Abstract
Background/Objectives
Reduced serum magnesium (Mg) levels have been associated with obesity, insulin resistance (IR), type 2 diabetes, and metabolic syndrome in adults. However, in the children population, the evidence is still limited. In this cross-sectional study, we aimed to analyze the association of serum Mg levels with the frequency of overweight and obesity and cardiometabolic traits in 189 schoolchildren (91 girls and 98 boys) between 6 and 12 years old from Mexico City.
Subjects/Methods
Anthropometrical data were collected and biochemical parameters were measured by enzymatic colorimetric assay. Serum Mg level was analyzed by inductively coupled plasma mass spectrometry (ICP-MS). The triglyceride-glucose (TyG) index was used as a surrogate marker to evaluate IR.
Results
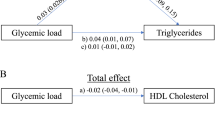
Serum Mg level was negatively associated with overweight (Odds ratio [OR] = 0.377, 95% confidence interval [CI] 0.231–0.614, p < 0.001) and obesity (OR = 0.345, 95% CI 0.202–0.589, p < 0.001). Serum Mg level resulted negatively associated with body mass index (BMI, β = −1.16 ± 0.26, p < 0.001), BMI z-score (β = −0.48 ± 0.10, p < 0.001) and TyG index (β = −0.04 ± 0.04, p = 0.041). Through a mediation analysis was estimated that BMI z-score accounts for 60.5% of the negative association of serum Mg level with IR (Sobel test: z = 2.761; p = 0.005).
Conclusion
Our results evidence that BMI z-score mediate part of the negative association of serum Mg level and IR in Mexican schoolchildren.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
Data availability
The datasets generated during and/or analyzed during the current study are available from the corresponding author on reasonable request.
References
Okati-Aliabad H, Ansari-Moghaddam A, Kargar S, Jabbari N. Prevalence of Obesity and Overweight among Adults in the Middle East Countries from 2000 to 2020: A Systematic Review and Meta-Analysis. J Obes. 2022;2022, 8074837.
Shamah-Levy T, Gaona-Pineda E, Cuevas-Nasu L, Morales-Ruan C, Valenzuela-Bravo D, Méndez-Gómez Humarán I, et al. Prevalencias de sobrepeso y obesidad en población escolar y adolescente de México. Ensanut Continua 2020-2022. Salud Publica Mex. 2023;65:S218–S22.
Piché ME, Poirier P. Obesity, ectopic fat and cardiac metabolism. Expert Rev Endocrinol Metab. 2018;13:213–21.
Lin X, Li H. Obesity: Epidemiology, Pathophysiology, and Therapeutics. Front Endocrinol. 2021;12:706978.
Blüher M. Obesity: global epidemiology and pathogenesis. Nat Rev Endocrinol. 2019;15:288–98.
Loos RJF, Yeo GSH. The genetics of obesity: from discovery to biology. Nat Rev Genet. 2022;23:120–33.
Piuri G, Zocchi M, Della Porta M, Ficara V, Manoni M, Zuccotti GV, et al. Magnesium in Obesity, Metabolic Syndrome, and Type 2 Diabetes. Nutrients. 2021;13:320.
Ricciuto L, Fulgoni VL 3rd, Gaine PC, Scott MO, DiFrancesco L. Intakes of Added Sugars, with a Focus on Beverages and the Associations with Micronutrient Adequacy in US Children, Adolescents, and Teens (NHANES 2003-2018). Nutrients. 2023;15:3285.
Fiorentini D, Cappadone C, Farruggia G, Prata C. Magnesium: Biochemistry, Nutrition, Detection, and Social Impact of Diseases Linked to Its Deficiency. Nutrients. 2021;13:320.
Maguire D, Talwar D, Shiels PG, McMillan D. The role of thiamine dependent enzymes in obesity and obesity related chronic disease states: A systematic review. Clin Nutr ESPEN. 2018;25:8–17.
Mishra S, Padmanaban P, Deepti G, Sarkar G, Sumathi S, Toora B. Serum magnesium and dyslipidemia in type-2 diabetes mellitus. Biomed Res. 2012;23:295–300.
Zhang Y, Huang B, Jin J, Xiao Y, Ying H. Recent advances in the application of ionomics in metabolic diseases. Front Nutr. 2022;9:1111933.
Al Shammaa A, Al-Thani A, Al-Kaabi M, Al-Saeed K, Alanazi M, Shi Z. Serum Magnesium is Inversely Associated with Body Composition and Metabolic Syndrome. Diabetes Metab Syndr Obes. 2023;16:95–104.
Lu L, Chen C, Yang K, Zhu J, Xun P, Shikany JM, et al. Magnesium intake is inversely associated with risk of obesity in a 30-year prospective follow-up study among American young adults. Eur J Nutr. 2020;59:3745–53.
Askari M, Mozaffari H, Jafari A, Ghanbari M, Darooghegi Mofrad M. The effects of magnesium supplementation on obesity measures in adults: a systematic review and dose-response meta-analysis of randomized controlled trials. Crit Rev Food Sci Nutr. 2021;61:2921–37.
Barbagallo M, Veronese N, Dominguez LJ. Magnesium in Type 2 Diabetes Mellitus, Obesity, and Metabolic Syndrome. Nutrients. 2022;14:714.
Chutia H, Lynrah KG. Association of Serum Magnesium Deficiency with Insulin Resistance in Type 2 Diabetes Mellitus. J Lab physicians. 2015;7:75–8.
Li W, Jiao Y, Wang L, Wang S, Hao L, Wang Z, et al. Association of Serum Magnesium with Insulin Resistance and Type 2 Diabetes among Adults in China. Nutrients. 2022;14:1799.
Akyuz O, Gucun M, Demirci R, Celik M. Relationship Between Serum Magnesium Level and Insulin Resistance in Turkey Non-obese Adult Population. Biol Trace Elem Res. 2022;200:3070–7.
Shamnani G, Bhartiy SS, Jiwane R, Gupta V, Verma N, Verma D. Correlation of Serum Magnesium with Insulin Resistance in North Indian Adult Population. Curr Diabetes Rev. 2020;16:254–61.
Tao LC, Xu JN, Wang TT, Hua F, Li JJ. Triglyceride-glucose index as a marker in cardiovascular diseases: landscape and limitations. Cardiovasc Diabetol. 2022;21:68.
Huerta MG, Roemmich JN, Kington ML, Bovbjerg VE, Weltman AL, Holmes VF, et al. Magnesium deficiency is associated with insulin resistance in obese children. Diabetes Care. 2005;28:1175–81.
Yakinci C, Pac A, Kucukbay FZ, Tayfun M, Gul A. Serum zinc, copper, and magnesium levels in obese children. Acta Paediatr Jpn. 1997;39:339–41.
Hassan SAU, Ahmed I, Nasrullah A, Haq S, Ghazanfar H, Sheikh AB, et al. Comparison of Serum Magnesium Levels in Overweight and Obese Children and Normal Weight Children. Cureus. 2017;9:e1607.
Guerrero-Romero F, Flores-Garcia A, Saldana-Guerrero S, Simental-Mendia LE, Rodriguez-Moran M. Obesity and hypomagnesemia. Eur J Intern Med. 2016;34:29–33.
Celik N, Andiran N, Yilmaz AE. The relationship between serum magnesium levels with childhood obesity and insulin resistance: a review of the literature. J Pediatr Endocrinol Metab. 2011;24:675–8.
Guerrero-Romero F, Rodriguez-Moran M, Hernandez-Ronquillo G, Gomez-Diaz R, Pizano-Zarate ML, Wacher NH, et al. Low Serum Magnesium Levels and Its Association with High Blood Pressure in Children. J Pediatr. 2016;168:93–8.e1.
WHO. Physical status: the use and interpretation of anthropometry. Geneva: World Health Organization. 1995.
WHO. Growth Reference Data for School-aged Children and Adolescents of 5-19 Years. World Health Organization. 2007. Retreived from: http://www.who.int/growthref/en/.
DeLong DM, DeLong ER, Wood PD, Lippel K, Rifkind BM. A comparison of methods for the estimation of plasma low- and very low-density lipoprotein cholesterol. The Lipid Research Clinics Prevalence Study. JAMA. 1986;256:2372–7.
Guerrero-Romero F, Simental-Mendia LE, Gonzalez-Ortiz M, Martinez-Abundis E, Ramos-Zavala MG, Hernandez-Gonzalez SO, et al. The product of triglycerides and glucose, a simple measure of insulin sensitivity. Comparison with the euglycemic-hyperinsulinemic clamp. J Clin Endocrinol Metab. 2010;95:3347–51.
Mohd Razali N, Yap B. Power Comparisons of Shapiro-Wilk, Kolmogorov-Smirnov, Lilliefors and Anderson-Darling Tests. J Stat Model Anal. 2011;2:21–33.
Baron RM, Kenny DA. The moderator-mediator variable distinction in social psychological research: conceptual, strategic, and statistical considerations. J Pers Soc Psychol. 1986;51:1173–82.
Preacher KJ, Hayes AF. SPSS and SAS procedures for estimating indirect effects in simple mediation models. Behav Res Methods Instrum Comput. 2004;36:717–31.
Morais JB, Severo JS, Santos LR, de Sousa Melo SR, de Oliveira Santos R, de Oliveira AR, et al. Role of Magnesium in Oxidative Stress in Individuals with Obesity. Biol Trace Elem Res. 2017;176:20–6.
Gaona-Pineda EB, Rodríguez-Ramírez S, Medina-Zacarías MC, Valenzuela-Bravo DG, Martinez-Tapia B, Arango-Angarita A. Consumidores de grupos de alimentos en población mexicana. Ensanut Continua 2020–2022. Salud Pública México. 2023;65:s248–s58.
Peuhkuri K, Vapaatalo H, Korpela R. Even low-grade inflammation impacts on small intestinal function. World J Gastroenterol. 2010;16:1057–62.
Lefebvre PJ, Paolisso G, Scheen AJ. Magnesium and glucose metabolism. Therapie. 1994;49:1–7.
Pelczynska M, Moszak M, Bogdanski P. The Role of Magnesium in the Pathogenesis of Metabolic Disorders. Nutrients. 2022;14:1714.
Brito ADM, Hermsdorff HHM, Filgueiras MS, Suhett LG, Vieira-Ribeiro SA, Franceschini S, et al. Predictive capacity of triglyceride-glucose (TyG) index for insulin resistance and cardiometabolic risk in children and adolescents: a systematic review. Crit Rev food Sci Nutr. 2021;61:2783–92.
Furdela V, Pavlyshyn H, Shulhai AM, Kozak K, Furdela M. Triglyceride glucose index, pediatric NAFLD fibrosis index, and triglyceride-to-high-density lipoprotein cholesterol ratio are the most predictive markers of the metabolically unhealthy phenotype in overweight/obese adolescent boys. Front Endocrinol. 2023;14:1124019.
Angoorani P, Heshmat R, Ejtahed HS, Motlagh ME, Ziaodini H, Taheri M, et al. Validity of triglyceride-glucose index as an indicator for metabolic syndrome in children and adolescents: the CASPIAN-V study. Eat Weight Disord. 2018;23:877–83.
Ahmed B, Sultana R, Greene MW. Adipose tissue and insulin resistance in obese. Biomed Pharmacother. 2021;137:111315.
Paolisso G, Scheen A, D’Onofrio F, Lefèbvre P. Magnesium and glucose homeostasis. Diabetologia. 1990;33:511–4.
Reis MAB, Reyes FGR, Saad MJA, Velloso LA. Magnesium Deficiency Modulates the Insulin Signaling Pathway in Liver but Not Muscle of Rats1. J Nutr. 2000;130:133–8.
Kostov K. Effects of Magnesium Deficiency on Mechanisms of Insulin Resistance in Type 2 Diabetes: Focusing on the Processes of Insulin Secretion and Signaling. Int J Mol Sci. 2019;20:1351.
Bravo M, Simón J, González-Recio I, Martinez-Cruz LA, Goikoetxea-Usandizaga N, Martínez-Chantar ML. Magnesium and Liver Metabolism Through the Lifespan. Adv Nutr. 2023;14:739–51.
Liu M, Dudley SC Jr. Magnesium, Oxidative Stress, Inflammation, and Cardiovascular Disease. Antioxid. 2020;9:907.
Matulewicz N, Karczewska-Kupczewska M. Insulin resistance and chronic inflammation. Postepy Hig Med Doswiadczalnej. 2016;70:1245–58.
Al-Beltagi M, Bediwy AS, Saeed NK. Insulin-resistance in paediatric age: Its magnitude and implications. World J Diabetes. 2022;13:282–307.
Acknowledgements
We thank all participants of this study.
Funding
The present work was supported by Consejo Nacional de Ciencia y Tecnología (CONACYT) in the following projects: Laboratorio Nacional de Ciencia, Tecnología y Gestión Integrada del Agua (Project: 315880-CONACYT) and by Hospital Infantil de México Federico Gómez (Fondos Federales HIM/2013/003).
Author information
Authors and Affiliations
Contributions
MJRL, HHM, JISF, JVG, and MVM, designed the study, performed the statistical analysis, wrote the manuscript, and designed tables and figures. MJRL, HHM, MKK, MC, JISF, ECP, IMN, JVG, and MVM, collect the data and critically reviewed the manuscript. MJRL, HHM, ECP, and IMN, samples treatment and analysis by ICP-MS. All authors read and approved the final manuscript.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethical approval
This observational study was conducted according to the guidelines established in the Declaration of Helsinki and based on the Regulations of the General Health Law on Health Research in Mexico. The research protocol was approved by the Hospital Infantil de México Federico Gómez Research, Ethics, and Biosecurity Committees (approval register: HIM/2013/003).
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Rios-Lugo, M.J., Serafín-Fabián, J.I., Hernández-Mendoza, H. et al. Mediation effect of body mass index on the association between serum magnesium level and insulin resistance in children from Mexico City. Eur J Clin Nutr (2024). https://doi.org/10.1038/s41430-024-01447-3
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41430-024-01447-3