Abstract
Immunotherapy, particularly immune checkpoint inhibitors (ICIs), such as anti-programmed death 1/programmed death-ligand 1 (PD-1/PD-L1) therapy, has emerged as a pivotal treatment modality for solid tumors, including recurrent or metastatic nasopharyngeal carcinoma (R/M-NPC). Despite the advancements in the utilization of ICIs, there is still room for further improving patient outcomes. Another promising approach to immunotherapy for R/M-NPC involves adoptive cell therapy (ACT), which aims to stimulate systemic anti-tumor immunity. However, individual agent therapies targeting dendritic cells (DCs) appear to still be in the clinical trial phase. This current review underscores the potential of immunotherapy as a valuable adjunct to the treatment paradigm for R/M-NPC patients. Further research is warranted to enhance the efficacy of immunotherapy through the implementation of strategies such as combination therapies and overcoming immune suppression. Additionally, the development of a biomarker-based scoring system is essential for identifying suitable candidates for precision immunotherapy.
Similar content being viewed by others
Introduction
Nasopharyngeal carcinoma (NPC) is particularly prevalent in East and Southeast Asia1. Unlike other subtypes of head and neck squamous cell carcinomas (HNSCCs), NPC is distinguished by its non-surgical treatment modality, etiology, and prognosis. Notably, trials that have led to the approval of promising immunotherapies for HNSCCs, such as nivolumab and pembrolizumab, have specifically excluded NPC patients from their study cohorts2,3. Among HNSCCs, NPC stands out as one of the most prone to recurrence and distant metastasis4, contributing to the limited clinical benefits and unfavorable prognosis associated with this cancer type. Patients with recurrent or metastatic NPC (R/M-NPC) are typically recommended to receive platinum-based chemotherapy as the first-line treatment. However, gemcitabine plus cisplatin (GP) therapy, while commonly used in recent years, provides only modest short-term benefits, with a 12-month progression-free survival (PFS) rate of only 20% in R/M NPC patients5. Immunotherapy has emerged as a transformative approach to cancer treatment, revolutionizing strategies for various types of cancer. In this review, we will focus on clinically approved immunotherapy regimens for R/M-NPC therapy and discuss novel immunotherapy strategies, challenges, and future directions for Immunotherapy combination strategies in R/M-NPC.
Tumor immune microenvironment and targets for immunotherapy
NPC is closely associated with the Epstein-Barr virus (EBV) infection, characterized by significant lymphocytic infiltrations in tumor tissues and heightened programmed death-ligand 1 (PD-L1) expression6. With advancements in understanding the tumor immune microenvironment (TIME), there is a growing emphasis on investigating the systemic anti-tumor immune responses, wherein dendritic cells (DCs) and CD8 T cells play pivotal roles7. CD8 T cells are known to be crucial in facilitating anti-tumor immunity through the recognition of tumor-related antigens presented on major histocompatibility complexes class (MHC) I via their T cell receptor (TCR). Moreover, specialized antigen-presenting cells, particularly DCs, are essential for the activation and maintenance of CD8 T cells’ cytotoxic immune responses. The interaction between co-stimulatory molecules CD80/CD86 and CD28 provides a secondary signal for T cell activation. Additionally, natural killer cells produce either FMS-related tyrosine kinase 3 ligand or C-C motif chemokine ligand 5 and X-C motif chemokine ligand 1, which induces the recruitment of DCs into the TIME. Bidirectional communication has also been demonstrated as necessary, with the production of interleukin-12 (IL-12) by DCs leading to the production of interferon-γ (IFN-γ) by CD8 T cells and natural killer cells. In summary, these processes highlight the beneficial aspects of cross-presenting tumor antigens to naive CD8 T cells in lymph nodes to induce successful anti-tumor immune responses. Conversely, within the TIME, NPC tumor cells hinder the function of DCs by secreting negative regulatory factors, such as IL-10 and vascular endothelial growth factor. Simultaneously, the high expression of PD-L1 on the surface of NPC tumor cells, and its binding to the inhibitory protein PD-1 produced by CD8 T cells, enable evasion of the adaptive immune system through down-regulation of T-cell response7,8,9,10 (Fig. 1).
PMDC Peripheral blood mononuclear cell, DC Dendritic cell, NK cell nature killer cell, EBV-CTL EBV-specific cytotoxic T lymphocyte, EBNA1 EBV nuclear antigen 1, LMP1 and LMP2 Latent membrane proteins 1 and 2, GM-CSF Granulocyte-macrophage colony-stimulating factor, IL-4 Interleukin-4, Flt3L FMS-related tyrosine kinase 3 ligand, XCL1 X-C motif chemokine ligand 1, CCL5 C-C motif chemokine ligand 5, IL-12: Interleukin-12, IL-10 Interleukin-10, VEGF Vascular endothelial growth factor, IFN-γ interferon-γ, MHC Major histocompatibility complex, TCR T cell receptor. (By Figdraw.).
Immunotherapy strategies can be broadly categorized into two main groups. The first group aims to enhance the existing adaptive immune response by inhibiting inhibitory pathways on T cells within the tumor. A common example of this approach is the use of immune checkpoint inhibitors (ICIs) targeting PD-1. The second group encompasses active immunotherapy methods such as DC vaccines, adoptive cell transfer of tumor-specific T cells, and engineered T cells with tumor antigen-specific T cell receptors or chimeric antigen receptors9,10,11.
Immune checkpoint inhibitors for R/M-NPC
Several studies have suggested a close association between elevated PD-L1 on NPC tumor cells and poor prognosis among patients undergoing traditional radiotherapy and chemotherapy12,13. This suggests that anti-PD-1/PD-L1 therapy could be a promising treatment approach and a means to improve patients’ prognosis.
In recent years, the emergence of PD-1 antibodies has presented a promising avenue for immunotherapeutic intervention in the management of R/M-NPC. In an international, double-blind, randomized, placebo-controlled phase 3 trial (JUPITER-02)14, Mai et al. compared the efficacy and toxicity of GP chemotherapy combined with either toripalimab or placebo as a first-line treatment for patients with R/M NPC. A total of 289 eligible patients from mainland China, Taiwan, and Singapore were evenly distributed between the toripalimab combination arm (arm A, n = 146) and the placebo combination arm (arm B, n = 143). The median PFS was 11.7 months in the toripalimab arm and 8.0 months in the placebo arm. The results showed that treatment with toripalimab in combination with chemotherapy reduced the risk of progression or death by 59% compared to placebo combined with chemotherapy (hazard ratio [HR] = 0.41, P < 0.0001), while maintaining a manageable safety profile. Furthermore, their findings suggested that the clinical benefits of the toripalimab-GP combination could be observed irrespective of PD-L1 expression status. In 2021, Yang et al. conducted a multicenter, randomized, double-blind, phase 3 trial (CAPTAIN-1st)15 to compare the clinical efficacy of camrelizumab plus GP versus placebo plus GP as a first-line treatment for R/M-NPC. A total of 263 eligible patients were randomly assigned to receive either camrelizumab (n = 134) or placebo (n = 129) plus GP. The study revealed a significantly longer PFS in the camrelizumab group compared to the placebo group (median, 9.7 vs 6.9 months; one-sided P = 0.0002). Furthermore, the safety profiles of camrelizumab plus chemotherapy were found to be manageable.
However, there is currently no established standard for salvage therapy plans for patients who have experienced treatment failure with initial platinum-containing regimens. In recent years, several anti-PD-1 monoclonal antibodies have emerged as potential options for salvage treatment following initial standard interventions for locally advanced NPC, with individual response rates ranging from 20% to 30%16,17,18,19. Among these trials, the most impactful is a phase II clinical trial (POLARIS-02) conducted by the Sun Yat-sen University Cancer Center18. This trial demonstrated an overall response rate (ORR) of 20.5%, with a median disease control rate (DOR) of 12.8 months, median PFS of 1.9 months, and a median overall survival (OS) of 17.4 months among patients with R/M-NPC who received toripalimab monotherapy as second-line and beyond therapy. In this systematic review, we conducted a meta-analysis to evaluate the association between second-line and subsequent treatments using anti-PD-1 antibodies and the primary endpoints in R/M-NPC, which include ORR, DCR, PFS, and OS. Table 1 presents a summary of the characteristics of the included 12 studies (including one randomized controlled trial and 11 retrospective cohort studies). The pooled analysis utilizing the random-effects model yielded an ORR of 23% (95% CI: 18-28%, I2 = 52%) and a DCR of 60% (95% CI: 49-71%, I2 = 95%) when anti-PD1 drugs were administered as second-line and subsequent treatments in R/M-NPC patients (Supplementary Figure 2). Detailed methods and results of the meta-analysis are provided in the Supplementary Material.
PD-1 monoclonal antibody is consistently administered following traditional chemotherapy as first-line treatment in the clinical setting. However, in second-line treatment or beyond, the therapeutic response to PD-1 monotherapy has been explored in 11 studies, with only one examining the clinical efficacy of PD-1 monoclonal antibody plus gemcitabine. This Phase II study of nibuzumab plus gemcitabine was conducted across seven centers of the Korean Clinical Research Group20. All participating patients with R/M-NPC received nibulizumab and gemcitabine intravenously every two weeks, with cycles repeated every 28 days for up to one year. Compared to previous studies on anti-PD-1/PD-L1 monotherapy, the combination of nibulizumab and gemcitabine demonstrated improved PFS and OS (Table 1). The notable clinical efficacy observed may be attributed to the synergistic interaction between nibulizumab and gemcitabine. It is suggested that gemcitabine-induced apoptosis of tumor cells could enhance DCs-mediated presentation of tumor antigens to T cells, thereby augmenting the response and survival outcomes of nibulizumab in R/M-NPC21. Conversely, in the Phase I randomized Study of Spartalizumab versus Chemotherapy in patients with R/M-NPC, no improvement in median PFS was observed in the crossover group of patients who switched to Spartalizumab following treatment progression on chemotherapy22. In conclusion, whether the survival benefits for patients with R/M-NPC can be enhanced by a combination of chemotherapy and immunotherapy or by immunotherapy postchemotherapy progression remains uncertain and requires further investigation.
Histological subtypes, EBV status, and PD-L1 expression were not utilized for patient selection in any of the clinical trials. The efficacy of anti-PD-1 monoclonal antibody in R/M-NPC may vary depending on the PD-L1 expression status, which raises an important question for investigation as PD-L1 expression could potentially serve as a biomarker for treatment guidance. A systematic review and meta-analysis23 comprising 12 prospective trials (n = 1088) examined the significance of PD-L1 expression in predicting response to anti-PD-1/PD-L1 therapy in HNSCCs. The study concluded that using a 1% threshold, ORR was greater for PD-L1 expressers vs non-expressers (18.9% vs 8.8%), but not at 12 or 18 months. In addition, significant benefits were not observed in ORR for PD-L1 expressers defined at different thresholds. Therefore, while PD-L1 expression serves as a crucial consideration for immunosuppressive treatment approaches, its prognostic significance remains controversial for R/M-NPC. In the JUPITER-02 trial, patients with PD-L1-positive and -negative tumors exhibited similar median PFS (11.4 vs. 11.0 months) when treated with the toripalimab-GP combination. In the POLARIS-02 trial, PD-L1-positive patients (PD-L1 > 1%) showed a numerically higher ORR (27.1% vs 19.4%) compared to PD-L1-negative patients, and with even higher ORR (38.1% vs. 19.3%) observed in individuals with high PD-L1 expression (PD-L1 > 25%). Additionally, patients with high PD-L1 expression had improved median PFS (7.2 vs. 1.9 months). Current evidence suggests that anti-PD-1/PD-L1 therapy may provide modest benefits regardless of PD-L1 expression status. The prognostic value of PD-L1 expression level as a biomarker in predicting the immunotherapy response in R/M-NPC appears to be controversial, warranting further exploration.
In conclusion, the progress in PD-1 monoclonal antibody development has provided further clinical benefits for R/M-NPC. However, due to the significant heterogeneity within the TIME, PD-1 blockade therapy may only benefit a limited proportion of R/M-NPC patients, and there is a lack of effective biomarkers to screen the most suitable candidates. This highlights the need for novel immunotherapeutic strategies to improve patient survival24.
Adoptive immune cell therapy for R/M-NPC
NPC cells express a limited repertoire of EBV proteins, predominantly EBV nuclear antigen 1 (EBNA1), with a subset of tumors also expressing latent membrane proteins 1 and 2 (LMP1 and LMP2)25,26,27. As EBV transitions into latency phase 2, most EBV proteins become transcriptionally silenced, an astute evasion tactic that impedes immune recognition. Consequently, these EBV proteins present as attractive targets for immunotherapy, as they can serve as specific antigens to stimulate the host immune system. Importantly, NPC cells possess the ability for immunologic processing, allowing recognition by cytotoxic T lymphocytes (CTLs)28,29. Taking inspiration from the successful use of adoptive EBV-targeted CTL (EBV-CTL) therapy in treating EBV-associated post-transplant lymphoproliferative disease30, anti-EBV immunotherapy strategies have gained attention as potential adjuvant treatments with the potential to improve R/M-NPC prognosis25,31,32. Table 2 presents the key characteristics and findings from 12 studies investigating the use of adoptive immune cell therapy to target systemic antitumor immunity in R/M-NPC.
EBV-specific cytotoxic T lymphocyte therapy
EBV-CTL therapy has emerged as a promising avenue in the pursuit of more effective treatment for R/M-NPC. The safety and efficacy of this approach have been investigated in several clinical investigations, offering valuable insights into its potential benefits.
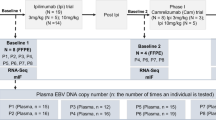
Smith et al.33 pioneered the use of AdE1-LMPpoly, a vector based on polyepitopes, in a phase I clinical trial. This adenovirus-based vector encodes several CTL epitopes derived from LMP1 and LMP2 fused to a truncated EBNA1, in the absence of an intrinsic glycine-alanine repeat sequence34,35. Expanded EBV-specific T lymphocytes were observed in 16 (72.7%) of the 24 NPC patients. Grade I and/or II toxicities were the only adverse effects identified with the administration of AdE1-LMPpoly-expanded T cells by infusion, suggesting its safety. Among the 14 patients who received T-cell treatment, 10 maintained stable disease and showed an extended PFS (median, 66.5 days). Further analysis of a larger NPC patient cohort36, including both pre-emptive and therapeutic treatments, emphasized that the stabilization of the disease in patients with active recurrent/metastatic disease was significantly associated with the functional and phenotypic composition of T cell immunotherapy expanded in vitro.
Huang et al.37 conducted a phase 1/2 trial involving the administration of EBV-CTLs to 21 patients with R/M-NPC. Only one patient with metastatic disease achieved a complete response, resulting in an ORR of only 4.8%. A low incidence of severe adverse events was observed. However, two patients showed renewed responses to gemcitabine following EBV-CTL immunotherapy. These findings, together with previous study results, suggest that EBV-CTL immunotherapy could potentially serve as a primer for or be combined with chemotherapy34,38. To enhance the efficacy of EBV-specific T cells, future efforts can involve exploring combination treatments with other immune modulators, such as checkpoint inhibitors or drugs that target regulatory T cells37. Furthermore, upcoming studies can investigate the possibility of renewed responses to chemotherapy in patients who have previously showed no response to either chemotherapy or immunotherapy.
Combination of chemotherapy with adoptive cell therapy
As previously noted, the clinical efficacy of EBV-CTL-based adoptive immunotherapy varies. However, when combined with the gemcitabine, carboplatin, and paclitaxel chemotherapy regimen, its therapeutic response and OS rates rank among the highest for palliative regimens33,38. Chia et al. conducted a phase 2 trial that paved the way for the investigation of its potential use in combination with chemotherapy as a first-line treatment39. In this study, 35 patients received CTLs following chemotherapy. The findings were encouraging, with two patients (5.7%) achieving complete response, 13 (31.7%) experiencing partial response, and seven (20%) maintaining stable disease as the best response to CTL therapy. This combined approach resulted in an impressive clinical benefit rate of 62.9% and a response rate of 42.9%. Notably, among these patients receiving both chemotherapy and CTLs (GP-CTL), the median PFS and OS were 7.6 months (95% CI: 7.4–8.4) and 29.9 months (95% CI: 20.8–39.3), respectively, surpassing the median PFS observed during the CTL immunotherapy phase alone (3.7 months; 95% CI: 2.4–4.0).
Transfusing autologous cytokine-induced killer cells (CIKs) represents another form of adaptive cell transfer. CIKs are co-induced with various cytokines, including anti-CD3 monoclonal antibody, IL-2, and IFN-γ. These cells exhibit robust antitumor effects because they co-express the markers for T cells (CD3) and natural killer cells (CD56)40,41. Both in vitro and in vivo studies have shown that their tumor-killing activity, which is restricted by non-major histocompatibility complex (MHC), to be effective against a wide range of tumor types. Li et al.42 utilized a retrospective cohort of 222 patients to evaluate the efficacy of GP followed by CIK. Their analysis of long-term efficacy revealed significantly higher rates of PFS and OS in the GP + CIK group. However, Fumet et al.43 showed that chemotherapy drugs have a dual effect, that is, they directly eliminate tumor cells and enhance their susceptibility to immune responses. While chemotherapy offers numerous benefits, it can also impair functional immune cells, thereby compromising immunity. Conversely, CIK immunotherapy, involving the artificial transfusion of functional immune cells, can achieve a combined effect that maximizes the benefits of both chemotherapy and immunotherapy. These findings bolster the concept that CIK and GP synergize to enhance antitumor efficacy.
Dendritic cells-targeting vaccine
DCs play a pivotal role in activating anti-tumor T cells and other functions that bridge innate and adaptive immunity44,45,46,47,48. Their primary function involves capturing, processing, and presenting exogenous antigens to T lymphocytes, characterized by the constitutive expression of MHC-I and costimulatory molecules. One of the most important steps in developing CD8 T cell immunity against tumors is cross-priming, in which DCs activate CD8 T cells by cross-presenting exogenous antigens7. Moreover, unlike other antigen-presenting cells, DCs may deliver tumor antigens to draining lymph nodes, where they can trigger the activation of T cells44,45,46,47,48. Tumor-resident DCs are emerging as key regulators of the T-cell response within tumors during therapy44,49,50,51, establishing DCs as the hub of the anti-tumor T-cell response and prompting the development of DC-based vaccines.
Currently, only a limited number of DC-based immunotherapies have been developed to target EBV antigens associated with NPCs. Given the scarce treatment options available for R/M-NPC, investigating DC vaccines to harness the antitumor immune capabilities of DCs holds promise in both immunological and clinical efficacy. Various approaches have been investigated in the development of DC vaccines. The most common method involves the ex vivo expansion of DCs derived from monocytes (Fig. 1). Initially, peripheral blood monocytes are isolated from the apheresis product. These cells are then cultured with IL-4 and granulocyte-macrophage colony-stimulating factor to induce their differentiation into DCs. Following this, a maturation cocktail is applied to stimulate the DCs, which are subsequently pulsed with relevant tumor-associated antigens or tumor lysates, enabling them to elicit tumor-specific immune responses52.
In 2021, Nickles et al.53 conducted a groundbreaking clinical trial utilizing EBV antigens pulsed into CD137 ligand (CD137L)-DC for R/M-NPC. Antigen-presenting cells express CD137L, which is crucial for costimulating CD137-expressing T cells. This innovative approach involves reverse CD137L signaling, inducing the differentiation of monocytes into CD137L-DC, a novel subtype of dendritic cells derived from monocytes. Notably, CD137L-DCs exhibit an increased capacity for T-cell stimulation. Approximately 33.3% (4/12) of the patients reported adverse effects of grade 1, indicating that the intervention was well-tolerated. Encouragingly, clinical benefit was observed in 42% of cases, including one patient achieving partial remission and four patients experiencing stable disease for 2 to 3 years. The median PFS was 16.5 weeks (ranging from 3 to 136 weeks). These study findings are particularly promising as they demonstrate a correlation between clinical benefit and T cell responses, particularly memory and effector T cells.
Discussion
R/M-NPC is a highly heterogeneous spectrum of disorders with various subtypes, such as de novo metastasis, locoregional recurrence, and locoregional recurrence with distant metastasis54. In recent years, immunotherapy has demonstrated manageable safety profiles and substantial benefits for different types of NPC.
Studies have shown that additional locoregional radiation therapy for patients with de novo metastatic NPC can significantly increase OS from 13.0-24.5 to 21.0-60.0 months55,56,57,58,59,60. Locoregionally recurrent NPC presents a different challenge, whereby patients have the option to undergo re-radiotherapy or salvage surgical intervention. Salvage intensity-modulated radiotherapy is the most commonly preferred treatment modality for this group. Some studies have demonstrated that combining radiotherapy with PD-1 monoclonal antibodies can achieve higher efficacy for R/M-NPC, suggesting that radiotherapy may augment the response rates to ICIs by creating a more favorable TIME61,62.
For R/M-NPC, palliative systemic chemotherapy remains the mainstream treatment option, typically involving platinum-containing regimens. Notably, results from the pivotal CAPTAIN-1st trial have garnered the approval of the National Medical Products Administration for the employment of the camrelizumab plus GP combination as a first-line therapeutic option for patients with R/M-NPC63. Afterward, following the results of the POLARIS-02 trial, toripalimab was granted approval for the management of patients with R/M-NPC who exhibited inadequate response to second-line or subsequent-line systemic therapy63. This implies that the addition of anti-PD1 antibodies into the standard palliative treatment regimen for R/M-NPC patients could potentially improve their OS.
Adoptive immune cell therapy, mainly targeting DCs, is well-tolerated in patients with NPC and has shown promising immune responses and clinical benefits. As previously mentioned, the traditional method for preparing DC vaccines involves culturing peripheral blood mononuclear cells with IL-4 and granulocyte-macrophage colony-stimulating factor. This process induces their differentiation into DCs, followed by stimulation of their maturation and pulsing with relevant tumor-associated antigens or tumor lysates. The administration route for DC vaccines varies; however, intranodal injection of DCs has demonstrated the ability to induce a more potent T cell anti-tumor immunity compared to intravenous or subcutaneous injection64. However, there are some uncertainties in the detection of vaccine-induced anti-tumor responses65. First, it has been noted that the amplification of adoptive CTL in peripheral blood is not as significant as observed in vitro. Second, no significant correlation has been established between CTL amplification and clinical efficacy.
Recently, Wen et al.66 introduced an innovative approach to tumor treatment whereby they used a nanoVaccine to induce the formation of intratumor tertiary lymphoid structures. This nanoVaccine contains the antigen EBNA1Δ93‑236, cytosine-phosphate-guanine, and Mn2+ formulated through physical interaction. T cells, DCs, and B cells are activated via the TLR-9 and STING signaling pathways by Mn2+ and cytosine-phosphate-guanine in a synergistic manner. In comparison to conventional NPC vaccinations, which primarily target T cell activation, this innovative nanoVaccine stimulates the development of tertiary lymphoid structures. NanoVaccine administered via subcutaneous injection can target and deliver antigens and adjuvants to the lymph nodes, activating robust innate and adaptive immunity. More importantly, this approach facilitates the infiltration of anti-tumor immunocytes into tumor sites, creating a favorable environment for interaction with the tumor microenvironment. By using this approach, it is possible to overcome the constraints associated with current therapeutic vaccinations and increase the population that may benefit from immunotherapy.
Challenges and prospects
According to our pooled analysis in supplementary materials, the ORR for anti-PD1 inhibitor monotherapy was 23% when it was used as a second-line and beyond treatment. The clinical benefits obtained from the application of immune checkpoint blockades are not as ideal compared to other solid tumors. Numerous theories have been advanced about the mechanisms that underlie ICI resistance. One theory suggests that inadequate anti-tumor responses, resulting from immune evasion, may hinder the effectiveness of immunotherapies. Resistance to ICIs could be attributed to insufficient neoantigens and evasion of specific tumor molecules targeted by ICIs67. Additionally, reduced expression of MHC-I/MHC-II molecules may impede antigen presentation and contribute to ICIs resistance68. Another theory posits that immunotherapies can be rendered unsuccessful due to inadequate antitumor effector T cell activity. Impairment of the therapeutic response could result from the suppression of critical immunological signaling pathways due to the absence of downstream immune signals, including IFN-γ and IL-1250. However, IL-10 released by macrophages or other immunosuppressive cells, as well as tumor-derived factors like Vascular endothelial growth factor, can inhibit the maturation of conventional dendritic cells and directly inhibit their production of IL-128.
Similarly, the limited efficacy of DC-targeting vaccines may be attributed to systemic immunosuppression factors, such as the increased frequency of inhibitory regulatory T cells and the presence of immunosuppressive cytokines like IL-10 or transforming Vascular endothelial growth factor-β in the peripheral blood. Additionally, the local TIME can induce immunosuppression, posing a significant challenge to cancer immunotherapy69,70,71. Indeed, the TIME-mediated regulation and suppression of tumor-infiltrating DCs might hinder their ability to initiate potent antitumor immunity and even promote tumor progression, as suggested by accumulating data. Overcoming tumor-induced immunosuppression represents a major hurdle in cancer immunotherapy. Consequently, extensive research is underway to elucidate the mechanisms by which DCs modulate anti-tumor CD8 T cell responses.
Building upon the existing achievements and addressing the unmet needs, future works and development of immunotherapy strategies for improving anti-tumor immune activity could focus on the following directions: 1) Understanding molecular mechanisms: Investigating the molecular mechanisms underlying the interactions between various immune cells and nasopharyngeal carcinoma cells to identify more targetable EBV antigens and enhance their immunogenicity; 2) Promoting immune migration: Exploring strategies to enhance the migration of peripheral immune effector cells to lymphatic organs or tumor sites and regulating the TIME; and 3) Combination therapies: Investigating the potential benefits of combining standard-of-care therapies with novel immunotherapies, which holds promise for improving treatment efficacy.
Identifying the ideal biomarker to effectively stratify R/M-NPC patients who could benefit from immunotherapy remains a significant challenge. However, there is consensus that metrics such as the the degree of early increase in EBV DNA titer and baseline plasma EBV DNA levels hold promise in forecasting long-term outcomes for R/M-NPC patients undergoing immunotherapy72. Other commonly used predictive biomarkers in immunotherapy include the expression of PD-L1, tumor mutation burden, and MHC-I/MHC-II gene expression73. These biomarkers have also been highlighted in the prognostic assessment of adoptive immune cell therapy.
However, due to the complexity of the TIME and the immune system, it is unlikely that a single biomarker alone can reliably predict prognosis and response to immunotherapy74. Instead, there is growing interest in exploring artificial intelligence (AI)-based approaches to integrate multi-omics data, such as genomics, pathomics, radiomics, and TIME heterogeneity, to define novel meta-biomarkers. AI techniques have been applied to various cancers, primarily non-small cell lung cancer, to discover predictive biomarkers for the efficacy of ICIs75. The application of AI in NPC studies could help identify more suitable patient populations for immunotherapy.
Conclusion
Immunotherapy, particularly ICIs, has proven its therapeutic efficacy in the treatment of R/M-NPC. Furthermore, adoptive immune cell therapy has exhibited promising therapeutic potential and merits continued investigation in clinical settings. Delving into the mechanisms governing the interaction between systemic immunity, local tumor immunity, and the TIME is anticipated to enhance anti-tumor activity and uncover additional targets for immunotherapy. Furthermore, the utilization of AI to analyze predictive biomarkers and identify appropriate patient cohorts for immunotherapy holds promise as a future advancement.
Data availability
As this is a review, there are no original datasets. However, all referenced data sources are cited within the manuscript.
Code availability
As this is a review, there are no codes generated.
References
Chen, Y. P. et al. Nasopharyngeal carcinoma. Lancet 394, 64–80 (2019).
Ferris, R. L. et al. Nivolumab for Recurrent Squamous-Cell Carcinoma of the Head and Neck. N. Engl. J. Med 375, 1856–1867 (2016).
Chow, L. Q. M. et al. Antitumor Activity of Pembrolizumab in Biomarker-Unselected Patients With Recurrent and/or Metastatic Head and Neck Squamous Cell Carcinoma: Results From the Phase Ib KEYNOTE-012 Expansion Cohort. J. Clin. Oncol. 34, 3838–3845 (2016).
Caudell, J. J. et al. NCCN Guidelines® Insights: Head and Neck Cancers, Version 1.2022. J. Natl Compr. Canc Netw. 20, 224–234 (2022).
Zhang, L. et al. Gemcitabine plus cisplatin versus fluorouracil plus cisplatin in recurrent or metastatic nasopharyngeal carcinoma: a multicentre, randomised, open-label, phase 3 trial. Lancet 388, 1883–1892 (2016).
Huang, Z. L. et al. The prognostic significance of PD-L1 and PD-1 expression in patients with nasopharyngeal carcinoma: a systematic review and meta-analysis. Cancer Cell Int 19, 141 (2019).
Fu, C. & Jiang, A. Dendritic Cells and CD8 T Cell Immunity in Tumor Microenvironment. Front. Immunol. 9, 3059 (2018).
Gardner, A., de Mingo Pulido, Á. & Ruffell, B. Dendritic Cells and Their Role in Immunotherapy. Front. Immunol. 11, 924 (2020).
Masterson, L. et al. Immune checkpoint inhibitors in advanced nasopharyngeal carcinoma: Beyond an era of chemoradiation? Int. J. Cancer 146, 2305–2314 (2020).
Yi, M. et al. Combination strategies with PD-1/PD-L1 blockade: current advances and future directions. Mol. Cancer 21, 28 (2022).
Durgeau, A., Virk, Y., Corgnac, S. & Mami-Chouaib, F. Recent Advances in Targeting CD8 T-Cell Immunity for More Effective Cancer Immunotherapy. Front Immunol. 9, 14 (2018).
Zhang, J. et al. Co-expression of PD-1 and PD-L1 predicts poor outcome in nasopharyngeal carcinoma. Med. Oncol. 32, 86 (2015).
Fang, W. et al. EBV-driven LMP1 and IFN-γ up-regulate PD-L1 in nasopharyngeal carcinoma: Implications for oncotargeted therapy. Oncotarget 5, 12189–12202 (2014).
Mai, H. Q. et al. Toripalimab or placebo plus chemotherapy as first-line treatment in advanced nasopharyngeal carcinoma: a multicenter randomized phase 3 trial. Nat. Med 27, 1536–1543 (2021).
Yang, Y. et al. Camrelizumab versus placebo in combination with gemcitabine and cisplatin as first-line treatment for recurrent or metastatic nasopharyngeal carcinoma (CAPTAIN-1st): a multicentre, randomised, double-blind, phase 3 trial. Lancet Oncol. 22, 1162–1174 (2021).
Poon, D., Chowbay, B., Cheung, Y. B., Leong, S. S. & Tan, E. H. Phase II study of irinotecan (CPT-11) as salvage therapy for advanced nasopharyngeal carcinoma. Cancer 103, 576–581 (2005).
Fang, W. et al. Camrelizumab (SHR-1210) alone or in combination with gemcitabine plus cisplatin for nasopharyngeal carcinoma: results from two single-arm, phase 1 trials. Lancet Oncol. 19, 1338–1350 (2018).
Wang, F. H. et al. Efficacy, Safety, and Correlative Biomarkers of Toripalimab in Previously Treated Recurrent or Metastatic Nasopharyngeal Carcinoma: A Phase II Clinical Trial (POLARIS-02). J. Clin. Oncol. 39, 704–712 (2021).
Hsu, C. et al. Safety and Antitumor Activity of Pembrolizumab in Patients With Programmed Death-Ligand 1-Positive Nasopharyngeal Carcinoma: Results of the KEYNOTE-028 Study. J. Clin. Oncol. 35, 4050–4056 (2017).
Jung, H. A. et al. A Phase II Study of Nivolumab plus Gemcitabine in Patients with Recurrent or Metastatic Nasopharyngeal Carcinoma (KCSG HN17-11). Clin. Cancer Res 28, 4240–4247 (2022).
Suzuki, E., Kapoor, V., Jassar, A. S., Kaiser, L. R. & Albelda, S. M. Gemcitabine selectively eliminates splenic Gr-1+/CD11b+ myeloid suppressor cells in tumor-bearing animals and enhances antitumor immune activity. Clin. Cancer Res 11, 6713–6721 (2005).
Even, C. et al. Phase II, Randomized Study of Spartalizumab (PDR001), an Anti-PD-1 Antibody, versus Chemotherapy in Patients with Recurrent/Metastatic Nasopharyngeal Cancer. Clin. Cancer Res 27, 6413–6423 (2021).
Patel, J. J., Levy, D. A., Nguyen, S. A., Knochelmann, H. M. & Day, T. A. Impact of PD-L1 expression and human papillomavirus status in anti-PD1/PDL1 immunotherapy for head and neck squamous cell carcinoma-Systematic review and meta-analysis. Head. Neck 42, 774–786 (2020).
Chow, J. C., Ngan, R. K., Cheung, K. M. & Cho, W. C. Immunotherapeutic approaches in nasopharyngeal carcinoma. Expert Opin. Biol. Ther. 19, 1165–1172 (2019).
Khanna, R., Moss, D. J. & Burrows, S. R. Vaccine strategies against Epstein-Barr virus-associated diseases: lessons from studies on cytotoxic T-cell-mediated immune regulation. Immunol. Rev. 170, 49–64 (1999).
Chang, K. L., Chen, Y. Y., Shibata, D. & Weiss, L. M. Description of an in situ hybridization methodology for detection of Epstein-Barr virus RNA in paraffin-embedded tissues, with a survey of normal and neoplastic tissues. Diagn. Mol. Pathol. 1, 246–255 (1992).
Khanna, R. et al. Molecular characterization of antigen-processing function in nasopharyngeal carcinoma (NPC): evidence for efficient presentation of Epstein-Barr virus cytotoxic T-cell epitopes by NPC cells. Cancer Res 58, 310–314 (1998).
Lee, S. P. et al. CTL control of EBV in nasopharyngeal carcinoma (NPC): EBV-specific CTL responses in the blood and tumors of NPC patients and the antigen-processing function of the tumor cells. J. Immunol. 165, 573–582 (2000).
Straathof, K. C., Savoldo, B., Heslop, H. E. & Rooney, C. M. Immunotherapy for post-transplant lymphoproliferative disease. Br. J. Haematol. 118, 728–740 (2002).
Chua, D. et al. Adoptive transfer of autologous Epstein-Barr virus-specific cytotoxic T cells for nasopharyngeal carcinoma. Int J. Cancer 94, 73–80 (2001).
Lin, C. L. et al. Immunization with Epstein-Barr Virus (EBV) peptide-pulsed dendritic cells induces functional CD8+ T-cell immunity and may lead to tumor regression in patients with EBV-positive nasopharyngeal carcinoma. Cancer Res 62, 6952–6958 (2002).
Comoli, P. et al. Adoptive transfer of allogeneic Epstein-Barr virus (EBV)-specific cytotoxic T cells with in vitro antitumor activity boosts LMP2-specific immune response in a patient with EBV-related nasopharyngeal carcinoma. Ann. Oncol. 15, 113–117 (2004).
Smith, C. et al. Effective treatment of metastatic forms of Epstein-Barr virus-associated nasopharyngeal carcinoma with a novel adenovirus-based adoptive immunotherapy. Cancer Res 72, 1116–1125 (2012).
Duraiswamy, J. et al. Induction of therapeutic T-cell responses to subdominant tumor-associated viral oncogene after immunization with replication-incompetent polyepitope adenovirus vaccine. Cancer Res 64, 1483–1489 (2004).
Smith, C. et al. Functional reversion of antigen-specific CD8+ T cells from patients with Hodgkin lymphoma following in vitro stimulation with recombinant polyepitope. J. Immunol. 177, 4897–4906 (2006).
Smith, C. et al. Pre-emptive and therapeutic adoptive immunotherapy for nasopharyngeal carcinoma: Phenotype and effector function of T cells impact on clinical response. Oncoimmunology 6, e1273311 (2017).
Huang, J. et al. Epstein-Barr virus-specific adoptive immunotherapy for recurrent, metastatic nasopharyngeal carcinoma. Cancer 123, 2642–2650 (2017).
Tan, E. H. et al. Phase II trial of a paclitaxel and carboplatin combination in Asian patients with metastatic nasopharyngeal carcinoma. Ann. Oncol. 10, 235–237 (1999).
Chia, W. K. et al. Adoptive T-cell transfer and chemotherapy in the first-line treatment of metastatic and/or locally recurrent nasopharyngeal carcinoma. Mol. Ther. 22, 132–139 (2014).
Zhang, L. et al. Phase II clinical study of gemcitabine in the treatment of patients with advanced nasopharyngeal carcinoma after the failure of platinum-based chemotherapy. Cancer Chemother. Pharm. 61, 33–38 (2008).
Bleakley, M. & Riddell, S. R. Molecules and mechanisms of the graft-versus-leukaemia effect. Nat. Rev. Cancer 4, 371–380 (2004).
Li, Y. et al. Sequential Cytokine-Induced Killer Cell Immunotherapy Enhances the Efficacy of the Gemcitabine Plus Cisplatin Chemotherapy Regimen for Metastatic Nasopharyngeal Carcinoma. PLoS One 10, e0130620 (2015).
Fumet, J. D., Limagne, E., Thibaudin, M. & Ghiringhelli, F. Immunogenic Cell Death and Elimination of Immunosuppressive Cells: A Double-Edged Sword of Chemotherapy. Cancers (Basel) 12, https://doi.org/10.3390/cancers12092637 (2020).
Broz, M. L. et al. Dissecting the tumor myeloid compartment reveals rare activating antigen-presenting cells critical for T cell immunity. Cancer Cell 26, 638–652 (2014).
Sánchez-Paulete, A. R. et al. Cancer Immunotherapy with Immunomodulatory Anti-CD137 and Anti-PD-1 Monoclonal Antibodies Requires BATF3-Dependent Dendritic Cells. Cancer Discov. 6, 71–79 (2016).
Hildner, K. et al. Batf3 deficiency reveals a critical role for CD8alpha+ dendritic cells in cytotoxic T cell immunity. Science 322, 1097–1100 (2008).
Roberts, E. W. et al. Critical Role for CD103(+)/CD141(+) Dendritic Cells Bearing CCR7 for Tumor Antigen Trafficking and Priming of T Cell Immunity in Melanoma. Cancer Cell 30, 324–336 (2016).
Salmon, H. et al. Expansion and Activation of CD103(+) Dendritic Cell Progenitors at the Tumor Site Enhances Tumor Responses to Therapeutic PD-L1 and BRAF Inhibition. Immunity 44, 924–938 (2016).
de Mingo Pulido, Á. et al. TIM-3 Regulates CD103(+) Dendritic Cell Function and Response to Chemotherapy in Breast Cancer. Cancer Cell 33, 60–74.e66 (2018).
Garris, C. S. et al. Successful Anti-PD-1 Cancer Immunotherapy Requires T Cell-Dendritic Cell Crosstalk Involving the Cytokines IFN-γ and IL-12. Immunity 49, 1148–1161.e1147 (2018).
Spranger, S., Dai, D., Horton, B. & Gajewski, T. F. Tumor-Residing Batf3 Dendritic Cells Are Required for Effector T Cell Trafficking and Adoptive T Cell Therapy. Cancer Cell 31, 711–723.e714 (2017).
Chow, M. T. et al. Intratumoral Activity of the CXCR3 Chemokine System Is Required for the Efficacy of Anti-PD-1 Therapy. Immunity 50, 1498–1512.e1495 (2019).
Nickles, E. et al. Dendritic cell therapy with CD137L-DC-EBV-VAX in locally recurrent or metastatic nasopharyngeal carcinoma is safe and confers clinical benefit. Cancer Immunol. Immunother. 71, 1531–1543 (2022).
Prawira, A. et al. Systemic therapies for recurrent or metastatic nasopharyngeal carcinoma: a systematic review. Br. J. Cancer 117, 1743–1752 (2017).
Rusthoven, C. G. et al. Metastatic nasopharyngeal carcinoma: Patterns of care and survival for patients receiving chemotherapy with and without local radiotherapy. Radiother. Oncol. 124, 139–146 (2017).
Verma, V., Allen, P. K., Simone, C. B. II, Gay, H. A. & Lin, S. H. Addition of Definitive Radiotherapy to Chemotherapy in Patients With Newly Diagnosed Metastatic Nasopharyngeal Cancer. J. Natl Compr. Canc Netw. 15, 1383–1391 (2017).
Liao, W. et al. Synchronous Metastatic Nasopharyngeal Carcinoma: Characteristics and Survival of Patients Adding Definitive Nasopharyngeal-Neck Radiotherapy to Systematic Chemotherapy. Cancer Manag Res 12, 10211–10219 (2020).
Sun, X. S. et al. Optimizing the Treatment Pattern for De Novo Metastatic Nasopharyngeal Carcinoma Patients: A Large-Scale Retrospective Cohort Study. Front Oncol. 10, 543646 (2020).
You, R. et al. Efficacy and Safety of Locoregional Radiotherapy With Chemotherapy vs Chemotherapy Alone in De Novo Metastatic Nasopharyngeal Carcinoma: A Multicenter Phase 3 Randomized Clinical Trial. JAMA Oncol. 6, 1345–1352 (2020).
Li, W. Z. et al. Development of a Prognostic Model to Identify the Suitable Definitive Radiation Therapy Candidates in de Novo Metastatic Nasopharyngeal Carcinoma: A Real-World Study. Int J. Radiat. Oncol. Biol. Phys. 109, 120–130 (2021).
Lin, J. et al. Stereotactic body radiotherapy extends the clinical benefit of PD-1 inhibitors in refractory recurrent/metastatic nasopharyngeal carcinoma. Radiat. Oncol. 17, 117 (2022).
Hua, Y. et al. Toripalimab plus intensity-modulated radiotherapy for recurrent nasopharyngeal carcinoma: an open-label single-arm, phase II trial. J. Immunother. Cancer 9, https://doi.org/10.1136/jitc-2021-003290 (2021).
Tang, L. L. et al. The Chinese Society of Clinical Oncology (CSCO) clinical guidelines for the diagnosis and treatment of nasopharyngeal carcinoma. Cancer Commun. (Lond.) 41, 1195–1227 (2021).
Lambert, L. A. et al. Intranodal immunization with tumor lysate-pulsed dendritic cells enhances protective antitumor immunity. Cancer Res 61, 641–646 (2001).
Louis, C. U. et al. Adoptive transfer of EBV-specific T cells results in sustained clinical responses in patients with locoregional nasopharyngeal carcinoma. J. Immunother. 33, 983–990 (2010).
Wen, Z. et al. Nanovaccines Fostering Tertiary Lymphoid Structure to Attack Mimicry Nasopharyngeal Carcinoma. ACS Nano 17, 7194–7206 (2023).
Gubin, M. M. et al. Checkpoint blockade cancer immunotherapy targets tumour-specific mutant antigens. Nature 515, 577–581 (2014).
Zaretsky, J. M. et al. Mutations Associated with Acquired Resistance to PD-1 Blockade in Melanoma. N. Engl. J. Med 375, 819–829 (2016).
Zong, J., Keskinov, A. A., Shurin, G. V. & Shurin, M. R. Tumor-derived factors modulating dendritic cell function. Cancer Immunol. Immunother. 65, 821–833 (2016).
Tang, M., Diao, J. & Cattral, M. S. Molecular mechanisms involved in dendritic cell dysfunction in cancer. Cell Mol. Life Sci. 74, 761–776 (2017).
Janikashvili, N., Bonnotte, B., Katsanis, E. & Larmonier, N. The dendritic cell-regulatory T lymphocyte crosstalk contributes to tumor-induced tolerance. Clin. Dev. Immunol. 2011, 430394 (2011).
Xu, J. Y. et al. Association of Plasma Epstein-Barr Virus DNA With Outcomes for Patients With Recurrent or Metastatic Nasopharyngeal Carcinoma Receiving Anti-Programmed Cell Death 1 Immunotherapy. JAMA Netw. Open 5, e220587 (2022).
Yang, Y. et al. Efficacy, safety, and biomarker analysis of Camrelizumab in Previously Treated Recurrent or Metastatic Nasopharyngeal Carcinoma (CAPTAIN study). J. Immunother. Cancer 9, https://doi.org/10.1136/jitc-2021-003790 (2021).
Acosta, J. N., Falcone, G. J., Rajpurkar, P. & Topol, E. J. Multimodal biomedical AI. Nat. Med 28, 1773–1784 (2022).
Prelaj, A. et al. Artificial intelligence for predictive biomarker discovery in immuno-oncology: a systematic review. Ann. Oncol. 35, 29–65 (2024).
Acknowledgements
We acknowledge financial support from the National Key Research and Development Program of China (2023YFF1204600); National Natural Science Foundation of China (82227802, 82302306, 82302336); Clinical Frontier Technology Program of the First Affiliated Hospital of Jinan University (JNU1AF-CFTP-2022-a01201); the Science and Technology Projects in Guangzhou (202201020022, 2023A03J1036, 2023A03J1038); the Science and Technology Youth Talent Nurturing Program of Jinan University (21623209); the Postdoctoral Science Foundation of China (2022M721349). We also thank Figdraw (www.Figdraw.com) for the assistance in creating Fig. 1.
Author information
Authors and Affiliations
Contributions
Xin Liu and Bin Zhang were responsible for the concept proposal and study design. Bin Zhang, Shuixing Zhang, Lu Zhang, and Wenhui Huang conceptualized the study, attained funding, provided supervision, prepared the initial draft, and reviewed and revised the final manuscript. Xin Liu wrote the manuscript with feedback and contributions from all other authors. Xin Lu, Hui Shen, and Bin Zhang contributed to the data analysis and writing of the manuscript. All authors have revised, read, and agreed to the final version of the manuscript.
Corresponding authors
Ethics declarations
Competing interests
The authors declare that they have no known competing financial interests or personal relationships that could have appeared to influence the work reported in this paper.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Liu, X., Shen, H., Zhang, L. et al. Immunotherapy for recurrent or metastatic nasopharyngeal carcinoma. npj Precis. Onc. 8, 101 (2024). https://doi.org/10.1038/s41698-024-00601-1
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41698-024-00601-1