; 24: 685–694.
Wen W, Gao YT, Shu XO, Yang G, Li HL, Jin F et al. Sociodemographic, behavioural, and reproductive factors associated with weight gain in Chinese women. Int J Obes Relat Metab Disord 2003; 27: 933–940.
Ball K, Crawford D . Socioeconomic status and weight change in adults: a review. Soc Sci Med 2005; 60: 1987–2010.
Laitinen J, Power C, Jarvelin M-R . Family social class, maternal body mass index, childhood body mass index, and age at menarche as predictors of adult obesity. Am J Clin Nutr 2001; 74: 287–294.
Okasha M, McCarron P, McEven J, Smith GD . Age at menarche: secular trends and association with adult anthropometric measures. Ann Hum Biol 2001; 28: 68–78.
vanLenthe FJ, Kemper CG, Mechelen W . Rapid maturation in adolescence results in greater obesity in adulthood: the Amsterdam Growth and Health Study. Am J Clin Nutr 1996; 64: 18–24.
Adair LS, Gordon-Larsen P . Maturational timing and overweight prevalence in US adolescent girls. Am J Public Health 2001; 91: 642–644.
Freedman DS, Khan LK, Serdula MK, Dietz WH, Srinivasan SR, Berenson GS . The relation of menarcheal age to obesity in childhood and adulthood: the Bogalusa heart study. BMC Pediatr 2003, http://www.biomedcentral.com/1471-2431/3/3 (accessed Jan 2005).
Social Survey Division of OPCS with Dietary and Nutritional Evaluations by the Ministry of Agriculture, Fisheries and Food and the Department of Health. The Dietary and Nutritional Survey of British Adults. HMSO: London, UK, 1990.
Food Standards Agency and the Departments of Health by the Office for National Statistics and Medical Research Council Human Nutrition Research. The National Diet and Nutrition Survey: adults aged 19 to 64 years. HMSO: Norwich, UK, 2004.
Hill JO, Wyatt HR, Reed GW, Peters JC . Obesity and the environment: where do we go from here? Science 2003; 299: 853–855.
Swinburn B, Egger G . The runaway weight train: too many accelerators, not enough brakes. Br Med J 2004; 329: 736–739.
Acknowledgements
We thank all participants in this study and the EPIC-Oxford study staff at the Cancer Research UK Epidemiology Unit. EPIC-Oxford is supported by Cancer Research UK and the Medical Research Council. MR was supported by a grant from the Swedish Council for Working Life and Social Research.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Rosell, M., Appleby, P., Spencer, E. et al. Weight gain over 5 years in 21 966 meat-eating, fish-eating, vegetarian, and vegan men and women in EPIC-Oxford. Int J Obes 30, 1389–1396 (2006). https://doi.org/10.1038/sj.ijo.0803305
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.ijo.0803305
Keywords
This article is cited by
-
Trend changes in age-related body mass index gain after coronavirus disease 2019 pandemic in Japan: a multicenter retrospective cohort study
Reproductive Biology and Endocrinology (2023)
-
Vegetarian and vegan diets and the risk of cardiovascular disease, ischemic heart disease and stroke: a systematic review and meta-analysis of prospective cohort studies
European Journal of Nutrition (2023)
-
Risk of cancer in regular and low meat-eaters, fish-eaters, and vegetarians: a prospective analysis of UK Biobank participants
BMC Medicine (2022)
-
Optimal annual body mass index change for preventing spontaneous preterm birth in a subsequent pregnancy
Scientific Reports (2022)
-
Annual body mass index gain and risk of hypertensive disorders of pregnancy in a subsequent pregnancy
Scientific Reports (2021)