Abstract
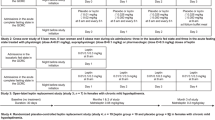
Leptin resistance is a hallmark of obesity, but its etiology is unknown, and its clinical measurement is elusive. Leptin-sensitive subjects have normal resting energy expenditure (REE) at a low leptin concentration, while leptin-resistant subjects have a normal REE at a higher leptin concentration; thus, the ratio of REE:Leptin may provide a surrogate index of leptin sensitivity. We examined changes in REE and leptin in a cohort of 17 obese subjects during experimental weight loss therapy with the insulin-suppressive agent octreotide-LAR, 40 mg i.m. q28d for 6 months. Six subjects lost significant weight (>10%) and BMI (>−3 kg/m2) with a 34% decline in leptin and a 46% decrease in insulin area under the curve (IAUC) to oral glucose tolerance testing. These subjects maintained their pretreatment REE, and thus exhibited a rise in REE:Leptin, while the other 11 showed minimal changes in each of these parameters. For the entire cohort, the change in IAUC correlated negatively with the change in REE:Leptin. These results suggest that the REE:Leptin ratio, while derivative, may serve as a useful clinical indicator of changes in leptin sensitivity within obese subjects. They also support the possibilities that hyperinsulinemia may be a proximate cause of leptin resistance, and that reduction of insulinemia may promote weight loss by improving leptin sensitivity.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Heymsfield SB, Greenberg AS, Fujioka K, Dixon RM, Kushner R, Hunt T, Lubina JA, Patane J, Self B, Hunt P, McCamish M . Recombinant leptin for weight loss in obese and lean adults: a randomized, controlled, dose-escalation trial. JAMA 1999; 282: 1568–1575.
Leibel RL, Rosenbaum M, Hirsch J . Changes in energy expenditure resulting from altered body weight. N Engl J Med 1995; 332: 621–628.
Rosenbaum M, Murphy EM, Heymsfield SB, Matthews DE, Leibel RL . Low dose leptin administration reverses effects of sustained weight reduction on energy expenditure and circulating concentrations of thyroid hormones. J Clin Endocrinol Metab 2002; 87: 2391–2394.
Ferrannini E, Natali A, Bell P, Cavallo-Perin P, Lalic N, Mingrone G . Insulin resistance and hypersecretion in obesity. J Clin Invest 1997; 100: 1166–1173.
Barr VA, Malide D, Zarnowski MJ, Taylor SI, Cushman SW . Insulin stimulates both leptin secretion and production by white adipose tissue. Endocrinology 1997; 138: 4463–4472.
Boden G, Chen X, Kolaczynski JW, Polansky M . Effects of prolonged hyperinsulinemia on serum leptin in normal human subjects. J Clin Invest 1997; 100: 1107–1113.
Kolaczynski JW, Nyce MR, Considine RV, Boden G, Nolan JJ, Henry R, Mudaliar SR, Olefsky J, Caro JF . Acute and chronic effects of insulin on leptin production in humans: studies in vivo and in vitro. Diabetes 1996; 45: 699–701.
Keim NL, Stern JS, Havel PJ . Relation between circulating leptin concentrations and appetite during a prolonged, moderate energy deficit in women. Am J Clin Nutr 1998; 68: 794–801.
Giustina A, Bussi AR, Pizzocolo G, Cimino A, Giustina G . Acute effects of octreotide, a long-acting somatostatin analog, on the insulinemic and glycemic responses to a mixed meal in patients with essential obesity: a dose-response study. Diabetes Nutr Metab 1994; 7: 35–41.
Lustig RH, Rose SR, Burghen GA, Velasquez-Mieyer P, Broome DC, Smith K, Li H, Hudson MM, Heideman RL, Kun LE . Hypothalamic obesity in children caused by cranial insult: altered glucose and insulin dynamics, and reversal by a somatostatin agonist. J Pediatr 1999; 135: 162–168.
Lustig RH, Hinds PS, Ringwald-Smith K, Christensen RK, Kaste SC, Schreiber RE, Rai SN, Lensing SY, Wu S, Xiong X . Octreotide therapy of pediatric hypothalamic obesity: a double-blind, placebo-controlled trial. J Clin Endocrinol Metab 2003; 88: 2586–2592.
Velasquez-Mieyer PA, Cowan PA, Buffington CK, Arheart KL, Cowan GSM, Connelly BE, Spencer KA, Lustig RH . Suppression of insulin secretion promotes weight loss and alters macronutrient preference in a subset of obese adults. Int J Obes Relat Metab 2003; 27: 219–226.
Lustig R, Greenway F, Velasquez-Mieyer P, Heimberger D, Schumacher D, Smith D, Smith W, Soler N, Zhu W, Hedrick J, Hohneker J . Weight loss in obese adults with insulin hypersecretion (IH) treated with Sandostatin LAR® Depot, 2003. NAASO OR-103 abstract, Obesity Research 2003; 11: A25.
Hutley LJ, Newell FM, Joyner JM, Suchting SJ, Herington AC, Cameron DP, Prins JB . Effects of rosiglitazone and linoleic acid on human preadipocyte differentiation. Eur J Clin Invest 2003; 33: 574–581.
Reaven GM, Brand RJ, Chen YDI, Mathur AK, Goldfine I . Insulin resistance and insulin secretion are determinants of oral glucose tolerance in normal individuals. Diabetes 1993; 42: 1324–1332.
Toft I, Bonaa KH, Lindal S, Jenssen T . Insulin kinetics, insulin action, and muscle morphology in lean or slightly overweight persons with impaired glucose tolerance. Metabolism 1998; 47: 348–354.
Kadish AH, Little RH, Sternberg JC . A new and rapid method for the determination of glucose by measurement of rate of oxygen consumption. Clin Chem 1968; 14: 116–119.
Banks WA, Kastin AJ, Huang W, Jaspan JB, Maness LM . Leptin enters the brain by a saturable system independent of insulin. Peptides 1996; 17: 305–311.
Schwartz MW, Peskind E, Raskind M, Boyko EJ, Porte D . Cerbrospinal fluid leptin levels: relationship to plasma levels and to adiposity in humans. Nat Med 1996; 2: 589–593.
Caro JF, Kolaczynski JW, Nyce MR, Ohannesian JP, Opentanova I, Goldman WH, Lynn RB, Zhang PL, Sinha MK, Considine RV . Decreased cerebrospinal fluid/serum leptin ratio in obesity: a possible mechanism for leptin resistance. Lancet 1996; 348: 159–161.
Bjorkbaek C, Elmquist JK, Frantz JD, Shoelson SE, Flier JS . Identification of SOCS-3 as a potential mediator of central leptin resistance. Mol Cell 1998; 1: 619–625.
El-Haschimi K, Pierroz DD, Hileman SM, Bjorbaek C, Flier JS . Two defects contribute to hypothalamic leptin resistance in mice with diet-induced obesity. J Clin Invest 2000; 105: 1827–1832.
Rosenbaum M, Nicolson M, Hirsch J, Murphy E, Chu F, Leibel RL . Effects of weight change on plasma leptin concentrations and energy expenditure. J Clin Endocrinol Metab 1997; 82: 3647–3564.
Guven S, El-Bershawi A, Sonnenberg GE, Wilson CR, Hoffman RG, Krakower GR, Kissebah AH . Plasma leptin and insulin levels in weight-reduced obese women with normal body mass index: relationships with body composition and insulin. Diabetes 1999; 48: 347–352.
Shi ZQ, Chinookoswong N, Wang JL, Korach E, Lebel C, DePaoli A, Davis W, Burton-Freeman B, Navratil A, Spancake C, Martin D . Additive effects of leptin and oral anti-obesity drugs in treating diet-induced obesity in rats. Diabetes 2002; 51 (Suppl 2): 1707.
Foster GD, Wyatt HR, Hill JO, McGuckin BG, Brill C, Mohammed BS, Szapary PO, Rader DJ, Edman JS, Klein S . A randomized trial of a low-carbohydrate diet for obesity. N Engl J Med 2003; 348: 2082–2090.
Niswender KD, Morton GJ, Stearns WH, Rhodes CJ, Myers MG, Schwartz MW . Intracellular signaling. Key enzyme in leptin-induced anorexia. Nature 2001; 413: 794–795.
Niswender KD, Schwartz MW . Insulin and leptin revisited: adiposity signals with overlapping physiological and intracellular signaling capabilities. Front Neuroendocrinol 2003; 24: 1–10.
Acknowledgements
The funding for this study was provided in part by Novartis Pharmaceuticals Corporation and the University of Tennessee General Clinical Research Center (5M01RR 00211). This work was presented in part at The Endocrine Society 85th Annual Meeting, Philadelphia, PA, USA, June 2003.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Lustig, R., Sen, S., Soberman, J. et al. Obesity, leptin resistance, and the effects of insulin reduction. Int J Obes 28, 1344–1348 (2004). https://doi.org/10.1038/sj.ijo.0802753
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.ijo.0802753
Keywords
This article is cited by
-
Role of Glucagon-Like Peptide-1 in Appetite Regulation in Patients with Morbid Obesity and Leptin Resistance
International Journal of Peptide Research and Therapeutics (2020)
-
Chronic consumption of the dietary polyphenol chrysin attenuates metabolic disease in fructose-fed rats
European Journal of Nutrition (2020)
-
Postprandial leptin and adiponectin in response to sugar and fat in obese and normal weight individuals
Endocrine (2019)
-
Neurobiology of food choices—between energy homeostasis, reward system, and neuroeconomics
e-Neuroforum (2016)