Abstract
Treatment of mucopolysaccharidosis type VII (MPS VII) mice with recombinant mouse β-glucuronidase injections has been shown to deliver enzyme to most tissues and to reduce lysosomal storage during the first 6 wk of life. Here we determine the effect of enzyme therapy limited to the first 6 wk of life on survival and growth and follow the subsequent accumulation of lysosomal storage after β-glucuronidase treatment is discontinued. MPS VII mice received 28,000 U of β-glucuronidase i.v. at weekly intervals from birth to 6 wk of life and were killed at intervals up to 1 y after the last injection. By 29 d after the last enzyme injection, lysosomal storage material in bone was no different in amount than that seen in untreated MPS VII mice. By 85 d, the fixed tissue macrophage system, meninges, and brain glia had also accumulated storage comparable to that seen in untreated controls. One year after treatment, lysosomal storage was similar to that of untreated MPS VII mice in all sites except cortical neurons, where there was still a slight reduction. All treated mice that were not killed earlier, lived longer, were larger, and had milder facial and skeletal deformities than untreated MPS VII mice. These data show that enzyme replacement therapy in MPS VII mice during the first 6 wk of life improves survival and growth. After treatment is discontinued, storage accumulates slowly in the brain and more rapidly in the fixed tissue macrophage system. Whether therapy continued later in life can further improve survival and growth remains to be established.
Similar content being viewed by others
Main
The MPS are inherited disorders caused by the deficiency of a lysosomal enzyme needed for the degradation of GAG. Affected patients have progressive accumulation of GAG in lysosomes, leading to organ dysfunction. A murine model of MPS type VII due to a single base-pair deletion in the β-gluc (EC 3.2.1.31) gene has undetectable levels of enzyme activity and shares clinical, pathologic, and biochemical features with human MPS VII or Sly syndrome(1–3). Affected mice have a shortened survival(1), cognitive dysfunction(4), and lysosomal storage in many sites including the brain, fixed tissue macrophage system, and skeleton(2). They are dwarfed with skeletal dysplasia similar to dysostosis multiplex. The MPS VII mice have proven to be a useful model for testing experimental treatment strategies for lysosomal storage diseases, including bone marrow transplantation, enzyme replacement, and gene therapy(5–9).
Treatment of lysosomal storage diseases with infusion of the deficient lysosomal enzyme has proven useful in Gaucher disease(10–13). The availability of phosphorylated recombinant β-gluc with the recognition marker necessary for receptor-mediated endocytosis allows investigation of the effect of enzyme replacement on murine MPS VII. We have previously shown β-gluc administered i.v. is taken up by many tissues in the MPS VII mouse(14) and causes a reduction in lysosomal storage in mice treated from birth until 6 wk of age(8). We now show that this short course of enzyme therapy early in life prolongs survival and improves growth. We also show the differences in the rates of lysosomal storage accumulation in various tissues and cell types after discontinuation of treatment.
METHODS
Fourteen homozygous newborn MPS VII mice received 6 weekly i.v. injections of 28,000 U recombinant mouse β-gluc prepared as previously described(8, 15). This dose is approximately 3.5-7 mg/kg in the 0.5-1-g newborn, but only 0.14 mg/kg in the 6-wk-old, 25-g mouse. All experiments were performed with the highest standards of humane care. The Jackson Laboratory is fully accredited by the American Association for Accreditation of Laboratory Animal Care.
Two of the treated MPS VII mice and one control, untreated MPS VII mouse were killed at 14, 29, 85, or 150 d after their last β-gluc injection when they were 49, 64, 120, or 185 d of age, respectively (group 1). One treated MPS VII mouse died unexpectedly at 375 d of age and was not examined histologically. The remaining five were killed at 391 d of age, 1 y after the last β-gluc injection (group 2). Mice were weighed, and tissues were sampled for biochemical analysis as previously described. The levels ofβ-gluc, β-hexosaminidase (EC 3.2.1.52), and α-galactosidase(EC 3.2.1.22) were determined in liver and spleen from the animals killed at 14, 85, and 150 d after the last enzyme injection and in liver, spleen, brain, and kidney from mice killed 1 y after enzyme injection. Enzyme levels were compared with those in organs from previously reported enzyme-replaced MPS VII mice(8), and with those of age-matched normal, and with three untreated MPS VII mice ranging from 53-153 d of age.
Tissues were collected, fixed, and prepared for histology as previously described(2, 8). For histology, toluidine bluestained, 0.5-μm-thick sections of tissue embedded in Spurr's resin were evaluated for lysosomal storage. For the brain, two transverse sections, one at the level of the hippocampus, and including the temporal cortex, and the other at the level of the brain stem and cerebellum were examined. Tissues were evaluated with those from other ongoing studies without knowledge as to therapy using a semiquantitative scale. Marked reduction in lysosomal storage was determined when storage was inapparent and tissue sections were indistinguishable by light microscopy from those of the normal mouse. A moderate decrease in storage was identified when lysosomal distention was present, but clearly much less than in untreated MPS VII controls, and a slight decrease indicated a mild but definite reduction in storage compared with untreated MPS VII controls. These assessments were made by histologic study of the entire tissue sample section for each organ, except for the brain, where two sections were studied. For all but the oldest animals, tissues from age-matched untreated MPS VII animals were used as controls. Because untreated MPS VII mice do not survive to 391 d, the 185-d-old control and untreated MPS VII mice older than 200 d from previous experiments were used as controls. Selected tissues were studied with a histochemical technique to demonstrate β-gluc(14, 16).
Survival of mice in group 2 was compared with that of previously reported untreated MPS VII and normal mice(5). Long bone lengths were determined from radiographs(6). Bone lengths and body weights from mice in group 2 were compared with those of adult sex-matched, untreated MPS VII mice up to 218 d of age, as previously described(6), using the t test for statistical significance.
RESULTS
Group 1 (14-150 d after β-gluc therapy).
In the treated MPS VII mice, β-gluc was histochemically and biochemically demonstrable in the liver and spleen at 14 d but not at 85 d after the last β-gluc injection (Table 1). The secondary elevations in the lysosomal enzymes α-galactosidase andβ-hexosaminidase remained lower than in untreated MPS VII mice at 14 d after the last enzyme injection (Table 1), but by 85 d, they had returned to levels similar to those observed in untreated MPS VII mice. Observations on accumulation of storage in various tissues and cell types are summarized in Table 2. Spleen and liver sinus lining cells in treated MPS VII animals had less storage than untreated mice at 29 d after therapy but, by 85 d of age, storage had accumulated to the same level seen in untreated animals. Lysosomal distention in the cells in the bone including osteocytes and osteoblasts, marrow cells and marrow sinus lining cells was less than in age matched MPS VII controls at 14 d after the last injection. However, by 29 d after treatment was discontinued, only the marrow cells showed less storage than those of age-matched controls. Chondrocytes failed to respond to enzyme therapy at any time, as previously observed(8).
In the brain, storage does not accumulate to mutant levels in hippocampal pyramidal, and neocortical neurons, even 150 d after last β-gluc injection (Fig. 1, A and B). Glial and meningeal lysosomal storage was clearly less than in untreated MPS VII mice at 14 and 29 d, but was no longer different by 85 d after the last enzyme injection. Purkinje cells showed no response to enzyme replacement therapy even at the earliest time point.
Cortical neurons from a MPS VII animal who received the last β-gluc injection 150 d before sacrifice (A) had less cytoplasmic vacuolization than a similarly aged untreated MPS VII mouse(B). A perivascular cell in the treated mouse (A) contains abundant lysosomal storage. One year after the last β-gluc injection, three of five treated MPS VII mice still had less lysosomal storage in cortical neurons (C) than old untreated MPS VII mice.(A-C, ×391; toluidine blue.)
Group 2 (365 d after β-gluc therapy).
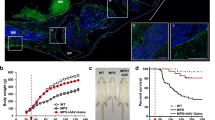
The mice studied 1 y after β-gluc therapy had a markedly prolonged life span compared with untreated MPS VII mice which usually die at 5-7 mo of age(1, 5) (Fig. 2). Although phenotypically still distinguishable as MPS VII mice, these long-term survivors had a marked improvement in their clinical appearance; they were more alert with a more normal gait and coat texture. Their body weight was 93.2% of normal, and bone lengths were 91.5% of normal 1 y after discontinuation of treatment. These both were markedly improved compared with those of adult untreated MPS VII animals up to 218 d of age (71.2 and 85.2% of normal, respectively, body weight p < 0.01, bone lengthp < 0.025).
All of the MPS VII mice in group 2 (circles) treated with β-gluc for 6 wk and then followed for effect of this early enzyme replacement therapy on survival and growth, lived for 1 y, and five of six lived until they were killed at 391 d of age. Untreated MPS VII mice have a much shorter life span (squares), and homozygous normal mice(triangles) have a normal survival of greater than 1 y.
β-Gluc was not detectable biochemically in liver, spleen, brain, or kidney 365 d after the last enzyme injection and the secondary increases inα-galactosidase and β-hexosaminidase were similar to those of untreated MPS VII mice (Table 1). Histologically, the bone cells had lysosomal distention similar to that seen in untreated MPS VII animals. However, the subchondral bone near the articular surface was more normally formed, in that it was more compact without the dilated perivascular lacunae characteristic of this area in the MPS VII mouse (Fig. 3, A-C). Three of the five long-term survivors had a decrease in neocortical neuronal cytoplasmic vacuolization (Fig. 1C), although storage in hippocampal pyramidal neurons, glia, meninges, and Purkinje cells was similar to that in old untreated MPS VII mice. Liver and spleen sinus lining cells had cytoplasmic vacuolization similar to that of the oldest untreated MPS VII mice examined(Table 2).
A stifle joint from a normal adult mouse (A), is distinguishable from that of a 391-d-old MPS VII mouse 1 y after the lastβ-gluc injection (B). The treated MPS VII animal's joint has osteocytes, chondrocytes, and synovial cells distended by lysosomal storage, but the subchondral bone is better formed and lacks the large perivascular lacunae typical of the untreated MPS VII mouse (arrow)(C). (A-C, ×62; hematoxylin and eosin.)
DISCUSSION
Recombinant β-gluc therapy administered to MPS VII mice in the first weeks of life, when clinical evidence of disease is minimal and the amount of lysosomal storage is small, results in a decrease in lysosomal storage in multiple tissues(8). The brain and bone, two sites which have been somewhat resistant to treatment with bone marrow transplant in adults(5, 6), have a clear reduction in lysosomal storage after 6 wk of β-gluc therapy begun in the newborn period(8). Until now, the effect of early enzyme therapy on survival, growth, and development in the young MPS VII animal was not defined, nor was the rate at which storage accumulates in various organs and cell types after cessation of β-gluc replacement therapy established.
We have determined that β-gluc activity is demonstrable for at least 14 d after the last enzyme injection in the fixed tissue macrophage system and lysosomal storage is reduced for at least 29 d after enzyme injection. The disappearance of β-gluc activity and the increase in the secondary elevations of α-galactosidase and β-hexosaminidase correlate with the appearance of lysosomal storage in the fixed tissue macrophage system. These observations suggest that monthly β-gluc injections might be sufficient to prevent accumulation of lysosomal storage in liver and spleen in the adult MPS VII mouse. Although bone accumulates lysosomal storage to the same extent as in untreated MPS VII mice by 29 d after the last injection, this short course of therapy markedly improved bone growth and morphologic evidence of dysplasia was reduced even after 1 y. It is likely that the high levels of β-gluc achieved in the bone with injections beginning in the newborn period(14) are important in improving GAG turnover in the rapidly growing skeleton and that this effect of early enzyme therapy has a lasting impact on bone development.
In the brain, several neuronal groups respond differently to early enzyme replacement therapy. The Purkinje cells are refractory even in young animals(8) but neocortical and hippocampal pyramidal neurons respond early and accumulate lysosomal storage slowly after cessation ofβ-gluc therapy. The relatively slow accumulation of lysosomal storage in the responsive neuronal groups in the neocortex and hippocampus suggests a low requirement for β-gluc in these neurons once the brain has developed. From these observations one can infer that the turnover ofβ-glucuronide-containing GAG is low in cortical neurons of the adult MPS VII mouse. Slow turnover of GAG in adult cortical neurons may explain why the mental retardation in many MPS VII patients is relatively nonprogressive after early childhood(17).
The good response in neocortical and hippocampal neurons, glia, and meninges early in life suggests that infused enzyme is accessible to these cell types in the very young mouse. This is surprising in view of data suggesting that the mouse blood-brain barrier becomes impermeable to protein around embryonic d 16(18). However, others have observed that this barrier is not morphologically mature in mice 10 d after birth(19). We have previously demonstrated β-gluc enzyme activity in meninges, choroid plexus, and vessels but not in neurons in the newborn MPS VII mouse pup brain after enzyme infusion(14). Whether there is a low level of β-gluc activity in neurons that is sufficient to produce correction but is below the level of detection with this histochemical stain remains to be established by a more sensitive detection method. How long after the newborn period the neocortical and hippocampal neurons are responsive to correction by infused enzyme also remains to be established. It is not clear why the Purkinje cells fail to respond to therapy even in the young animal.
The clinical improvement resulting from early enzyme replacement lasts well beyond the time when histologic improvement in most tissues is no longer apparent. Whatever the mechanism, early β-gluc therapy clearly has an impact on survival and growth in the MPS VII mouse. Presumably, it is the early amelioration of GAG accumulation which allows more normal growth and development. The importance of GAG in early brain development has been established(20). There is preliminary evidence of a decrease in neuronal cell density in the brain in murine MPS VII, suggesting either cell loss or abnormal neuronal development in this model(21). Reducing abnormal GAG accumulation early in brain development in murine MPS VII may prevent these neuronal alterations. The present studies lack quantitative data on GAG accumulation to correlate with the morphologic and enzymatic data. However, defining GAG accumulation and its correlation with clinical and pathologic findings in enzyme replaced MPS VII mice should be possible with this model.
This model system has several attractive features for evaluating experimental strategies for lysosomal storage diseases. These include the remarkable stability of the murine and human β-gluc, detailed information on their oligosaccharide side chains(22, 23), considerable information from prior studies on the uptake, distribution, and fate of infused β-gluc in rodents(24, 25), and data on the cell surface receptors that mediate enzyme uptake by various cell types(25, 26). Although many lessons derived from this model should apply to other storage diseases, some storage diseases have unique features that are not generalizable. For example, Gaucher disease affects mainly fixed tissue macrophages, and the enzyme which has been successful in treatment of Gaucher disease(10–13) is an acid hydrolase that does not use the mannose 6-phosphate targeting pathway, as do most other hydrolases. On the other hand, it is worth remembering that the mannose receptor, which is the target of mannose-terminated β-glucosidase in Gaucher disease, was actually discovered by studies of binding and uptake of nonphosphorylated forms of β-gluc by fixed tissue macrophages in the rat(25, 26). The murine model presented here should, at the very least, define the target cells accessible to infused phosphorylated enzyme. Because many acid hydrolases are considerably smaller than the 300-kD tetrameric β-gluc, the smaller enzymes may have even greater access to some cell types, and results of enzyme replacement with these enzymes may be even more favorable than those reported here for murine MPS VII.
Abbreviations
- MPS:
-
mucopolysaccharidosis
- GAG:
-
glycosaminoglycan
- β-gluc:
-
β-glucuronidase
References
Birkenmeier EH, Davisson MT, Beamer WG, Ganschow RE, Vogler CA, Gwynn B, Lyford KA, Maltais LM, Wawrzyniak CJ 1989 Murine mucopolysaccharidosis type VII: Characterization of a mouse with-glucuronidase deficiency. J Clin Invest 83: 1258–1266.
Vogler C, Birkenmeier EH, Sly WS, Levy B, Pegors C, Kyle JW, Beamer WG 1990 A murine model of mucopolysaccharidosis VII: gross and microscopic findings in -glucuronidase-deficient mice. Am J Pathol 136: 207–217.
Sands MS, Birkenmeier EH 1993 A single-base-pair deletion in the β-glucuronidase gene accounts for the phenotype of murine mucopolysaccharidosis type VII. Proc Natl Acad Sci USA 90: 6567–6571.
Chang PL, Lambert DT, Pisa MA 1993 Behavioural abnormalities in a murine model of a human lysosomal storage disease. Neuroreport 4: 507–510.
Birkenmeier EH, Barker JE, Vogler CA, Kyle JW, Sly WS, Gwynn B, Levy B, Pegors C 1991 Increased life span and correction of metabolic defects in murine mucopolysaccharidosis type VII after syngeneic bone marrow transplantation. Blood 78: 3081–3092.
Sands MS, Barker JE, Vogler C, Levy B, Gwynn B, Galvin N, Sly WS, Birkenmeier E 1993 Treatment of murine mucopolysaccharidosis type VII by syngeneic bone marrow transplantation in neonates. Lab Invest 68: 676–686.
Sands MS, Erway LC, Vogler C, Sly WS, Birkenmeier EH 1995 Syngeneic bone marrow transplantation reduces hearing loss associated with murine mucopolysaccharidosis type VII. Blood 86: 2033–2040.
Sands MS, Vogler C, Kyle JW, Grubb JH, Levy B, Galvin N, Sly WS, Birkenmeier EH 1994 Enzyme replacement therapy for murine mucopolysaccharidosis type VII. J Clin Invest 93: 2324–2331.
Wolfe JH, Sands MS, Barker JE, Gwynn B, Rowe LB, Vogler CA, Birkenmeier EH 1992 Reversal of pathology in murine mucopolysaccharidosis type VII by somatic cell gene transfer. Nature 360: 749–753.
Barton NW, Brady RO, Dambrosia JM, DiBisceglie AM, Doppelt SH, Hill SC, Mankin HJ, Murray GJ, Parker RI, Argoff CE, Grewal RP, Yu KT, and collaborators 1991 Replacement therapy for inherited enzyme deficiency-macrophage targeted glucocerebrosidase for Gaucher's disease. N Engl J Med 324: 1464–1470
Beutler E 1993 Modern diagnosis and treatment of Gaucher's disease. Am J Dis Child 147: 1175–1183.
Zimran A, Elstein D, Kannai R, Zevin S, Hadas-Halpern I, Levy-Lahad E, Cohen Y, Horowitz M, Abrahamov A 1994 Low-dose enzyme replacement therapy for Gaucher's disease: effects of age, sex, genotype and clinical features on response to treatment. Am J Med 97: 3–13.
Grabowski GA, Barton NW, Pastores G, Dambrosia JM, Banerjee TK, McKee MA, Parker C, Schiffmann R, Hill SC, Brady RO 1995 Enzyme therpay in type I Gaucher disease: comparative efficacy of mannose-terminated glucocerebrosidase from natural and recombinant sources. Ann Intern Med 122: 33–39.
Vogler C, Sands M, Higgins A, Levy B, Grubb J, Birkenmeier EH, Sly WS 1993 Enzyme replacement with recombinantβ-glucuronidase in the newborn mucopolysaccharidosis type VII mouse. Pediatr Res 34: 837–840.
Grubb JH, Kyle JW, Cody LB, Sly WS 1993 Large scale purification of phosphorylated recombinant human β-glucuronidase from overexpressing mouse L cells. FASEB J 7:A1255.
Wolfe JH, Sands MS 1995 Murine mucopolysaccharidosis type VII: A model system for somatic gene therapy of the central nervous system. In: Lowenstein P, Enquist L (eds) Gene Transfer into Neurones, Towards Gene Therapy of Neurological Disorders. J Wiley & Sons, Essex, England (in press) pp
Neufeld EF, Muenzer J 1995 The mucopolysaccharidosis. In: Scriver CR, Beaudet AL, Sly WS, Valle D (eds) The Metabolic Basis of Inherited Disease, 7th ED. McGraw-Hill, New York, pp 2465–2494.
Risau W, Hallmann R, Albrecht U 1986 Differentiation-dependent expression of proteins in brain endothelium during development of the blood-brain barrier. Dev Biol 117: 537–545.
Stewart PA, Hayakawa EM 1987 Interendothelial junctional changes underlie the developmental `tightening' of the blood-brain barrier. Dev Brain Res 32: 271–281.
Oohira A, Katoh-Semba R, Watanabe E, Matsui F 1994 Brain development and multiple molecular species of proteoglycan. Neurosci Res 20: 195–207.
Galvin NJ, Levy B, Vogler C 1994 Brain morphology in murine mucopolysaccharidosis type VII. Mol Biol Cell 5: 360a
Natowicz M, Baenziger JU, Sly WS 1982 Structural studies of the phosphorylated high mannose-type oligosaccharides on humanβ-glucuronidase. J Biol Chem 257: 4412–4420.
Shipley JM, Grubb JH, Sly WS 1993 The role of glycosylation and phosphorylation in the expression of active humanβ. J Biol Chem 268: 12193–12198.
Achord D, Brot F, Gonzalez-Noriega A, Sly WS, Stahl P 1977 Human β-glucuronidase II. Fate of infused human placentalβ-glucuronidase in the rat. Pediatr Res 11: 816–822.
Achord DT, Brot FE, Bell CE, Sly WS 1978 Humanβ-glucuronidase: in vivo clearance and in vitro uptake by a glycoprotein recognition system on reticuloendothelial cells. Cell 15: 269–278.
Stahl PD, Rodman JS, Miller MJ, Schlesinger PH 1978 Evidence for receptor-mediated binding of glycoproteins, glycoconjugates, and lysosomal glycosidases by alveolar machrophages. Proc Natl Acad Sci USA 75: 1399–1403.
Author information
Authors and Affiliations
Additional information
Supported by National Institutes of Health Grant DK41082 (to E.H.B. and C.V.), DK40163 and GM34182 (to W.S.S.), and DK08546 (to M.S.S.).
Rights and permissions
About this article
Cite this article
Vogler, C., Sands, M., Levy, B. et al. Enzyme Replacement with Recombinant β-Glucuronidase in Murine Mucopolysaccharidosis Type VII: Impact of Therapy during the First Six Weeks of Life on Subsequent Lysosomal Storage, Growth, and Survival. Pediatr Res 39, 1050–1054 (1996). https://doi.org/10.1203/00006450-199606000-00019
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1203/00006450-199606000-00019
This article is cited by
-
Mucopolysaccharidoses and the blood–brain barrier
Fluids and Barriers of the CNS (2022)
-
Vestronidase Alfa: A Review in Mucopolysaccharidosis VII
BioDrugs (2019)
-
Pharmacokinetic and Pharmacodynamic Modeling to Optimize the Dose of Vestronidase Alfa, an Enzyme Replacement Therapy for Treatment of Patients with Mucopolysaccharidosis Type VII: Results from Three Trials
Clinical Pharmacokinetics (2019)
-
Early initiation of enzyme replacement therapy improves metabolic correction in the brain tissue of aspartylglycosaminuria mice
Journal of Inherited Metabolic Disease (2010)
-
Mannitol-facilitated CNS entry of rAAV2 vector significantly delayed the neurological disease progression in MPS IIIB mice
Gene Therapy (2009)