Abstract
CONTEXT: Long-term success in weight loss with dietary treatment has been elusive.
OBJECTIVE: To evaluate a diet moderate in fat based on the Mediterranean diet compared to a standard low-fat diet for weight loss when both were controlled for energy.
DESIGN: A randomized, prospective 18 month trial in a free-living population.
PATIENTS: A total of 101 overweight men and women (26.5–46 kg/m2).
INTERVENTION: (1) Moderate-fat diet (35% of energy); (2) low-fat diet (20% of energy).
MAIN OUTCOME MEASUREMENTS: Change in body weight.
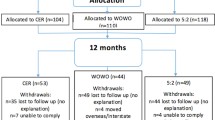
RESULTS: After 18 months, 31/50 subjects in the moderate-fat group, and 30/51 in the low fat group were available for measurements. In the moderate-fat group, there were mean decreases in body weight of 4.1 kg, body mass index of 1.6 kg/m2, and waist circumference of 6.9 cm, compared to increases in the low-fat group of 2.9 kg, 1.4 kg/m2 and 2.6 cm, respectively; P≤0.001 between the groups. The difference in weight change between the groups was 7.0 kg. (95% CI 5.3, 8.7). Only 20% (10/51) of those in the low-fat group were actively participating in the weight loss program after 18 months compared to 54% (27/50) in the moderate-fat group, (P<0.002). The moderate-fat diet group was continued for an additional year. The mean weight loss after 30 months compared to baseline was 3.5 kg (n=19, P=0.03).
CONCLUSIONS: A moderate-fat, Mediterranean-style diet, controlled in energy, offers an alternative to a low-fat diet with superior long-term participation and adherence, with consequent improvements in weight loss.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Kuczmarski RJ, Carroll MO, Flegal KM, Troiano RP . Varying body mass index cutoff points to describe overweight prevalence among US adults: NHANES III (1988–1994) Obes Res 1997 5: 542–548.
National Institutes of Health/National Heart, Lung, and Blood Institute/Obesity Education Initiative Expert Panel . Identification, evaluation, and treatment of overweight and obesity in adults Obesity Res 1998 6: (Suppl 2): 51S–209S.
Bray GA . Obesity: a time bomb to be defused. (Comment.) Lancet 1998 352: 160–161.
Jeffery RW, Hellerstedt WL, French SA, Baxter JE . A randomized trial of counseling for fat restriction versus calories restriction in the treatment of obesity Int J Obes Relat Metab Disord 1995 19: 132–137.
Kinsell LW, Schlierf G . Alimentary and nonalimentary hyperglyceridemia Ann NY Acad Sci 1965 131: 603–613.
Bray GA . The obese patient. Major problems in internal medicine Vol 9: W.B. Saunders: Philadelphia, PA 1976
Sacks FM . Dietary prevention trials. In: Hennekens CH, Buring JE, Manson JE, Ridker PM (eds). Clinical trials in cardiovascular disease: a companion to Braunwald's Heart Disease. WB Saunders: Philadelphia, PA 1999 423–431.
Davis PO, Dotson CO, Manny P . NIR evaluation for body composition analysis Med Sci Sports Exercise 1988 20.
Rimm EB, Giovanucci EL, Stampfer MJ, Colditz GA, Litin LB, Willett WC . Reproducibility and validity of an expanded self-administered semi-quantitative food frequency questionnaire among male health professionals Am J Epidemiol 1992 135: 1114–1126.
Feskanich D, Rimm EB, Giovanucci et al. Reproducibility and validity of food intake measurements from semiquantitative food frequency questionnaire J Am Diet Assoc 1993 93: 790–796.
Blair SN, Haskell WL, Ho P et al. Assessment of habitual physical activity by a seven-day recall in a community survey and controlled experiments Am J Epidemiol 1985 122: 794–804.
SAS Institute Inc . SAS/STAT User's Guide, version 6, 4th edn. SAS Institute: Chicago, IL 1989
Johnson RK, Goran MI, Poehlman ET . Correlates of over- and underreporting of energy intake in healthy older men and women Am J Clin Nutr 1994 59: 1286–1290.
Lichtman SW, Pisarska K, Berman EK et al. Discrepancy between self-reported and actual caloric intake and exercise in obese subjects New Engl J Med 1992 327: 1893–1989.
Schlundt DG, Hill JO, Popie-Cordle J et al. Randomized evaluation of a low fat ad libitum carbohydrate diet for weight reduction Int J Obes Relat Metab Disord 1993 17: 623–629.
Kasim SE, Martino S, Kim P et al. Dietary and anthropometric determinants of plasma lipoproteins during a long-term low-fat diet in healthy women Am J Clin Nutr 1993 57: 146–153.
Shepard L, Kristal AR, Kushi LH . Weight loss in women participating in a randomized trial of low fat diets Am J Clin Nutr 1991 54: 821–828.
Powell JJ, Tucker T, Fisher AG, Wilcox K . The effects of different percentages of dietary fat intake, exercise, and calorie restriction on body composition and body weight in obese females Am J Health Prom 1994 8: 443–448.
Shah M, McGovern P, French S, Baxter J . Comparison of a low-fat, ad libitum complex-carbohydrate diet with a low-energy diet in moderately obese women Am J Clin Nutr 1994 59: 980–984.
Toubro S, Astrup A . Randomized comparison of diets for maintaining obese subjects weight after major weight loss ad lib, low fat, high carbohydrate diet vs fixed energy intake Br Med J 1997 314: 29–34.
Sjostrom L, Rissanen A, Andersen T et al. Randomized placebo-controlled trial of orlistat for weight loss and prevention of weight regain in obese patients Lancet 1998 352: 167–172.
Jebb SA, Prentice AM, Goldberg GR, Murgatroyd PR, Black AE, Coward WA . Changes in macronutrient balance during over- and underfeeding assessed by 12-d continuous whole body calorimetry Am J Clin Nutr 1996 64: 259–266.
Flatt JP . The difference in the storage capacities for carbohydrate and for fat, and its implications in the regulation of body weight Ann NY Acad Sci 1987 499: 104–123.
Prentice AM . Manipulation of dietary fat and energy density and subsequent effects on substrate flux and food intake Am J Clin Nutr 1998 67: (3 Suppl): 535S–541S.
Stubbs RJ, Prentice AM, James WP . Carbohydrates and energy balance Ann NY Acad Sci 1997 819: 44–69.
Rolls BJ, Kim-Harris S, Fischman MW, Foltin RW, Moran TH, Stoner SA . Satiety after preloads with different amounts of fat and carbohydrate: implications for obesity Am J Clin Nutr 1994 60: 476–487.
Friedman MI . Fuel partitioning and food intake Am J Clin Nutr 1998 67: 513S–518S.
Blundell JE, Macdiarmid JI . Passive overconsumption. Fat intake and short-term energy balance Ann NY Acad Sci 1997 827: 392–407.
Stubbs RJ, Ritz P, Coward WA, Prentice AM . Covert manipulation of the ratio of dietary fat to carbohydrate and energy density: effect on food intake and energy balance in free-living men eating ad libitum. Am J Clin Nutr 1995 62: 330–337.
Kendall A, Levitzky DA, Strupp BJ, Lissner L . Weight loss on a low-fat diet: consequences of the imprecision of the control of food intakes in humans Am J Clin Nutr 1991 53: 1124–1129.
Bell EA, Castellanos VH, Pelkman CL, Thorwart ML, Rolls BJ . Energy density of foods affects energy intake in normal-weight women Am J Clin Nutr 1998 67: 412–420.
Drewnowski A, Kurth C, Holden-Wiltse J, Saari J . Food preferences in human obesity: carbohydrates versus fats Appetite 1992 18: 207–221.
Trichopoulos A, Lagiou P, Trichopoulos D . Traditional Greek diet and coronary heart disease J Cardiovasc Risk 1994 1: 9–15.
Acknowledgements
Funding for this study was equally supported by the Peanut Institute, the International Olive Oil Council, and the International Tree Nut Council.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
McManus, K., Antinoro, L. & Sacks, F. A randomized controlled trial of a moderate-fat, low-energy diet compared with a low fat, low-energy diet for weight loss in overweight adults. Int J Obes 25, 1503–1511 (2001). https://doi.org/10.1038/sj.ijo.0801796
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.ijo.0801796
Keywords
This article is cited by
-
Switching diets after 6-months does not result in renewed weight loss: a secondary analysis of a 12-month crossover randomized trial
Scientific Reports (2024)
-
Mediterranean dietary pattern and the risk of type 2 diabetes: a systematic review and dose–response meta-analysis of prospective cohort studies
European Journal of Nutrition (2022)
-
Refined critical boundary with enhanced statistical power for non-directional two-sided tests in group sequential designs with multiple endpoints
Statistical Papers (2021)
-
Adherence to Mediterranean and low-fat diets among heart and lung transplant recipients: a randomized feasibility study
Nutrition Journal (2018)
-
Consumption of extra virgin olive oil improves body composition and blood pressure in women with excess body fat: a randomized, double-blinded, placebo-controlled clinical trial
European Journal of Nutrition (2018)